Playlist
Show Playlist
Hide Playlist
Atherosclerosis: Histopathologic Consequences
-
Slides 01 VascularMedicine advanced.pdf
-
Reference List Vascular Medicine.pdf
-
Download Lecture Overview
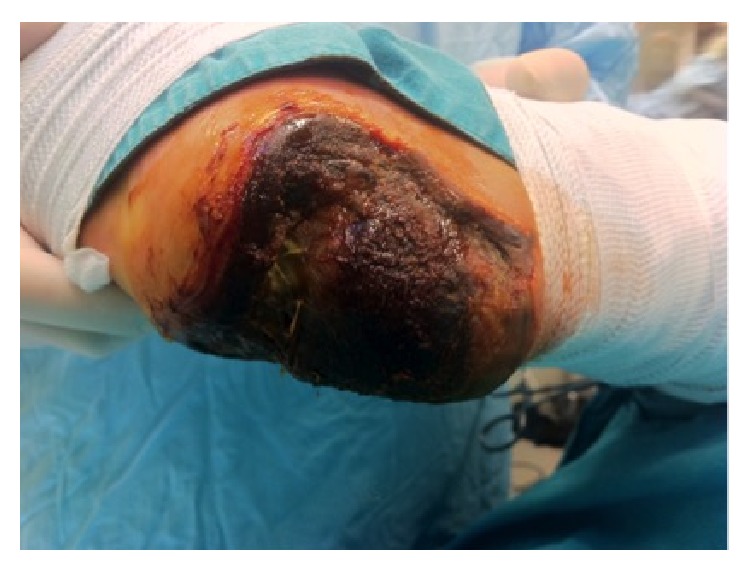
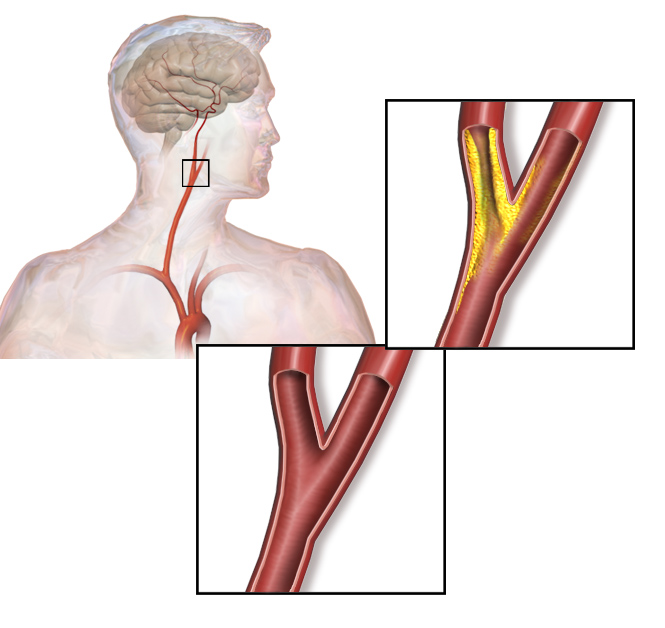
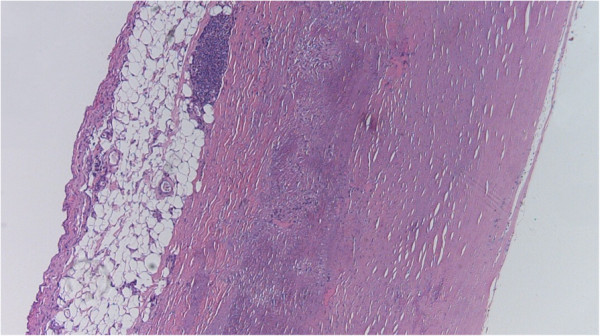
00:01 Here is an example of atheroma under the microscope. 00:05 You can see all these little what look like needles and little, round holes. All of those are accumulation of cholesterol in the artery, and mixed in there is lots of scar tissue. 00:20 And you can see that this material is under the tunica intima—that is, the top layer of the arterial wall that's right up against the channel. In this picture, you can actually see the little white needles where there had been cholesterol crystals collected in this atherosclerotic plaque. Now, sometimes, an embolus will travel in the bloodstream and get stuck at a point where there is atherosclerotic narrowing of the blood vessel, and when that embolus causes obstruction, again, you can start to have death of tissue beyond that. 00:58 So there's two kinds of pathophysiology here (abnormal physiology): the atherosclerotic process and then the blood clot process. And the two of them often interact to cause a lot of symptoms and even fatal illness. So let's take an example of atherosclerosis. 01:21 Let's take the carotid artery. Here, in this little cartoon, you see narrowing, or constriction, of the inner surface, the lumen—that is, the channel of the carotid artery. And this is almost always caused by atherosclerosis. This accounts for 25% of all strokes, and the stroke can also be the result of embolization from the left atrium in atrial fibrillation, as we said. That's also a common cause of stroke. Detection by physical exam of the narrowing is very poor. I mentioned before: Sometimes you'll hear a bruit or a turbulent blood flow, a sort of "ch—ch—ch" when you put your stethoscope over the neck. But often, there's no sound, and the only way to detect it is with, usually, an ultrasound examination. And you can see, in this little cartoon, there is a narrowing in the carotid artery which, if that became severe, patients might start to have symptoms: brief symptoms where they lose their ability to speak, or where their hand becomes lame or numb and then it gets better. Eventually, when there's a complete blockage in that artery, the stroke won't get better. So in the lower extremity, that in the legs, as I mentioned before in the basic series, patients develop so-called intermittent claudication—that is, intermittent pain and cramping while walking that goes away with rest. Why does that happen? Because during walking, the muscle requires more blood flow. 03:03 And then, when not enough blood flow gets through, the muscle starts to give a signal of pain. When the patient stops, the blood flow gets through again, the muscle demand goes down, and the pain goes away. When the atherosclerotic narrowing in the legs is severe, you can start to get some severe changes in the leg, such as hair loss or shiny, thin skin. And eventually, you may even have death of tissue, usually of the toes—blackened areas—and I'll show some pictures later of areas of gangrene on the toes and the fingertips.
About the Lecture
The lecture Atherosclerosis: Histopathologic Consequences by Joseph Alpert, MD is from the course Arterial Diseases.
Included Quiz Questions
Atheroma forms in which layer of the blood vessel?
- Tunica Intima.
- Tunica externa.
- Tunica media.
- Outer epithelium.
- Endothelium.
In case of carotid artery stenosis which of the following may be seen temporarily in the patient?
- Inability to speak.
- Pale complexion.
- Blurry vision.
- Loss of balance.
- Dry nose.
Lower extremity arterial disease could lead to which of the following?
- Gangrene
- Increased temperature
- Redness in the affected area
- Pain during rest in the affected area
- Complete loss of sensation
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |