Playlist
Show Playlist
Hide Playlist
Inflammatory Vascular Diseases: Classification
-
Slides Inflammatory Vascular Diseases.pdf
-
Reference List Vascular Medicine.pdf
-
Download Lecture Overview
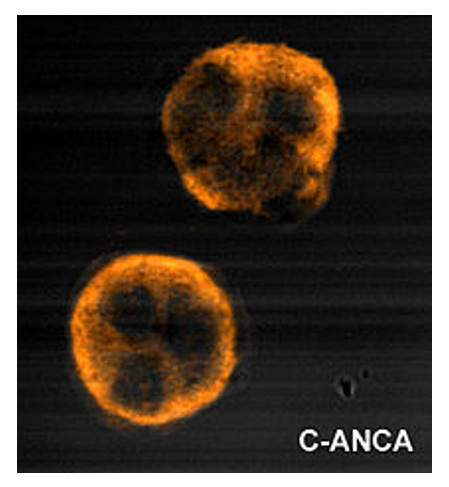
00:00 So here is an overall classification of vasculitis. 00:06 You'll notice that there are primary vasculitis syndromes and there are secondary vasculitis syndromes, we're not going to talk in this presentation about the secondary ones because they've already been discussed under various diseases. 00:25 So, for example, lupus erythematosus often has vasculitis and there's a discussion under that entity of the vasculitis, rheumatoid arthritis and and the sarcoidosis. 00:38 Similarly also can result in vasculitis. 00:43 And again, under those entities, you will see discussions on the vasculitis and then sometimes they're not uncommon. 00:50 As drug induced vasculitis, hepatitis B or C can be associated with vasculitis. 00:57 Some forms of cancer can be associated with vasculitis, and he knocks line purpura as well. 01:04 So those are all separate entities discussed in a separate lecture by Lecturio. 01:12 We're going to talk about the primary forms of vasculitis. 01:19 It comes in three forms small vessels, medium size vessels and medium to large sized vessels, and we'll start with the small vessel vasculitis syndromes. 01:32 So. Let's take the first one, this one, so-called granulomatosis with polyangiitis that means multiple vessels with granulomas in them used to be called Wegner's. 01:46 It was named after a physician, Wegner, who turned out to have done some rather immoral things. 01:53 And so his name has been stricken from this syndrome. 01:56 It's now called granulomatosis with polyangiitis. 02:01 It's this granulomatous inflammation of small vessels, as we said. 02:06 The mean age of onset is around 40 years. 02:09 It affects the upper airways, often is diagnosed initially as sinusitis and patients are treated with antibiotics and the lungs are involved in a high percentage of cases. 02:22 And there can be infiltration of the lungs with nodules and hemoptysis. 02:26 75% also involve the kidneys with with an immune form of glomerulonephritis. 02:34 It can also involve multiple other organs, the eyes, skin, joints and so forth. 02:39 And sometimes a rash that gets biopsied is a clue to what's going on. 02:45 The diagnosis, again, is from biopsy, often in the sinus or the nasal passages, and the biopsy shows granuloma granulomas or we're in the vascular inflammation. 02:59 There's also a positive blood test the so-called anchor, the anti-proteinase three anchor test that can be positive and other vasculitis. 03:08 But here it's very specific for granulomatosis with polyangiitis. 03:14 And the treatment, as I mentioned already, is anti-inflammatory, and that is with glucocorticoids, cortisone like drugs, cyclophosphamide and even more powerful immunosuppressive. 03:28 If they don't respond, the patient doesn't respond to the initial steroid treatment. 03:35 The next syndrome is so-called Churg-Strauss syndrome, also known as granulomatosis with polyangiitis. 03:46 except that there is an additional term added on eosinophilic. 03:50 That is. 03:51 So it's the same term as with the previous one granulomatosis with polyangiitis. 03:57 But eosinophils are a prominent component of this entity so that there is both peripheral eosinophilia and they can also be seen in the vascular inflammation. 04:11 The mean age is about 50 years. 04:14 Often, these patients present with pulmonary issues, severe asthma and infiltrates are seen on chest X-ray. 04:22 There can be involvement of the nerves so-called mononeuritis multiplex. 04:28 That is, individual nerves may suddenly develop neuritis and abnormal function, for example, abnormal sensation or motor function. 04:39 There is often an allergic rhinitis or sinusitis, so that's why this can be confused with the previous entity with granulomatosis with polyangiitis and they can even have a positive ANCA test. 04:53 But in this case, it's nonspecific. 04:55 And again, the diagnosis is made by biopsy. 04:59 By the way, this entity can affect the heart and can even lead to fatal arrhythmias. 05:04 So this is a very nasty disease. 05:07 And again, the treatment is with glucocorticoid, cyclophosphamide or other immunosuppressive glucocorticoids. 05:14 I don't do it. 05:17 The next syndrome, also still small vessel syndrome is microscopic polyangiitis. 05:24 This one predominantly affects the kidneys and the lungs and often is associated with hemoptysis. 05:32 So him assist with glomerulonephritis and decreasing kidney function. 05:39 The diagnosis is very often microscopic polyangiitis. 05:44 There can also be elements like in Churg-Strauss with mononeuritis multiplex and, of course, skin rashes. 05:51 The diagnosis, again by tissue biopsy, the ANCA test can be positive but is nonspecific. 05:58 And again, the treatment is done with glucocorticoids and cyclophosphamide and more potent immunosuppressive if the glucocorticoids and cyclophosphamide don't work.
About the Lecture
The lecture Inflammatory Vascular Diseases: Classification by Joseph Alpert, MD is from the course Inflammatory Vascular Diseases.
Included Quiz Questions
One classification of the various forms of vasculitis involves which of the following characteristics? Identify the CORRECT characteristic.
- By vessel size.
- By the shape of the vessel.
- By the quantity of blood flow carried by the vessel.
- By quality of the vessel's endothelium.
What is a secondary vasculitis?
- Sarcoidosis
- Churg-Strauss syndrome
- Microscopic polyangiitis
- Kawasaki disease
- Giant cell arteritis
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |