Playlist
Show Playlist
Hide Playlist
Subdural Hemorrhage – Intracranial Hemorrhage (ICH)
-
Slides 21 IntracranialHemorrhage HeadNeckAnatomy.pdf
-
Download Lecture Overview
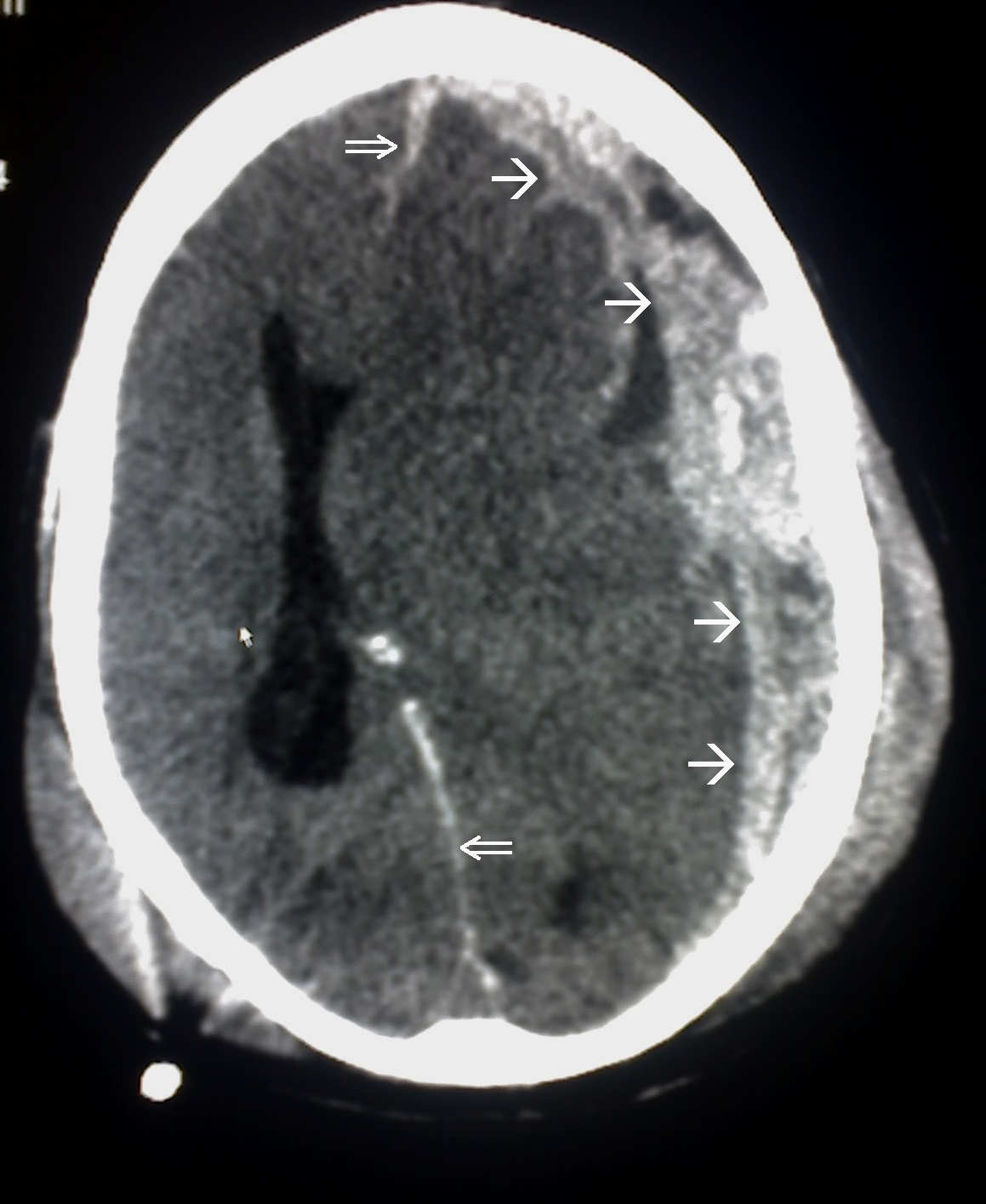
00:01 The next form of intracranial bleed is a subdural hematoma. This is due to tearing of bridging veins as a result of trauma. We do see in the illustration an example of a bridging vein. It is shown right in through here. It’s running within the subarachnoid space and then will cross the arachnoid mater and then drain into, in this case the superior sagittal sinus. So, if there’s any rupture or tearing of this bridging vein along its course that will cause a bleed that is going to be subdural in its variety. That will separate the dura mater from the arachnoid mater as a result. So what are the structural and clinical considerations of a subdural hematoma? Again, the first consideration is it’s due to a tearing of a bridging vein or maybe multiple bridging veins due to head trauma. 01:17 As a result, the hemorrhage will separate the meningeal layer specifically of the dura mater and the arachnoid. So the bleed then causes this pathologic subdural space of which we see over here on the left side of the image. We also see another subdural bleed over here on the right side of the image. This is bleeding into the lateral sulcus region. Again, a subdural hematoma will create a pathologic space, the subdural space, as it separates the meningeal layer of the dura mater from the arachnoid mater. Its appearance is different from that of an epidural hematoma. The subdural hematoma is said to be crescent-shaped in its appearance. We can appreciate it on this side of the image. The increased intracranial pressure may cause herniation of the cingulate gyrus or of the uncus. But being a tear of a vein, these are much slower bleeds. These tend to be more common in the elderly and in individuals who are chronic alcoholics. As we age, our brain just shrinks or undergoes atrophy. In chronic alcoholics, they will accelerate the course of brain atrophy. This just increases the space then between the brain and the dura where the bridging veins are found. 03:07 With trauma to the skull, there’s much more tension or forces being placed on these bridging veins due to a smaller brain. Here, we’re looking at a subdural bleed into the lateral fissure as mentioned before. We can see here along the outer cortical area, we can see that this increased pressure of the subdural hematoma is starting to produce edema. 03:39 This edema then is tissue swelling. Here, we’re looking at a post-mortem view of a subdural hematoma. In this case, the subdural hematoma occurred bilaterally. You can appreciate the large hematoma regions here, black arrows on this side and then one black arrow on this side. This dark substance represents the hematoma. 04:07 This structure here that is separating both bleeds is the falx cerebri.
About the Lecture
The lecture Subdural Hemorrhage – Intracranial Hemorrhage (ICH) by Craig Canby, PhD is from the course Head and Neck Anatomy with Dr. Canby.
Included Quiz Questions
Which of the following is a common cause of subdural hematoma?
- Chronic alcoholism
- Berry aneurysm
- Obesity
- Diabetes mellitus
- Hypertension
When subdural hematoma occurs, it creates a pathological space. Which areas are on either side of this space?
- Dura mater and arachnoid mater
- Arachnoid mater and pia mater
- Dura mater and pia mater
- Arachnoid and skull
- Dura mater and skull
What seperates bilateral subdural hematomas?
- Falx cerebri
- Uncus
- Cavernous sinus
- Lateral ventricles
- Suture line
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Manifold information was expressed pretty clearly, making me grasp almost the necessary knowledge of Intracranial hemorrhage.