Playlist
Show Playlist
Hide Playlist
Diagnoses of Reproductive Hormone Disorders– Reproductive Pathology
-
Slides Reproductive Pathology Differential Diagnoses.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
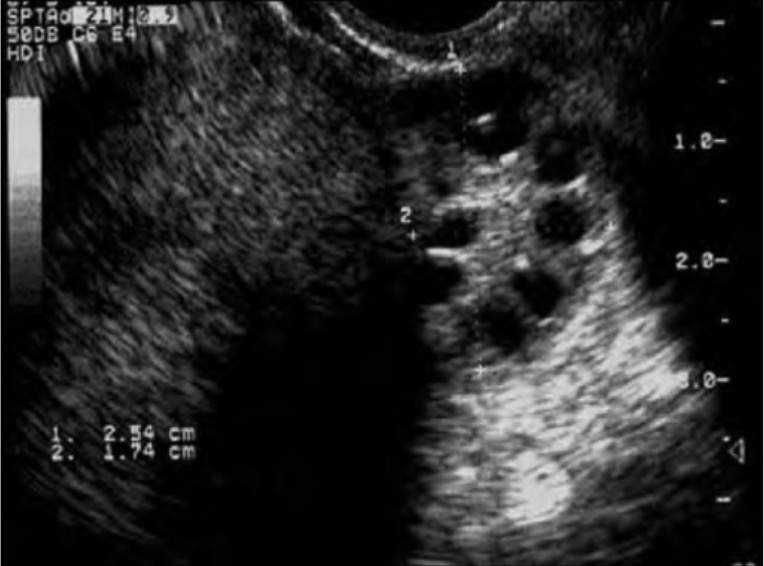
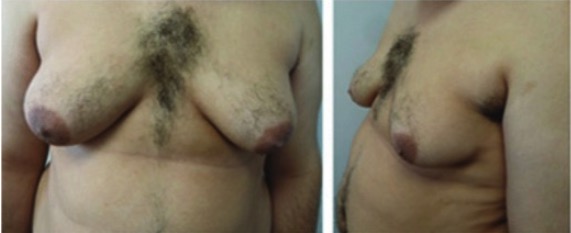
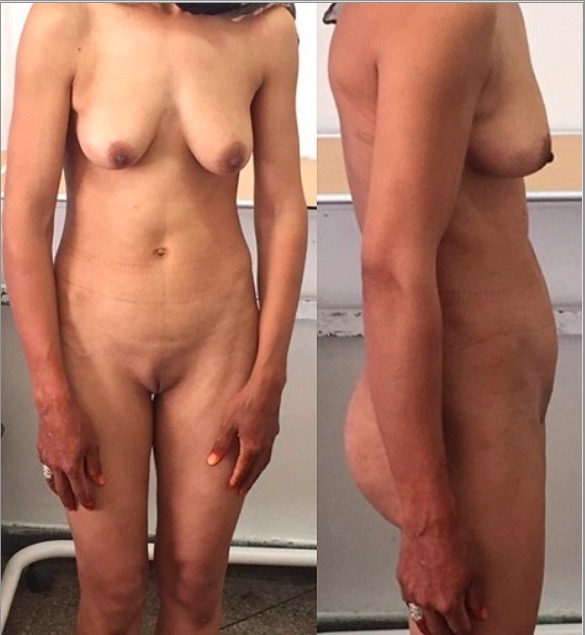
00:00 Let's have a look at a patient who has Klinefelter syndrome. The most common chromosomal abnormality that you will encounter will be the 47 XXY type. Take a look at the patient. Tall, lanky. Take a look at the arm span. So obviously you have a tall individual. And as a differential perhaps Marfan. But with Marfan, quite simple. Looking for issues in which the fibrillin gene, the elastic tissue and such has been compromised. And arachnodactyly so on and so forth. In Klinefelter, you'll notice that we have arm span that's quite long and then also take a look at the eunuchoid features. Eunuchoid referring to features of both a man and a lady. You'll notice that the breast here are gynecomastic. And at the same time though the facial features might be that of a male. A patient with Klinefelter may present with infertility. And this is due to the fact that, that there is loss of the sertoli cells or maybe even perhaps fibrosis taking place of the seminiferous tubules. Please picture in the testis the sertoli cells which are then responsible for proper maturation of sperm. Correct? Of course sertoli cells require the help of testosterone. And if the sertoli cells are either not there, then what may happen is that the sperm may not be properly formed and so therefore may result in infertility. Laboratory wise you're looking for increased levels of FSH and LH, and decreased levels of testosterone. 01:39 And the concept is exactly what you would expect with menopause as well. In which the inner layers, in this case we have the sertoli cells, has a hormone called inhibin. And so therefore when the sertoli cells are not present, inhibin is not present. 01:55 Inhibin more profoundly inhibits FSH. So therefore, if inhibin is not present in your Klinefelter patient, then FSH levels will be high. This patient with Klinefelter, how would they behave? Well up until puberty really there is no issue. So, difficult to actually diagnose prior to puberty. It's during puberty in which now the patient may not not start or finish typical pubertal development. So suboptimal type of functioning is important. Now the increase in FSH will then drive, well the estrogen. And here you will notice once again the gynecomastia that's taking place. So there are certain features that are ladily. Estrogen will bring about female secondary sexual characteristics as we, as I'd just mentioned. And keep in mind that the female secondary characteristic including the gynecomastia and the female distribution. Legs are disproportionately long as well as the arms as well. And because of gynecomastia there is an increased risk of going on to breast cancer. Here we have androgen insensitivity syndrome. So here is a child that's been born and you notice that for all intended purpose, phenotypically the child and the patient looks like a female. Take a look at the patient here over to the right. Phenotypically, looks like a female. However, genotypically notice that now we have chromosomes that are of the male type. X and Y. Loss of testosterone receptors. So therefore, anytime that there is there is loss of receptor activity, that hormone that should be working on it is always going to be elevated isn't it. For example, you've heard of pseudohyperparathyroidism or here in this case the receptors for testosterone aren't working. So testosterone levels are going to be quite high. Next, the problem is testosterone gives rise to the, well, the internal male structures. And those then would include in a male, vas deferens, your epididymis, the seminal vesicle. So that would be then your internal male structures but the testosterone and the receptors are not accepting it. So therefore that doesn't develop in this patient. Next, remember testosterone is converted into a hormone. A testosterone derivative with the help of finasteride. Excuse me, well finasteride will be the drug that targets the enzyme that we call 5 alpha reductase, correct? So 5 alpha reductase converts your testosterone into dihydrotestosterone. Well the problem is that is not happening either. Do you notice a penis in this patient? No. What about scrotum and such? No. The external male structures and the prostate is not present in my patient either. So absolutely no male structures in my patient here. Except for the obviously testis. Resistance also results in a loss of the negative feedback mechanisms that regulate LH release. So, you might find elevated LH levels. No conversion of your testosterone into DHT. And so therefore your patient doesn't have any external male structures, including the penis. 05:03 We do have the Y chromosome. And then with the sertoli cells, gives rise to your hormone that we call mullerian inhibiting factor. And because of the mullerian inhibiting factor being present in our patient here, we don't have the internal female structures which then include our fallopian tube, the uterus, the cervix, and the proximal 1/3rd of the vagina. We have a blind pouch. Let's have a look at a patient who has premature ovarian failure. The way that you want to approach this rather quickly, so you're able to identify your patient and move on, is the fact that this is a young lady. In young I mean less than 40. And she's presenting with exactly the same symptoms or nearly that of menopause. It's unfortunate. Now in menopause obviously there's no bleeding taking place in menopause. Remind me which hormone that you're looking for to be elevated? And that would be your FSH. That's because inhibin level will be; significantly will be FSH. That's because inhibin level will be lost due to the fact that you have your granulosa cells normally responsible for producing inhibin not being there. So FSH levels will be elevated. So if you have like young lady presenting with amenorrhea, there is no bleeding. Premature ovarian failure. Loss of the entire ovarian function. So therefore as I told you, the granulosa cells of the follicle are not producing inhibin. There is decreased estrogen and then inhibin which normally inhibit the release of FSH from the anterior pituitary. However, without that negative feedback mechanism, we will see a significant rise in FSH (to a much greater extent than LH). 06:38 And if you were to mimic menses. For example, at this point understand the concept please. This test known as a progesterone challenge test or the withdrawal test refers to the fact that you are mimicking the last stages of the menstrual cycle. So let's say that a young lady is on a 28 day cycle. 06:57 And then on the 28th day all hormones have been withdrawn. So therefore there is now apoptosis taking place of the endometrium resulting in sloughing off and then bleeding taking place. That's in normal patient. Our patient with premature ovarian failure, the ovaries are not present or excuse me, the ovaries are not functioning. And if they are not functioning, you are not going to have bleeding, negative of bleeding taking place in your patient. Here we have a patient with polycystic ovarian syndrome. So female, presents with amenorrhea and hirsutism. There is increased production of LH with an intact ovary. I emphasize intact ovary because in premature ovarian failure, we had an ovary that was completely not intact. So now, this patient please know you're going to begin here. What you have to accept is that a patient has increased LH. Next, LH is going to work upon the follicle. Intact ovary. Important that you understand that. LH then works upon the? Theca cells, correct? The LH receptor working and being triggered by LH. That increase in LH will cause an increase in production of testosterone. This testosterone will then give you the male hair like distribution which we then call hirsutism. Next, that testosterone will then be aromatized into estrogen. And then what happens now is the following. So now with this FSH being low in this patient with polycystic ovarian syndrome, that perhaps, perhaps the follicle is not going to be chosen. In other words, lack of development of a follicle in the ovary. If that follicle in the ovary does not develop and it sits there dormant, it is increasing its physiologic osmotic pressure isn't it? Now, this osmotic pressure is pulling in fluid into the follicle and then now we call this technically a cyst. So that statement there gives you the pathogenesis of the cyst like formation of polycystic ovarian syndrome. I remind you once again you don't have to find a cyst. So what's the criteria? Number 1, there will be oligoovulation. What does that mean? Well, there could possibly be ovulation. However, if a normal 28 days in average and on the 14th day approximately, you have LH surge and ovulation. If it's oligoovulation, instead of that occuring, well maybe it's a delayed or perhaps even it's absent. Number 1 criteria, oligoovulation. Number 2, clinically or laboratory. Clinically meaning observation by you the doctor, or number 2, interpretation of the lab. There are findings in this patient of hyperandrogenism. In other words, interpretation of the lab. There are findings in this patient of hyperandrogenism. In other words, you're going to find increase in testosterone obviously. And in clinically upon obeservation of your patient, you're going to find male hair like distribution aren't you. Those are all signs of masculinization. So that's two. If you find just those two androgen type of issues. And number 2, oligoovulation, that's good enough to diagnose polycystic ovarian syndrome. Now, just to be complete, guess what that third criteria is, the polycyst or multiple cyst in the ovary. But you only need 2 of the 3 criteria to diagnose polycystic ovarian. Be careful. Here we have estrogen and because you do have estrogen, if you're able to mimic the menses or the menstrual cycle, here in this case with polycystic or progesterone challenge test, you would indeed find positive for bleeding.
About the Lecture
The lecture Diagnoses of Reproductive Hormone Disorders– Reproductive Pathology by Carlo Raj, MD is from the course Reproductive Hormone Disorders. It contains the following chapters:
- Klinefelter Syndrome
- Androgen Insensitivity Syndrome
- Premature Ovarian Failure
- Polycystic Ovary Syndrome (PCOS)
Included Quiz Questions
Which of the following is NOT seen in Klinefelter syndrome?
- Male-pattern hair distribution
- Secondary sexual characteristics that start to appear after puberty
- Decreased intelligence
- Infertility
- Long arm span
Which of the following is NOT seen in Klinefelter syndrome?
- Increased inhibin
- At least one supernumerary X chromosome with a Y chromosome
- Increased estrogen
- Increased FSH
- Increased LH
Which of the following statements about androgen insensitivity syndrome is NOT true?
- It is usually discovered at preschool age.
- The condition presents as amenorrhea.
- Those affected by it are genotypic males.
- Those affected by it have testicles.
Which of the following patients has symptoms suggesting primary ovarian insufficiency (formerly known as premature ovarian failure)?
- 29-year-old female with amenorrhea
- 32-year-old female with multiple ovarian cysts and diabetes mellitus
- 35-year-old female with dysmenorrhea
- 32-year-old female with oligomenorrhea
- 51-year-old female with amenorrhea
Which of the following is NOT characteristic of primary ovarian insufficiency (formerly known as premature ovarian failure)?
- Increased inhibin
- A normal karyotype
- Increased FSH
- Increased LH
- Decreased estrogen
Which of the following is NOT usual in a patient with PCOS?
- Low testosterone
- Multiple ovarian cysts
- Diabetes mellitus
- Hirsutism
- Amenorrhea
Which of the following conditions is characterized by low DHT?
- Androgen insensitivity syndrome
- None of the other answer choices are correct.
- Klinefelter syndrome
- Premature ovarian failure
- PCOS
In which of the following conditions is a progesterone withdrawal test negative?
- Premature ovarian failure
- None of the answer choices is correct.
- Both premature ovarian failure and PCOS.
- PCOS
Customer reviews
1,0 of 5 stars
| 5 Stars |
|
0 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
7 |
7 customer reviews without text
7 user review without text