Playlist
Show Playlist
Hide Playlist
Inflammatory Myopathies: Types, Diagnosis, Manifestations, Treatment
-
Slides Inflammatory Myopathies.pdf
-
Reference List Rheumatology.pdf
-
Download Lecture Overview
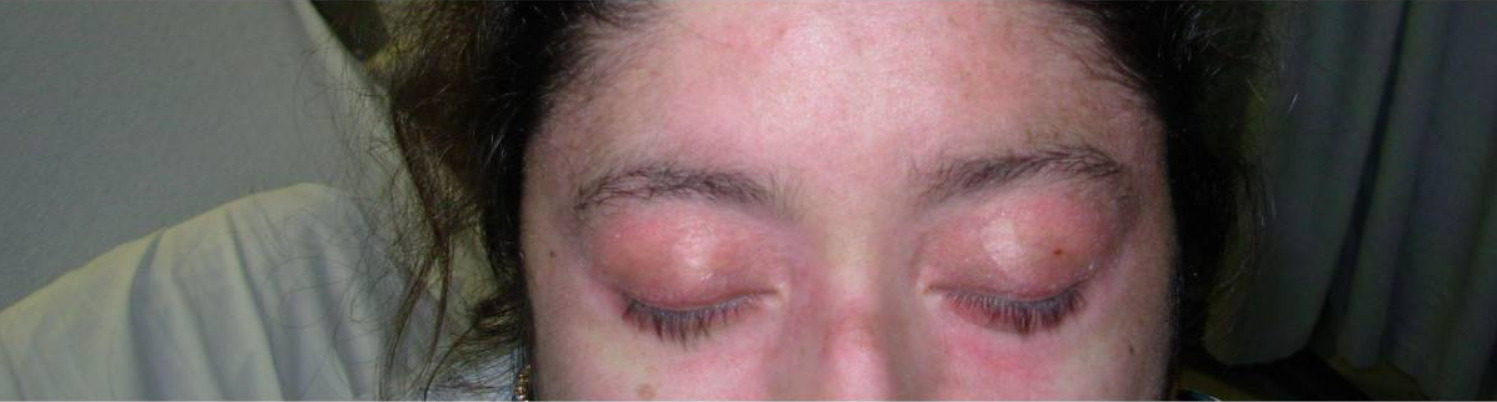
00:01 So before we go back to review some key-features of our case, let's just compare and contrast the three different inflammatory myopathies. 00:07 There are few things that are common to all of them; they're all gonna have some degree of lymphocytic infliltration and disruption and degeneration of normal myofiber architecture. 00:17 Looking at polymyositis in particular it can be acute or subacute and onset as it was in our patient. 00:24 You're gonna see symmetric findings, proximal muscles are involved. 00:28 And it's typically gonna occur in patients over the age of 50. 00:31 Importantly there's kind of a variable treatment response but you'll hope that you'll have a good prognosis. 00:37 Dermatomyositis is essentially the same thing as polymyositis. 00:42 In fact, there's been a lot of debate in the nomenclature about these two conditions. 00:45 The big difference however is of course the presence of dermatologic manifestations in which we've gone through a number of them. Otherwise, the same bullet points are listed below. 00:55 The big splitting off point is inclusion body myositis. This is a very different condition. 01:01 It has an indolent onset potentially over many years, asymmetric findings and a mixed picture of proximal and distal muscle weakness. 01:11 Often times the patient will report difficulty with hand strength in addition to having asymmetric weakness of the left lower extremity. 01:19 These folks have an earlier age of onset potentially in the 30's and this condition is notorious for having a poor treatment response. 01:27 Okay, with that let's bring it back home to our case to review some key points. 01:33 Again, in terms of dermatomyositis the age is typical. 01:37 The subacute course over three to four months is also typical of polymyositis rather than inclusion body myositis. 01:44 We've highlighted the proximal muscle weakness issues; both of the upper and lower extremities and the absence of hand weakness is stirring us away from inclusion body myositis. 01:53 The absence of systemic symptoms supports this as well. 01:57 Importantly the absence of systemic features is gonna stir us clear of a mixed connective tissue disease. 02:03 We'll talk about how important it is to look for mixed connective tissue disease when you see inflammatory myositis in just a moment. 02:10 Reviewing the physical exam again, they commented on these scaling hyperkeratotic erythema on the ulnar surface of the thumb. And again, that's basically symptoms in this area here. 02:21 It's often times called mechanics hands because you can imagine that somebody works a lot with their hands, handling tools, could get this kind of scaling erythema and hyperkeratosis like calluses in that part of the hand. 02:33 But that is just one of many characteristic features of dermatomyositis. 02:36 In addition we already talked about what's called the gottron's papules which are those erythematous papules on the dorsum of the fingers, between the joints, also the V-neck sign, and also the shawl sign which is a similar hyper erythematous plaques that can on be the back of the neck. 02:55 Other things you might find are also heliotropic rash with erythema around the eyes. 03:00 Alright, so common manifestations of inflammatory myopathies. 03:04 Now that we've told them what the diagnosis is, we have to review some other complications that he might expect over time. 03:11 First stop, interstitial lung disease. 03:13 I've already highlighted that patients with antisynthetase syndrome in particular are at a higher risk of developing interstitial disease and this can potentially be a devastating diagnosis. 03:23 Otherwise look for dysphagia, this is indicative of weakness of the oralpharyngeal musculature, polyarthritis. 03:31 And again, I might have mention of this before, there's this concept of overlap syndromes and mixed connective tissue diseases. 03:38 You know, in medicine there's a lot of diseases that occur in families and this is an example of one of those. 03:43 When you see an inflammatory myositis, you also want to look for Raynaud's phenomenon, rheumatoid arthritis, lupus, systemic sclerosis, and Sjogren's syndrome either within the patient or in their family tree. 03:55 Malignities happen showing to be somewhat higher in frequency particularly for polymyositis though not anyone disease or type of cancer in particular. 04:06 And lastly, Myocarditis. 04:08 We are talking about muscles of course and the heart muscle is no exception. 04:12 In terms of treatment we definitely wanna look for cancers and make sure our cancer screening is up to date especially for those patients with dermatomyositis. 04:20 We're gonna use glucocorticoids. Pretty high doses of glucocorticoids for a decent length of time. 04:26 Often times we have to treat for up to a year or more while starting steroid sparing disease modifying agents like methotrexate, azathioprine, and mycophenalate mofetil. 04:37 For severe disease, you can consider the use of IVIG or IV rituximab. 04:42 Alright, so let's highlight a few key points of inflammatory myopathies. 04:46 Number one, variable onset of proximal weakness. More so even than having pain. 04:52 There is an association with interstitial lung disease and with certain types of cancer and of course there's a number of skin findings that you'll see with dermatomyositis. 05:01 The anti-synthetase antibodies and anti-synthetase syndrome most often diagnosed by looking for an anti-Jo-1 antibody is an important prognostic feature. 05:11 All of the different inflammatory myopathies are gonna be characterized by a biopsy showing lymphocytic infiltration and inclusion bodies if you're looking for inclusion body myositis. 05:21 And lastly, you're gonna treat with high dose steroids and ultimately adding on some DMARDs.
About the Lecture
The lecture Inflammatory Myopathies: Types, Diagnosis, Manifestations, Treatment by Stephen Holt, MD, MS is from the course Connective Tissue Diseases.
Included Quiz Questions
Which of the following is characteristic of dermatomyositis?
- Violaceous papules over the dorsal surfaces of the metacarpophalangeal and interphalangeal joints
- Asymmetric muscle weakness
- Distal muscle weakness
- Silver, scaly papules over the knees
- Fatigue and weight gain
Which of the following is NOT found in inflammatory myopathies?
- Obstructive lung disease
- Muscle weakness
- Skin rash
- Swallowing difficulty
- Joint pain
What would a muscle biopsy from a patient with polymyositis show?
- Lymphocytic infiltration
- Neutrophilic infiltration
- Myofiber necrosis and regeneration
- Absence of dystrophin protein
- Normal-appearing muscle tissue
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Reumathology is a very difficult matter. Profesor Holt explain it very well and make it esay. Thank you so much