Playlist
Show Playlist
Hide Playlist
Secondary Headache (Emergency Medicine)
-
Emergency Medicine Bord Approach Headache.pdf
-
Download Lecture Overview
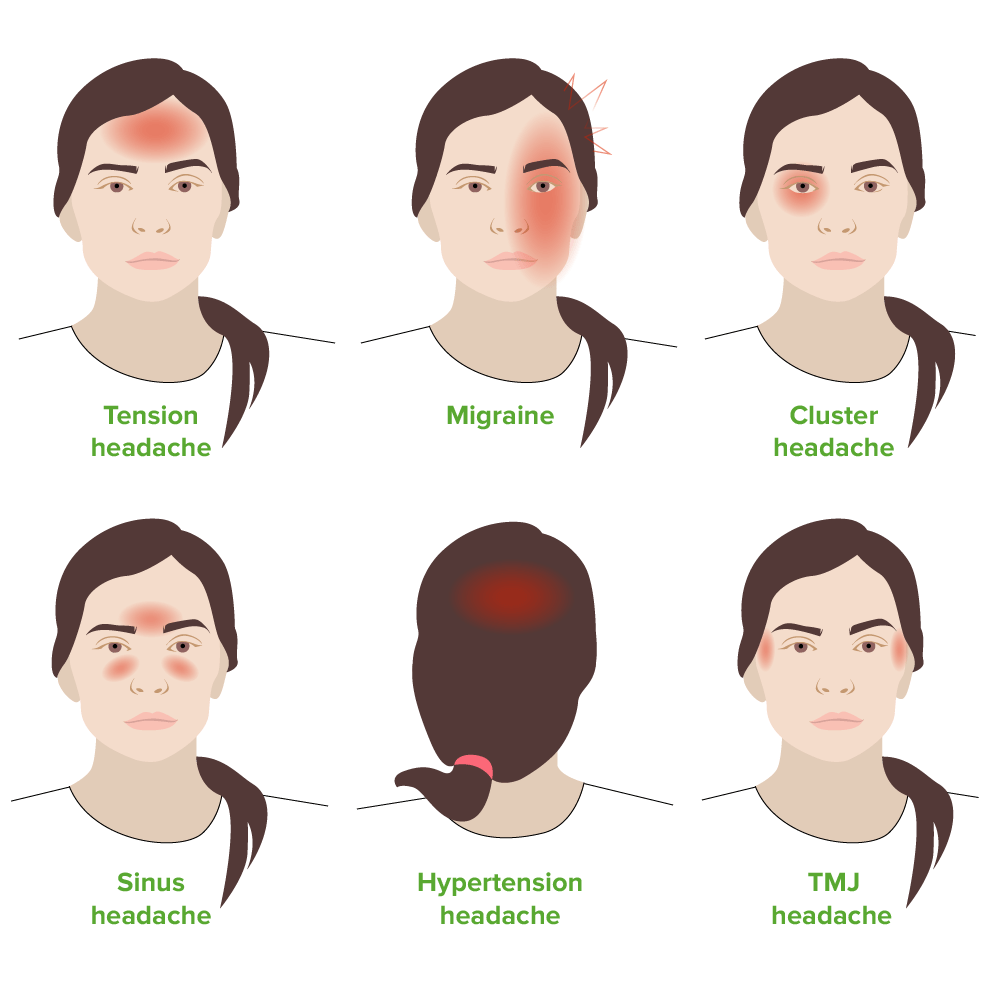
00:01 Now lastly, just to talk briefly about secondary headaches. 00:05 There's lots of causes. 00:06 Subarachnoid hemorrhage is one of them. 00:08 We’ll be discussing this in another lecture. 00:11 But patients who present with subarachnoid hemorrhage that’s generally a sudden onset, thunder clap headache. 00:17 The classic way it presents is with you know, patients getting an exertional related headache, patients may have loss of consciousness, and this is one of those serious, serious causes of headache that's on our differential of consequence, and if you're worried about it, that patient will require additional work up and testing. 00:36 Giant cell arteritis is generally seen in elderly people. 00:40 Patients will have pain over one of their eyes in the temporal area. 00:45 If a patient has a history of having had a spinal tap or lumbar puncture recently, post lumbar puncture headache, can present with a patient having more severe symptoms when they stand up and that's due to the fact that the patient generally has a low level or a low pressure in the cerebrospinal fluid. 01:04 So they don't have enough cerebrospinal fluid circulating around their brain. 01:07 Hypertension can sometimes lead to a headache. 01:10 So patients who have a known history of hypertension or new diagnostic hypertension, those patients can sometimes have a headache associated with that. 01:19 Infectious things, meningitis is a possible cause. 01:23 Meningitis is an infection around the brain. 01:26 Infection though can also such as influenza or other infections, can sometimes cause an associated headache for patients. 01:34 Cerebral venous thrombosis is when you have a clot in the central venous system of your brain. 01:42 This is most classically associated with elevated estrogenic states such as pregnancy is a classic one. 01:49 And then, idiopathic intracranial hypertension is when you have an elevated pressure in the cerebrospinal fluid. 01:56 The classic presentation of that are patient who presents with a headache. 02:00 Classically, it's in an obese female patient with associated vision changes. 02:05 The treatment for that is removal of this cerebrospinal fluid. 02:09 And the diagnosis is actually also in the procedure of a lumbar puncture. 02:14 So when someone presents in your concern about elevated CSF pressures, doing a lumbar puncture and measuring the opening pressure can help you diagnose this condition. 02:25 The other classic thing that can help you diagnose idiopathic intracranial hypertension is looking in the back of the eye for papilledema. 02:34 So patients who have IIH or idiopathic intracranial hypertension will have papilledema on their physical exam. 02:42 So the conclusion here for headache. 02:46 Headaches are divided into primary benign headaches and secondary headaches, due to the underlying etiology. 02:52 Our goal in the Emergency Department is to understand these red flag symptoms. 02:56 So do the headaches starts suddenly? Are there neurologic symptoms? Was there loss consciousness associated with it? To help differentiate between this benign headaches and these secondary headaches. 03:06 Because the benign headache is something that you go ahead and you treat and you make your patient feel better. 03:11 But the secondary headache oftentimes needs to be diagnosed and have that underlying problem fixed. 03:17 Many patients presenting what headache though are of that primary or benign etiology. 03:22 Those patients require minimal diagnostic testing and for the most part, your goal in the ED is to get them feeling better. 03:28 Migraine headaches are a very common presenting complaint to the Emergency Department. 03:33 You’ll diagnose those based on your patient having history of similar headaches and basically telling you that this feels like a prior migraine headache. 03:41 Cluster headaches more common in men and patients when they arrive can be in a very severe amount of distress. 03:48 Treatment for this headache like I said is pretty simple. 03:51 You wanna go ahead and place your patient on non-rebreather mask oxygen and that’ll hopefully get them feeling better because that generally help some majority of patients who present with cluster headaches.
About the Lecture
The lecture Secondary Headache (Emergency Medicine) by Sharon Bord, MD is from the course Neurologic and Psychiatric Emergencies.
Included Quiz Questions
Which of the following is NOT characteristic of a headache caused by subarachnoid hemorrhage?
- Involuntary urination occurs
- Described also a thunderclap headache
- Has a sudden onset
- Can be precipitated by exertion
- Is associated with a loss of consciousness
Which of the below is NOT an example of a secondary headache?
- Tension-type headache
- Post-lumbar puncture headache
- Central venous thrombosis headache
- Intracranial hypertension headache
- Hypertensive headache
Which of the following statements regarding headaches is TRUE?
- Many patients presenting with headaches require minimal diagnostic testing.
- Patients with cluster headaches arrive with altered mental status.
- Headaches are divided into primary and secondary based on the onset of presentation.
- Meningitis is the most common cause of primary headaches in children.
- The ultimate goal in the emergency department is to provide sumatriptan for every patient with a headache.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |