Playlist
Show Playlist
Hide Playlist
Scrotal Mass, Congenital- & Acquired Hydrocele and Spermatocele
-
Slides Introduction Male Repro.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
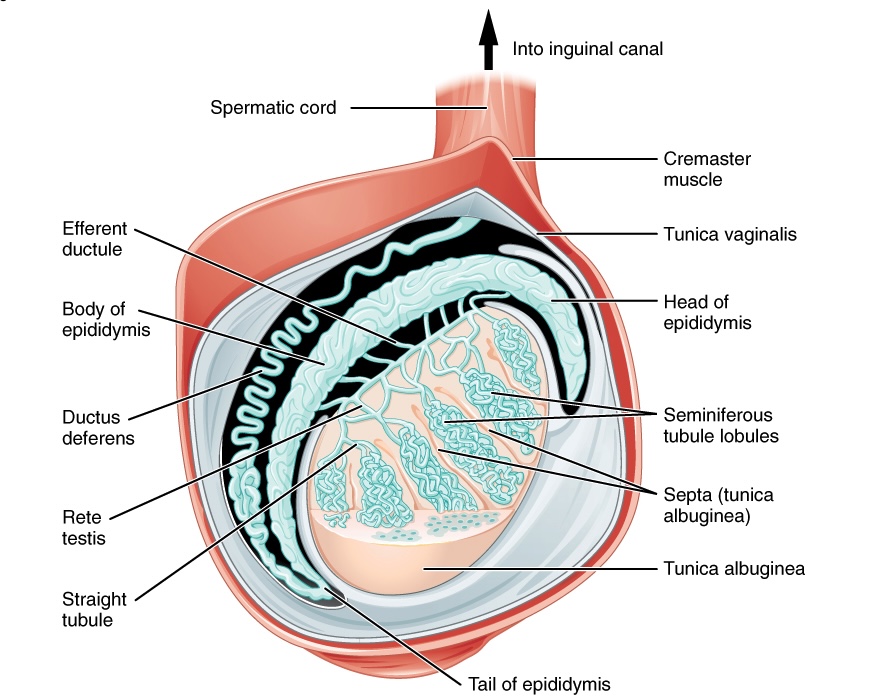
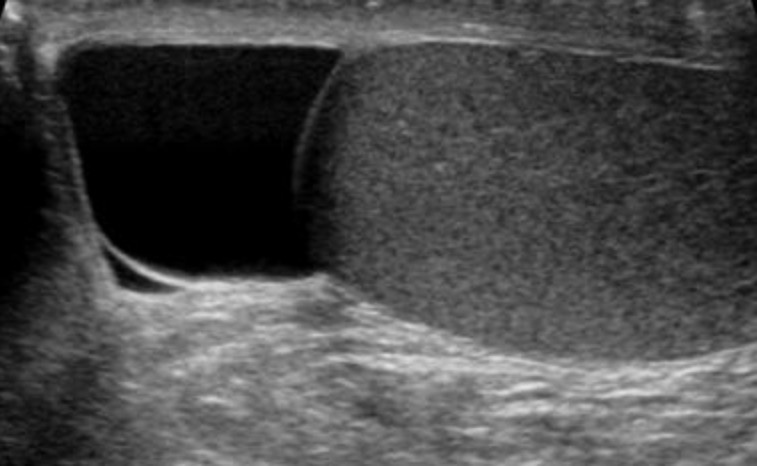
00:01 Here, we’ll take a look at the scrotum. 00:04 Up until now, we’ve looked penile pathology. 00:06 I’ve walked you through varicocele and also looked at testicular torsion. 00:10 And each one of those points are incredibly important, make sure you know clinical presentation and also management for every single board. 00:17 Scrotal masses, well it depends on what the consistency of the mass is, okay? For example, if you find that the scrotal mass can be either transilluminating or you can have scrotal mass that might be solid and that to you should mean testicular tumors. 00:34 So now, with that said, what is the most common enlargement of your scrotum? Varicocele. 00:42 Which side of the testis? Or which side of the scrotum? Left side. 00:47 Let’s take a look at congenital hydrocele. 00:51 Here, common cause of transillumninating. 00:54 Would you tell me as to what the illumination was with varicocele? It didn’t. 00:59 It did not transilluminate. 01:01 Varicocele. 01:03 Why? Because in the veins, we have thick blood. 01:08 It does not transilluminate. 01:10 If it’s thin fluid and not blood, yes it will. 01:14 Congenital hydrocele, common cause of transilluminating scrotal swelling in infants. 01:18 What happened here? Congenital hydrocele is due to incomplete obliteration of the processus vaginalis. 01:25 Remember please your patient is a boy. 01:27 Boy, boy. Genotypic and phenotypic. 01:31 Acquired hydrocele: How did the patient acquire the hydrocele? Scrotal fluid collection usually secondary to infection, maybe perhaps trauma. 01:42 And if it’s bloody, you would call this hematocele. 01:48 Spermatocele: What is this? It’s paratesticular fluctuant nodular cyst formed by the obstruction of the rete testis or the epididymal passage, exactly as the name implies. 02:02 I want you to picture now. 02:04 Close your eyes and think about the Sertoli cells, and they all form at the apical membrane, what lumen is this? Surrounding cells, Sertoli. 02:16 What’s the lumen that it produces or creates? The seminiferous tubule, right? Can you picture that in the testis? And then from the seminiferous tubules, you have the rete testis. 02:26 And then you have the epididymis, vas and so forth, all right? So then that’s the passage that you should have in mind. 02:33 What happens is that if you have a cyst, an obstruction of rete testis or epididymal passage, resulting in a dilated duct with sperm-containing fluid. 02:42 Exactly as to what the name implies. 02:44 Your sperm is not in the vein. 02:47 Your sperm is not in the artery. 02:49 It’s in the seminiferous tubule. 02:51 So if you’re thinking about sperm and fluid being accumulated. 02:54 Do you understand you have to be in the passage from the the seminiferous tubule out into, you know, the vasa deferentia. 03:00 Are we clear? Now, it is often the presence of debris with the cyst that distinguishes spermatocele from simple cyst of the epididymis, that’s a little bit more detailed than might be necessary. 03:13 At this point, it would behoove you to at least know the differences between congenital and acquired hydrocele, varicocele and spermatocele.
About the Lecture
The lecture Scrotal Mass, Congenital- & Acquired Hydrocele and Spermatocele by Carlo Raj, MD is from the course Male Reproductive System Diseases.
Included Quiz Questions
Which condition is the MOST common cause of scrotal enlargement?
- Varicocele
- Hydrocele
- Hematocele
- Spermatocele
- Testicular cancer
What is a scrotal fluid collection called that results from incomplete obliteration of the processus vaginalis?
- Hydrocele
- Spermatocele
- Hematocele
- Varicocele
- Spermatic cord cyst
Customer reviews
3,0 of 5 stars
| 5 Stars |
|
0 |
| 4 Stars |
|
0 |
| 3 Stars |
|
1 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Clear explanations but the lack of diagrams and images for the explanations is very problematic. Add that then it would be really helpful