Playlist
Show Playlist
Hide Playlist
Apnea of Prematurity and Necrotizing Enterocolitis (NEC)
-
Slides Prematurity Pediatrics.pdf
-
Download Lecture Overview
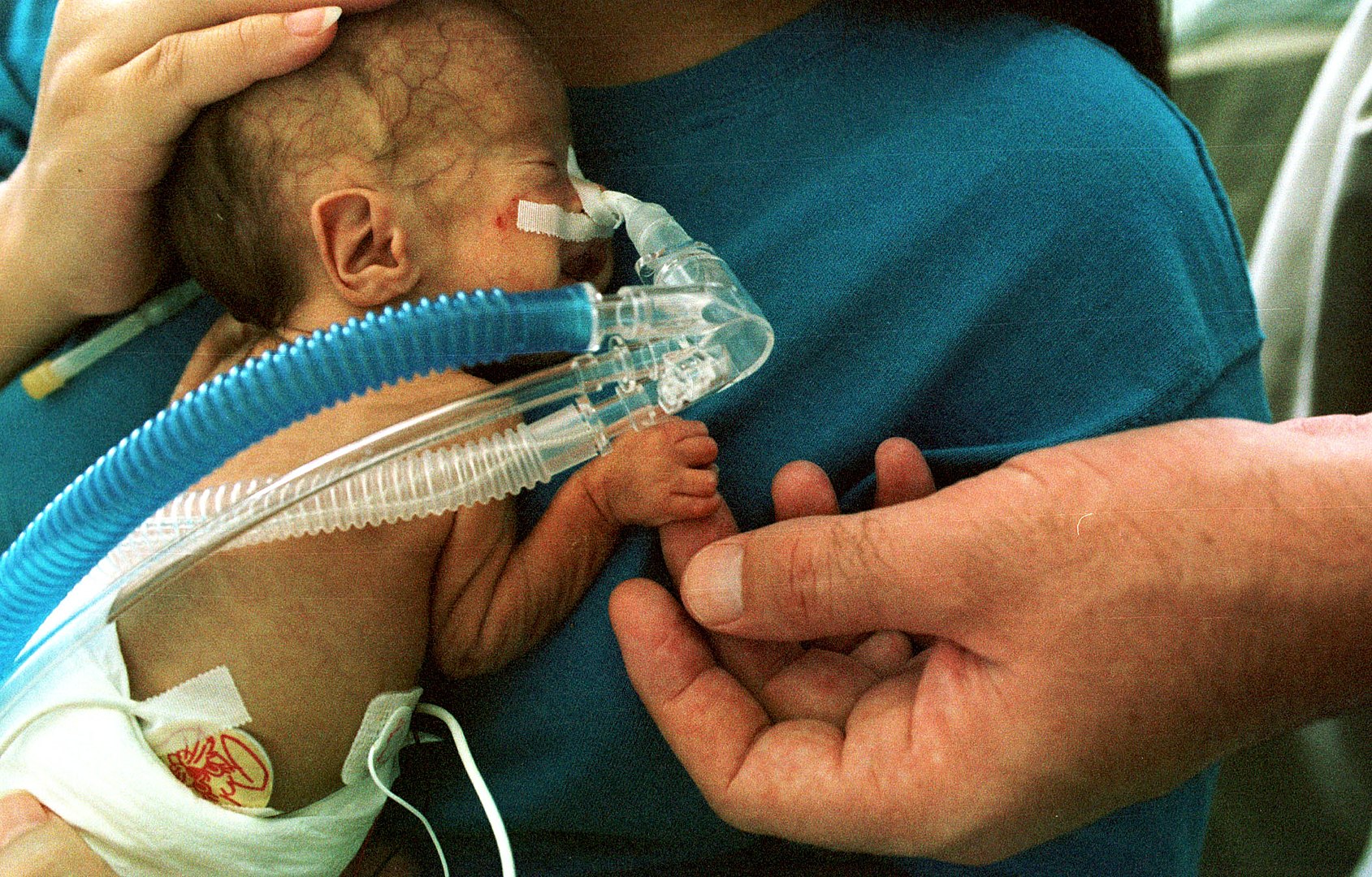
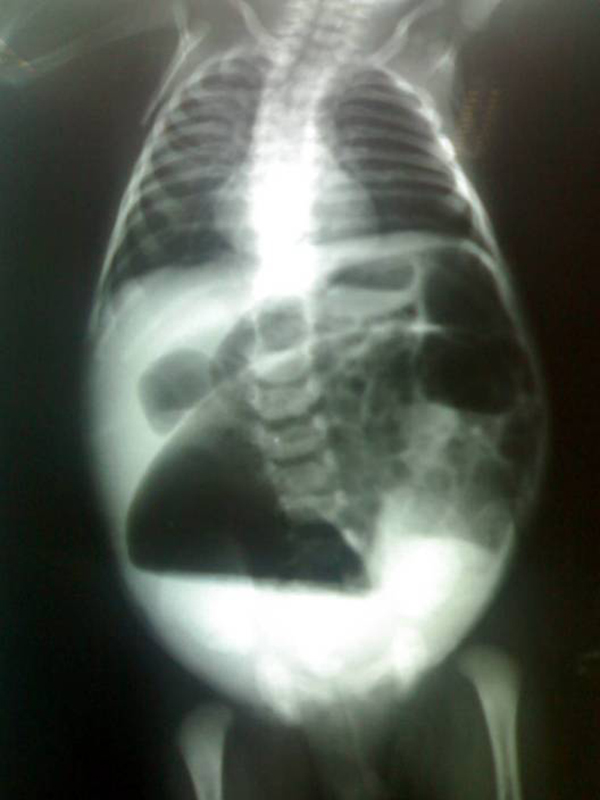
00:01 Okay, let’s talk about apnea of prematurity. 00:04 This happens in premature infants presumably because their brains haven’t developed enough to remind them to breathe. 00:11 This usually goes away as they age. 00:14 We define apnea of prematurity as a cessation of breathing for more than 20 seconds. 00:19 Remember, normal newborns may hold their breath for 15 seconds and that’s just fine. 00:24 They’re just a little premature. 00:26 Okay. 00:28 Ninety percent of infants who are under 1 kilo will have apnea of prematurity. 00:33 It’s a common problem due to CNS immaturity. 00:38 We need to differentiate this apnea, however, from things like sepsis or hypoglycemia or electrolyte imbalances or bleeds inside the brain like IVH or seizure. 00:50 All of these are possibilities. 00:52 So as a result with these infants, we will monitor them. 00:55 We will give them supportive care and we may provide CPAP as a way of preventing them from having significant apneic episodes. 01:03 Eventually, we may not want to have them on a breathing machine or be giving them the supportive care, so we would give them caffeine. 01:11 Caffeine is effective at reducing apnea episodes in premature infants. 01:18 Let’s switch gears to another common problem in premature infants which is necrotizing enterocolitis or NEC. 01:26 This is an ischemic necrosis of immature intestines in an infant. 01:31 This can happen between 1 and 8% of infants depending on how premature that group of infant is. 01:38 It is associated with extreme prematurity, intrauterine growth retardation or a patent ductus arteriosus. 01:47 And it typically happens right after the first feed. 01:51 Here’s why. 01:52 The baby’s intestine is pretty much sterile. 01:56 As this infant is having a vascular supply issue with their intestines or poor blood flow to their intestines, we introduce food in trophic amounts, tiny amounts, to allow the intestines to start growing. 02:13 Shortly thereafter, we’ve also been introducing bacteria and some of those bacteria can somehow get into the intestinal wall and start growing inside the intestinal wall. 02:24 An x-ray might reveal air in the wall. 02:27 If that goes too far, it can actually perforate the abdomen and that can cause peritonitis. 02:33 These kids can get very sick. 02:36 So again, feeding intolerance in an infant, they start having increased residuals after they feed. 02:44 They then develop temperature instability and that may be our first clue. 02:48 Then, they start having bloody stools and that is a real clue that something is going wrong. 02:53 We may notice abdominal distension or discoloration of the abdomen as you can see in this patient. 03:01 In fact, the NICU nurses are usually measuring abdominal girths in these infants and will notice when they go up acutely and say, “Aha! Here’s the problem.” Patients may develop apnea just from being sick and they may develop hypotension if they become septic. 03:19 Labs we get for NEC include a CBC which may show anemia, thrombocytopenia or a high white count. 03:26 We will often stool occult the stool just to check and see if there is blood in the stool. 03:32 That can be a clue. 03:34 And what’s classic is we get an abdominal x-ray which shows dilated bowel loops and may show pneumatosis, air in that portal tract or air right under the diaphragm. 03:43 That’s certainly a key. 03:46 So how do we manage NEC? Unfortunately, some of these infants can go to surgery, but first we’ll usually try medical NEC which means a medical treatment. 03:56 What we do is we provide supportive care. 03:58 We will make them NPO. 04:00 We may do rectal and gastric decompression by suction perhaps. 04:05 And then we will usually provide antibiotics, broad spectrum antibiotics because the intestines tend to have a broad spectrum of bacteria. 04:13 Sometimes that will do it, but other times they go on to get sicker and it requires surgery. 04:20 We hate it when it requires surgery because, well, sometimes they only need to resect a small amount of bowel. 04:26 If it’s gone on for a while or it’s particularly severe, they have to resect a large amount of bowel. 04:32 Patients who have a large amount of bowel resection may go on to develop something we call short gut syndrome. 04:40 This is incredibly challenging to deal with. 04:42 These infants don’t have enough intestine to absorb the amount of nutrients they need. 04:48 They may end up on hyperalimentation which eventually leads to liver failure and death. 04:54 Or they may require an intestinal transplant, which unfortunately doesn’t have a great prognosis. 05:01 So there are ways we can prevent infants from getting NEC. 05:04 One is slow trophic feeds. 05:07 When they’re premature, we start it really slow and very gradual in moving up and that allows the intestine to develop with the trophic feeds. 05:17 Those are feeds that are providing nutrients so that intestine can develop until it’s ready to take more full feeds. 05:23 The other key is to use breast milk. 05:25 For reasons I don’t know, patients tend to do a little bit better with breast milk than they do with formula.
About the Lecture
The lecture Apnea of Prematurity and Necrotizing Enterocolitis (NEC) by Brian Alverson, MD is from the course Neonatology (Newborn Medicine). It contains the following chapters:
- Apnea of Prematurity
- Necrotizing Enterocolitis (NEC)
Included Quiz Questions
Which of the following is true about apnea of prematurity?
- It may be defined as a cessation of breathing for more than 20 seconds.
- It is due to maternal consumption of caffeine.
- It is caused by sepsis.
- It is caused by hypoglycemia.
- It reflects an underlying seizure disorder.
Approximately what percentage of premature babies under 1 kg have apnea of prematurity?
- 90%
- 50%
- 70%
- 80%
- 100%
Which of the following is not a typical clinical manifestation of neonatal necrotizing enterocolitis?
- Jaundice
- Feeding intolerance
- Temperature instability
- Bloody stool
- Abdominal distension
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
That very well summarized and understandable, very good way to reinforce knowledge
Excellent lecture: clear, concise, good overview of the diseases and the management.