Playlist
Show Playlist
Hide Playlist
Infective Endocarditis (IE)
-
Slides Endocarditis Myocarditis and Pericarditis Cardiomyopathy.pdf
-
Reference List Pediatric Nursing.pdf
-
Download Lecture Overview
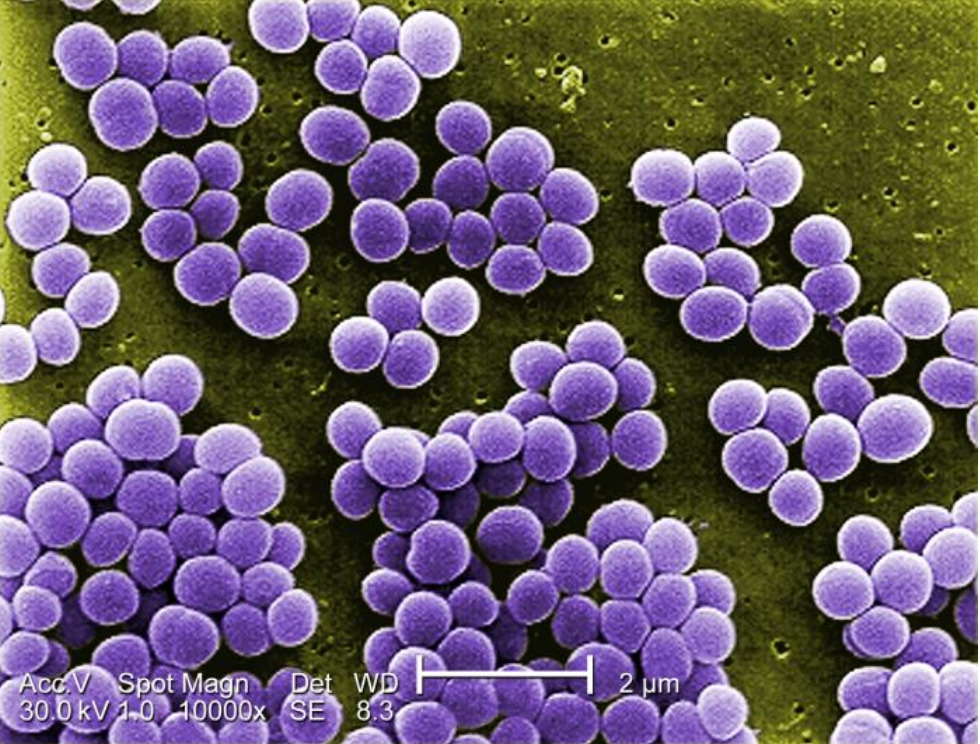
00:00 In this lecture, we're going to focus on acquired conditions of the heart. 00:05 Specifically, we're going to look at endocarditis, myocarditis, causes of cardiomyopathy, and also pericarditis. 00:15 Let's start with infective endocarditis. 00:20 Infective endocarditis is quite rare in children. 00:23 It's more common in infants who've had catheters, or in adolescents who were using IV drugs. 00:30 But we see it rarely, maybe 1 in 300,000 people. 00:33 But despite of it being rare, it is dangerous and it does confer about an 11 percent mortality rate in children. 00:42 The incidence in the United States in children is increasing likely through more children going through NICUs and through increased use of IV drugs. 00:54 Let's look at the bacteria that are most likely to cause endocarditis and specifically focus on how the bacteria relate to the presentation of the patient. 01:05 One of the most common causes of bacteria causing endocarditis in children is Staphylococcus aureus - we'll call it "Staph aureus". 01:13 Staph aureus is a very aggressive ogranism. 01:16 It can cause acutely very ill children and can also cause abscess formation within the context of the inside of the heart. 01:24 Coagulase-negative Staph is more subacute - results in chronic fevers. 01:32 Alpha-hemolytic Strep can also cause endocarditis - and again, that's more a subacute condition with chronic fevers. 01:40 Gram-negative rods can rarely cause endocarditis. 01:44 Those patients will have subacute illness and chronic fevers, but also may be more likely to develop embolic disease, clots forming as the blood flicks out of the heart. 01:55 Fungal endocarditis is very severe and these infants will present usually with very acute illness and they have a very high mortality rate. 02:06 When you're seeing a patient with endocarditis, there would be a few key points to their history. 02:14 Often, they will have diffused myalgias. 02:16 They may have fatigue. 02:20 They'll have arthralgias or sore joints. 02:23 But key is they'll have fever, and this is in you differential for a child with fever of unknown origin. 02:31 On exam, there are many key findings that are pretty high-yield or likely to show up on an exam. 02:39 They may have a toxic appearance. 02:41 They may have a new onset heart murmur, though they don't have to. 02:45 You'll notice neurologic symptoms if they have a left-sided endocarditis, which is common among endocarditis, and those bacteria could be flicking off systematically and getting into the brain resulting in abnormal mentation, stroke, brain abscesses, meningitis. 03:07 You may see Osler nodes on their exam - and we'll talk about what those are in a second - you may see Janeway lesions, and you may see splinter hemorrhages. 03:18 And last, you may see Roth spots. 03:21 I'm going to go through these four physical exam findings carefully. 03:26 First, Osler nodes. Osler nodes are found usually on the extremities. 03:31 They are small, tender, raised nodules. 03:35 They're usually on the pads of the fingers and toes. These are rare. 03:41 I have personally never seen an Osler node, but they love asking about them on test questions. 03:47 Janeway lesions are also rare. These are flat, red lesions. 03:53 They're found on the palms and soles. 03:55 In this patient on this slide, you can see them right there on their fingers. 03:59 These are painless unlike the Osler nodes, which are a little bit tender. 04:04 Also, these patients may have splinter hemorrhages on their nails. 04:09 Last is Roth spots. These are on the ophthalmologic exam. 04:13 On fundoscopy, you can see these little lesions in there that are in the retina. 04:19 These are retinal hemorrhages as a result of clots landing in the retinal artery in that capillary bed. 04:27 You'll notice, especially with the one with the white arrow, that there's a pale center, and that's what's key in a Roth spot. 04:36 If you see something in a patient regarding their history or their physical exam and you suspect endocarditis, what's key is a large volume blood culture. 04:46 This is a blood culture of between 5 and 15 milliliters of blood. 04:51 It's a huge amount of blood obtained for blood culture. 04:55 Small volume blood cultures are suboptimal. 04:59 These large volume blood cultures will be positive in more than 90 percent of cases. 05:04 Often, if we suspect it, we may obtain multiple large volume blood cultures on subsequent days to make the diagnosis. 05:13 A cardiac echo is indicated to look for a lesion that may be growing on one of those valves. 05:20 But remember, false positives and false negatives on endocarditis on the echo are common. 05:27 Frequently, the echo will be normal in a patient with endocarditis. 05:34 How do we treat endocarditis? Antibiotics are key. 05:38 Generally, you're going to treat the organism that grows on the culture. 05:42 If you strongly suspect endocarditis but don't have the identity of the organism, remember that everyday this child has bacteria growing on his or her valve is a day of valvular destruction, which can result in great pathology down the road. 06:00 So initial therapy should be broad coverage and aggressive. 06:06 We'll often give this children vancomycin and ceftriaxone, and maybe add in amphotericin if we suspect a fungal agent, especially in the critically ill children. 06:18 The therapy is going to be prolonged and will usually require a PICC line placement and a very prolonged six to eight weeks of IV antibiotics. 06:28 In patients who have a history of endocarditis, we may put them on prophylaxis. 06:35 If they have a history of endocarditis, they'll be on antibiotics every day to prevent a reinfection. 06:40 They may also need prophylaxis of the prosthetic valves, or if they are a heart transplant.
About the Lecture
The lecture Infective Endocarditis (IE) by Brian Alverson, MD is from the course Pediatric Cardiology. It contains the following chapters:
- Pathology
- Clinical Presentation
- Diagnosis & Management
Included Quiz Questions
Roth spots are identified on physical exam by which of the following findings?
- Retinal hemorrhage with pale center.
- Swelling of the optic nerve.
- Painless splinter hemorrhages on the extremities.
- Small tender raised nodules on the fingers.
- Purpura on the trunk.
A 13-year-old boy comes to you with clinical features of Infective endocarditis. After drawing blood for large volume blood culture, an immediate echocardiogram was done which revealed abscess formation in the Tricuspid valve. Which of the following is the most likely organism?
- Staphylococcus aureus
- Streptococcus pneumoniae
- Hemophilus influenzae
- Streptococcus pyogenes
- Gram-negative rod
A 15-year-old with suspected infective endocarditis is planned to be started on empiric antibiotics while waiting for the blood culture reports. Which of the following combination of antibiotics is most appropriate?
- Ceftriaxone and Vancomycin
- Gentamicin and Vancomycin
- Flucloxacillin and Ampicillin
- Amoxicillin and Metronidazole
- Clindamycin and Piperacillin
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Excellent lecture as usual. I particularly appreciated to have the epidemiology and the clinical differences between the different organisms.
Very good lecture! It flows nicely, and really helps you understand the process. It makes learning easy and interesting