Playlist
Show Playlist
Hide Playlist
Other Agents to Treat Tuberculosis – Antimycobacterial Agents
-
Slides Other Agents to Treat Tuberculosis Antimycobacterial Agents.pdf
-
Reference List Pharmacology.pdf
-
Download Lecture Overview
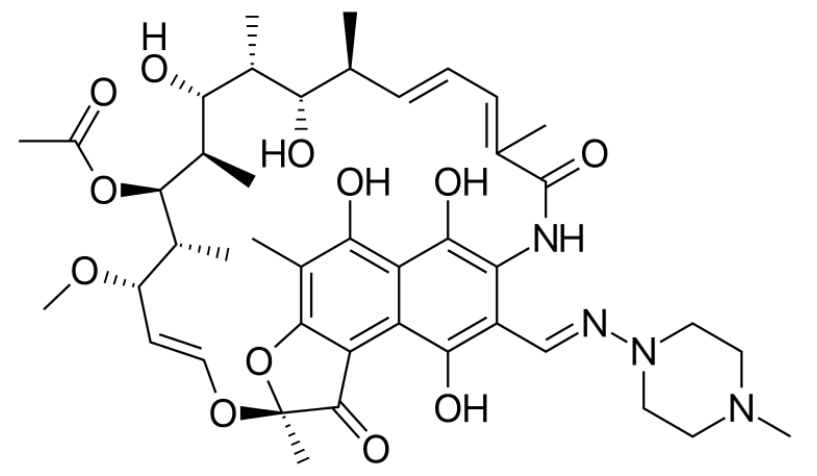
00:01 Now this issue of multiple resistance with our traditional drugs is why we have these other TB agents that we can use. 00:09 Streptomycin is a great example. 00:11 Now streptomycin is an aminoglycoside, it’s a complex molecule as you can see here and the nice thing about this particular agent is that we can use it multiple drug resistance tuberculosis. 00:23 We’ve also used it in mycobacterium avium complex, we’ve used it in endocarditis. 00:28 We can use it brucellosis and other kinds of infections including Burkholderia. 00:34 It’s even used in the plaque tularemia or even rat bite fever, so this is a fairly broad spectrum well-used medication. 00:44 It’s reasonably well-tolerated but the toxicity is definitely there and you have to be aware of it. 00:50 One of the toxic issues that we have with this and all aminoglycoside is renal dysfunction. 00:55 Another thing that we have to be aware of like all aminoglycoside is otosclerosis and ototoxicity. 01:01 Now the ototoxicity can also include auditory toxicity in others words ringing of the ears or loss of hearing. 01:09 Of course, in pregnant woman we have to be very careful because there’s a risk of ototoxicity in the fetus or child and that may result in permanent deafness so it is a drug that we have to be wary of in pregnant patients. 01:25 Now it is safe in breastfeeding, it is not excreted in any meaningful quantity in breast milk. 01:31 Another drug that we use often in this class are is amikacin. 01:37 Now we’ve already spoken about this particular drug in our other lectures. 01:41 It is a drug that binds to the 30S subunit of the ribosome. 01:47 It is very good at preventing or inhibiting protein synthesis within the organism. 01:52 It has multiple uses. 01:53 We use it in multi-drug resistant TB which is what this particular lecture is about but also, we use it in aerobic gram-negative bacterial infections that includes things like pseudomonas or acinetobacter infections. 02:07 We’ve used it in enterobacter ECA, we've used it in E. coli, we used it in salmonella, we used it on Klebsiella - so it’s a very useful drug in multiple areas. 02:18 We also used it to treat gram-positive infections and that includes things like staph and that includes things like nocardia. 02:25 The next drug in our list is a ethionamide. 02:28 Now, this particular drug is used in patients who have isoniazid resistant strains of TB. 02:37 It’s a prodrug and it is also converted by the bacterium into an active agent so it is something that requires an active bacterium, if it’s a dormant bacterium it may not work so well. 02:49 Now, it forms and adduct and it works in the same way as isoniazid did in - that I described earlier. 02:56 Resistance is actually quite common which is why this particular drug isn’t used as much as it was say 20 years ago. 03:04 Toxicity is exceedingly common and one of the things that we really notice about this particular drug is the amount of GI irritation - diarrhea, upset stomach, gassiness, bloating that people will complain about. 03:18 You can even get peptic ulcers from this medication and of course this drug is commonly seen with hypersensitivity reactions. 03:27 Rifabutin is another agent that we commonly use. 03:32 It is the same class as rifampin which you can see that’s a little bit more complicated of a structure. 03:38 It’s equally as affective as rifampin and it’s often preferred in patients who are HIV positive. 03:45 The reason being is because there’s less cytochrome activity of rifabutin compared to rifampin. 03:51 Rifampin is always problematic because it always messes with the drug levels of the other agents you're giving it with. 03:57 Many of the HIV drugs that we use go through cytochrome P450 systems and so therefore using rifampin at the same time can really be difficult in terms of figuring out what your drugs level are like. 04:09 The nice thing about rifabutin is that it doesn’t have as much cytochrome effects and therefore you have less drug interaction. 04:17 I’m just gonna throw in another drug here, rifaximin. 04:19 Rifaxamin is used in travelers diarrheas, it’s not used as an anti-tuberculosis drug. 04:24 The reason why I put it here is because this is acting in the same way - it has the same mechanism of action, it has some of the same pharmacologic profiles so just remember that this is not a TB drug, this is a traveler’s diarrhea drug. 04:37 Okay, I’m gonna add two more drugs to our list and you’re probably familiar with them already and in fact I’ve already spoken about them in other lectures. 04:46 One is ciprofloxacin and the other one is ofloxacin. 04:50 Now these are also used in drug resistance TB infections. 04:53 It’s used in combination with other anti TB drugs and it’s usually used when other drugs have failed.
About the Lecture
The lecture Other Agents to Treat Tuberculosis – Antimycobacterial Agents by Pravin Shukle, MD is from the course Antimicrobial Pharmacology.
Included Quiz Questions
What is the current term for what was previously known as "latent TB infection"?
- Tuberculosis Infection
- Active TB
- Tuberculosis Disease
- MDR-TB
- XDR-TB
What statement is FALSE regarding streptomycin?
- This medication is safe to use while pregnant.
- This medication is safe to use while breastfeeding.
- This medication can lead to renal dysfunction.
- This medication can lead to auditory toxicity.
- This is an aminoglycoside.
What statement is FALSE regarding amikacin?
- It binds the 50S subunit of the ribosome.
- It inhibits protein synthesis
- It covers aerobic gram-negative bacteria.
- It covers gram-positive bacteria.
- It may be used in the treatment of Klebsiella.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |