Playlist
Show Playlist
Hide Playlist
Lymphatics Anatomy and Physiology
-
Slides Lymphatic Model Treatment Approach and Techniques.pdf
-
Reference List Osteopathic Manipulative Medicine.pdf
-
Download Lecture Overview
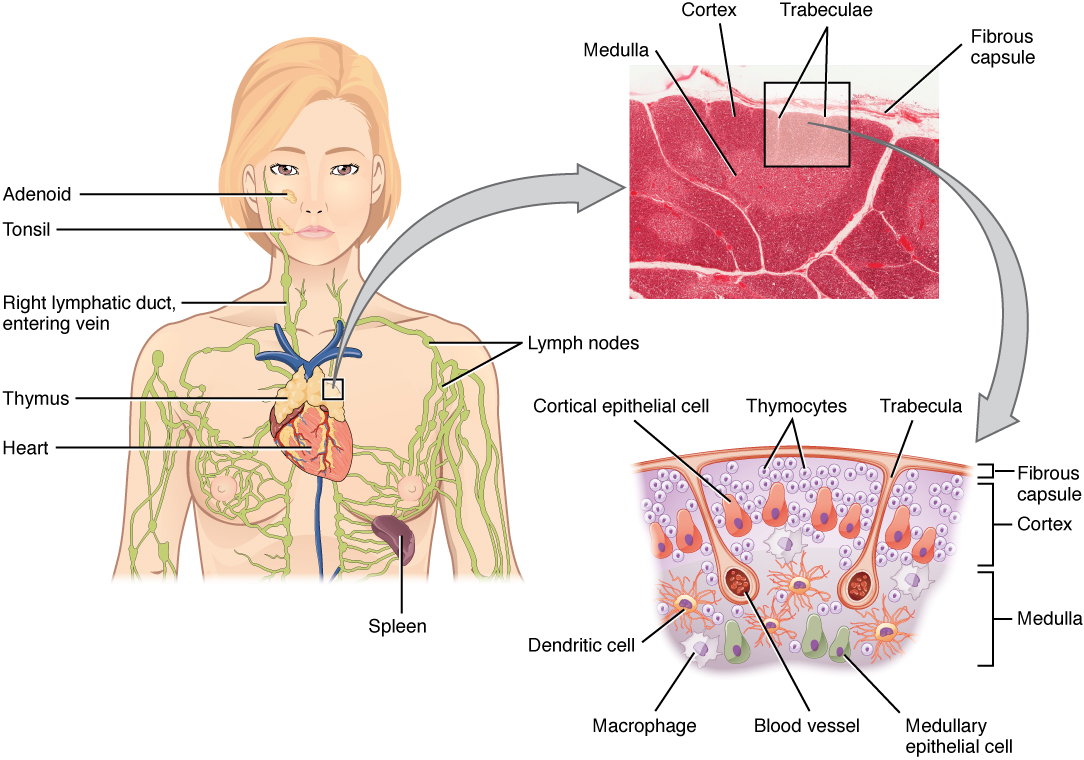
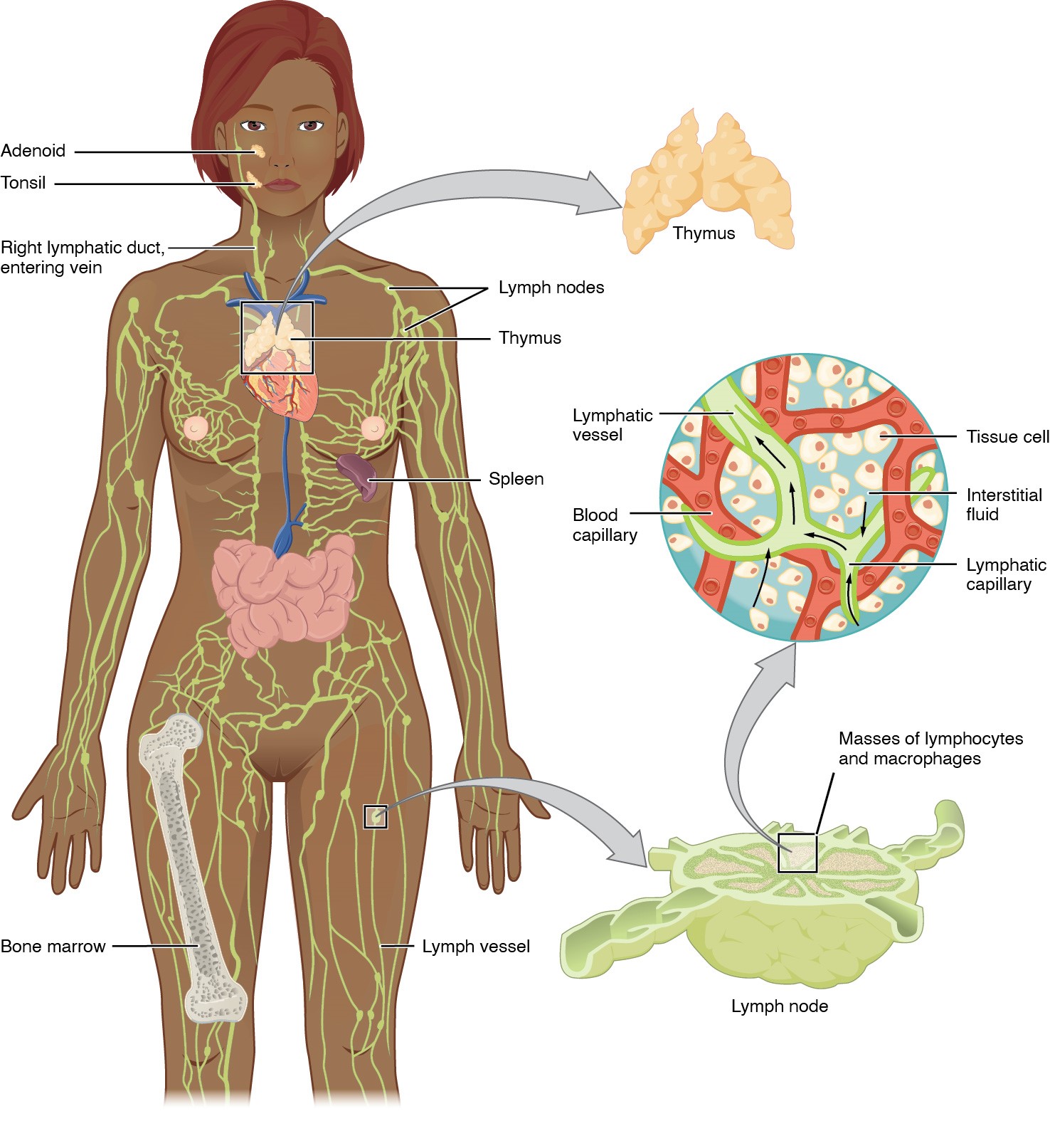
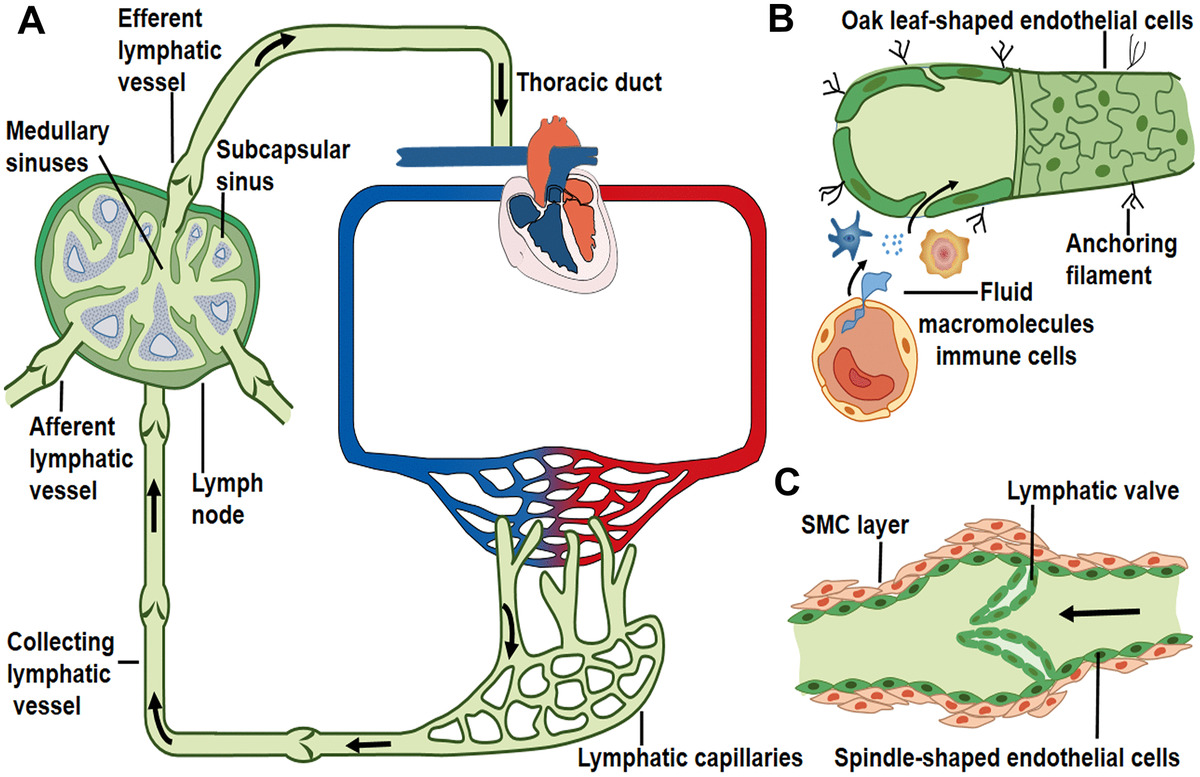
00:00 Our lymphatic system is vital to our survival. Our lymphatic system plays a major role in our body. Our lymphatics help with balancing the interstitial fluid, transporting waste, distributing immune cells, filtering foreign material and absorbing nutrients especially from our GI tract. 00:23 Lymphoid tissue starts at 5 weeks of fetal age. At birth, lymphoid tissue is still immature And about the age of 15 to 16 that lymphoid tissue reaches adult levels. Primary lymphoid tissue could be found in the thymus and also in the bone marrow. We have secondary lymphoid tissue that could be found in the tonsils, the spleen, our GI tract, our appendix and our lymph nodes. Our lymph nodes is a system of nodes that are connected by the lymphatic ducts and the lymphatic system and these lymph nodes interact to help filter our blood and protect against foreign material and also cancer cells. They are superficial and deep nodes and this collection of cells work in a network with the connective tissue. Our lymph flows through lymph channels. These channels start in the soft tissue as closed endothelial line capillaries. They are single layer squamous cells and they are supported by anchoring filaments into the interstitial matrix. This is important to consider because it is these anchoring filaments connect into the cells that help to hold open the gaps between individual cells to allow for lymph to come in and for lymph formation. These small tubes join to form larger lymph channels. In the larger vessels, these have more of a traditional intima-media and valves. There is some smooth muscle control that helps to propel the lymphatics and that is innervated by the sympathetic nervous system then these larger vessels communicate with the circulatory system through nodes and through lymph ducts. Lymph vessels could be found almost through all tissues of the body. The exceptions include the epidermis including the hair and nails, the bone marrow, the endomysium of muscles and cartilage and portions of the peripheral nerves. It was once thought that there were no lymph vessels in the CNS and brain, but the lymphatic system was recently found to run along the venous sinuses. Drainage of the lymphatic channels of the abdomen, pelvis and lower limbs all drain into the cisterna chyli. The cisterna chyli is a dilation of the thoracic duct to the right side of L1/L2 and it lies right behind the right crus of the diaphragm next to the abdominal aorta. This is important because that dilation actually helps to get pumped whenever we breathe and pulsations of the aorta help to propel fluid through the thoracic duct at that dilation. It is really important to understand how lymphatics drain throughout the body and run especially when we are trying to address any somatic dysfunctions that may impede lymphatic flow. Most of the body drains through the left thoracic duct. The left side of the head and neck, the left arm and thorax, the left and right portions of the lower bodies of both lower extremities, the thoracic and abdominal viscera all drain into that thoracic duct. The right side gets the right side of the head and neck, the right side of the chest including parts of the heart and lung on the right. Understanding what regions and organs drain to the right and left side of the body is important because you will then address key structural issues based on what area you are trying to promote lymphatic drainage. The right lymphatic duct will drain into the right subclavian vein whereas the thoracic duct usually will drain into the left subclavian vein, but first it pierces the fascia covering the thoracic outlet so it is important to address any sort of somatic dysfunction or restrictions in that region to allow for proper flow. So, let us take a closer look at the formation of lymph. Interstitial fluid is an ultrafiltrate of blood. The production of interstitial fluid is the filtration out of the capillaries versus reabsorption. Lymph vessels could collect interstitial fluid and it's about 2 to 3 liters per day. About 100 grams per day of protein could escape from blood capillaries and then the