Playlist
Show Playlist
Hide Playlist
Sub-Acute Headache, Chronic Headache and Migraine
-
Slides 08 Headache Neuropathology I.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
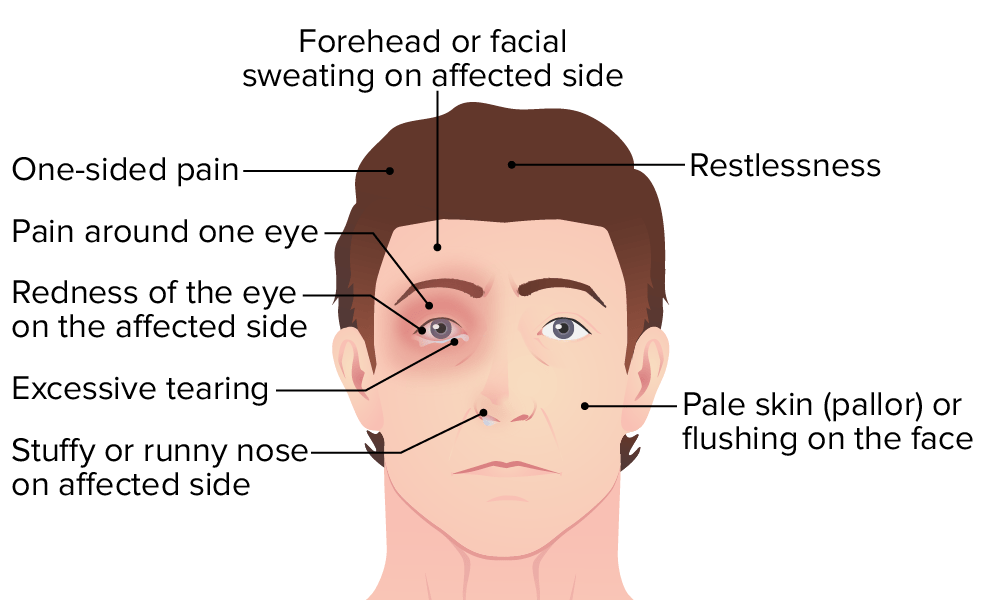
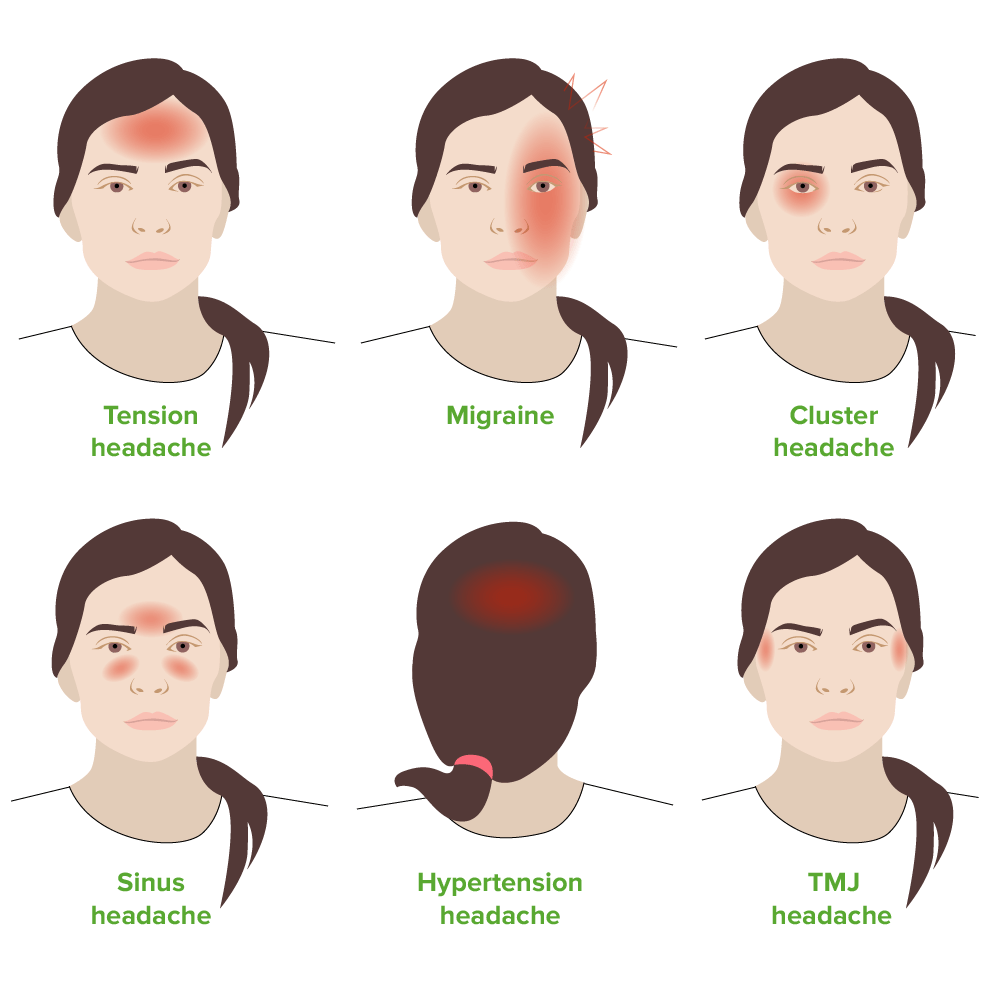
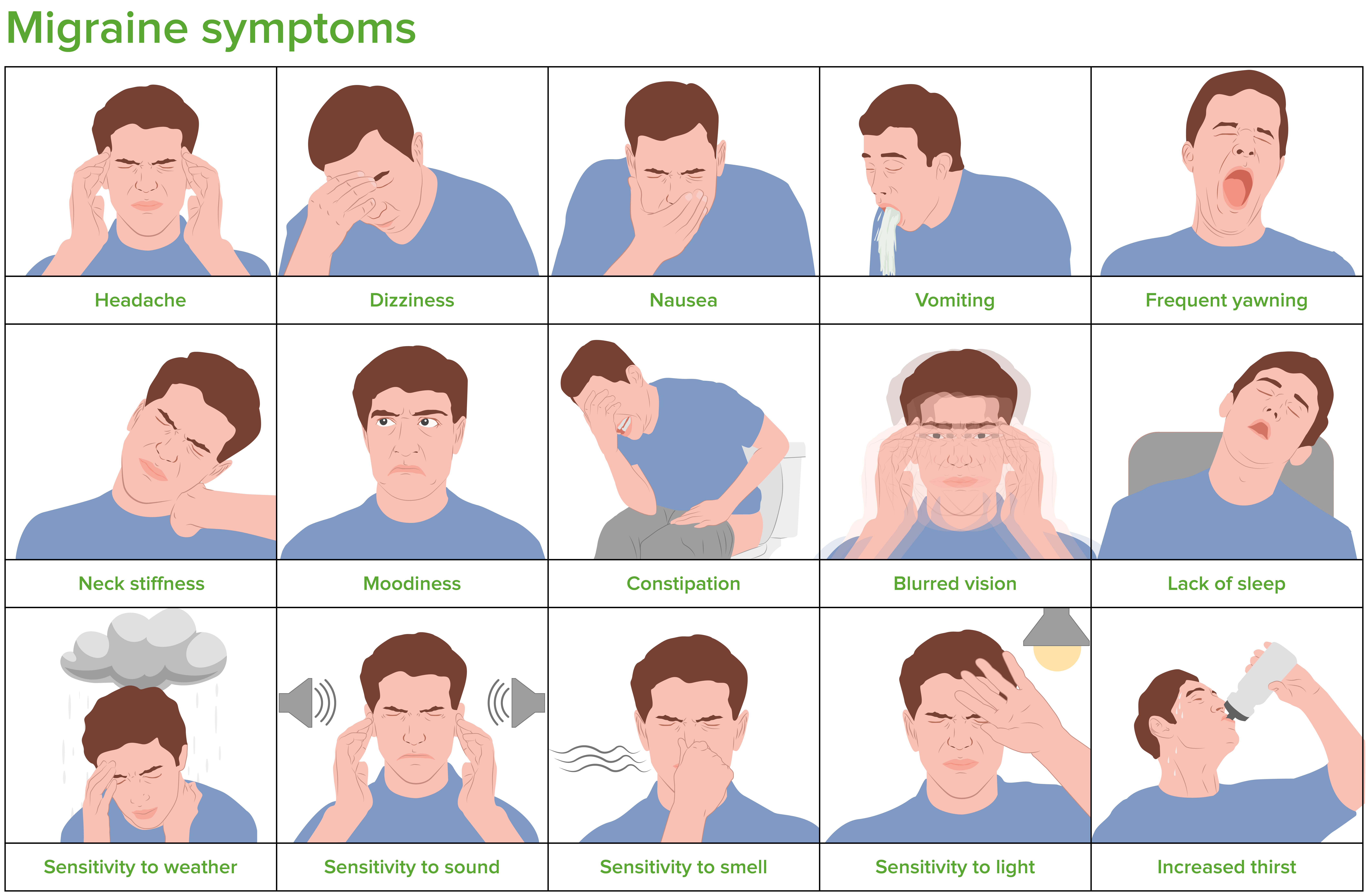
00:01 Our topic now brings us to sub-acute and chronic headache. 00:07 Up until now, we’ve looked at acute headache. 00:09 We’ve closed the chapter on that. 00:11 Let’s get into chronic and subacute. 00:13 Migraine, pseudotumor cerebri, mass lesion, tumor, abscesses, tension type headache, chronic daily headache, trigeminal neuralgia. 00:23 All of these extremely common in our society. 00:27 We need to make sure that you’re quite well-versed with how to first identify it, diagnose it, and management, you’re good to go. 00:36 We'll first take a look at migraines. 00:38 Unilateral, throbbing, throbbing. 00:42 “Doc, I feel like my head is throbbing, pulsating.” Associated nausea and vomiting. 00:49 Typically, unfortunately, begins in childhood, adolescence, young patient, 90% of your patients will be less than 40 years of age. 00:58 Much more common in females, migraines. 01:01 What about cluster? Much more common in males, young. 01:05 Patients generally want to still lie in the dark because if they are exposed to light, it bothers them. 01:13 Be careful. Differential obviously here, meningitis, migraine headache. 01:18 Classification: Classic, you have the aura. 01:22 Common, without the aura. 01:27 Migraine variants, maybe there’s involvement of the eye, so ophthalmic or retinal, menstrual, hemiplegic, and basilar. 01:37 These are variants. 01:38 Common without aura, classic with aura. 01:44 All are based on, well, sterile inflammation of blood vessels. 01:47 Sterile, not infective. 01:49 Note that when we say “sterile inflammation” in migraines, we are talking about a concept known as “neurogenic inflammation” and not the typical inflammatory response you see in other tissues such as activation of immune cells and/or autoimmunity. 02:06 The neuroinflammation theory in migraines states that the trigeminal meningeal nociceptors are activated due to the release of the neuropeptides. 02:16 Substance P and calcitonin gene-related peptide - to be precise. 02:22 Many things can activate the trigeminovascular system leading to sterile neurogenic inflammation. 02:28 The majority of patients with migraines identify at least one trigger. 02:32 Common triggers include emotional stress, hormones, missing meals, weather changes, insufficient sleep, strong odors, neck pain, bright lights, alcohol, certain foods, and exercise. Once identified, some of these triggers can be managed or avoided in some cases. 02:49 Classic migraine is accompanied by an aura that precedes or occurs during the headache pain. About 25% of patients experience auras with migraines, which are visual or other sensory phenomena. Auras last less than an hour, and can be confused with transient ischemic attacks (TIAs). 03:05 Progression to severe, usually unilateral headache occurs within an hour. Both classic and common migraine often have associated symptoms of nausea, vomiting, photophobia or sensitivity to light, and phonophobia or sensitivity to sound. Common migraine is a migraine headache without aura. Patients with classic migraines with aura may also sometimes have common migraine without aura. 03:28 Classically, an aura begins as a small area of visual loss, or as flashes or spots of lights. Some patients report bright lines like “lightning bolts” or other shapes. S Some patients have auditory auras with tinnitus, noises, or decreased hearing. Others experience vertigo or other sensory changes such as paresthesias. Rarely, patients can present with stroke-like symptoms, and any migraine aura may present like a TIA at first until the headache starts. 03:54 Occasionally, patients will have an aura without a headache, and these last less than one hour - the same as auras followed by or accompanied by headache. 04:02 Management of your migraine: Abortive therapy; triptans, ergotamine, and caffeine, perhaps, NSAIDs, IV steroids, valproate IV, narcotics. 04:16 Newer options include calcitonin-gene related peptide (CGRP) antagonists and the selective serotonin 1F receptor agonist, lasmiditan. 04:26 Triptans are a big thing here. 04:28 Preventive: Avoid the trigger such as light, maybe the sounds. 04:32 Treat attacks early if possible. 04:35 Beta-blockers, tricyclics, antiepileptics even, and calcium-channel blockers are all preventive therapies for your migraines. 04:46 Summary of migraine. 04:48 Female. 04:49 Age: Young. 04:51 Most of your patients, 90% less than 40. 04:54 Preventive: As we said, avoid the triggers. 04:57 Your medications that we talked about earlier, with calcium channel blockers. 05:01 Signs and symptoms: Unilateral throbbing, nausea, photophobia. 05:07 But as you said earlier with common, it could be bilateral. 05:10 Differential: We talked about tension type, sinusitis. 05:14 Earlier, we talked about temporal arteritis with acute and mass lesion. 05:18 H and P for sure. 05:20 Image to make sure that rule out other possible underlying issues. 05:25 The triptan can cause chest pain and flushing in such patients. 05:29 Look for this. 05:30 And ergotamines that we talked about, prolonged use can cause gangrene. 05:34 In addition to the triptans and dihydroergotamine, there are other “migraine-specific” agents. Calcitonin gene-related peptide antagonists work on the therapeutic target in migraine which is CGRP. They work by affecting the role of CGRP in pain transmission and neurogenic inflammation. 05:52 There are also several monoclonal antibodies that target CGRP and are used in the prevention of migraine. Botulinum toxin or “Botox” is not effective for the treatment or prevention of acute migraine, but is used by injection for patients with chronic migraine.
About the Lecture
The lecture Sub-Acute Headache, Chronic Headache and Migraine by Carlo Raj, MD is from the course Headache – Pathophysiology. It contains the following chapters:
- Sub-Acute and Chronic Headache
- Classic Migraine
- Common Migraine
Included Quiz Questions
Which of the following statements regarding migraines is TRUE?
- They may be preceded by a visual aura for 30–60 minutes.
- They start suddenly within a few minutes.
- They are more common in men than women.
- They are not associated with nausea and photophobia.
- They are usually described as bilateral, stabbing pain.
What is the pathophysiology of headache pain in a patient with a migraine?
- Activation of trigeminal meningeal nociceptors by the release of substance P and calcitonin gene-related peptide (CGRP)
- Activation of the innate immune system
- Activation of the adaptive immune system
- Release of inflammatory cytokines
- Stretching of the meninges
Which type of medication is used for prophylaxis of migraine without aura?
- Beta-blockers
- Serotonin reuptake inhibitors
- Lithium
- ACE inhibitors
- Ergotamines
Customer reviews
3,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
1 |
| 2 Stars |
|
0 |
| 1 Star |
|
1 |
i was reading the reviews and there is a big mistake, this lecture it's a resume, it can't be your only source of information, so don't cry about it and use it with your books.
seriously these series of lectures are the absolute worst. no explanation at all, no physiopathology, no images...just a pathologist who seems to be severely under qualified to teach a comprehensive clinical neurology lecture , reading a bunch of bullet points off the most lazily prepared power point presentation. seriously strating to wonder what the point of lecturio is. I do the q bank right after the lectures and literally nothing that is asked is mentioned in these lectures.
It would have been good to further discuss migraine headaches and tensions headaches. I would have like to learn more about the features of aura (incl scotomas). Moreover, a discussion on what constitutes medication overuse headache is warranted given the ease of access to OTC analgesics. Finally an opportunity has been missed to discuss if which circumstances you would consider the use of prophylactic therapies