Playlist
Show Playlist
Hide Playlist
Bronchiolitis: Causes and Risks
-
Slides Bronchiolitis.pdf
-
Download Lecture Overview
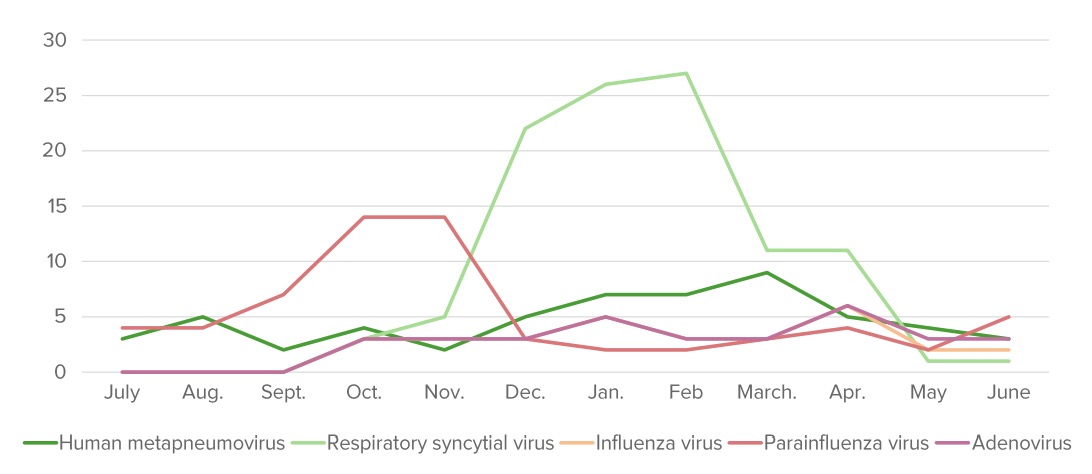
00:02 In this lecture, we’re going to talk about bronchiolitis, which is a viral infection of the lower airways of a child. 00:11 So we in pediatrics see this almost every day. 00:15 This is the number one cause of hospitalization in the United States. 00:18 A child, perhaps 16 months of age, and the parents noted that today he’s had increased work of breathing. 00:25 You noticed some wheezing on exam, he has a copious runny nose, he’s been having fever, and he’s had decreased oral intake for about the last two days. 00:35 What’s your medical diagnosis? It’s probably bronchiolitis. 00:40 So bronchiolitis is the inflammation of the bronchioles, which are the smallest air passages of the lungs. 00:47 This narrowing of the airways as a result of accrual of mucus is what causes children to develop respiratory distress. 00:55 Children have weaker respiratory musculature so it’s harder for them to clear the mucus out of their lower airways. 01:06 At its peak, RSV accounts for about a third of bronchiolitis so we frequently think of RSV when we think of bronchiolitis. 01:16 And as you can see here, RSV is much more popular in the winter months than in the summer months. 01:24 This may be because children are more likely to be in enclosed areas where they can share viruses, but because there are other viruses that happen at other times of the year, it’s not entirely clear why we have this seasonal variation of RSV. 01:40 So, other than RSV, what else causes bronchiolitis? Well, influenza could certainly cause bronchiolitis. 01:49 Rhinovirus can actually cause fairly severe bronchiolitis. 01:53 The parainfluenza virus is what we normally think is causing croup, but also can cause bronchiolitis, as can adenovirus. 02:02 Children with adenovirus can be very, very sick. 02:05 Human metapneumovirus is a relatively new comer on the stage, which we didn’t know about much before the mid-1980s. 02:13 Bocavirus maybe causes bronchiolitis or maybe it’s a virus we’ve just found in our studies that goes along for the ride. 02:22 There may be Middle Eastern respiratory syndrome virus or severe and acute respiratory syndrome virus. 02:31 There are lots of viruses out there and probably thousands we don’t even know about. 02:38 And each virus has its own season. 02:42 So here, you can see the familiar green line of RSV, but also you can see that the red line of parainfluenza is happening a little bit earlier and some of the other viruses are sort of just lingering along all year long. 02:57 So all of that together, we do typically see the bronchiolitis season starting around October and ending around May, with the summer seeing less but absolutely not zero bronchiolitis. 03:12 There is one state, Florida, where they have RSV almost year-round and nobody knows why. 03:20 So does it matter though what virus is causing bronchiolitis? The fact is rapid viral panels are somewhat expensive depending on where you are and knowing the virus doesn’t seem to really matter in terms of your plan of care. 03:37 As a result, the AAP recommends not screening for types of viruses. 03:42 Chances are the American hospital where you’re working is screening and that is against the recommendations of the American Academy of Pediatrics and this is because knowing does not affect the management of the patient. 03:55 We’re going to base our management of the patient on how sick the patient is, not which kind of virus they have. 04:01 Some viruses may cause generally worse disease, like RSV, but we’ll treat them based on what their severity of illness is, not based on the virus. 04:11 So what puts kids at risk for bronchiolitis? There are a number of things that are known to be risk factors, although it’s not entirely clear why. 04:21 So, socioeconomic status does play into risk for bronchiolitis. 04:25 Mothers who didn’t study past high school are more likely to have children admitted for bronchiolitis. 04:32 Crowding in the home, two or more children to a bedroom increases risk of bronchiolitis. 04:37 Having school-age siblings increases the risk of bronchiolitis. 04:42 Breastfeeding is protective. 04:44 This is because the mother may have the virus, as well, and extrude antibodies against that virus in her breastmilk, which then protects the infant who is eating the breastmilk. 04:55 So failing to breastfeed is a risk factor independently for a child being hospitalized with bronchiolitis. 05:04 Passive smoke exposure is a risk factor for bronchiolitis. 05:08 Children who have a particulate environment are more likely to have problems with their lung function and are more likely to be hospitalized when they get that inevitable viral infection. 05:19 Attendance in daycare is a risk factor because if you’re around children with viruses, well, you’re more likely to get one. 05:27 And the last point seems fairly obvious, since younger children are more likely to get severe bronchiolitis, if you’re born early in the year and you’re less than six months old at the start of the season of bronchiolitis, you’re more likely to be hospitalized simply because you are younger during the outbreak of the illness.
About the Lecture
The lecture Bronchiolitis: Causes and Risks by Brian Alverson, MD is from the course Pediatric Pulmonology.
Included Quiz Questions
Which of the following is a risk factor for hospitalization with bronchiolitis?
- Passive smoke exposure
- Cockroaches in the home
- Breastfeeding
- Being a single child
- Being older than 6 months of age
A 16-month-old boy is brought to the physician by his parents with a copious runny nose, fever and decreased oral intake during the month of November. All of the following viruses may be the causative agent, EXCEPT?
- Herpes virus
- Rhinovirus
- Respiratory Syncytial Virus
- Para Influenza virus
- Influenza virus
Which of the following is the number-one cause of hospitalization of children in the United States?
- Bronchiolitis
- Diarrhea
- Constipation
- Asthma
- Trauma by fall
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Another great lecture, where all the following are covered: - Myths: oxygen, etc. - Asthma vs Bronchiolitis - Pavalizumab - Current literature on brochiolitis - Experience from an advanced practitioner I work in a Swiss hospital and even though we follow as much as possible the AAP recommendation, we are not all the time up-to-date.