Playlist
Show Playlist
Hide Playlist
Conditions with Tissue Edema
-
Slides 14 VascularMedicine advanced.pdf
-
Reference List Vascular Medicine.pdf
-
Download Lecture Overview
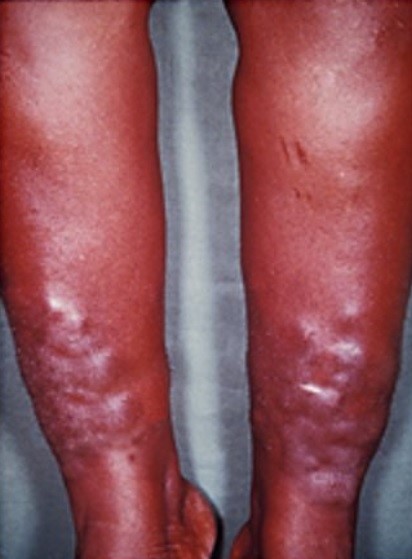
00:01 Well, let’s talk about edema that develops not because of an abnormality in the lymphatic vessels but because of another disease. 00:09 There are two very common diseases that lead to edema, particularly in the legs. And sometimes it can spread all the way up into the lower abdomen. One of these is heart failure and the other is liver failure. Let’s talk a little bit about heart failure. 00:27 What happens in heart failure is that the heart doesn’t contract adequately, particularly the left ventricle. When it doesn’t contract adequately, there’s all kinds of remodelling, changes. The ventricle dilates in an attempt to keep up the cardiac output. And when it does that, the pressures during diastole – that is during the resting phase – rise and are transmitted back to the lung and, eventually, are transmitted back to the venous system and venous pressure rises. 01:00 When venous pressure rises, then capillary pressure rises. And now you have a marked difference between the hydrostatic and the oncotic pressure and fluid leaks out at a much faster rate into the tissues. At a rate so fast that the lymphatics cannot drain it adequately. And what you end up with is swelling – or edema, which is the medical term – particularly in the lower extremities. 01:25 Persistent edema is often a sign of heart failure. It can also be a sign, on the other hand, of liver failure. What happens in liver failure is that the liver fails to produce albumin and other proteins to maintain oncotic pressure. So down in the capillaries instead of increased hydrostatic pressure, you have decreased oncotic pressure. And, again, excess fluid leaks out of the capillaries and into the tissues. 01:56 Both of these forms of edema can be very difficult and challenging to remove although most patients with mild liver failure or mild heart failure will respond to diuretics – that is medicines that increase the flow of urinary fluid and increase the amount of urine that one makes and therefore gets rid of this extra fluid that’s in the body. 02:20 So, for heart failure, we have a whole variety of other drugs. We’re not going to review them right now. Those of you who are interested, it’s in the Cardiology series. There’s a whole lecture on heart failure. It discusses all of the various drugs, particularly a drug called beta blockers which decrease the heart rate and allow the heart to heal to some degree from whatever injury it’s had. And, of course, diuretics increase the urine flow and get the fluid out. 02:48 In liver failure, we also use diuretics. But in particular there’s a diuretic called spironolactone that blocks aldosterone. Remember the renin-angiotensin-aldosterone system? Well, this spironolactone drug blocks the aldosterone and allows the kidneys to get rid of more fluid. 03:08 Often edema in liver failure is much more challenging to get rid of than in heart failure and often will collect in the abdomen. The patients will have a belly full of fluid at the end stage of liver failure. It’s a little easier to control the edema in heart failure. 03:27 Well let’s talk about conditions where the lymphatics are destroyed by disease or surgery. 03:34 The commonest one – although much less common these days – is when a female patient with breast cancer gets a radical mastectomy in which all the lymph nodes and the upper thoracic lymph nodes are removed to make sure that there’s no cancer cells that survive. What you do then is you cause a marked decrease in the lymphatic ability to drain the arm and, very often, these women have chronic arm edema. 04:02 It’s often managed as I’ll mention in a moment. Sometimes you can put a pump on that squeezes the lymphatic fluid out of the arm. And compressive or elastic bandages will help. 04:14 There are a number of parasitic diseases that actually destroy the lymph vessels and, of course, then the fluid doesn’t drain out of the tissues. And you actually see a picture here of a woman who has had a parasitic disease that destroyed her lymphatic vessels. And you can see her massive peripheral edema in her legs. 04:37 The massive edema that occurs is called elephantiasis because it looks like the bulky leg of an elephant. 04:45 The commonest parasite that does this is in Africa. It’s Wuchereria bancrofti. This little worm is introduced through the skin usually by insect bites. And it then works its way into the lymphatic vessels and the lymphatic vessels develop fibrosis and scarring and close down. And that leads to elephantiasis. 05:03 There’s a genetic disease where people are born without good lymph vessels. That’s known as the Proteus syndrome. It’s very rare but again you get the same thing: elephantiasis because the tissue fluid never can leave the limb or leaves very, very poorly. 05:21 And occasionally there will be an autoimmune disease which will attack the lymph vessels and result in their scarring and fibrosis and could also lead to elephantiasis – to huge edema. 05:32 There’s a huge problem there. This amount of edema impairs tissue nutrition because the blood flow has a hard time getting in because of the massive edema. And often you can develop ulcers and even necrosis – death of tissue. And sometimes even amputation is required. 05:51 So the therapy for all of these forms of edema consists of diuresis – that is you increase urine flow in an attempt to get the fluid out of the body. 06:01 If you raise the limb, that will help some of it with gravity to drain the fluid out. 06:07 And then, as I mentioned, compression stockings or arm binding. And there are intermittent compression devices that can be bought. Particularly women who’ve had a radical mastectomy often two or three times a day will put their arm in the compression device and it squeezes the lymph fluid out of the arm so that there’s not so much edema in the arm.
About the Lecture
The lecture Conditions with Tissue Edema by Joseph Alpert, MD is from the course Diseases of the Lymphatic System.
Included Quiz Questions
Identify the TWO medical conditions that are most commonly associated with edema in the legs.
- Heart failure.
- End stage liver disease.
- Ulcerative colitis.
- Bacterial pneumonia.
Edema in case of liver failure occurs due to which of the following abnormalities in pressure?
- Decreased oncotic pressure.
- Reduced capillary pressure.
- Reduced diastolic blood pressure.
- Increased diastolic blood pressure.
- Increased hydrostatic pressure.
Diuretics are used for reduction of edema in which of the following situations?
- In both liver and heart failure.
- In excess salt intake.
- In excess sugar intake.
- In liver failure but not heart failure.
- In neither liver nor heart failure.
Spironolactone is a diuretic, which one of the following is its CORRECT mechanism of action?
- Blocks aldosterone.
- Acts as an alpha blocker.
- Acts as a beta blocker.
- Blocks ADH.
- Blocks vasopressin.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |