Playlist
Show Playlist
Hide Playlist
Systemic Lupus Erythematosus (SLE) in Children
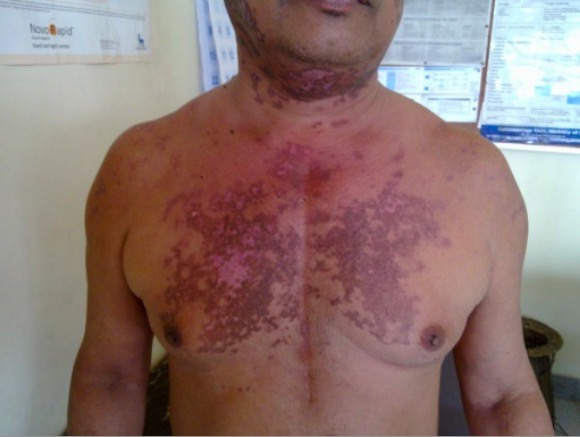
00:01 In this lecture, we're going to discuss lupus, more formally known as systemic lupus erythematosus or SLE. 00:11 Lupus has a unique pathology. 00:15 Basically, this is a multisystem inflammatory autoimmune disease that's caused by immune complex mediated damage. 00:24 It affects multiple organs, in different ways, in different people. 00:28 And the cause is unknown. 00:30 There are genetic factors, environmental factors, and hormonal factors, which mitigate the disease. 00:37 It is more common in girls than boys. 00:41 And the peak pediatric age of diagnosis is 9 to 15 years of age. 00:46 We don't usually see it in the very young children. 00:50 So the pathophysiology of lupus is, as we stated both genetic and environmental. 00:56 In a susceptible individual who has susceptibility genes, they're going to have an event that results in a apoptosis. 01:05 For example, they might have got a sunburn on their skin, a UV radiation. 01:10 A period during which cells are breaking down on a larger scale. 01:16 These patients because of their genetic susceptibility, will have a defective clearance of these apoptotic bodies, resulting in an increase burden of nuclear antigens throughout the body. 01:29 In this susceptible person, the B cells and T cells will mount an immune response against these nuclear antigens. 01:37 This will create anti-nuclear antibody antigen complexes, which will then go through the body going to stimulate both dendritic cells, which then stimulate B cells and create antibodies vastly against nuclear antigens. 01:54 These nuclear antigen with antibody complexes are causing the mainstay of the disease in organs throughout the body. 02:02 So let's go through some of the basic symptoms of SLE or lupus. 02:08 Constitutionally, these patients get frequent fevers, they may have fatigue, and they'll develop weight loss as well. 02:16 Their skin has a few key findings. 02:18 This girl has one of them, a malar rash. 02:22 They may also have a discoid rash, which are little round circles around the skin. 02:28 Discoid rashes are also common in babies with lupus and we'll talk about that entity separately. 02:35 Also, patients may get photo sensitivity, which is a increased susceptibility to burn when exposed to the sun. 02:44 Patients do get lung involvement. 02:46 They can get pleuritis, pleural effusions, pulmonary hemorrhage, or even pulmonary hypertension. 02:52 They have cardiac findings. 02:55 In additionally, they will have pericarditis, myocarditis, and endocarditis. 03:00 Any part of the heart can be evolved, and they can get cardiovascular or vascular problems such as Raynaud's phenomenon, which you can see in this patient here. 03:09 Where there is decreased blood flow to the distal end of a digit. 03:15 In patients with lupus, they can get an endocarditis that is unique called Libman-Sacks endocarditis. 03:22 It looks grossly like bacterial endocarditis, but does not grow any organisms on blood culture. 03:29 This can appear as single or multiple 1 to 3 millimeter warty deposits on those valves and you can see a picture of one here. 03:39 These patients may have involvement of their renal pathways. 03:43 They may develop proteinuria or hematuria depending on if they're having more nephritic or nephrotic syndrome. 03:49 They may develop pyuria from just white blood cells that are inflamed in the kidney, but they will not grow anything on the urine culture. 03:57 They may develop hypertension as a result of their end stage renal disease and they may proceed to renal failure. 04:05 The GI system can get involved as well and in particular, these patients may develop oral ulcers, pancreatitis, hepatitis, intestinal vasculitis or even a protein-losing enteropathy. 04:18 Essentially, any part of the GI tract can be involved. 04:23 They may have muscle disorders, they may develop arthritis or myositis, or a vascular necrosis of a joint. 04:31 And importantly, they may develop brain problems. 04:34 Roughly 10% of patients with lupus will present with a brain problem. 04:40 Examples include stroke, psychosis, seizure, chorea or a tremor, they may develop a transverse myelitis of the spine. 04:52 Additionally, patients can get problems with their blood and any blood line can be affected. 04:57 They may get lymphopenia, anemia, or thrombocytopenia any cell line on the CBC can go down. 05:05 So there are several ways that people can diagnose lupus, and it gets confusing, I think, for a lot of students because we used to have 11 criteria and now there's two different sets of criteria. 05:17 There's the ACR criteria and the SLICC criteria. 05:20 The SLICC criteria are probably more commonly used in children. 05:23 So I want to go through them here. 05:25 To meet criteria you need four clinical criteria. 05:29 And then additionally one immunologic criteria. 05:33 So we can go through them here. 05:35 And the clinical criteria include acute cutaneous lupus, chronic cutaneous lupus, oral or nasal ulcers, Non-scarring alopecia, arthritis, Serositis. 05:47 Remember, the cirrhosis are the lining of the pericardium, the pleura and the peritoneum. 05:52 So any kind of inflation of those services, renal, any renal involvement, any neurologic involvement. 05:59 Keep in mind that about 10% of patients will present with a primary neurologic condition. 06:04 Hemolytic anemia, leukopenia and thrombocytopenia. 06:09 Additionally, patients need to meet an immunologic criteria, and those include a positive ANA, a positive anti DNA, a positive anti Smith antibody, positive antiphospholipid antibody lo complement levels or also a direct Coomb's test, which doesn't count in the presence of hemolytic anemia has to sort of be in addition. 06:32 Keep in mind that the ANA is an interesting test. 06:35 It's commonly a false positive, but virtually never a false negative. 06:40 So a patient doesn't have an ANA it's very unlikely that they have lupus. 06:45 So, this is a lot of stuff. 06:48 These are a lot of symptoms to remember. 06:51 And unfortunately, there's no gene test for lupus. 06:55 it's a clinical diagnosis. 06:57 For a diagnosis, you need 4 or more of the 11 major criteria of lupus. 07:04 Who can remember 11 criteria of lupus? Well, you can with a little pneumonic. 07:09 Here it goes. 07:10 M.D., please offer all RNs a holiday immediately. 07:15 Again, M.D., please offer all RNs a holiday immediately. 07:20 You have to do the S after the RNs. 07:22 Let's look at it this way. 07:24 M.D., please offer all RNs a holiday imediately. 07:29 What's clever about this is the last three are lab criteria. 07:33 And the first eight are body physical exam criteria. 07:38 Let's go through them again so we can remember them. 07:41 M is the malar rash. D is the discoid rash. 07:45 And P is the photosensitivity. 07:48 Those are the skin findings in lupus. 07:51 O is oral ulcers. 07:54 A is arthritis. 07:56 The R is renal involvement, and the N is neurologic involvement. 08:02 The S is tricky. It's Serositis. 08:05 Remember, your serosa are superficial coverings of your organs. 08:10 So the area around the heart is the pericardium that is a serosa. 08:14 So pericarditis is a serositis. 08:17 Peritonitis is a serositis. 08:19 Pleuritis or a pleural effusion is a serositis. 08:24 Next, the labs. 08:26 The ANA test is its own criteria. 08:29 The interesting thing about the ANA test is that virtually every patient with lupus will have a positive ANA. 08:36 This is the one that almost all of them have that is positive. 08:39 So a positive ANA is necessary almost for a diagnosis of lupus, If they're not any positive, they will be very soon. 08:50 The challenge is, is that one in three people walking down the street will have a positive ANA. 08:55 Hack,they're even a little bit infectious. 08:58 And by that I mean, if you are ANA negative and you move into the home of someone who has ANA positive, you're more likely to become ANA positive. 09:07 That doesn't mean you're getting lupus. 09:09 So the ANA positivity is necessary but not sufficient for the diagnosis. 09:16 H is heme labs. 09:18 Again, back to any of those elements of the CBC. 09:21 They may have an abnormal white count, abnormal hemoglobin, or abnormal platelets and all of them are usually low. 09:28 And I is immune labs. 09:31 And I'll walk you through what those are in a bit.
About the Lecture
The lecture Systemic Lupus Erythematosus (SLE) in Children by Brian Alverson, MD is from the course Pediatric Rheumatology and Orthopedics. It contains the following chapters:
- Systemic Lupus Erythematosus (SLE)
- Clinical Presentation of SLE
Included Quiz Questions
Which of the following is NOT a diagnostic criterion for systemic lupus erythematosus (SLE)?
- Peeling of the skin of the hands and feet
- Malar rash
- Photosensitivity
- Serositis
- Oral ulcers
Which of the following statements is TRUE regarding systemic lupus erythematosus (SLE)?
- It is an inflammatory autoimmune disease.
- The primary feature of SLE is antibody-mediated damage to the joints.
- SLE can only be caused by genetic causes, without external triggers.
- SLE is more common in boys than in girls.
- SLE is usually diagnosed around 2-5 years of age.
Which of the following is NOT part of the pathophysiology of systemic lupus erythematosus (SLE)?
- B-cell suppression
- Activated T-cells
- Dendritic cells
- Anti-nuclear antibodies
- B-cell hyperactivity
Which of the following statements is FALSE regarding endocarditis in systemic lupus erythematosus (SLE)?
- A microorganism must be isolated for diagnosis.
- The warty deposits can be 1-3 mm in size.
- Blood cultures don't reveal any organisms.
- It is also referred to as Libman-Sachs endocarditis.
- It looks like bacterial endocarditis on gross examinaton.
Which of the following is NOT a CNS finding seen in systemic lupus erythematosus (SLE)?
- Ataxia
- Transverse myelitis
- Stroke
- Chorea/tremors
- Seizure
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
3 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Very informative. Keeping it to the point. Perfect for an introduction before opening the book!
Excellent lecture, one more complex topic explained in its most essential components. Thanks!
Excellent means of simplifying a complex topic especially the numerous symptoms