Playlist
Show Playlist
Hide Playlist
Obstructive Lung Diseases: Etiology and Pathology
-
Emergency Medicine Bord Obstructive Lung Disease.pdf
-
Download Lecture Overview
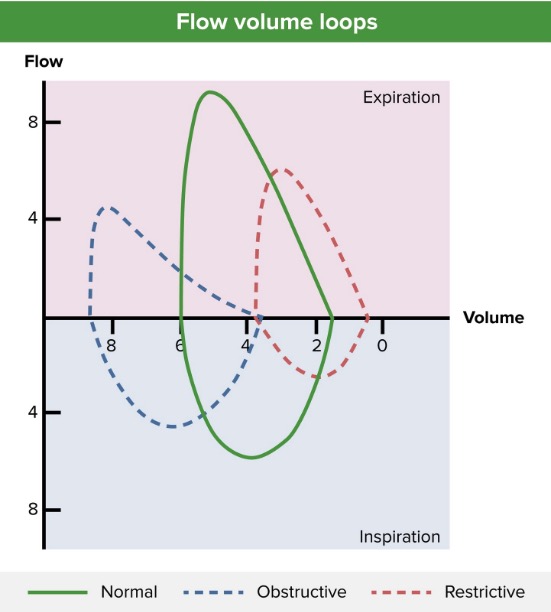
00:01 You know, thinking about COPD and asthma, COPD is primarily in older patients, and it usually develops after a long time of smoking. 00:10 You know, not always, there are definitely other things that can cause COPD, but for the most part that's the patient that you're gonna be seeing. 00:17 This is rarely a diagnosis that you make any emergency department. 00:22 This is more likely a diagnosis that the patient comes into the emergency department with. 00:26 So in those long time smoking patients, patients who are older, who come in with wheezing, you wanna think about this. 00:33 Asthma is generally something that begins at a younger age, so oftentimes asthma begins in childhood with patients who, you know, are very, very young. 00:41 Not always, but generally that's what we think about when we're thinking about asthma. 00:45 When we're thinking about the pathology behind it, what is causing these patients to have obstructive lung disease. 00:52 The underlying thing here is that the patient is unable to adequately exhale carbon dioxide, and that's the obstructive component. 00:59 So the alveoli in a lung are unable to effectively make that exchange. 01:04 Now, this is definitely more prominent in COPD, compared with asthma. 01:09 But for sure this place are rolling both of these conditions. 01:12 Whenever we're thinking about lung disease and problems with the lungs. 01:16 I always think about problems with oxygenation, and problems with ventilation. 01:21 Problems with the oxygenation are that the patient is unable to adequately oxygenate their blood. 01:26 They're not unable to inhale enough oxygen, and get that into their blood stream. 01:29 Problems with ventilation are that the patient is unable to adequately exhale their carbon dioxide. 01:35 Now, this is due to lots of pathologic concerns. 01:39 One of them is inflammation, so when the airway gets inflamed, they're not able to work effectively. 01:44 You have a big, swollen airway, you're not able gonna be able to do anything. 01:49 I also wanna highlight that we're talking here about our lower airways. 01:52 So we're talking about the airways within our lungs. 01:55 We're not talking about our upper airways, our trachea. 01:58 That generally does not have a role to play in obstructive lung disease. 02:02 So we're talking about our lower airways within our lungs. 02:05 Also, overtime there can be structural airway changes, so the lungs in a patient with COPD, are not gonna be as compliant in a patient who does not have COPD. 02:18 Mucociliary dysfunction place a role here as well. 02:21 So within our lungs we have cilia, which are these little hairs that helped us our lungs basically get rid of all the junk within them. 02:31 Get rid of all the bad stuff that we inhale, and when patients are smokers or when there COPD in place, those cilia, those little hairs aren't able to work effectively. 02:42 You also can have bronchial hyperresponsiveness. 02:45 So basically, the airways are kind of spasming, they’re not able to adequately expand and let the air in, or let the air out.
About the Lecture
The lecture Obstructive Lung Diseases: Etiology and Pathology by Sharon Bord, MD is from the course Respiratory Emergencies.
Included Quiz Questions
What is the classical cause of chronic obstructive lung disease in an elderly patient?
- Long-time history of smoking
- History of asthma
- History of pulmonary tuberculosis
- History of cardiac disease
- History of pulmonary embolism
What is the primary result of obstructive lung disease?
- Inability to adequately exhale carbon dioxide.
- Inability to adequately inhale oxygen.
- Structural airway changes.
- Bronchial hyperresponsiveness.
- Mucociliary dysfunction.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |