Playlist
Show Playlist
Hide Playlist
Human Papilloma Virus (HPV) and Genital Warts in Adolescents
-
Slides HPVandHerpes Pediatrics.pdf
-
Download Lecture Overview
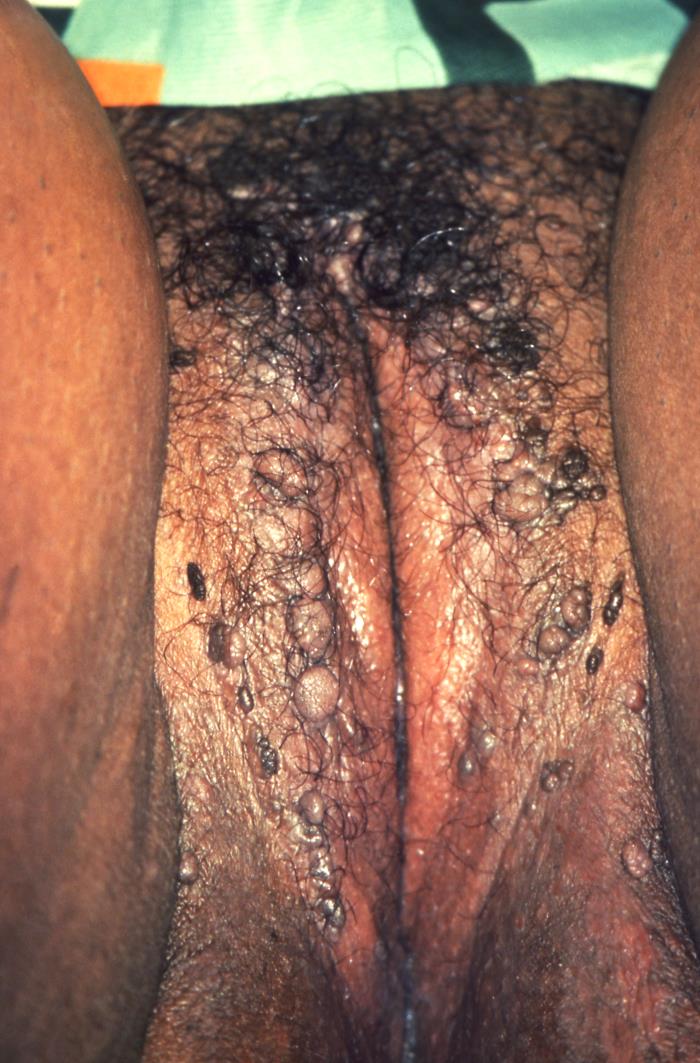
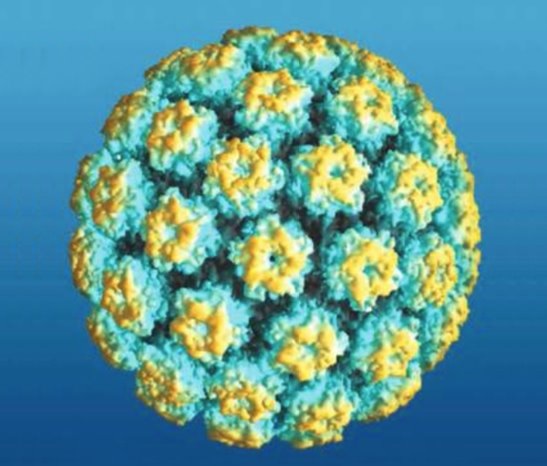
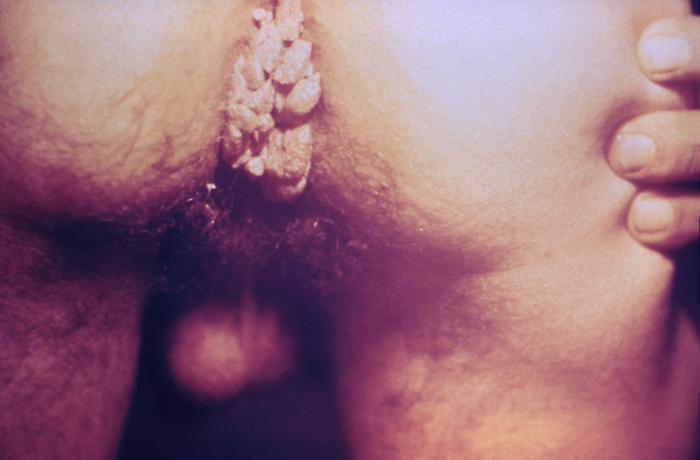
00:01 In this lecture, we will discuss the human papilloma virus and the herpes virus. 00:06 Let’s start with human papilloma virus. This is a double stranded DNA virus with more than 100 genotypes. It causes genital warts which are a condyloma acuminata in sexually active adolescents. It also causes anal, oral, and cervical cancer in adults. 00:26 Early sexual debut and having multiple sex partners increases a patient's risk for the HPV. 00:34 Let’s review the epidemiology of HPV before the vaccine came out. There used to be 6 million new infections per year and at least half of sexually active people got HPV. A low risk HPV, serotypes 6 and 11 caused 90% of genital warts. High risk HPV, serotypes 16 and 18 caused 70% of cervical cancer. But that risk is reduced but not prevented through condom use. 01:15 Most cases of HPV are completely asymptomatic. Most people don’t know they ever got it. 01:22 It can be transmitted through hand, oral, or genital sexual contact. It’s transmitted to newborns during birth. That newborn rarely can present with disease years later. The virus tends to infect the basal layer of epithelial cells in skin and mucous membrane. This can cause a cellular proliferation and hyperplasia which leads to wart formation or it can lead to anogenital and cervical carcinoma. 01:56 So, important questions to ask in patients where there is a concern for genital warts is has there been sexual activity? Does the patient have bumps in the genital region? These are usually non tender. And has the patient gotten an HPV vaccine? This is because the HPV vaccine is reasonably effective at preventing genital warts. Generally on exam, in patients, adolescents or children, you can see fleshy, exophytic, pedunculated lesions with a cauliflower like appearance. These can be small, discrete, sessile, or smooth-topped papules. 02:37 They may be single or they can come in great number. In males, they can be found on the penis, the scrotum, the inguinal area, and the perianal areas. In females, they may be found on the vulva, the cervix, inside the vagina, in the urethra, or in the perianal area. Generally, our diagnosis is based on the clinical appearance of the lesions. A Pap smear or a liquid-based cytology can be used to screen for cervical dysplasia. We typically do this starting at the age of 21. This is because there is a low yield early in adolescence. Generally, as things are moving along, we’re moving more towards PCR as the standard of care as opposed to Pap smears. In general, the natural history of this problem is that spontaneous regression of most genital warts will occur into 70%-90% of women within two years if they are untreated. Treatments include for patients a patient applied imiquimod 5% cream or podofilox solution or gel. Providers can apply cryotherapy, trichloroacetic acid, or a surgical, or a laser removal of these warts. Recurrence is common because the virus is not eliminated, just the wart. Recurrence can occur many years later. The HPV vaccine has done a great job at reducing the risk of not only warts but more importantly, cervical and anogenital cancer. 04:18 HPV vaccines are administered as a two-dose series (0, 6-12 months) for most persons who initiate vaccination at ages 9 through 14 years, and a three-dose series (0, 1-2, 6 months) for persons who initiate at ages 15 through 45 years, and for immunocompromised persons. 04:44 It currently protects against types 6, 11, 16, and 18 with the quadrivalent vaccine or if patients are using the bivalent vaccine, it protects against serotypes 6 and 11.
About the Lecture
The lecture Human Papilloma Virus (HPV) and Genital Warts in Adolescents by Brian Alverson, MD is from the course Adolescent Medicine.
Included Quiz Questions
The HPV vaccine is primarily designed to...?
- ...reduce rates of cervical cancer.
- ...reduce the prevalence of genital warts.
- ...allow improved safety of unprotected sex.
- ...allow relative safety for earlier sexual activity.
- ...allow relative safety for multiple partners.
Which of the following types of human papillomavirus are high risk genotypes?
- 16 and 18
- 6 and 10
- 5 and 11
- 6 and 11
- 14 and 17
Which of the following is the recommended starting age for cervical cancer screening with Pap smear?
- 21 years
- 18 years
- 16 years
- 23 years
- 25 years
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Excellent summary with interesting details regarding the Pap smear. Also, good descriptions for the clinical aspects.