Playlist
Show Playlist
Hide Playlist
Psoriasis
-
Slides Psoriasis.pdf
-
Reference List Dermatology.pdf
-
Download Lecture Overview
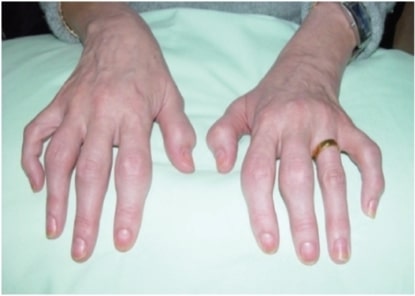
00:01 Okay. First up, is pustular psoriasis. 00:04 Now, this can be quite severe, as you can tell from this image. 00:07 It has a predilection for the hands and the feet -- -- the soles, that is, the soles and the palms. 00:12 And it's often interestingly enough precipitated by the wrongful use of systemic steroids to treat chronic psoriasis. As we'll see later, when we get to treatment, this is one of those few autoimmune conditions for which steroids is not helpful and may actually be quite counterproductive. The next subtype is called inverse psoriasis, so called because the lesions are the inverse of the typical plaque psoriasis. 00:35 Rather than having lesions on the extensor surfaces, you have them on the flexural intertriginous creases side. 00:42 So you might have them in the axilla. You might have them underneath the breast line, in the intergluteal cleft, or in the groin area. 00:49 The lesions look fairly similar to run-of-the mill plaque psoriasis. The difference is that you're unlikely to see the silvery scale. 00:59 Next up is erythrodermic psoriasis, and this is the least common form. 01:04 It's characterized by generalized erythema and scaling from head to toe. As you might imagine, with such significant involvement of the skin, it's associated with significant electrolyte derangements and systemic infections. This one is also like pustular psoriasis, often precipitated by the injudicious use of systemic steroids. Next up, we're coming to the end, is guttate psoriasis. A little etymology point here. Guttate comes from the same latin word that gout comes from, which means drops. 01:37 Gout was believed to be excess fluid or toxic humors in the joints, and in this case, guttate psoriasis refers to dewdrop lesions all over the skin. They're typically less than a centimeter in size. 01:48 You'll find them on the torso and on the proximal extremities, as depicted in our image here. It may come on fairly acutely, unlike some other forms that are more chronic in nature. 01:59 And it's been linked with recent streptococcal infection for reasons that aren't entirely clear. 02:04 Next up, finally, we've reached plaque psoriasis. Now, this is the most common variant and the one that I presume you're all familiar with. 02:12 It's characterized by the symmetric distribution of lesions to the extensor elbows, the knees, the scalp, and oftentimes, around the umbilicus. 02:19 And a very good example of it is shown here in this image. 02:23 It may have features of some of the other subtypes. 02:26 There may be some lesions in interdigital creases, like in the intergluteal cleft. 02:30 There may be some small pustules on the hands, as well. 02:33 Classically, there's nail involvement, and this may involve nail pitting, onycholysis, and a lesion called oil spotting, which is basically onycholysis on the nail plate. 02:43 Lastly, these lesions may in fact be pruritic. 02:47 So that's plaque psoriasis. Okay. Having spoken about the 5 different subtypes of psoriasis, I think we can say that our patient, who's presenting with waxing and waning lesions on his extensor surfaces of his elbows and his knees, as well as some nail findings that are classic, it looks like this guy has plaque psoriasis. 03:04 So having discussed the type of psoriasis we're looking at, why don't we jump a little bit into some pathophysiology. 03:11 So, psoriasis is a complex immune-mediated disease of T cells and dendritic cells, which is leading to the hyperproliferation of keratinocytes. 03:21 Essentially, a thickening of the skin. 03:23 It can actually start at any age with an equal male to female prevalence. 03:27 There are certain risk factors that we should think of, though. 03:30 So smoking is a risk factor, alcohol, obesity. 03:34 Interestingly enough, TNF alpha inhibitors, while they're sometimes used to treat psoriasis, strangely enough can actually manifest with worsening psoriasis. 03:43 Other things to think about are Lithium and HIV disease is associated with worse psoriasis. 03:49 So it's important to recognize that 30% of patients who have psoriasis will develop psoriatic arthritis and this is one of the axial spondyloarthritis. It's a chronic, progressive, peripheral arthritis and it most commonly afflicts the distal interphalangeal joints and the sacroiliac joints. 04:06 These are destructive, erosive lesions and it can be quite debilitating. 04:10 Just like all the other axial spondyloarthritis, it is associated with the HLA B27 haplotype. 04:17 In addition, patients with psoriasis oftentimes can develop ocular symptoms like scleritis or episcleritis. 04:23 Other autoimmune diseases may be found in patients with psoriasis as well. 04:27 And as a chronic inflammatory disease, you should also be mindful of the increased risk of cardiovascular disease. 04:33 This is really a clinical diagnosis. There are some classic features that we see with psoriasis, so biopsy is rarely indicated. 04:40 So let's take a quick look at some of the key features of this case again, just to highlight some key points. So this was a 33-year-old man. 04:47 That is a pretty typical demographic for someone having psoriasis. 04:51 He states that his lesions have been coming at various times over the past several years. Psoriasis is one of those chronic relapsing remitting diseases that typically resolving spontaneously in the summertime. For some reason, some patients do have symptoms that come and go with seasonal variation. The lesions are itchy. 05:07 This is not always the case, but certainly these plaques can be pruritic. 05:11 The fact that he smokes a pack per day, definitely relevant oth by virtue of the fact that it can increase his risk of developing worsening psoriasis, but also, again, with a chronic inflammatory disease, quitting smoking is going to be very important to reduce his risk of cardiovascular disease down the road. 05:27 And next, his family history is definitely important. 05:30 aving an uncle with ankylosing spondylitis means that he has a family history of one of the axial spondyloarthritis, which is going to increase his risk of developing psoriatic arthritis. 05:43 On the physical exam, one of the important findings that we had commented on before was when scraping off one of the plaques, it caused punctate bleeding. 05:52 This is a classic finding called Auspitz sign and it's just something to look for that you might find on the boards. 05:58 So let's start talking about the management of psoriasis. 06:01 Like many conditions, we have a stepwise approach to addressing the problems of psoriasis. First off, for a limited disease, we're exclusively going to use topical agents. 06:11 This may involve just emollients to soften up the skin, vitamin D analogs like, calcipotriene, medium to high potency corticosteroids like clobetasol, or retinoids, like tazarotene. For moderate to severe disease in contrast, we're going to use topical agents in combination with systemic therapy. This may involve simply PUVA, or a type of phototherapy. We may add on immunomodulators like methotrexate or cyclosporine. 06:37 Or we could use the biologic medications like TNF inhibitors and anti-IL-17 agents. Importantly, as I mentioned before, anti-TNF agents, ironically, while being used to treat psoriasis, have been shown to sometimes exacerbate psoriasis. 06:52 So that's something that you would necessarily have to be watching for. 06:57 Okay. So let's highlight some key points. Psoriasis is a chronic, relapsing, inflammatory skin disease with multiple phenotypes as we've discussed. It's a T cell-mediated hyperproliferation of keratinocytes. 07:12 It causes erythematous plaques, most commonly with thick, silvery scale. 07:17 There are symmetric extensor surface distribution, there's often going to be nail findings with nail pitting or onycholysis. 07:24 And we're going to use a stepwise approach: topicals, up to systemic treatment with biologics or UV radiation.
About the Lecture
The lecture Psoriasis by Stephen Holt, MD, MS is from the course Allergic and Immune-mediated Skin Disorders.
Included Quiz Questions
Which of the following may be precipitated by wrongful use of systemic steroids?
- Pustular psoriasis
- Guttate psoriasis
- Intertriginous psoriasis
- Nail psoriasis
Which of the following nail abnormalities is associated with psoriasis?
- Nail pitting
- Onychomycosis
- Yellow nail syndrome
- Beau lines
Which of the following statements is true?
- Psoriatic arthritis is associated with the HLA-B27 haplotype.
- A skin biopsy is necessary for the diagnosis of psoriasis.
- Psoriatic arthritis typically spares the sacroiliac and distal interphalangeal joints.
- Auspitz sign refers to the development of psoriasis over sites of injury.
Which of the following statements is correct?
- TNF inhibitors are used for the treatment of psoriasis, but they are occasionally linked to its exacerbation.
- Because of the increased risk of cutaneous malignancy, phototherapy is indicated only for limited psoriasis.
- Female patients with childbearing potential must have two negative pregnancy tests before calcipotriene is initiated.
- The wrongful use of systemic steroids to treat chronic psoriasis has been linked to inverse psoriasis.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |