Playlist
Show Playlist
Hide Playlist
Acute Inflammation
-
Slides Innate Immune System.pdf
-
Reference List Immune System.pdf
-
Download Lecture Overview
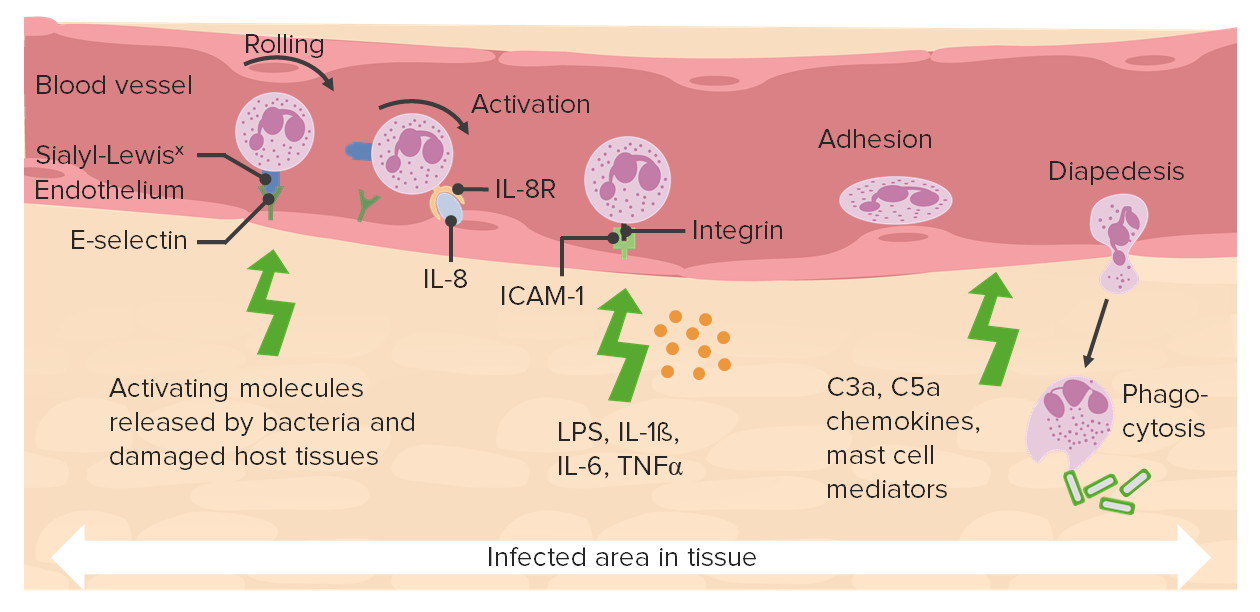
00:01 So let’s now turn to the normal inflammatory response to an infection, which would be acute inflammation. 00:08 You only get chronic inflammation if things really go wrong. 00:10 So, what happens usually following an infection? Well, in acute inflammation there are many different cell types that are involved and as we’ve already heard, neutrophils are really at the heart of the acute inflammatory response. 00:26 If you were to ask me, well what is the most important cell in the acute inflammatory response? I’d probably say, it’s the neutrophil because, indeed it is. 00:35 But neutrophils are normally present in the blood circulation. 00:38 They need to get out of the blood circulation to the site where the infection is. 00:43 So the blood vessel endothelium plays a very important role in acute inflammation. 00:50 Mast cells in the tissues, and basophils in the blood are also important; as are eosinophils, which can be present both in the blood and in the tissues, platelets which are involved in clotting, and fibroblasts, which can also contribute to the acute inflammatory response. 01:10 So many different cells involved, but also many different molecules. 01:14 Proinflammatory cytokines like interleukin-1 and interleukin-18 that we’ve already mentioned. 01:19 Chemokines - which are chemotactic cytokines that attract cells of the immune response to the site of the infection. 01:28 The acute phase proteins that I’ve already mentioned, some of which are produced by the liver as you saw. 01:35 Adhesion molecules, allowing cells of the immune response to adhere to the blood vessels and then get out to the site of the infection. 01:44 Complement, which we’ll discuss in detail in a few moments. 01:50 Histamine which is released from mast cells and basophils, as are prostaglandins and leukotrienes. 01:59 Histamine, prostaglandins and leukotrienes are very good examples of inflammatory mediators, along with the already mentioned cytokines which can contribute to inflammation. 02:16 So, what can actually cause an acute inflammatory response? Well there are a number of different stimuli; infection of course, but also tissue damage, toxins and a variety of other types of foreign substance can induce acute inflammation. 02:39 Consequences of acute inflammation are many, many different things. 02:45 Again, we’ve already mentioned, proinflammatory cytokine production - interleukin-1β, interleukin-18, tumor necrosis factor α or TNFα. 02:56 Those are just a few of many proinflammatory cytokines that are produced. 03:02 Complement becomes activated and in particular the complement components C3a, C4a, and C5a act as what are called anaphylatoxins. 03:15 These are substances that cause mast cells and basophils to release inflammatory mediators such as histamine. 03:23 So these mediators that are released from mast cells - histamine, leukotrienes, prostaglandins; that release of these inflammatory mediators from the mast cells can be triggered by a number of things including complement components C3a, C4a, and C5a. 03:42 Neutrophil adhesion to the endothelium; a family of molecules called the integrins, some of those are present on the surface of the neutrophil and they bind to molecules called ICAMs on the surface of the blood vessel endothelium. 03:59 There needs to be vasodilation, and bradykinin is a molecule that helps mediate vasodilation. 04:09 There also needs to be increased vascular permeability, leading to edema. 04:16 This is part of the fact that during the acute inflammatory response, you get swelling, as we’ve already heard. 04:22 And recruitment of neutrophils into the tissues, and a variety of molecules are involved in recruiting the neutrophils into the tissues - complement component C5a, the cytokine interleukin-8, leukotriene B4 which is released from mast cells and basophils, and N-formyl methionyl peptides which are actually produced by infectious bacteria.
About the Lecture
The lecture Acute Inflammation by Peter Delves, PhD is from the course Innate Immune System. It contains the following chapters:
- Acute Inflammation
- Acute Inflammation Consequences
Included Quiz Questions
Which of the following is an important anaphylatoxin?
- Complement component 5a
- Prostaglandin
- Leukotriene
- Histamine
- Interleukin 18
Which of the following is NOT considered an inflammatory mediator?
- Albumin
- Histamine
- Leukotrienes
- Prostaglandins
- Cytokines
Which of the following triggers degranulation of mast cells and basophils?
- Complement component 5a
- Histamine
- Bradykinin
- Interleukin 18
- Intercellular adhesion molecule 1
Customer reviews
4,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
1 |
| 1 Star |
|
0 |
excellent lecture for all med students and normal people thanks!
good, I really like the information, thank u Dr., bla bla bla bla bla
A very concise lecture but too much so. I was really hoping to learn more about mechanisms and detail. For example, there was no detail provided about the mechanisms involved with how vascular permeability increases. There was no explanation for what cells produce bradykinin and how this causes vasodilation. This was not advanced enough for medical school.