interstitial fluid also receives metabolic waste. So, taking a look at pressures that drive fluid out of the arterial and include hydrostatic pressure and then on the venous end, plasma and colloidal osmotic pressure helps to draw fluid back in and in between there is an exchange of fluid between the interstitial fluid and the lymph and our circulatory system. So interstitial fluid itself could be intracellular and extracellular. 05:41 Intracellular fluid is about 40% of the weight, extracellular is about 20% with interstitial lymph actually being 15% and plasma itself being about 5%. There are a lot of factors that affect the flow of lymphatics. It is important to understand these factors to better understand how to address lymphatic issues and problems. So any sort of increase in the interstitial fluid pressure will increase the absorption of lymph into lymph capillaries up to a certain pressure. So normally interstitial fluid has a normal resting negative pressure of -6.3. Now, as I slowly rise it so if I start to get a little bit of swelling and it becomes more positive it would open up the small capillary filaments to increase the amount of lymph flow into the lymphatic system. So once I reached pretty much a pressure of zero, lymphatic flow could be increased up to 20 times but once I increased the interstitial fluid pressure greater than zero what happens is it now collapses those channels and prevents any sort of flow into the lymph channels. So again, interstitial fluid normally is negative and as it slowly gets towards positive it will increase the amount of fluid being absorbed into the lymph channels but once the pressure goes above zero meaning the pressure becomes positive those channels collapse and it does not allow for any sort of lymph to get into the lymph channels. The actual flow of lymph could be influenced by many different things. Intrinsically, the lymph vessels itself will contract when dilated so if there is distention of the lymph fibers it is going to cause it to contract. The smooth muscle and the lymphatic channels itself could also cause contraction and propel lymph through the lymph vessels. The lymphatic channels thta are in our lymphatic system does not have a specific pump like our circulatory system has the heart to pump fluid throughout the system. Instead, our lymphatic system really depends a lot on extrinsic factors to get lymphatics to move and so the extrinsic factors that affect lymph flow include the diaphragm. So whenever the diaphragm moves we talked about the placement of the cisterna chyli which is the dilation along the thoracic duct collecting all the lymph from our GI tract, our internal organs, our legs so whenever the diaphragm moves with inhalation-exhalation they will actually physically help to pump the cisterna chyli because the cisterna chyli lies right posterior to that right crus of the diaphragm. 08:31 Whenever we take a deep breathe in that creates a negative pressure in the chest and abdomen and then when we exhale it becomes a positive pressure. So whenever we breathe, the motion the diaphragm helps to contribute to pressure changes in the thoracic cage. That pressure change actually helps to draw lymphatics into the thoracic cage. So when I inhale and take a deep breath in and create a negative pressure more lymphatics is drawn into thoracic cage and when I exhale that change in pressure helps to propel it along. So when you think about it, we breathe about 12 breaths a minute that is almost 17,000 pressure changes a day whenever we are breathing. Abdominal peristalsis also helps to move along lymph so whenever our abdomen contracts that is going to help move lymphatics. Our lymphatic vessels tend to run within the fascia surrounding muscle so every time we contract our muscles that also helps to propel lymphatics. It has actually been studied vigorous exercise could actually increase lymphatic flow 15 to 20 times compared to normal resting flow. Our lymphatic vessels typically run side by side to arteries. This is to help with improving flow due to the pulsations of the arteries. So when the arteries pulse, that motion and movement also helps to affect the flow of lymphatics.
About the Lecture
The lecture Lymphatics Anatomy and Physiology by Sheldon C. Yao, DO is from the course Osteopathic Treatment and Clinical Application by System.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
great clear synopsis of a very complex topic. Easy to memorize