Playlist
Show Playlist
Hide Playlist
Headache: Introduction
-
Slides 08 Headache Neuropathology I.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
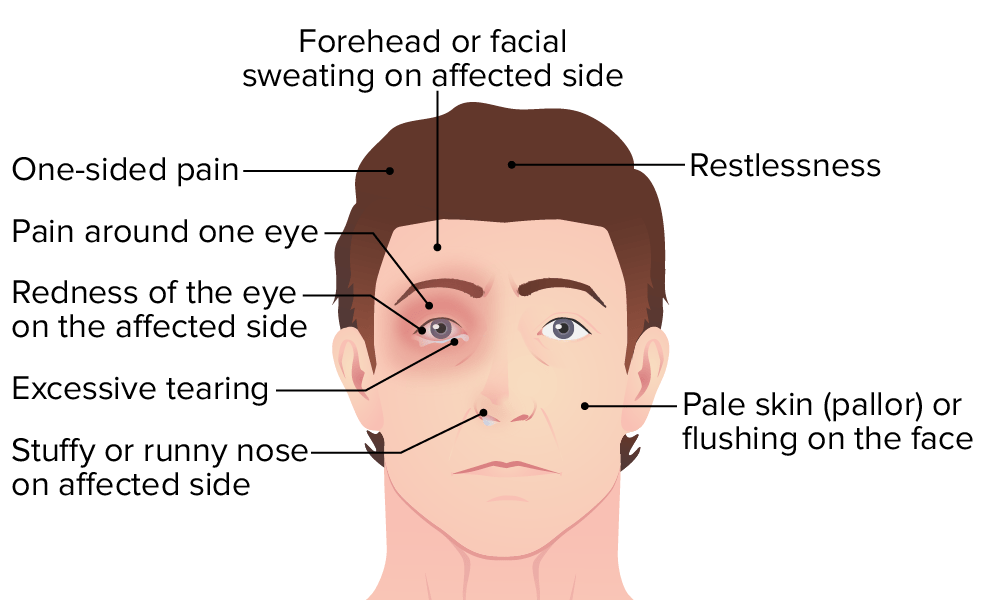
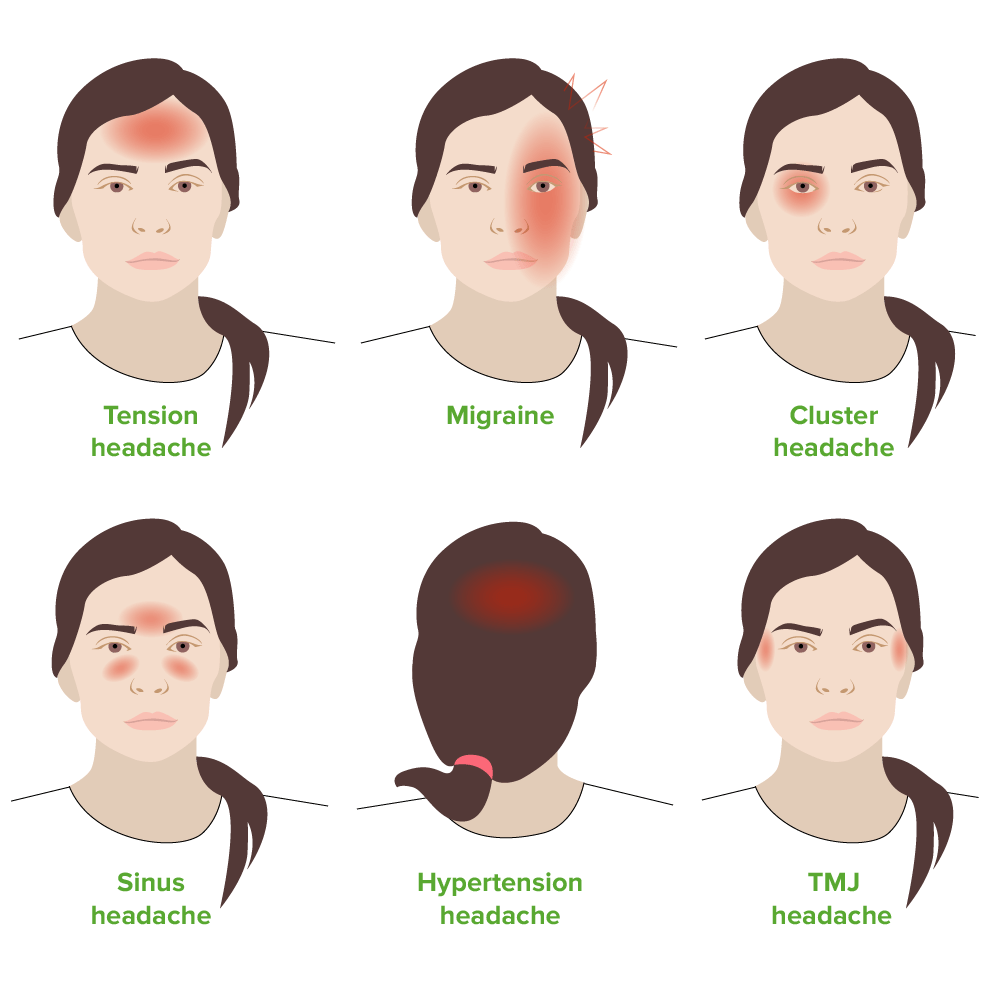
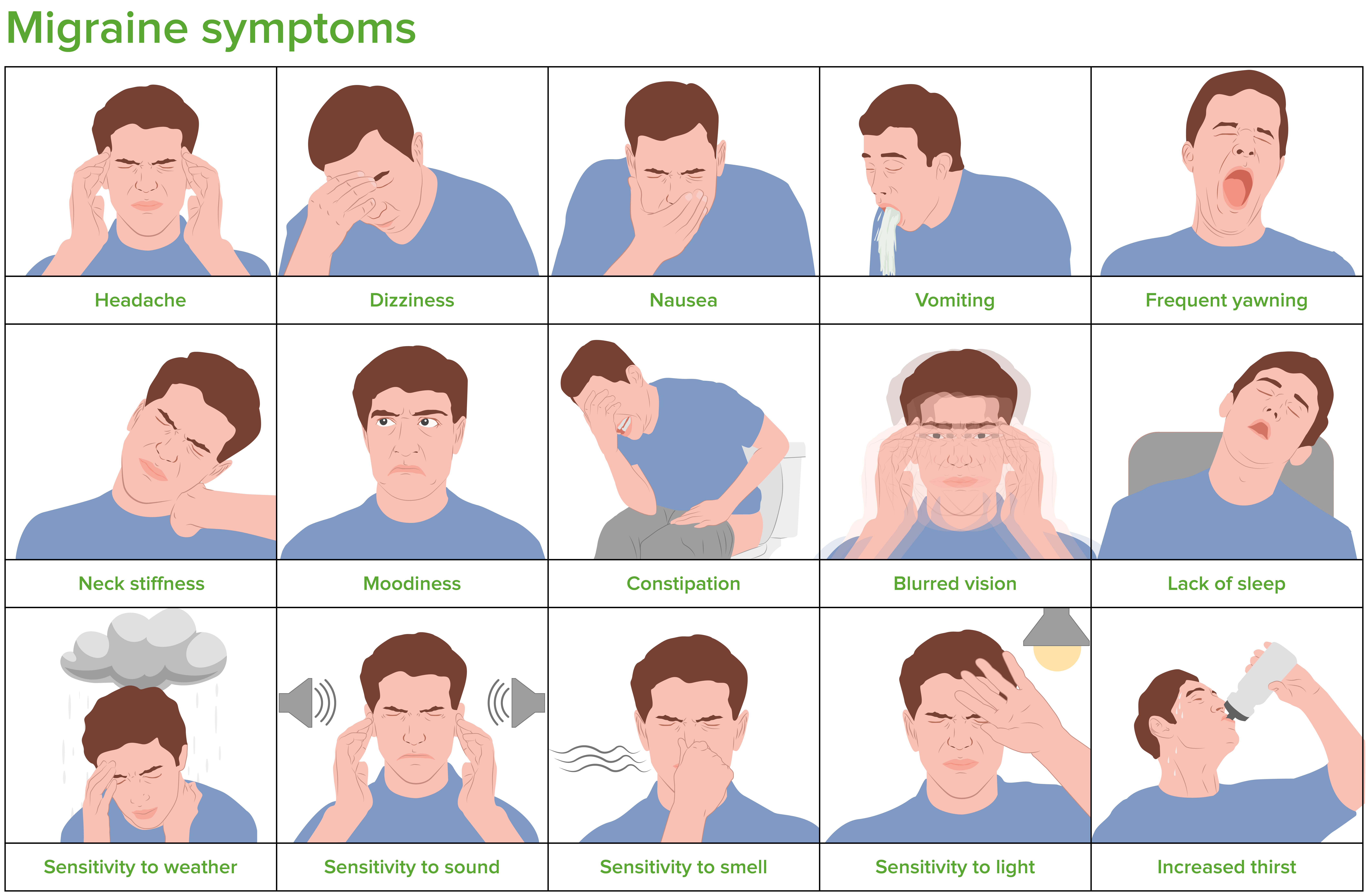
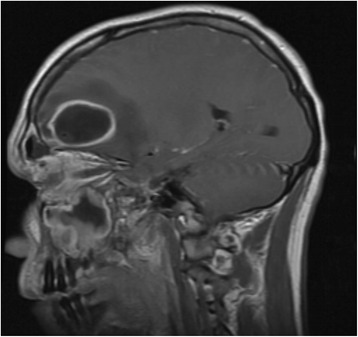
00:01 Here, we’ll take a look at headache, a big topic. 00:04 List of differentials. 00:05 We’ll be integrating many of the neuropathologic issues that we’ve seen prior when we get into the topic of headache. 00:16 The pathophys. 00:18 Pain sensitive structure of the head: scalp, scalp blood supply, head and neck muscles, venous sinuses, meningeal arteries, large cerebral arteries, pain sensitive fibers in cranial nerves V, IX, and X, dura mater at the base of the brain. 00:37 Any one of these could result in “headache.” Brain parenchyma has no pain fibers, and that’s important for you to understand. 00:49 Let’s spend a minute, make sure that you have thoughts organized here in terms of what’s pain sensitive and not having pain receptors or fibers. 00:58 Primary headache syndromes: migraine, cluster, tension, post coital. 01:07 We’ll take a look at these in terms of differential diagnoses. 01:10 Secondary headache. 01:14 Was there a metastatic or primary brain tumor? Was it metastatic for melanoma? Was it small cell lung cancer? Was it breast cancer? Was it kidney cancer? And so forth. 01:27 Was it primary? Glioblastoma multiforme resulting in a secondary headache. 01:32 Abscesses, secondary headache. 01:35 What if there was a hemorrhage? Intracerebral, subdural, epidural, subarachnoid. 01:41 Any one of these types of hemorrhages may result in a secondary headache. 01:46 Remember, once again, meningitis, pain sensitive, closer to the scalp. 01:54 You have blood vessels, and all these are pain sensitive causing secondary headache. 02:00 Temporal arteritis. 02:01 Think about that older lady in which there is a giant cell arteritis, headache. 02:09 Pseudotumor cerebri. 02:11 Who’s this patient? A female in her reproductive age, and all of a sudden, there is a headache. 02:18 And upon fundoscopic examination, you find papilledema but there’s no tumor, absolutely no evidence of tumor. 02:24 Short-lived. 02:26 It’s interesting. 02:27 Nowadays, it’s often referred to as idiopathic. 02:29 Hypertension, hydrocephalus, glaucoma, all differential diagnoses for secondary headache. 02:36 H&P for headache: the quality, severity, location, duration and time course becomes important as we shall see, associated symptoms, and aggravating and alleviating factors. 02:48 As you would with any type of questionnaire when you are interviewing a patient with headache. 02:54 General exam, general neurological exam, fundoscopic exam becomes important, palpation of superficial temporal artery if you’re suspecting a giant cell arteritis, palpation of cervical spine and paraspinal muscles. 03:09 Always make sure you get a good history. 03:11 Your clinical approach. 03:14 Once again, it’s important that you pay attention to quality, severity, location. 03:18 Next, time course is extremely useful: acute, subacute, and chronic, and we will divide it as such. 03:26 All I’m doing right now is quickly going through how we shall approach headache in this entire section.
About the Lecture
The lecture Headache: Introduction by Carlo Raj, MD is from the course Headache – Pathophysiology.
Included Quiz Questions
Which structure has no pain fibers?
- Brain parenchyma
- Scalp
- Head and neck muscles
- Venous sinuses
- Meningeal arteries
Which of the following regions of the head lacks sensitivity to pain?
- Brain parenchyma
- Trigeminal nerve distribution
- Vagal nerve distribution
- Middle meningeal artery
- Muscles of the head
Which of the following types of headache is due to a secondary pathology?
- Temporal arteritis
- Migraine headache
- Cluster headache
- Tension headache
- Postcoital headache
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |