Playlist
Show Playlist
Hide Playlist
Ischemia-reperfusion Injury
-
Slides Cellular Pathology Mechanisms of Injury.pdf.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
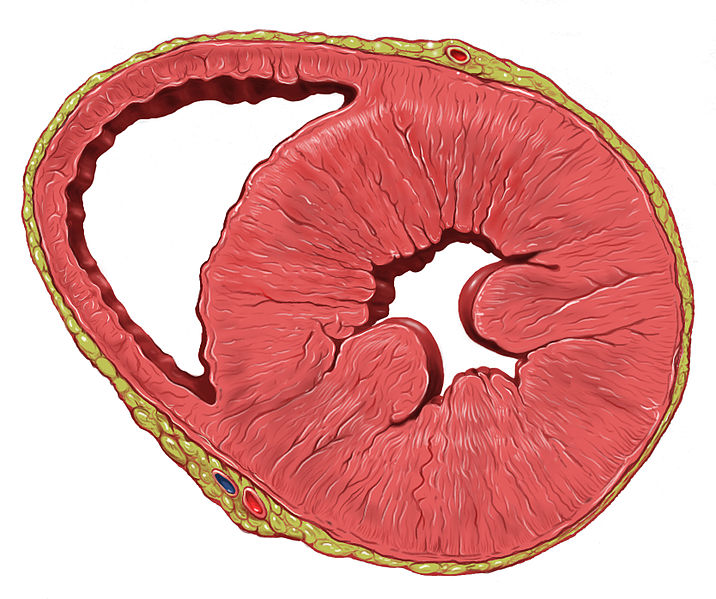
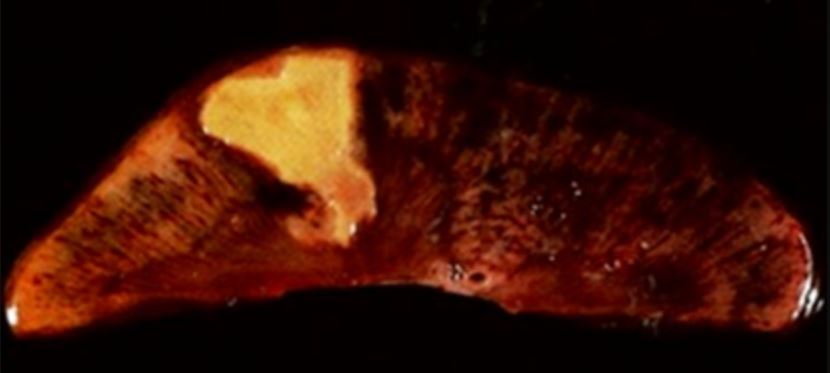
00:02 One last topic in this topic, of kind of cell injury and mechanisms there of is Ischemia and Reperfusion. 00:11 So, in the typical clinical setting where this occurs, a patient comes in there having crushing substernal chest pain. 00:18 They're having a heart attack. 00:20 We know that most commonly this is due to a plaque rupture in the coronary artery with a blood clot on top of it. 00:27 So we rushed them into the angiography suite, and we inject tissue plasminogen activator, a clot buster, and we break up the clot. 00:35 Except that the heart has been ischemic for a certain period of time. 00:39 Now we're restoring blood flow into tissues that have had partial injury. 00:45 So when that happens, we have a high concentration of extra cellular calcium that's coming into a potentially compromise cell. 00:54 We already talked about cells. 00:56 If they see a spike of calcium, we'll start down that calpain activation pathway, and we'll end up with some cell death. 01:03 So that's one part of ischemia reperfusion. 01:07 When we reperfuse ischemic tissue, we also get increased recruitment of inflammatory cells. 01:13 And recall the inflammatory cells have a rich resource of for generating reactive oxygen species. 01:21 So as a result of that, we will get more damage because we recruit more inflammatory cells into this area of reperfusion. 01:30 The damage mitochondria in that tissue. 01:32 So the mitochondria been scheming for a certain period of time to, and they are not firing on all cylinders. 01:38 They are not working as well as they should. 01:41 The electron transport chain is not quite up to par yet, and so as a result, those damaged but still working mitochondria will pump out more of the reactive oxygen species because they're getting incomplete oxygen reduction down the electron transport chain. 01:59 It turns out that injured endothelium in a hypoxic or ischemic tissue will lead to the not specific deposition of certain forms of antibodies that will lead to complement activation, so there will be damaged there too. 02:12 So ischemia, and then reperfusion, even when it's saving the life of the patient can have secondary consequences in terms of injury to the tissue. 02:24 That's important to understand, because there is clearly a therapeutic intervention that we need to do. 02:31 We want to save patients lives, so we will do the reperfusion. 02:36 But we don't want to have any more damage. 02:38 So, we all, you and I need to be more clever about preventing that reperfusion damage. 02:46 And with that, we've covered the biochemical mechanisms by which cells get injured.
About the Lecture
The lecture Ischemia-reperfusion Injury by Richard Mitchell, MD, PhD is from the course Cellular Injury.
Included Quiz Questions
Which of the following contributes to the formation of reactive oxygen species in reperfusion injury? Select all that apply.
- Increased recruitment of inflammatory cells
- Decreased extracellular calcium concentration
- Decreased activity of the Golgi apparatus
- Increased intracellular proton concentration
- Damaged mitochondria release free radicals
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
1 customer review without text
1 user review without text