Playlist
Show Playlist
Hide Playlist
Greenstick-, Buckle-, Apophyseal Avulsion-, Supracondylar and Toddler's Fractures
-
Slides Fractures Pediatrics.pdf
-
Download Lecture Overview
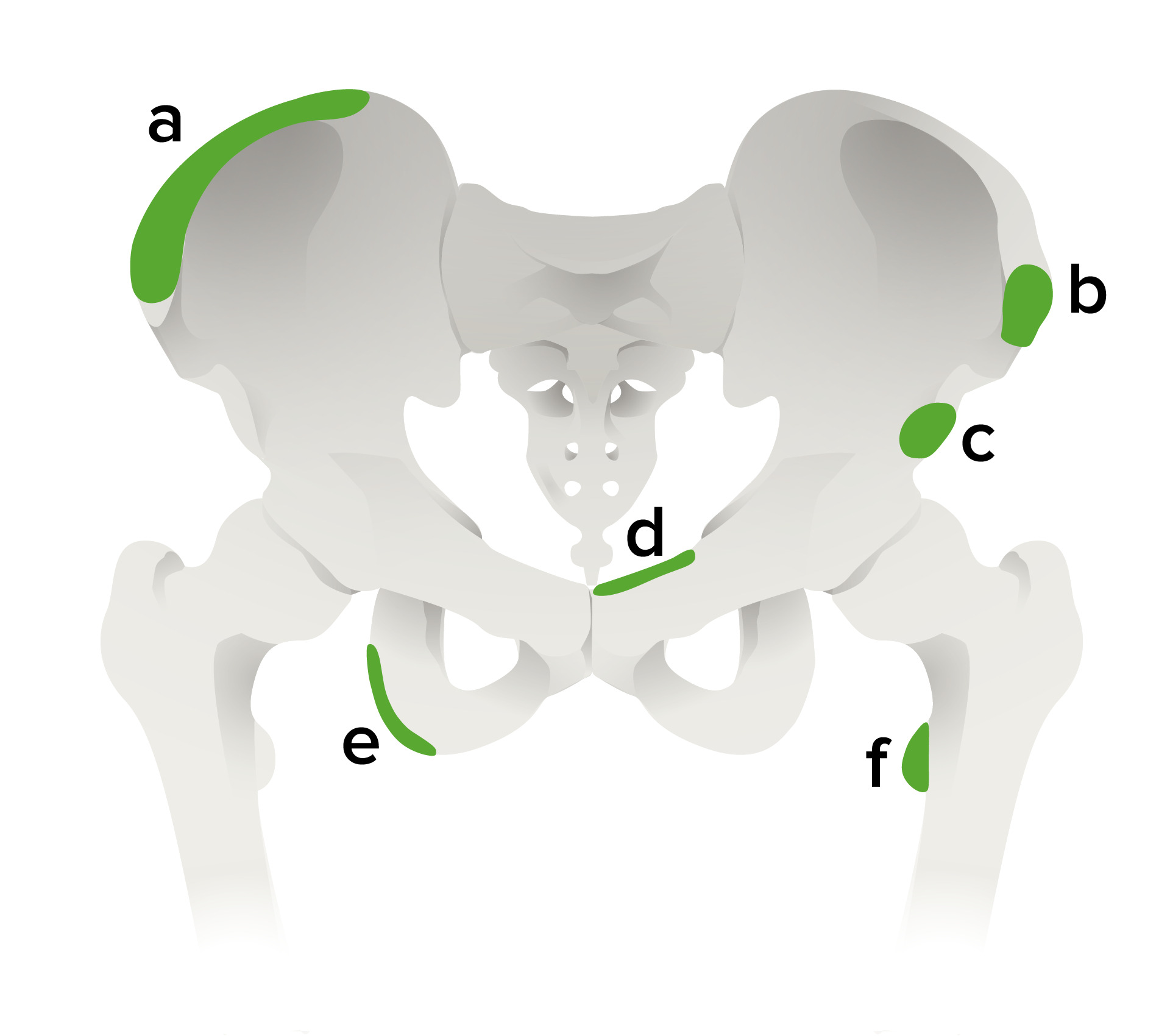
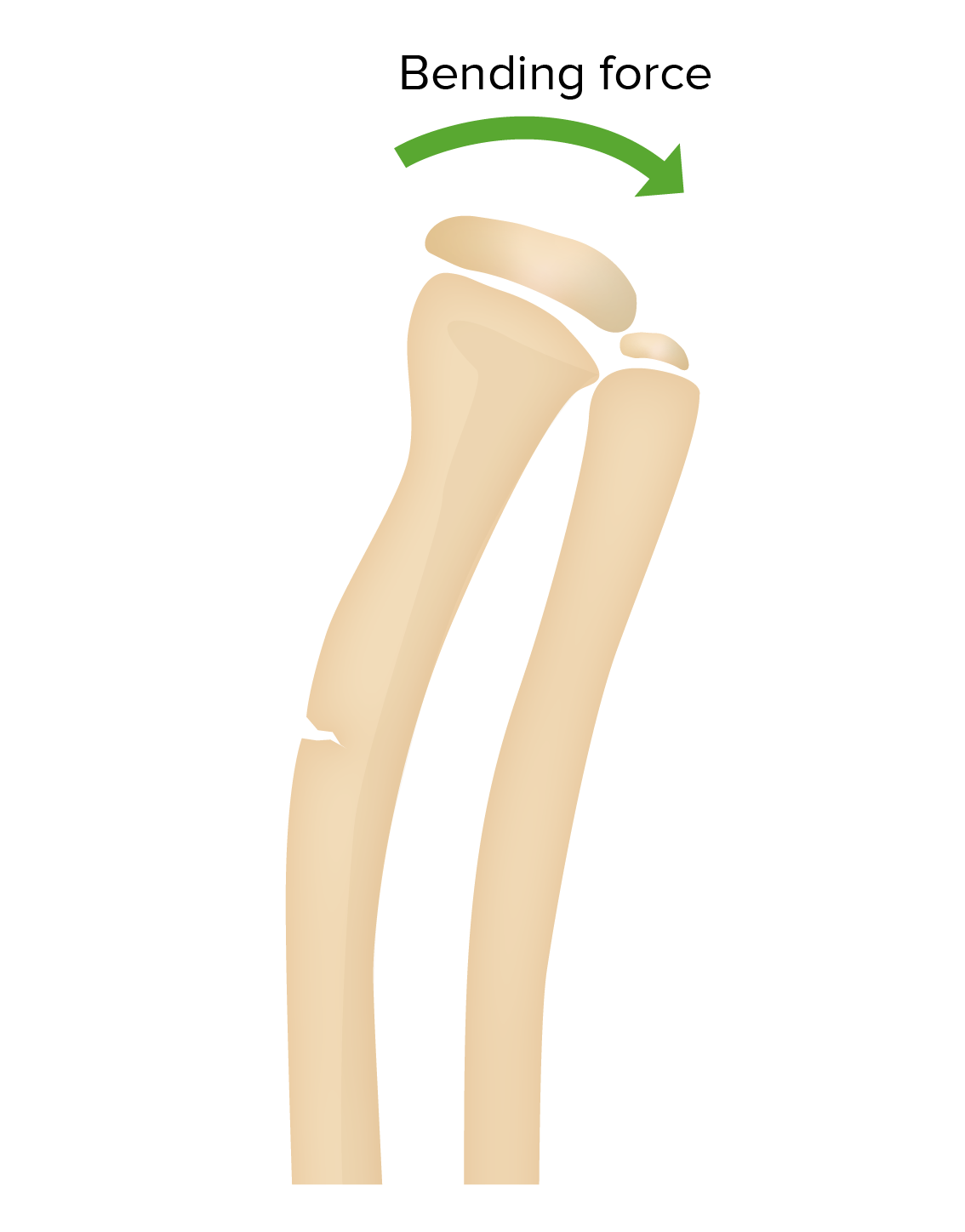
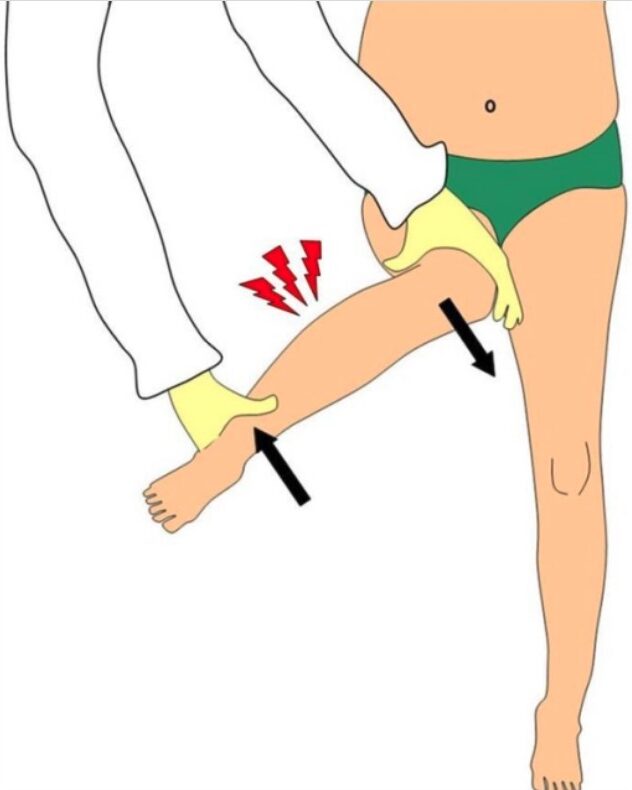
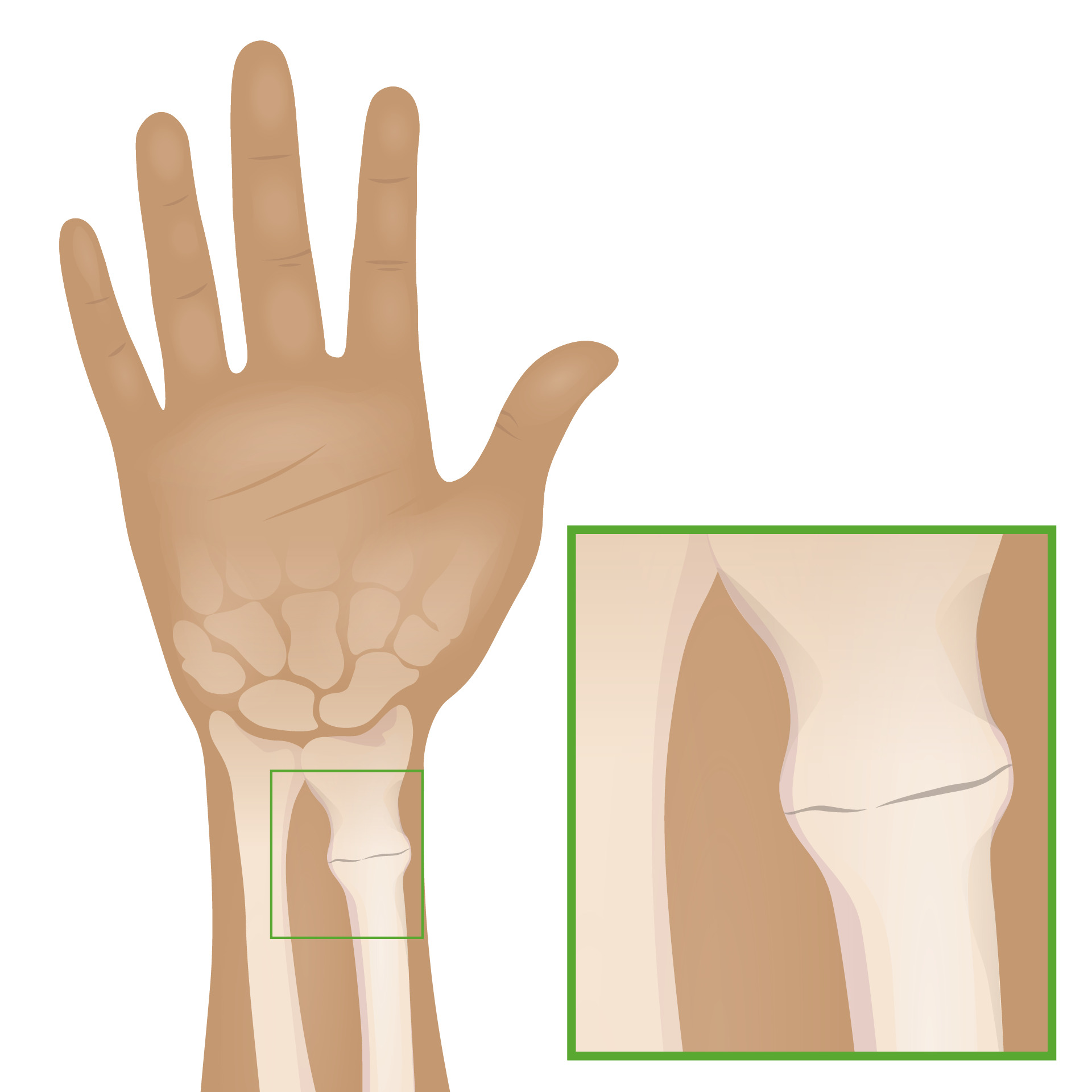
00:01 Another type of fracture that’s somewhat unique to children is a greenstick fracture. 00:06 This happens because the child’s bone is fairly flexible and pliable and it’s result of an incomplete fracture. 00:14 Here, you can see a Colles’ fracture going through the distal radius of this child and what you can see from one view, you’d say, “Oh, that’s a simple Colles’ fracture.” But when you look at it from the other angle, you can see it’s broken almost like a greenstick when you can’t quite break it all the way. 00:30 This may require the orthopedist to break it by bending it the other way. 00:34 We would definitely put a child to sleep under deep sedation for that procedure and then setting it straight so it can heal correctly. 00:43 We usually treat these like regular fractures with long term immobilization, pain control, and casting and then eventually they usually get better. 00:53 This is another type of fracture which we would call a buckle fracture. 00:58 If you sort of imagine a hotdog and you held the two ends and you squeezed it together, you get a little bulging in the middle, that’s a buckle fracture. 01:06 You can even see it on the view where it’s more subtle. 01:10 There’s a little bit of subtle increase in the size of the wrist of the bone, right around the wrist where that fracture is if you trace the sides of the wrist. 01:15 For this, we’re going to immobilize, provide pain control, and have them followup with an orthopedist for casting. 01:27 We don’t usually cast right away. 01:30 The reason why we don’t cast right away as there may be some continued increased swelling, so first we’ll splint. 01:35 The splint allows for a little bit of swelling out the sides and then we’ll cast later. 01:42 Another type of pediatric fracture is the apophyseal avulsion fracture. 01:45 Avulsion fracture happened because the tendon of a muscle is inserted in the bone and through vigorous exercise, that insertion point gets pulled off the edge of the bone. 01:57 The apophysis is torn off by the muscle after repeated overuse. 01:59 This is classic in the anterior superior iliac crest. 02:03 This happens more in swimmers and runners. 02:08 And in the tibial tubercle, as you can see here, this is consistent with Osgood Schlatter’s disease. 02:15 This is more common in jumpers and runners. 02:17 Usually athlete’s common problem and you can see the end of the apophysis pulling off. 02:23 Another fracture that we should know about because it can be hard to see is the supracondylar fracture of the distal humerus. 02:30 It’s hard to see because, well, the elbow’s hard to appreciate, but there’s a phenomenon that can happen with a fat pad, which you normally not see. 02:41 It slips out and you see a little bit of a darkened lucency outside of the bone. 02:44 This requires an immediate orthopedic consult. 02:46 So this is a subtle finding you have to get used to seeing, but it’s very important to call an orthopedist because these are a great risk for harming the neurovascular bundle that goes past the elbow. 03:00 So it’s very important that these patients are stabilized, immobilized, and orthopedics sees them and oftentimes they’ll just take them straight to the OR to correct this problem surgically. 03:13 One final common pediatric fracture you don’t see in adults is the toddler’s fracture. 03:16 Yes, this happens in toddlers. 03:19 Very young kids who are walking and it’s a spiral fracture of the distal tibia as you can see here. 03:27 It’s usually a little line going diagonally down the bone. 03:30 Usually, there’s no story of trauma and of course, in a child with a broken bone with no history of trauma, we would worry about child abuse. 03:41 But this is not child abuse. 03:44 What’s happened is the child was stepping and then forcefully quickly turns on one leg, causing a twisting and a torsing of that tibial area where you get that tibial fracture. 03:54 Again this is not a sign of child abuse. 03:58 It’s common in toddlers. 04:00 So that’s my review of the important aspects of pediatric fractures. 04:03 Thanks for your time.
About the Lecture
The lecture Greenstick-, Buckle-, Apophyseal Avulsion-, Supracondylar and Toddler's Fractures by Brian Alverson, MD is from the course Pediatric Emergency Medicine. It contains the following chapters:
- Greenstick Fractures
- Buckle Fractures
- Apophyseal Avulsion Fractures
- Supracondylar Fracture of Distal Humerus
- Toddler's Fracture
Included Quiz Questions
Fracture of which of the following parts of the body is commonly known as the Colles fracture?
- The wrist
- The elbow
- The hand
- The foot
- The cervical spine
Which of the following terms refers to a fracture following bending of a young bone?
- Greenstick frature
- Incomplete fracture
- Buckle fracture
- Avulsion fracture
- Supracondylar fracture
Which of the following is a common location for an avulsion fracture?
- Anterior superior iliac spine
- Femoral neck
- Wrist
- Supracondylar region
- Spine
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |