Playlist
Show Playlist
Hide Playlist
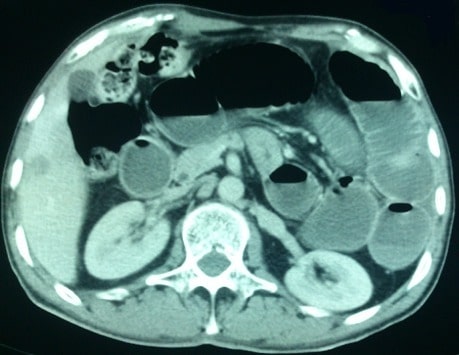
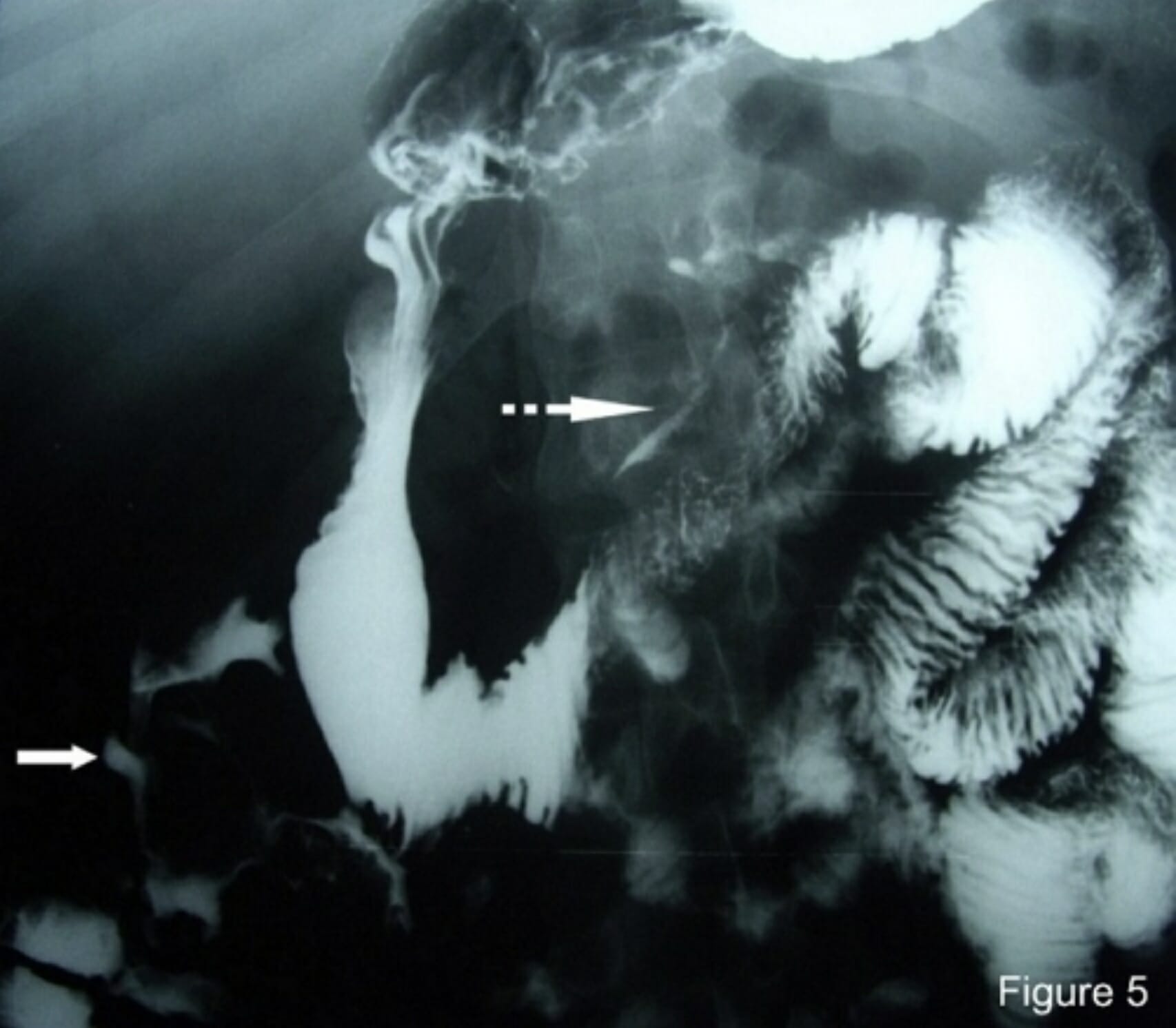
Small Bowel Obstruction (SBO): Management
-
Emergency Medicine Bord Bowel Obstruction.pdf
-
Download Lecture Overview
00:02 What do we wanna do for these patients? So we’ve gotten our diagnosis. 00:05 We’ve asked all the appropriate questions for the patient. 00:07 We wanna start out by giving IV fluids. 00:11 So IV fluids are gonna help rehydrate a patient. 00:13 Oftentimes, these patients when they come in have a lot of nausea and vomiting. 00:18 So IV fluids are gonna help resuscitate them. 00:21 They’re gonna hopefully help get them feeling better. 00:23 Anti-emetics can also be very, very helpful. 00:26 They can help with the vomiting. 00:28 They can help hopefully slow some of that down. 00:32 NG or nasogastric tube placement is a little bit debatable. 00:36 There is little evidence that says that it definitely helps a lot with patients but sometimes the surgery team will request it. 00:43 You wanna think about doing this for patients with altered mental status who are at risk for aspiration. 00:48 It’s not without risk and it can be a painful procedure for patients. 00:52 So we wanna make sure that we’re selecting the right patient population to perform this in. 00:57 NG tubes can potentially go in the lungs, they can increase risk for aspiration in certain patients, and again, it’s a very uncomfortable procedure for patients. 01:06 What you would do is if you put an NG tube, you would hook that up to wall suction. 01:10 So essentially, what you will be doing is you’d be helping relieve some of that obstruction. 01:14 For some patients, it definitely does anecdotally make them feel a lot better. 01:18 So when I’m taking care of patients with a bowel obstruction, sometimes they report that an NG tube makes them feel a lot better because it decreases some of that fluid build-up. 01:28 Lastly, you wanna think about giving empiric antibiotics. 01:32 That would be coverage against gram negative as well as anaerobic flora. 01:36 For the most part, those wanna be used for patients who have perforations. 01:40 So patients who their bowel wall got so ischemic with decreased blood flow that it ruptured and that’s definitely you wanna make sure you give those patients empiric antibiotics. 01:52 Also, for patients who are going for operative management. 01:54 Now, who in fact goes for operative management for bowel obstruction, for small bowel obstruction? This is for patients who have perforation. 02:04 That’s an obvious kind of an indication, right? You have a hole in your bowel. 02:08 You’re spilling your intestinal contents into your abdominal cavity. 02:11 That’s a surgical emergency. 02:13 That patient needs to get to the operating room immediately. 02:16 Strangulation of the bowel is when there is a portion of the bowel in which the blood supply is cut off. 02:22 Those patients also have a surgical emergency. 02:25 Time is bowel. 02:26 The sooner you get that relieved, the quicker those patients will feel better. 02:30 And peritonitis and perforation go hand in hand. 02:33 So when you have that perforation, you’re gonna have the bowel contents in the abdomen and that irritation. 02:38 Those patients needs to go emergently to the operating room. 02:42 Again, for the most part, this diagnosis is gonna be based on your imaging study, based on your CT scan, but possibly also on that plain film x-ray. 02:51 What’s the recurrence rate? So are people gonna go for an operation and never have a small bowel obstruction again? That’s definitely not true. 03:00 So certain patients who go for an operation, about 27% of them will actually have a recurrent bowel obstruction at some point. 03:07 Non-operative management though, the recurrence rate is a little bit higher, so it’s about 40%. 03:13 So definitely, this can be a condition that can recur. 03:16 So patients can get repetitive small bowel obstruction. 03:19 Sometimes patients will come in and say, “This feels like when I had a bowel obstruction before.” And more often than not, they’re likely right in when they report that.
About the Lecture
The lecture Small Bowel Obstruction (SBO): Management by Sharon Bord, MD is from the course Abdominal and Genitourinary Emergencies.
Included Quiz Questions
In the management of small bowel obstruction, NG tube placement is currently no longer a requirement. However, in what kind of patients is NG tube insertion still indicated?
- In patients with altered mental status who are at risk for aspiration
- In patients who are suffering from nausea and vomiting
- In patients who are placed on NPO diet
- In patients who have poor appetite
- In patients who have high tolerance for pain
What is the recurrence rate of small bowel obstruction in patients who are managed without having surgical intervention?
- 40%
- 10%
- 15%
- 30%
- 60%
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |