Playlist
Show Playlist
Hide Playlist
Amebic Liver Abscess
-
Slides BenignLiverMasses Surgery.pdf
-
Download Lecture Overview
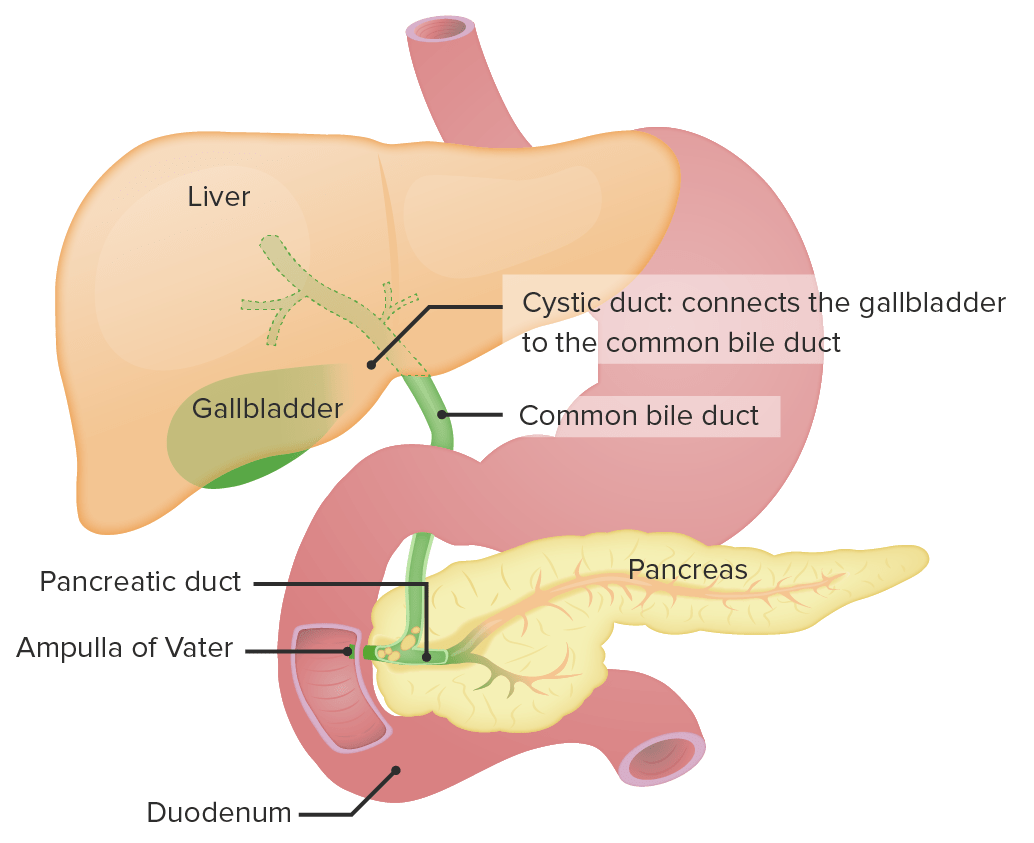
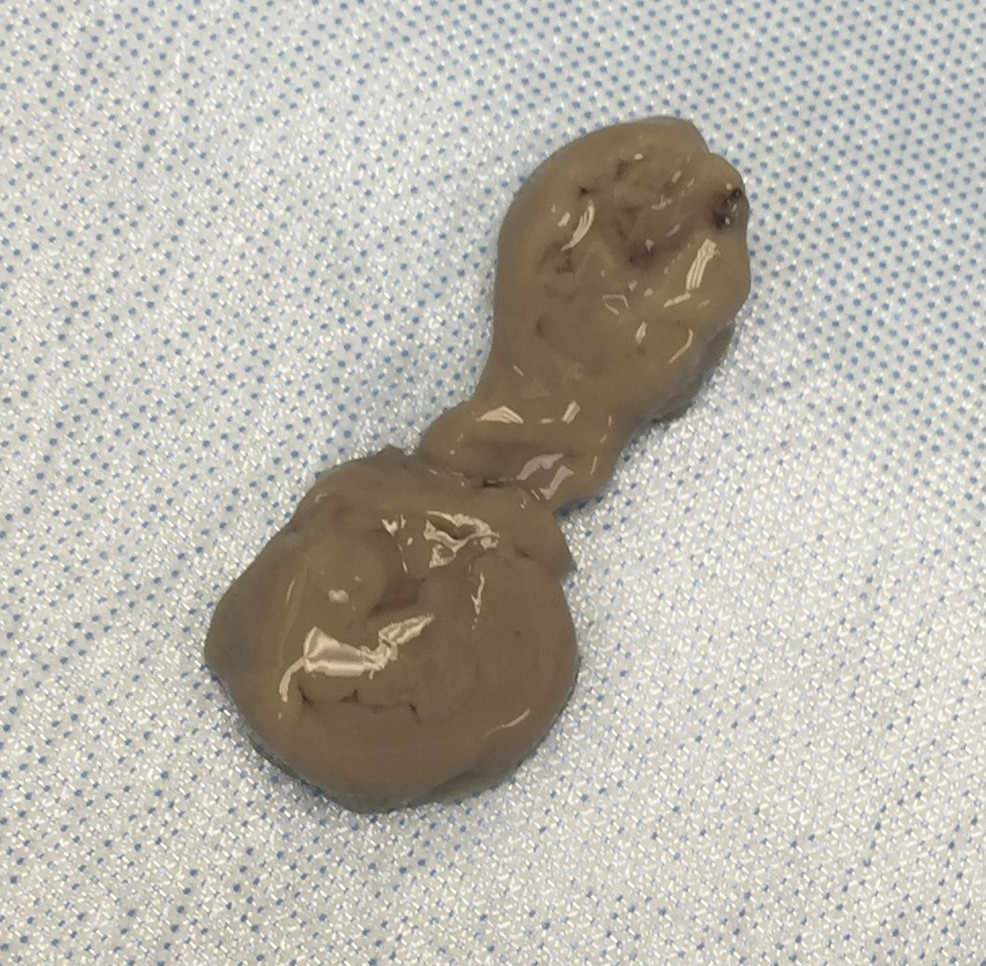
00:01 Let’s move on to a discussion of liver abscesses. We’ll focus on amebic and pyogenic liver abscesses. 00:09 Let’s begin with amebic abscesses. This is a picture of a pathology after the drainage of pus from a liver. 00:19 You’ll notice that the pus is in central region of this picture. Amebic abscesses are classically associated with some recent travel to indigenous regions usually in the subtropics such as Mexico or India. 00:34 Organism involved is a protozoan Entamoeba histolytica. Demonstrating symptoms are usually between 8 and 12 weeks after the exposure. It’s suspected to be a fecal-oral contamination. This is an important slide describing a portal circulation explaining how the Entamoeba histolytica which has oral feces transmission can end up in the liver. Once a protozoan enters the colon, it follows the green arrow. 01:08 The green arrow shows where the colon drains into the superior mesenteric venous system that then has a confluence onto the portal system. As you know, the liver’s blood supply is 75% contributed by the portal vein. This is how Entamoeba histolytica obtains access to the liver and sets up shop causing an abscess. I have a question for you. What are some potential complications of amebic abscesses? I’ll give you a second to think about this. The answer is the biggest fear is rupture. Rupture or extension of the abscess into the abdomen, pleural space, or extension to the pericardium particularly from the left lobe of the liver can cause significant problems. If the rupture occurs in the abdomen, it can cause peritonitis creating a surgical abdomen. If the rupture happens into the pleural space, patients may complain of difficulty breathing. It can lead to an empyema or an abscess collection in the lung. Lastly, because of the proximity of the left lobe of the liver to the pericardium, this can cause pericarditis and an abscess in the heart.
About the Lecture
The lecture Amebic Liver Abscess by Kevin Pei, MD is from the course General Surgery.
Included Quiz Questions
Which of the following is NOT true about amoebic liver abscesses?
- The left lobe of the liver is more commonly affected than the right lobe.
- Liver abscess is the most frequent extraintestinal manifestation of Entamoeba histolytica infection.
- Entamoeba histolytica enters the portal venous system from the colon.
- The highest prevalence is found in developing countries in the tropics, particularly in Mexico and India.
- Symptoms take 8 to 12 weeks after being infected to appear.
Which of the following is NOT a complication of an amoebic liver abscess?
- Pathologic involvement of the central nervous system
- Cardiac involvement following the rupture of an abscess involving the left lobe of the liver
- Rupture of a liver abscess into the chest cavity
- Intraperitoneal rupture
- Empyema
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |