Playlist
Show Playlist
Hide Playlist
Stages of Hemostasis
-
Slides NormalHemostasis.pdf
-
Download Lecture Overview
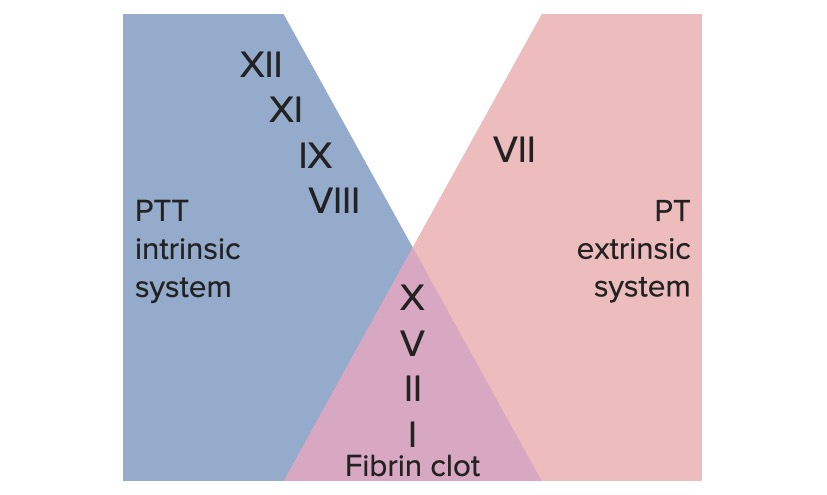
00:01 Ultimately, let's take a look at the stages of hemostasis here. 00:06 So remember, we began way back where we caused damaged to the vascular phase. 00:11 What happened here? Endothelial cell was damaged and when endothelial cell was damaged, what did they express? Von Willebrand factor. Good. 00:20 Where do they bind to? Glycoprotein Ib. 00:22 Next, what made then happen? This was adhesion, wasn't it? Process called adhesion. 00:27 What if there is a defect in von Willebrand factor? So now I'm gonna give you a fourth test. 00:31 The fourth test is called bleeding time. 00:35 The time that you'll have to memorize here will be 2 to 7 minutes, okay? 2 to 7 minutes. 00:44 In other words, the bleeding time is going to tell you how well is my platelet working only. 00:51 May I ask you a very important question? Can you form a plug without the coagulation cascade? Technically speaking, yes you can, right? All you need is platelet and fibrinogen without the coagulation cascade and you can form a temporary hemostatic plug. 01:10 I bring this to your attention because if you're missing von Willebrand factor here and it cannot bind and you don't even have it, the bind the glycoprotein Ib, the test that you'll find to be elevated will be bleeding time. 01:23 Remind me one more time that von Willebrand factor stabilizes which coagulation cascade? Which coagulation cascade component is von Willebrand factor stabilized? Factor VIII. 01:38 Factor VIII is part of which coagulation pathway? The intrinsic. 01:44 What's the next step after adhesion? It's called aggregation. 01:49 What do you need for aggregation? What's the glycoprotein receptor here? IIb/IIIa. 01:54 Initially, what is it going to bind to? Those beads that were called fibrinogen. 01:58 What else helps you with aggregation? TXA2 stands for thromboxane. 02:04 Give me a drug that you should know. 02:08 We even recommend this. 02:09 A little controversy but point being is aspirin. 02:11 Baby aspirin, 81mg. 02:13 Why do you wanna give aspirin to a patient who may be at risk of developing, let's say, coronary arterial disease? Oh, because it inhibits what's known as your COX, cyclooxygenase. 02:24 When you inhibit cyclooxygenase then you might be inhibiting the synthesis of thromboxane in which you will then not have aggregation. 02:34 But if you continue forward physiologically, you may then form what kind of plug? A temporary hemostatic plug. 02:41 Stop there mentally because at this point we form temporary hemostatic plug. 02:46 What's my next step? The fibrinogen must be cleaved. 02:49 What's the name of that enzyme that cleaves fibrinogen? Ah, thrombin. 02:54 So now with thrombin we get into our coagulation cascade. 02:58 We have two branches, intrinsic and extrinsic. 02:59 It converges about which factor please? Factor X, remember that, factor X. 03:06 And then with this you activate your prothrombin and that thrombin will then cleave the fibrinogen. 03:12 Now that you formed a proper stable clot, you must then have your factor XIII to make it insoluble. 03:21 Mentally stop there. 03:22 What's next, now that you formed a clot? Well, you gotta break it down. 03:28 What do we call this? Ah, the final phase. 03:30 They're all part of proper hemostasis. 03:32 Proper, balance, a seesaw. 03:36 And who then is the enzyme that activates your or degrades your fibrin? It's called plasmin and this factor is factor XII. 03:45 This is then called the fibrinolytic phase. 03:48 What's the name of the test in which you made them have excessive thrombi breakdown? D-dimer. 03:57 To summarize the plugs, here they are. 03:59 The one on the left is your temporary. 03:59 Remind me again, what are those receptors on the platelet here that are binding those beads? Glycoprotein IIb/IIIa. 04:08 What are those beads? Fibrinogen. 04:12 Any coagulation components? None. 04:15 While the one on the right is your stable. 04:18 What's the difference? Take a look at the beads. 04:22 Hah! It became a concrete brick. 04:23 How did that happen? The concrete brick was developed due to cleavage of the fibrinogen with the help of which enzyme? Is it thrombin or plasmin please? Good. 04:38 Thrombin. 04:39 And you cleave up the ogen to form your fibrin which is your stable clot and the factor XIII will come in to make it insoluble. 04:46 Is that understood? Remind me again, what is then going to break down this fibrin clot? Factor XII will then activate your plasminogen and the plasmin will then start breaking down your stable clot all to make sure that you maintain homeostasis because if you then form too many thrombi, you may then have pathologies such as DIC, TTP, if it's a young child maybe HUS.
About the Lecture
The lecture Stages of Hemostasis by Carlo Raj, MD is from the course Hemostasis: Basic Principles with Carlo Raj.
Included Quiz Questions
Which of the following is the typical normal range for bleeding time?
- 2-7 min
- 1-3 min
- 12-15 min
- 7-10 min
- 15-18 min
Which of the following coagulation tests is most likely to be abnormal in von Willebrand disease?
- Partial thromboplastin time
- International normalized ratio
- Prothrombin time
- Hemoglobin
- Platelet count
Which of the following enzymes cleaves fibrinogen?
- Thrombin
- Von Willebrand factor
- Factor VIII
- Fibrin
- Plasmin
What is the final stage of hemostasis before fibrinolysis?
- Coagulation phase
- Vascular phase
- Platelets plug formation
- Vasodilation
- Platelet activation
Customer reviews
4,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
1 |
| 1 Star |
|
0 |
love how you repeat many times & explain clinical example thank you
This lecture was perfect. I really liked that he repeated the really important information over and over and would ask you to recall information as well. He spoke at a good pace and was really good with giving tips here and there to help with memorization
There were no quiz questions. Spoke quickly. Good information though.