Playlist
Show Playlist
Hide Playlist
Osteoporosis in Women
-
Slides Osteoporosis Menopause.pdf
-
Download Lecture Overview
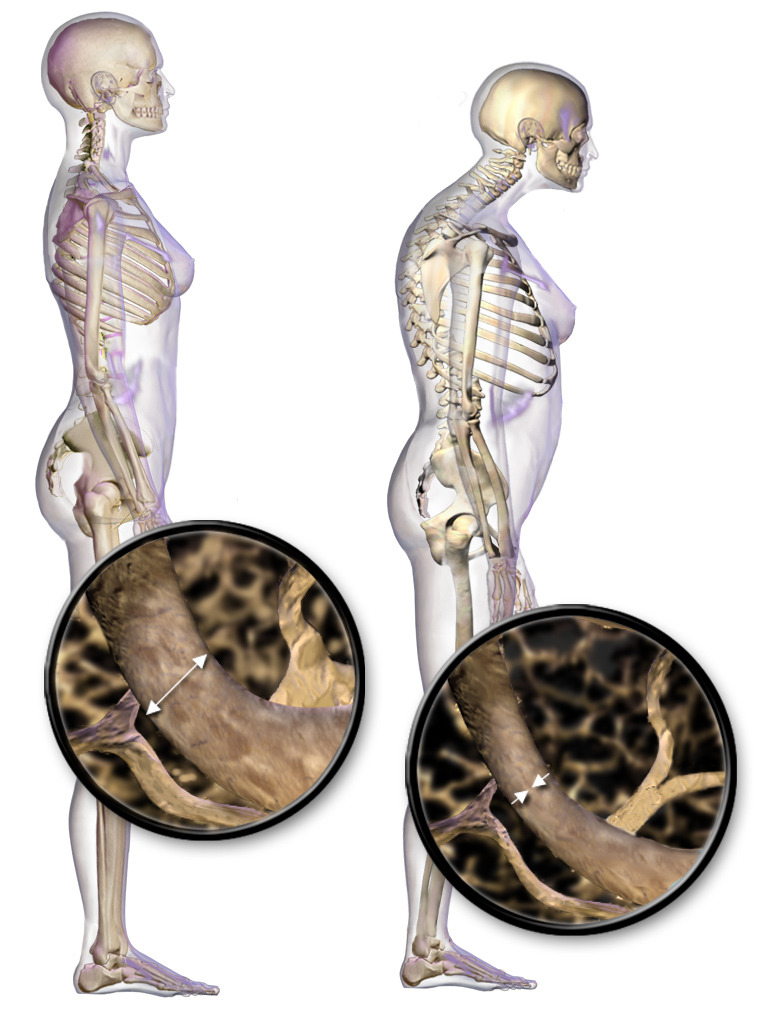
00:01 Hello, today we'll be discussing menopause, osteoporosis, and DEXA screening. 00:06 Let's first review what an osteoporotic bone looks like. 00:12 As you can tell here, the bone has increased fragility and decreased structural density. 00:20 Sometimes you can see osteoporosis present like this. 00:25 This is an elderly woman who has a Dowager's Hump which is a curvature of the spine from osteoporosis. 00:32 Osteoporosis affects many individuals worldwide approximately 44 million. 00:41 In the US, about 10 million people are affected by the disease. 00:45 34 million people have osteopenia which is the precursor for osteoporosis. 00:51 There are different etiologies for osteoporosis. 00:56 They can be pathophysiologic factors such as low estrogen or hypoestrogenism, diseases, as well as environmental factors such as diet, lifestyle, and medications. 01:11 You'll find with osteoporosis patients that they may have a poor diet that lacks calcium and vitamin D. Patients may also report having a sedentary lifestyle and certain medications such as glucocorticoids that can put them at risk for osteoporosis. There are other inherent risk factors such as age. 01:30 The incidence of this disease increases with increasing age. 01:34 Ethnicity usually you'll find this disease in women who are Caucasian or of European decent. Women who are low body weight are also in increased risk. Family history of fractures and osteoporosis also puts your patient at risk. 01:50 Now, I'd like to give you a brief overview about adolescent pregnancy and osteoporosis and how that can affect a woman in her postmenopausal stage of life. 02:00 Adolescence is a critical time of life to accumulate bone for peak bone mass. 02:05 Factors that may interfere with bone mass accrual include pregnancy during adolescence, eating disorders such as anorexia or bulimia, and poor calcium intake. So if you are seeing a young patient who's an adolescent it's important to remind them to eat well, exercise, and also prevent them from having unintended pregnancy. 02:29 Let's now talk about which you find when you have a patient who presents with potential osteoporotic fractures. 02:36 You can find they have a vertebral compression fracture, Colles' fracture, head of the femur fracture, or potentially tooth loss. 02:45 When do we actually screen patients for osteopenia and osteoporosis? The recommendations currently state that women aged 65 and older should actually be screened. However, younger women should be screened earlier than 65 if they have one or more additional risk factors. 03:06 Can you think of any risk factors? I'm gonna let you answer that. 03:12 I'll be quiet for one second. How about smoking? How about eating disorders? How about a sedentary lifestyle? All those potentially could be risk factors. 03:23 However, smoking, fitness, low BMI, and actually a family history of osteoporosis would make you screen earlier. Who should have a Bone Mineral Density Test or a DEXA? Well, anyone who's being considered for pharmacological therapy who maybe already have osteopenia. Also, anyone who's being treated for osteoporosis to monitor the effect of treatment. 03:51 We should screen anyone not receiving therapy in whom evidence of bone loss would lead to treatment. We should also screen postmenopausal women who are discontinuing hormone replacement therapy or HRT. 04:05 Let's now discuss the risk factors for osteoporotic fractures. 04:11 History of fragility fracture, a family history of fracture in a close relative like a sister or a mother, current smoking and drinking, thinness, a family history of osteoporosis, amenorrhea and hypoestrogenism or low estrogen, lifelong deficient calcium and vitamin D intake, and bone losing medications such as heparin, anticonvulsants, glucocorticoids which are also corticosteroids, thyroxine, and SSRIs.
About the Lecture
The lecture Osteoporosis in Women by Lynae Brayboy, MD is from the course Menopause.
Included Quiz Questions
At what age does screening for osteoporosis begin in women without any risk factors?
- 65 years
- 60 years
- 55 years
- 50 years
- 45 years
Which of the following is NOT a risk factor that would warrant early screening for osteoporosis in women?
- Increased intake of dietary fiber
- Low BMI
- Family history of osteoporosis
- Smoking
- Lack of exercise
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |