Playlist
Show Playlist
Hide Playlist
Acute inflammatory, Type I interferon and NK cell responses
-
Slides Innate Immune System.pdf
-
Reference List Immune System.pdf
-
Download Lecture Overview
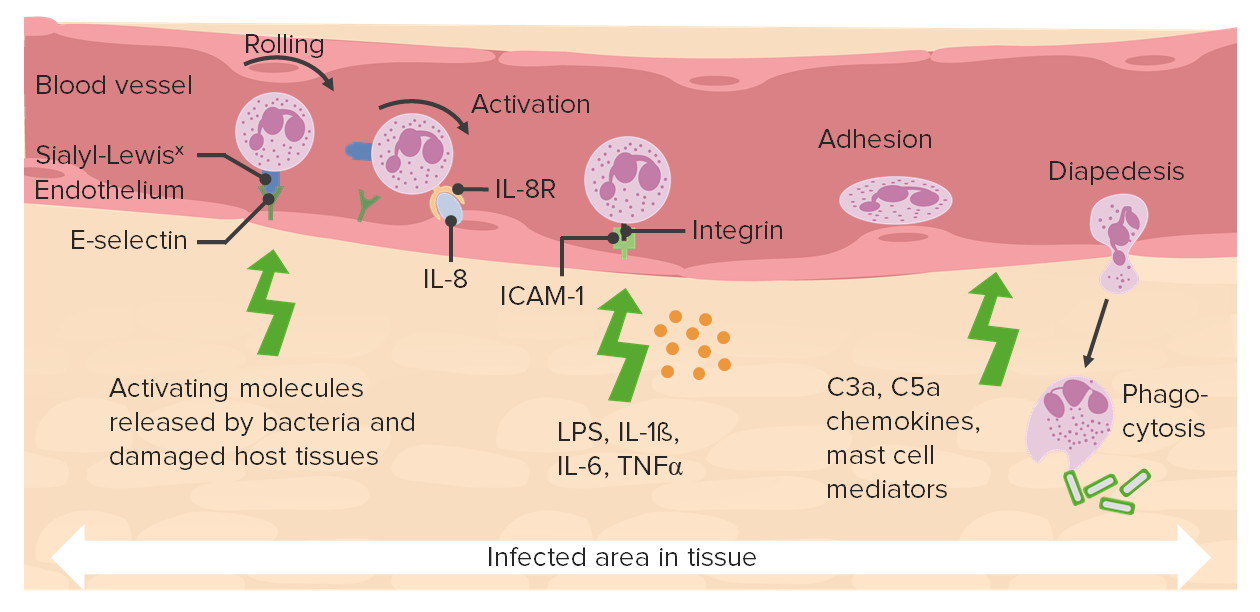
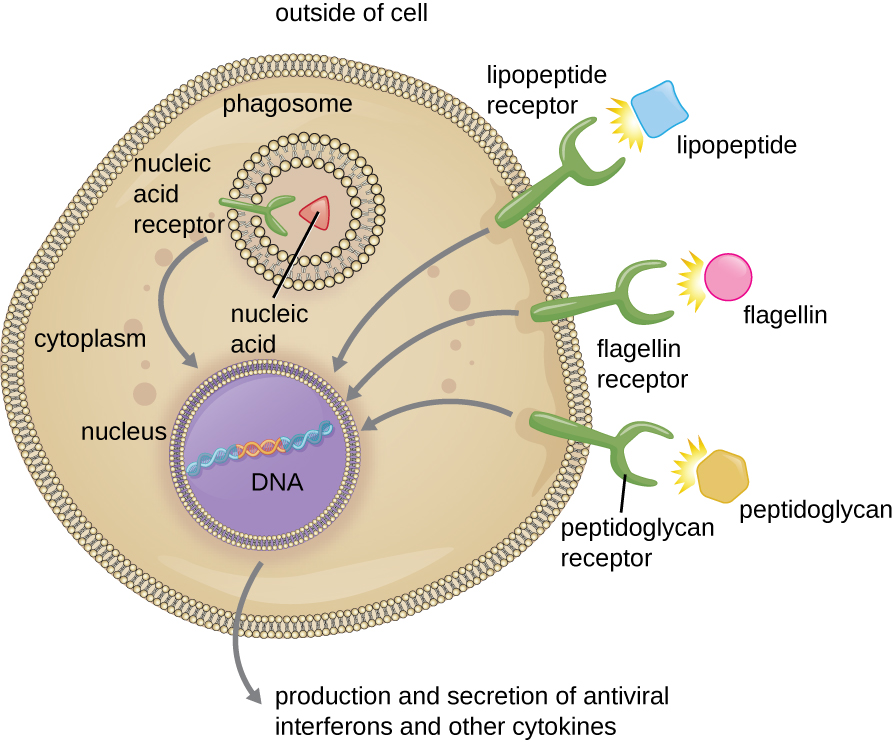
00:01 So let’s look at what actually happens when you have an area of tissue that’s infected. 00:11 So, overlying that tissue will be a blood vessel, as we can see at the top on this slide. 00:16 And you’ll see a neutrophil, multilobed nucleus very typical of a neutrophil. 00:24 And normally this neutrophil along with all the other white blood cells and red blood cells will be racing through the blood vessel, doesn’t need to stop. 00:32 It just needs to carry on its journey. 00:34 But if there’s an infection in the tissues, those neutrophils and other immune system cells need to be alerted to the fact that there’s an infection. 00:43 So how does that happen? It happens by adhesion molecules becoming expressed on the blood vessel endothelium. 00:53 It’s a bit like putting your hand out to stop the bus. 00:55 Okay? You need to stop that neutrophil. 00:59 You need to tell it, “Stop! Leave the blood vessel, get out into the tissue because there’s an infection that you need to deal with." So a variety of adhesion molecules become expressed on the blood vessel endothelium. 01:12 For example: E-selectin. 01:16 E-selectin gets expressed on the surface of the blood vessel endothelium in response to activating molecules that are released both by the infectious agents themselves, for example bacteria, but also by any damaged host tissues. 01:33 In other words, our own cells that become damaged as a result of that infection. 01:38 And the neutrophil begins to slow down in its journey, and it begins to roll along the blood vessel wall. 01:47 A consequence of that is that other molecules begin to get expressed on the surface of the neutrophil. 01:55 For example: a receptor for the cytokine interleukin-8. 02:00 In other words, the interleukin-8 receptor. 02:03 And the interleukin-8 receptor on the surface of the neutrophil can then be recognized by interleukin-8 on the blood vessel endothelium. 02:15 Other molecules begin to be expressed. 02:18 So for example, integrin molecules begin to be expressed on the surface of the neutrophil. 02:23 And these bind to the cell adhesion molecule ICAM-1 that now additionally becomes expressed on the endothelium in response to substances like lipopolysaccharide from Gram-negative bacteria, and cytokines that the response is producing, like interleukin-1β, interleukin-6 and tumor necrosis factor α. 02:44 So you see, from an initial start with just recognition of one adhesion molecule, CD15 by E-selectin on the blood vessel endothelium. 02:53 This response really gets going. 02:55 Lots of additional adhesion molecules get expressed, both on the blood vessel endothelium and on the neutrophil. 03:01 And this leads to activation of the neutrophil and very, very firm adhesion. 03:07 So initially the neutrophil is just rolling along the blood vessel wall, but it comes to a complete stop. 03:13 And then it squeezes through the gaps between the blood vessel endothelial cells attracted to the site of the infection by complement components such as C3a and particularly C5a by chemotactic cytokines, in other words the chemokines. 03:30 And also, mast cell mediators are involved in this process of permitting the neutrophil to leave the blood circulation and enter the tissues to get to the area where there’s an infection. 03:45 And this process of squeezing through the blood vessel endothelium, between the junctions between the blood vessel endothelium, is called diapodesis. 03:56 And ultimately, the neutrophil will reach its destination where the infectious material is. 04:03 So just a couple of other things to round off now, whilst we’re looking at innate inflammatory responses in the innate immune response. 04:15 There are a variety of different cytokines that are referred to as interferons. 04:19 And there are two particular interferons that are referred to as Type I interferons. 04:24 They’re called interferon α and interferon β. 04:28 And following an infection with a virus, and replication of viruses within the infected cell, one of the results is that cells-- and virtually all cells in the body can do this, they produce interferon α and interferon β. 04:46 The consequence of that production of interferon α and interferon β is that there is the production in response to those cytokines, there is a production of proteins inside cells, surrounding the area where there’s an infection. 05:01 And these proteins prevent viral replication. 05:04 So the cells surrounding the area of the infection are no longer able to permit replication of the virus. 05:12 So there may be transmission of the virus from one cell to another, but that’s it. 05:17 Virus can’t then replicate in the surrounding cells. 05:20 And this prevents the spread of the virus. 05:23 A very important type of response, the Type I interferon response. 05:27 Another important aspect of innate immunity is the so called natural killer cell, NK cell. 05:35 These are cells that patrol around the body looking for abnormal cells. 05:42 Normally, all of our nucleated cells have on their cell surface a variety of different molecules, including a group of molecules called MHC Class I. 05:53 What the natural killer cell does is it goes round looking at every single cell in the body, looking to see if a cell does not have MHC Class I. 06:03 And I’ve just told you, all nucleated cells have MHC Class I, so if there’s no MHC Class I there, there’s something really strange or odd about that cell. 06:11 And one of the things that can happen when a cell becomes infected with a virus, is it can lose expression of MHC Class I. 06:19 So there needs to be some way of picking up on that. 06:22 That’s what natural killer cells do. 06:24 Essentially they have two groups of receptors on their cell surface - activating receptors and inhibitory receptors. 06:31 And the activating receptors will look for a variety of different molecules on the surface of the cells, apart from MHC Class I, a variety of other molecules that are normally expressed on all nucleated cells. 06:44 And they’ll send an activation signal into the natural killer cell, telling it to kill that cell. 06:49 And these activating signals come through protein tyrosine kinases that add phosphates to a signaling pathway to initiate that pathway. 07:01 But you don’t want to kill a normal cell. 07:04 So to prevent that killing occurring all the time, as well as having activating receptors, the natural killer cells have inhibitory receptors. 07:15 And those inhibitory receptors are linked to protein tyrosine phosphatases. 07:21 And they remove the phosphate groups and prevent activation of the natural killer cells. 07:26 So normally, the natural killer cell is not activated and there is no cell killing. 07:33 However, if a cell has become infected with a virus and has lost MHC Class I, then there is signaling through the activating receptors, but there is no signaling through the inhibitory receptors. 07:44 Because if there’s no MHC Class I, you can’t signal through the inhibitory receptor. 07:49 That activating signal isn’t overwritten and the infected cell becomes killed by the natural killer cell. 07:57 So hopefully you now understand the role of inflammation in innate immunity and the way that the innate immune response deals with infection and tissue damage.
About the Lecture
The lecture Acute inflammatory, Type I interferon and NK cell responses by Peter Delves, PhD is from the course Innate Immune System. It contains the following chapters:
- The Acute Inflammatory Response
- The Type I Interferon Response
- NK Cell Activating and Inhibitory Receptors
Included Quiz Questions
During neutrophil activation, integrin molecules on the surface of neutrophils typically bind to which molecule on the surface of the blood vessel endothelium?
- Intercellular adhesion molecule 1 (ICAM-1)
- Interleukin 8 (IL-8)
- Pathogen-associated molecular pattern (PAMP)
- Lipopolysaccharides (LPS)
- Interleukin 1ß (IL-1ß)
Which of the following is the correct order of neutrophil migration from the blood to damaged tissue?
- Rolling, Activation, Adhesion, Diapedesis
- Activation, Rolling, Adhesion, Diapedesis
- Activation, Adhesion, Rolling, Diapedesis
- Rolling, Activation, Diapedesis, Adhesion
- Rolling, Adhesion, Activation, Diapedesis
Regarding interferon-alpha and beta, what is the mechanism of their action against viral infections?
- They are released by a virus-infected cell and cause nearby cells to heighten their anti-viral defenses.
- They are released by a virus-infected cell and attach directly to a virus, preventing it from entering other cells.
- They signal the innate immune system to respond to viral antigens with phagocytes.
- They bind to a cell that has been infected by a virus and prevent it from pyroptosis.
- They bind to a cell and activate the classical component pathway.
What is a possible mechanism by which natural killer cells recognize and destroy virus-infected cells?
- Low levels of MHC class I molecules are not recognized by inhibitory receptors on natural killer cells.
- High levels of MHC class I molecules suppress inhibitory receptors on natural killer cells.
- Low levels of MHC class I molecules avoid recognition by stimulatory receptors on natural killer cells.
- High levels of MHC class I molecules are recognized by inhibitory receptors on natural killer cells.
- High levels of MHC class I molecules are recognized by stimulatory receptors on natural killer cells.
Which of the following mechanisms allows normal cells to avoid destruction by natural killer cells?
- A more prominent signaling of inhibitory receptors on the natural killer cell
- A more prominent signaling of stimulatory receptors on the natural killer cell
- A more prominent signaling of stimulatory receptors on the normal cell
- A more prominent signaling of inhibitory receptors on the normal cell
Customer reviews
4,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
1 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Way better than the 3 hour lecture at our school. Thank you.
When you touched on leukocyte migration, you began at the stage of "adhesion" when many medical students should include the first two steps before this. It should include Margination, where leukocytes follow lamina flow while being pushed by erythrocytes onto the barriers of the endothelial cells, then rolling, where selectin proteins are adhesion molecules which weakly attach onto these leukocytes causing them to "roll" .... and then do i believe you should be able to talk about the adhesion and transmigration parts. If you could add this in, it would be quite useful. especially because many students are trusting these lecture to have the utmost information. Thank you very much. When you spoke on the topic itself though, it was quite organised and detailed.