Playlist
Show Playlist
Hide Playlist
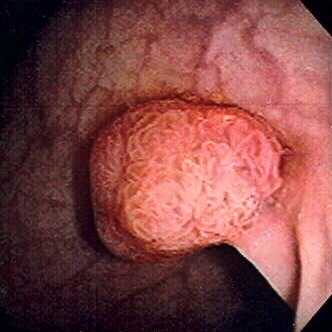
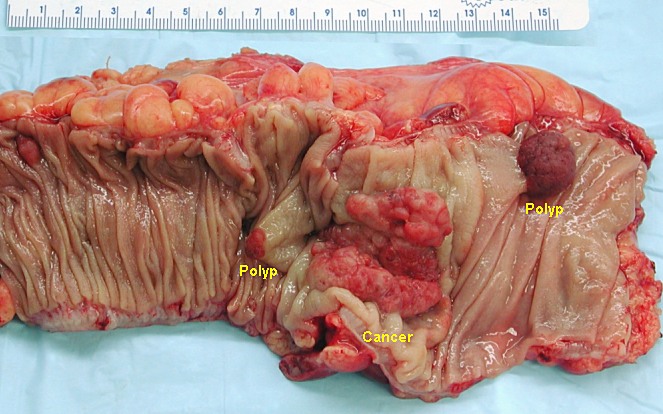
Colorectal Tumor
00:00 Right. 00:04 Now, the next part will take us to another important MCQ in your exam which is what type of operation you do for different tumors, colorectal tumors. 00:46 Adenocarcinoma, you'd say Dukes B adenocarcinoma. 00:55 What's the most appropriate resection? Until what point would you excise/resect? You want to go from the ileocecal junction to mid-transverse colon. 01:13 Mid-transverse colon, I would just take… That should be fine. Fine, you resect that. 01:22 What will you anastomose? You can anastomose the ileum onto the transverse colon. 01:30 So, you can do a primary ileocolic anastomosis. 01:33 If you're unsure, you can leave to say stoma, ileostomy for a short while, but then you can anastomose. 01:40 Usually, when you do a right hemi, you are just anastomosing it. 01:46 Now here, one important concept you need to understand which I'm sure you'd understand by now, what is the normal resection margin for an adenocarcinoma anywhere in the body. 01:55 How much do you need? Just think of any carcinoma. 02:01 What's the maximum resection margin we need, breast cancer, any cancer? 5 centimeters, any sarcoma, anything, unless it is a very rare tumor, you need to go for 10, you really don't go for anything more than 5, isn't it? So, if you take 5, that's all you need, right? Then, the question is why are you going until there? Because you’ve got to assume that the blood supply to the affected colon is also possibly you’ve got to take the whole of that and take blood supply basically to that portion as well. 02:32 Why do you have to take the blood supply to that portion? I’m just leading you to that part. 02:37 You’re right. Why do you have to take the blood supply? Let me put it this way. 02:41 You have the right colic supplying here. 02:42 You have the middle colic supplying there. 02:44 If you anastomose this to that, won’t that heal? It will still heal, won’t it? If you anastomose this part of the colon to that part of the colon, it will still heal. 02:54 Does it do drainage? Drainage, yeah. Tell me more there. 02:57 Your lymphatic drainage, okay, so that's right. 03:01 So, your lymphatic drainage follows the arteries. 03:04 Your right colic territory is somewhere down there. 03:09 If this patient has got a metastatic disease, tumor would have already spread all the way up there. 03:18 That's why you are resecting more of the colon. 03:21 One is to do the blood supply and two is to do the lymphatic drainage because the tumor has spread. 03:29 That would have been the area it would have spread to. 03:32 It could have even disseminated further. 03:34 You never know. 03:35 But most likely even through submucosal spread, it will go until there. 03:40 So, it's safe to take this much, okay? Tumor here, ascending colon in the hepatic flexure, what's the most appropriate surgery? It's fine. 04:05 Absolutely. That's called the extended right hemi. 04:07 It's still the same principle. 04:09 You are going to the middle colic territory as well. 04:12 This is your right colic. 04:14 You're just going to the middle colic territory and taking that much off. 04:19 Your answer to the exam is extended right hemi simply because these are the levels they are going to give you. 04:26 The next level they’ll give you will be, to confuse you, will be here, transverse colon. 04:34 One of the options they always give is a transverse colectomy. 04:37 Would you do that? No such thing. 04:39 Huh? No such thing. 04:41 There is such - something called transverse colectomy. 04:43 You can do but would you even really do for a tumor. 04:46 So, if you have a tumor here, what do you do? Can you see that? He’s got a tumor in the transverse colon right there. 04:55 Extended hemi? Extended what, hemi right or left? Extended right hemi. 04:59 Absolutely. Well,extended right or left. Both are acceptable. 05:02 If this is more towards that side, you could have gone for extended right or if it did towards this side, you can go for extended left. It doesn't matter. 05:12 But the answer is extended right hemi or extended left hemi. 05:15 No transverse colectomy because when you do transverse colectomy, you're going across two or three different territories. 05:20 You're going across right colic, middle colic, left colic. 05:24 So, you’re totally sort of buggering up the entire lymphatic drainage. 05:29 So, you try not to do a transverse colectomy. 05:32 Now, the next bits are easy. 05:34 If you are having a splenic flexure tumor, we either go for a left hemicolectomy or an extended left hemi depending on how far it has gone. 05:45 If you’re just on the splenic flexure, you can probably get away with a straightforward left hemi because you're taking off the left colic artery’s area. 05:56 Then you come to the sigmoid colon or descending colon. 06:01 Again, left hemi is fine, but if in the sigmoid colon because you have the sigmoid artery for its own, you can do a sigmoid colectomy. 06:10 Then you’ve come down further, upper part of the rectum. 06:15 So, say superior one-third of the rectum, what do you do? Anterior resection. 06:18 Anterior resection, okay. 06:20 Until where do you do anterior resection? Until the dentate line. 06:26 Dentate line or until you can’t preserve the anal sphincter. 06:29 If you can't preserve the anal sphincter, there’s absolutely no point in doing anterior resection. 06:33 You can already go for an AP resection. 06:35 So, the upper rectal tumors, you go for anterior resection; lower rectal or anal cancer, you go for AP resection. 06:46 So, these are the choices they give you. 06:48 Then the other things they'll give you will be Hartmann's. 06:52 When you do it, is there any indication for Hartmann's in this? We see an incumbent perforation. 06:58 Okay, very good, go on. Tell me more about Hartmann’s. 07:00 Hartmann's is an emergency procedure essentially where basically you’re taking out the affected part of the bowel. 07:09 If you’re doing it in a cancer, for perforation secondary to cancer, then you would do as much as you would need to do to ideally clear everything in one operation but rather than perform primary anastomosis, well, you might perform primary anastomosis but you will pull out the stoma ... 07:27 That’s right. Hartmann's is not a definitive procedure. 07:30 Hartmann's is more of a temporary emergency or a life-saving procedure. 07:35 You inevitably bring it towards the stoma. 07:37 The classical thing, what we see is a left-sided tumor, perforated or a diverticular disease, perforated or about to perforate. 07:46 You’re just going to anastomose this and this back because it's all infected or there's tumor. 07:52 So, what do you do? You bring this out as a stoma, and then this part, the inside bit, either you bring it out as a mucous fistula or you leave it back in, leave it in the bowel. 08:06 Then when this all cleared up, you can do an end-to-end anastomosis. 08:11 So, Hartmann's is an emergency procedure. 08:14 It is not a definitive procedure for any tumor. 08:17 A definitive procedure for any cancer is resection of the entire bowel. 08:22 Then your options are either to have a temporary colostomy or a permanent colostomy. 08:30 When do you decide to have a permanent colostomy? If you’re removing the entire bowel for something like diverticulitis and protocolectomy or subtotal colectomy then you have permanent colostomy or if anastomosis isn’t feasible. 08:52 Yeah, yes. That's right. 08:52 Temporary colostomy is more of a defunctioning colostomy. 08:55 So, imagine you have a tumor here. 08:59 You brought this out as a stoma. 09:01 You're just waiting for further staging, maybe radiotherapy. 09:07 You have cleared out everything. 09:08 Then you put it all back together. 09:09 That's your temporary stoma and that's your Hartmann's. 09:15 Well, not Hartmann's. 09:16 That's more of a temporary defunctioning colostomy. 09:18 Permanent colostomy, sometimes we have to do when you had to resect a lot of the lower rectum or the anal canal, there's nothing to anastomose. 09:28 You have gone all the way up, lower down the sigmoid. 09:31 You have done an AP resection. 09:33 This is where I go down to anastomose. 09:34 You have to bring it out as a stoma. 09:36 So, that is a permanent colostomy.
About the Lecture
The lecture Colorectal Tumor by Stuart Enoch, PhD is from the course Upper Part of the Body Anatomy.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |