Playlist
Show Playlist
Hide Playlist
Endometrial Cycle
-
Slides Female Hormones Endocrine System.pdf
-
Download Lecture Overview
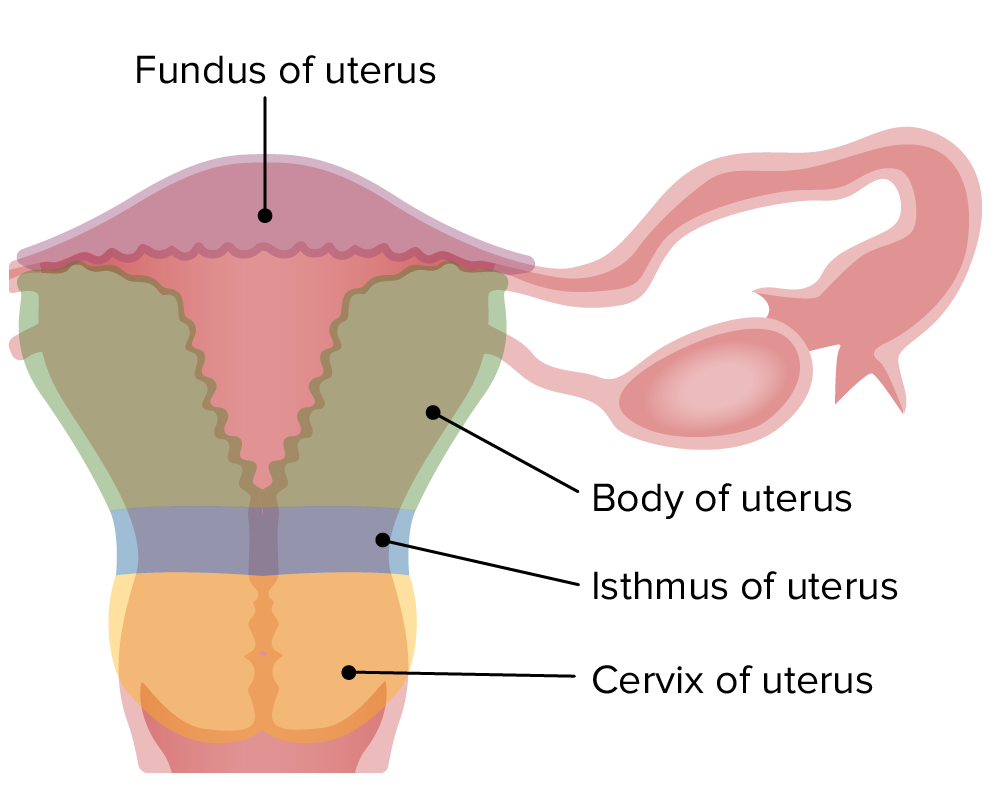
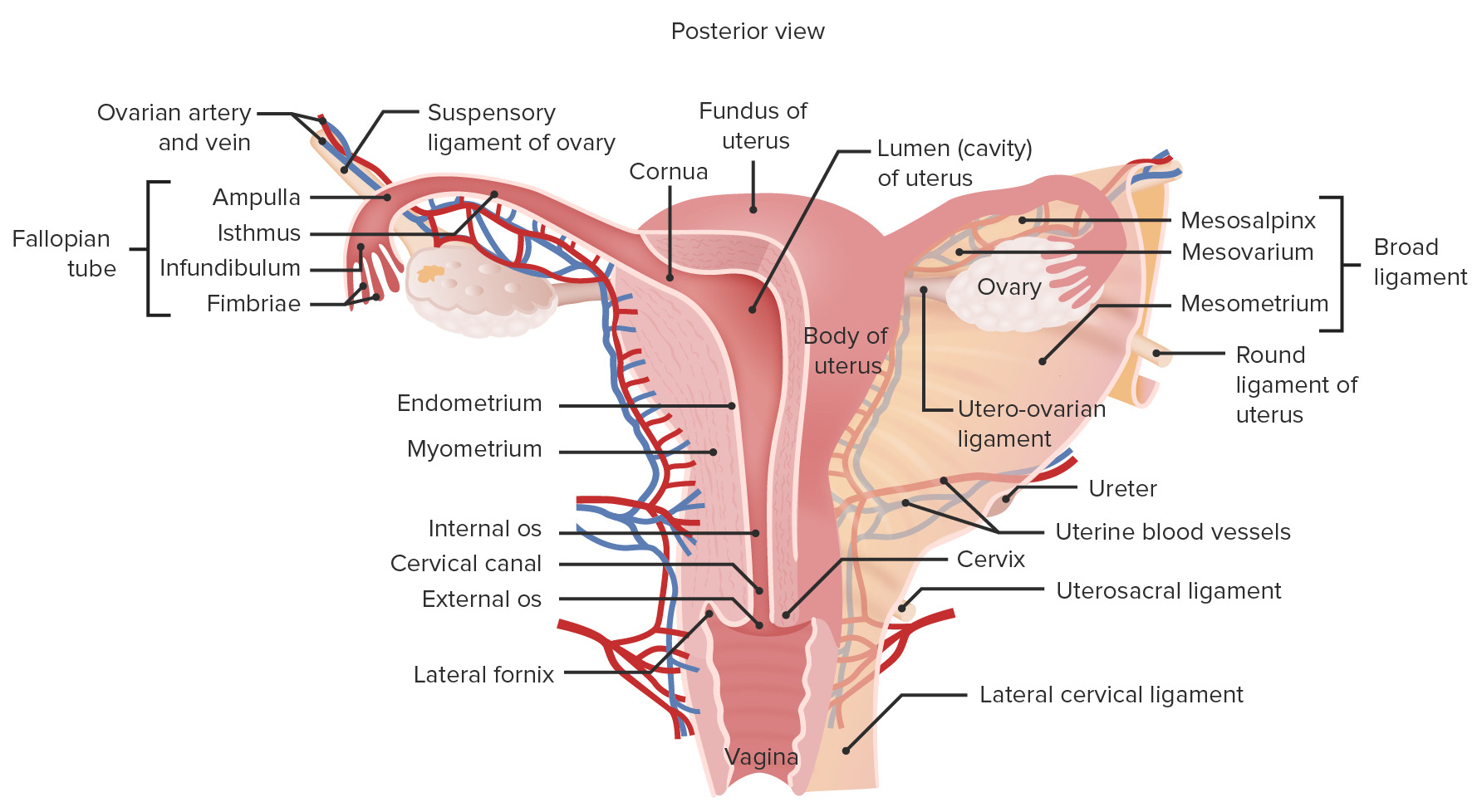
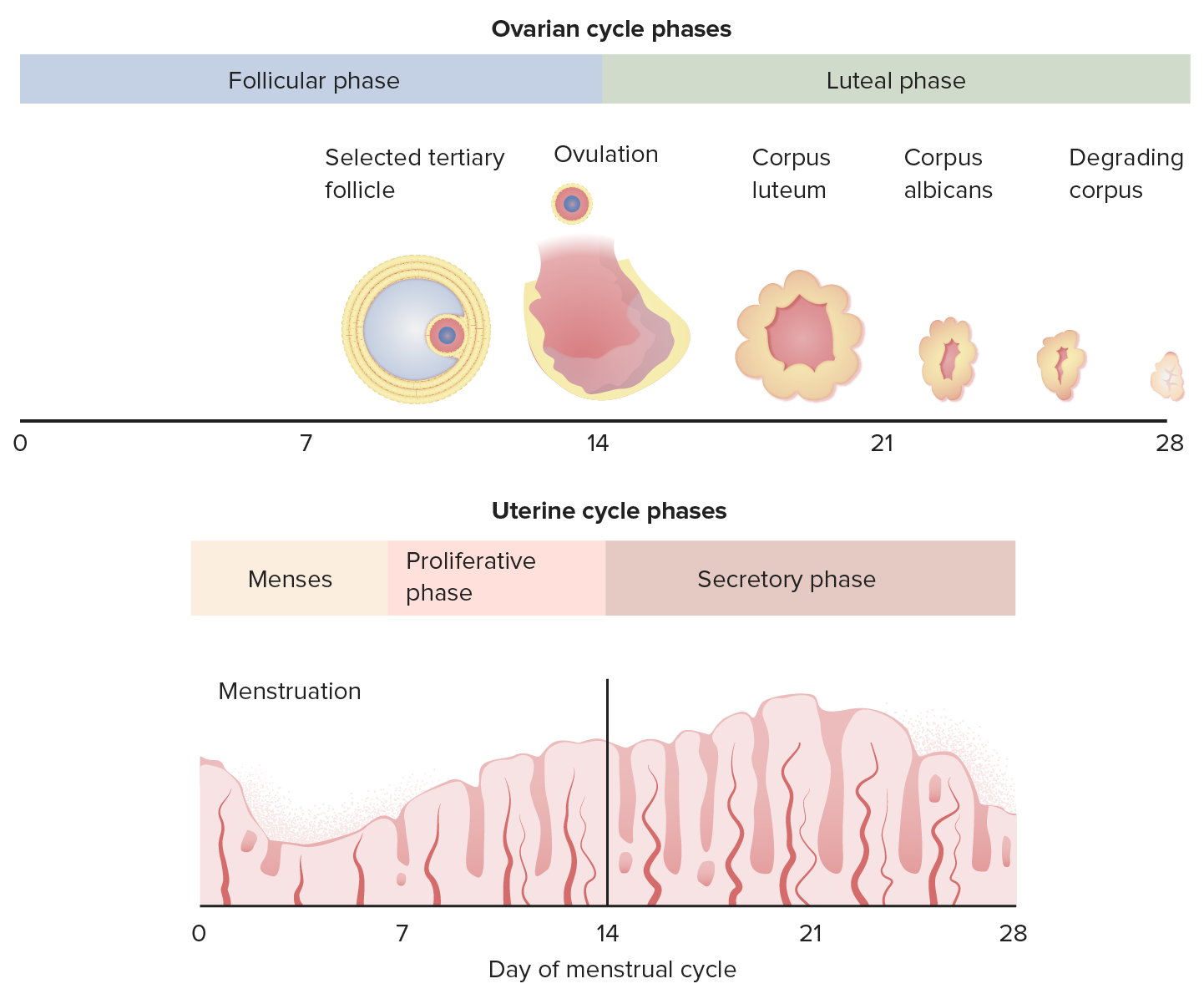
00:00 Endometrial Cycle. The endometrial cycle is broken into three phases rather than the two phases of the ovarian cycle. So the ovarian cycle had a follicular phase and a luteal phase. 00:16 In the endometrial cycle, we have a menstrual phase, a proliferation phase and a secretion phase. In these three phases, you want to focus on what is happening at the endometrial lining. 00:30 During the menses phase, it is sloughing. During the proliferation phase, you are increasing the endometrium. During the secretion phase, there are secretions happening but it will be maintained in terms of size for prolonged portion. Only towards the very end you start to lose some of that volume. To link these two together becomes very important and this is the process that you want to think about. What is happening at these different levels and why do you need to have the lining a certain size at a certain time? To do that, you think about the follicle and how it is maturing. You're going to have to release the follicle at the right time and have the endometrium at the right level for there to be potential for fertilization to occur and then binding to that uterine wall. So let's talk about the follicle in a little bit more detail. 01:30 In this case, you start off with a primordial follicle. It starts to develop into a primary follicle, then a secondary follicle, finally a tertiary follicle and then a Graafian follicle. Here is where you're ready to eventually release the oocyte. I will point out that if you can see here the different cell types, you have granulosa cells and theca cells. These are the exact cells that are undergoing the production of progesterone and estradiol. So it is the cells here that are producing those hormones necessary for you to have estradiol and progesterone in the body. 02:16 Once you release the oocyte, you have then the corpus luteum and at that particular point you will still be producing hormones even though you have lost that oocyte. The corpus luteum. 02:32 This corpus luteum will have both granulosa cells and theca cells. This re-forms as part of the process after releasing the egg. It's interesting to think about the various cell layers involved with the corpus luteum. The corpus luteum has this theca lutein and granulosa lutein cells. 02:59 These will produce things like estradiol and progesterone. The corpus luteum will become a corpus albicans unless hCG rescues it and this is an important process to think about. So where does the hCG come from? Only a fertilized egg. So that is the process that saves this thing or rescues it from going into an inactive state. Let's summarize this by looking at the combined cycles of both the follicular phase and luteal phase associated with the ovarian cycle and then the various phases that are _ with the endometrial cycle. So let's look at the hormones first and link them up with the various changes that happen with either the egg or with the endometrial cycle. Here in the follicular phase, you have fairly low levels of LH and FSH. 04:06 Estradiol levels are starting to climb as the follicle is developing. That makes sense because the follicle is what's going to have the theca and granulosa cells. They start to peak just before the LH surge. At this time, you have the proliferation that's also occurring in the endometrium. 04:32 Therefore, you're now ready to receive that particular egg. You notice then that LH drops off dramatically, estradiol drops off just before the LH and progesterone starts to climb. 04:48 Progesterone is going to be associated with secretions and that is what is maintaining then the endometrium throughout that rest of the time in the secretory phase. As you do secretions though, the egg has already been released and therefore you have this corpus luteum.
About the Lecture
The lecture Endometrial Cycle by Thad Wilson, PhD is from the course Reproductive Physiology.
Included Quiz Questions
Which hormone rescues the corpus luteum from becoming a corpus albicans?
- hCG
- Estradiol
- Progesterone
- Luteinizing hormone
Which of the following follicles release the oocyte?
- Graafian follicles
- Primordial follicles
- Early primary follicles
- Secondary follicles
- Late primary follicles
Which of the following hormone-releasing patterns are seen during the release of the oocyte?
- LH surge
- LH drop
- Estradiol surge
- hCG drop
- hCG increase
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |