Playlist
Show Playlist
Hide Playlist
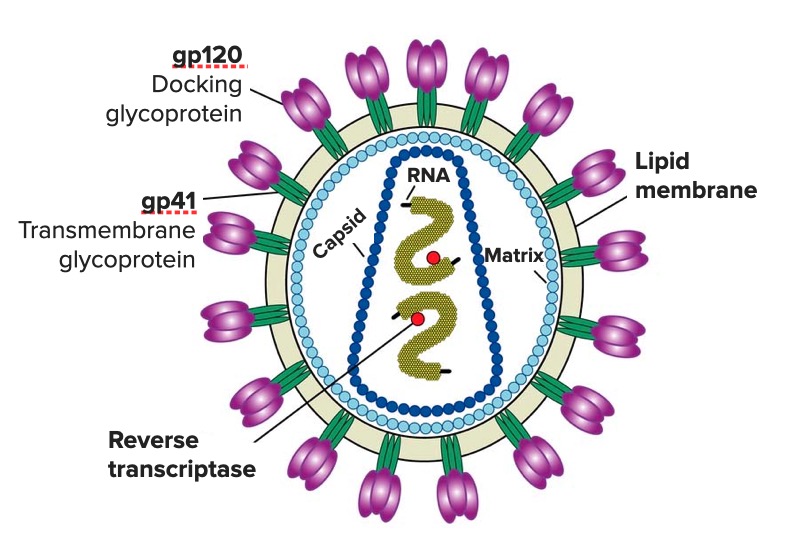
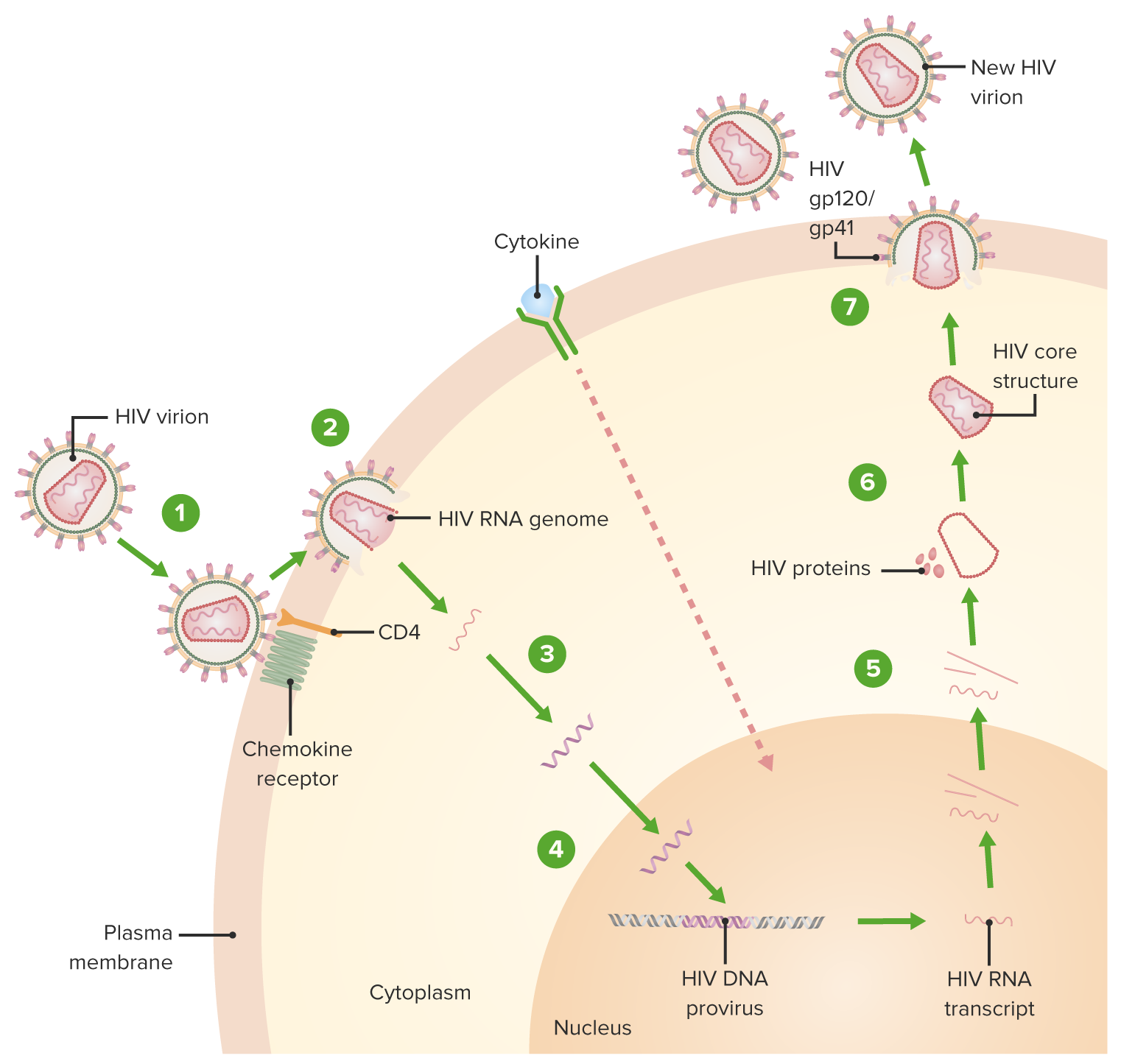
HIV Infection in Women
-
Slides CareofHIVwomen PathologyInfectionsNeoplasmsandScreening.pdf
-
Download Lecture Overview
00:01 Hi! today we're gonna discuss gynecologic care of the HIV-infected woman. 00:08 HIV in the US accounts for about 900,000 people living with HIV. 00:16 Heterosexual contact is the most common way for HIV transmission to women in the US, at least. 00:23 About 23% of these women will be exposed to HIV through injection drug use and about 2% will have perinatal infection which is to say that the infection is passed from the mother to the baby. 00:37 In the US we have a disproportionate amount of women who are African-American and Latina or "Latinx" who account for 78% of HIV infected women. 00:48 It's important to know that most women are diagnosed during their reproductive years with HIV. 00:53 This is the time when they'd be seeing a obstetrician gynecologist or primary care provider. 00:59 HIV infected women are increased risk of persistent and recurrent vaginitis, usually caused by bacterial vaginosis or candida albicans. 01:11 Women who have HIV have higher rates of cancer of the vagina, the vulva and peri-anal region. 01:18 Their cancer also tends to be very high grade compared with the general population. 01:23 Now let's discuss the management of non-pregnant women who are HIV positive. 01:28 Let's review how sexually transmitted infection should be managed. 01:32 First though, let's discuss PrEP. 01:34 And PrEP is pre-exposure prophylaxis. 01:37 Usually that's an anti-retroviral medication that is given to the partner of an HIV positive woman. 01:44 Herpes simplex virus prophylaxis is also given to HIV positive women to improve their chances of not having severe HSV outbreaks. 01:55 Also women who are HIV positive need to be screened for syphillis at the entry of care and at least annually thereafter. 02:05 Let's talk about the goals for the management of the non-pregnant woman who's HIV-positive. 02:11 So the number one goal for anti-retroviral therapy is to achieve a fully suppressed HIV viral load for their own benefit and long-term health. 02:22 and the second goal is to decrease transmission to uninfected partners. 02:29 In terms of cervical screening, normally we start at the age of 21 years old in the average general population. 02:36 However, HIV-positive women should begin within one year of onset of sexual activity. 02:43 If already sexually active, it should happen within the first year of HIV diagnosis. 02:49 No later than 21 years of age should they commence doing PAP smears and continue throughout life, not stopping at 65 years old as in the general population. 03:01 In terms of contraceptives of women who have HIV, we recommend that women actually use copper IUDs or intra-uterine devices or levonorgestrel-releasing IUDs. 03:12 And those can both be safely used in HIV-positive or HIV infected women. 03:18 Hormonal contraception is also considered safe for use by HIV-positive women and those who are taking antiretroviral therapy. 03:28 Another alternative that is a more long acting medication is depot medroxyprogesterone acetate and this can be prescribed to women who have HIV. 03:38 It's considered MEC category 1. 03:42 In terms of other contraceptive choices, it's important to remember to avoid vaginal spermicides such as Nanoxynol-9 which actually may increase the risk of HIV transmission due to vaginitis. 03:56 I just want to point out to you one high-yield fact in the care of HIV-positive women and that is stopping transmission. 04:03 Women with HIV should be screened for high risk behaviors and offered interventions. 04:09 We know that high risk behaviors including sexual and drug behaviors can lead to increased transmission of HIV. 04:18 So just to remember: African-Amercian and Latina or Latinx women are increased risk for HIV infection. 04:25 Partners of HIV infected women should use PrEP. 04:29 HIV infected women should be offered intra-uterine devices such as the copper IUD or the levonorgestrel IUD And women should be encouraged to use condoms and hormonal contraception. 04:41 Discourage women from partaking in high-risk behaviors that can lead to increased transmission. 04:48 Thank you for listening and good luck on your exam.
About the Lecture
The lecture HIV Infection in Women by Lynae Brayboy, MD is from the course Gynecologic Pathology: Infections, Neoplasms and Screening.
Included Quiz Questions
Which of the following is NOT a part of the cervical cancer screening for HIV affected women?
- Stopping the PAP screening after 65 years of age
- Screening with PAP smear should begin within one year of onset of sexual activity
- If the patient is already sexually active within the first year after HIV diagnosis
- Screening should begin no later than 21 years of age
- Screening with PAP smear must be throughout life
Which of the following contraceptives are contraindicated in women affected with HIV?
- Spermicidal jelly
- Hormonal IUD
- Oral contraceptives
- Condoms
- Depot medroxyprogesterone acetate
Which population cohort is at increased risk of HIV Infection?
- African American women
- Caucasian women
- Japanese women
- Middle eastern women
- Chinese women
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |