Playlist
Show Playlist
Hide Playlist
Migraine: Presentation & Diagnosis
-
Emergency Medicine Bord Approach Headache.pdf
-
Download Lecture Overview
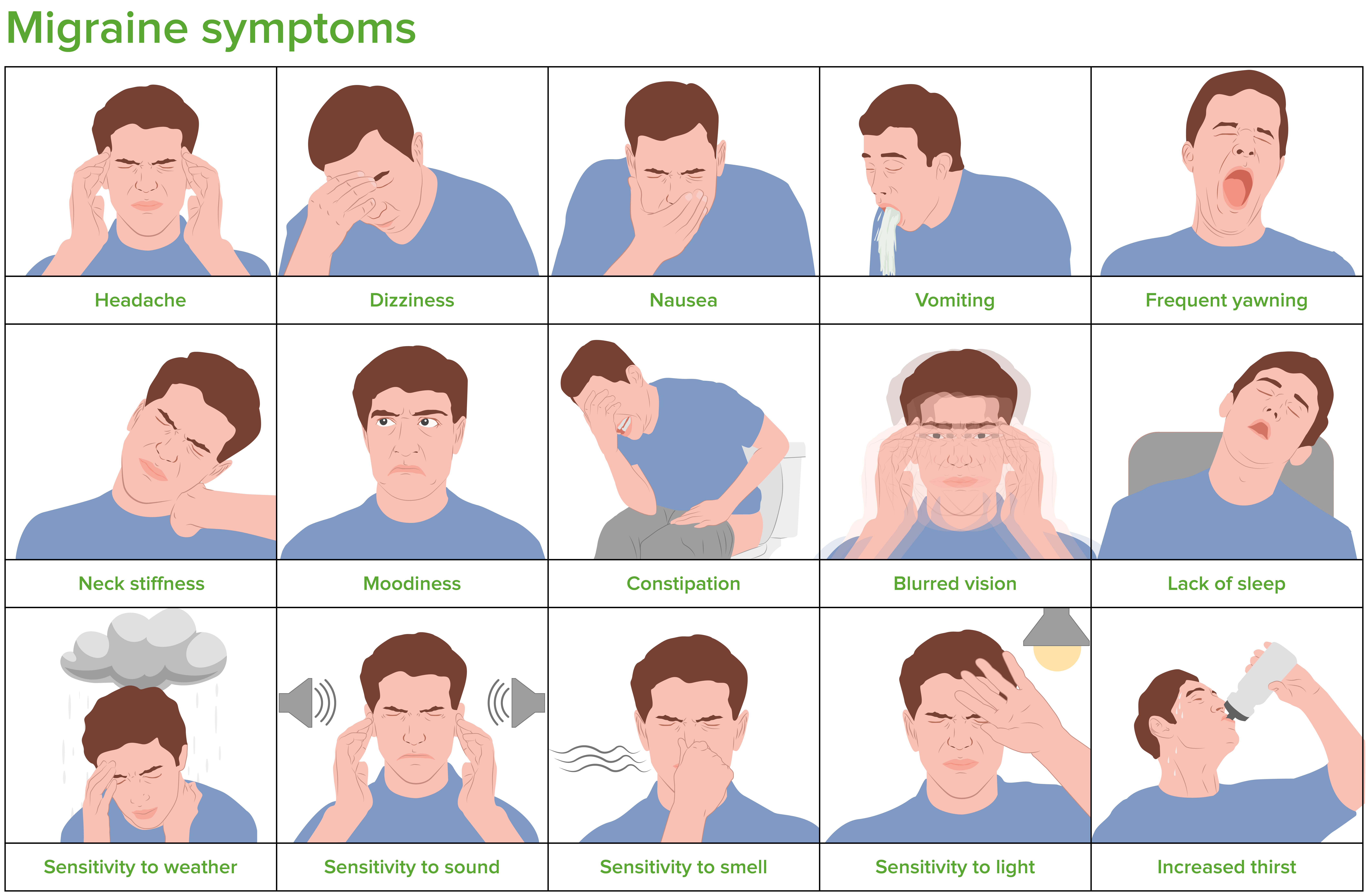
00:01 Now for patients who present with a migraine, this is a very common presenting symptom to the Emergency Department. 00:07 This is something that we see relatively frequently. 00:10 Migraines are chronic causes of headaches and can be very incapacitating to patients. 00:15 So patients who have a history of severe migraines can get very severe headaches that limit their ability to get work done, to interact. 00:24 They most commonly begin in the second decade of life and there is a genetic component. 00:28 So patients will often relate to the fact that their parents or brothers, or sisters have similar headache symptoms that they experience. 00:37 Patients with migraines can present with lots of different symptoms. 00:41 A common one is that they may have an aura associated with their headache. 00:45 And what we mean by an aura is that they may see spots prior to their headache, or they may have other sensations that they experience prior to their headaches or when their headaches are first beginning. 00:55 Patients with migraines also can present with a handful of other symptoms. 00:58 So common things that patients have are photophobia which is when bright lights will bother patients. 01:04 The classic thing that you sometimes may see is patients who present with migraine headaches may come into the Emergency Department wearing sunglasses, even though it’s kind of dark outside. 01:13 So at night, that’s a classic sign of patients who have migraine headaches. 01:18 Phonophobia is when loud noises might bother patients as well as nausea and vomiting may be associated with migraine headaches. 01:25 In extreme cases, patients may also present with neurologic abnormalities with their migraine headaches, such as dizziness and actually patients may experience weakness as well and really might mimic very closely a stroke. 01:39 So sometimes when this patients present with those symptoms especially if they don’t have a headache, history of migraine headaches. 01:46 You definitely can sometimes be a little bit confused or trying to sort out whether or not this is a migraine, or more serious neurologic problem. 01:55 So what should we do for these patients? So for some patients you may need to get some neuroimaging. 02:02 So you might need to get a head CT for patients who have a new headache. 02:05 So they say that I've never had a headache like this before. 02:08 For patients who are immunocompromised. 02:11 Patients who are on medications that might suppressed there immune system or patients who have underlying diseases that can make them be immunocompromised, the classic one being HIV or AIDS. 02:23 Any kind of neurologic abnormalities such as weakness, numbness, tingling, problems with their ambulation, potentially problems with speech might prompt you to get neuroimaging. 02:35 And then sudden onset of headache is the other thing that might make you more concerned or point you in that direction. 02:41 You know, if your patient has a prior history of similar symptoms, then they come in and they say this feels very similar to my migraine that I’ve had before, that definitely kind of puts you out or points you in that direction that this is in fact most likely a migraine headache.
About the Lecture
The lecture Migraine: Presentation & Diagnosis by Sharon Bord, MD is from the course Neurologic and Psychiatric Emergencies.
Included Quiz Questions
Which of the following is NOT a true statement about a migraine headache?
- It can frequently present as a sudden onset of the worst headache the patient has ever experienced.
- It is a very common chief complaint seen in the emergency department.
- It can be incapacitating to the patient.
- It can have a genetic component.
- The patient may or may not experience an aura before the headache.
Neuroimaging would be most likely to be requested in which of the following situations?
- An immunocompromised patient
- A patient with controlled diabetes mellitus
- A patient with a prior history of similar headaches
- A patient who complains of having a mild headache during all of final exam week
- A patient with chronic sinusitis
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |