Playlist
Show Playlist
Hide Playlist
Proximal Convoluted Tubule (PCT): Pathology
-
Slides PCT ClinicalEffectsSyndromsandDiseases RenalPathology.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
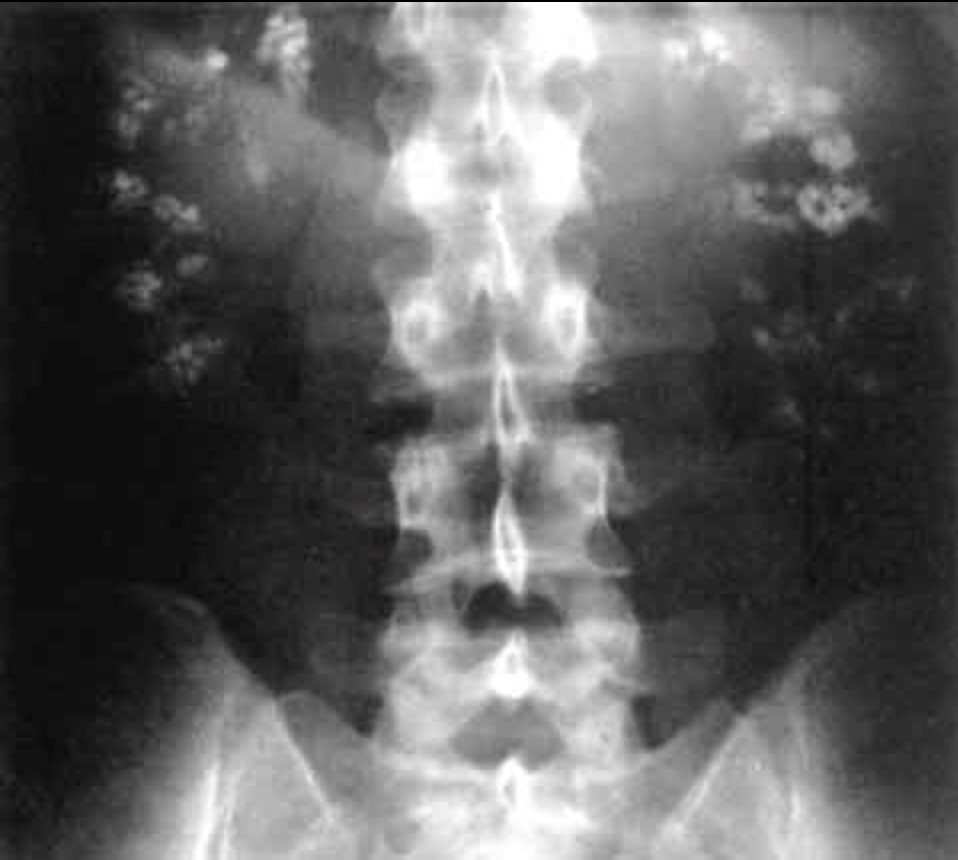
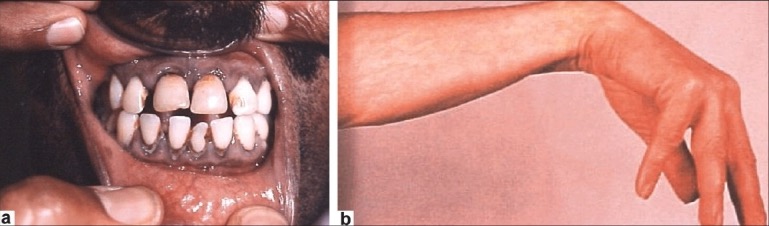
00:01 Now, in the PCT, we are going to wrap this conversation up in the PCT by looking at important pathologies of the PCT. Begin by looking at hartnup disease and then we will walk through cystinuria, Fanconi syndrome, obviously I am emphasizing syndrome on purpose, and type II RTA. With heavy metal poison, we will take a look at lead or mercury. Lead we will spend a lot of time with. You tell me sideroblastic anemia, why? Quick review. It inhibits two enzymes. One is called ALA, it's a synthase or it is going to be dehydratase? Good. Dehydratase. Take the D in lead and do dehydratase. 00:55 Look for that enzyme, not synthase, is that clear? The other enzyme would be ferrochelatase. 01:00 We will use that information later on when we do our sideroblastic anemia, but you should know in the meantime the lead also causes what? Lead nephropathy. They cause damage to the PCT. The proximal convoluted tubule will undergo a second example of coagulation necrosis. Second, what was the first? Obviously, know about the heart. Isn't that the prototype when we talk about coagulation necrosis? What does that mean? Take the g in the coagulation and you may want to call it ghost town. What happens when you walk into a ghost town? No people, but the architecture is preserved. Look at all the buildings. You see them. It is the ghost town. That is what the organ looks like. The architecture is preserved, but there is nobody home. Who is nobody? The nucleii. The nucleii are up or dead? How do you know? It is called necrosis. What does that mean? Cell death. So, therefore, proximal convoluted tubule or tubular epithelial cells, if they undergo ischemia, they then result in coagulation necrosis. Let me take you one step further. If you did have death of the PCT and the two epithelial cells are dead, they're falling into the urine. Everything is crumbling. It is falling into the urine. They are being sloughed off. They might then aggregate together. What is an aggregation of cells known as in the urine? It's called a cast, good. What am I referring to right now? It is called acute tubular necrosis. What is in my hand? A cast. What kind of cast? It is called a multi brown granular cast. We will talk about that later with ATN. Make sure that you are able to integrate all this. Move on. Now produce a nephrotoxic acute tubular necrosis. Heavy metal poisoning specifically focused upon lead, please. Now all the normal PCT functions are destroyed when you have damage. So think of Fanconi syndrome, think about acute tubular necrosis may be due to lead poisoning so on and so forth. If that PCT is dead, oh! my goodness, I cannot reabsorb 66 percent of my sodium. Welcome to hyponatremia. 03:15 I cannot reabsorb my 99 percent of glucose, hypoglycemia. And I cannot take up my uric, literally it's hypourecmia. Remember with uric acid that will be an important component when we have our discussion and further explained upon gout and such. But in general, if your PCT is dead, you are losing a lot of things. Emia means blood. Hypo means lack that of because you are losing it. Also, if you have destruction of your PCT, you have completely lost the homeostatic mechanism for phosphate. Remember that vitamin D and PTH work opposite. Listen. 04:00 Vitamin D and PTH work opposite when it comes to phosphate. Vitamin D is going to cause reabsorption of phosphate, whereas PTH wants to get rid of it. But when your PCT is dead, please understand the homeostatic mechanism has also been lost. What else? Well you are not able to properly reabsorb bicarb, amino acids and those have been lost. Now hold on for one second here. If you have destruction of PCT, stop. I am not able to reabsorb bicarb. 04:29 Are we clear? No chance of carbonic anhydrase working properly. Bicarb gets lost. What about in the plasma? I don't have as much bicarb because things are being lost. So, therefore, tell me about the renal threshold for bicarb with reclaiming it. It is decreased, isn't it? There is decreased renal threshold for bicarb reclaiming. Do you understand the English and the terminology that I just put forth? So if there is decreased renal threshold for reclaiming bicarb, what happens to your bicarb? What is your normal plasma level? 22 to 26. 05:06 If you are losing your bicarb here in the urine, then my bicarb drops down to maybe 15. What is my pH in your plasma? Decreased. What do we call this clinically? What is your diagnosis? It is called renal tubular acidosis. What kind and where am I? Proximal. See that X please. See the X. How many lines did it take to form that X? One, two. Oh! yeah, two. 05:39 So type II renal tubular acidosis is in the or is of the proximal renal tubular acidosis. 05:47 Is that clear? Type II RTA is of the proximal convoluted tubule. Do not ever forget that. 05:53 It is the inability of your PCT to reabsorb the bicarb. I don't care how it happens, destruction of the PCT, you decrease renal threshold of bicarb reclaiming. Let's move on. 06:09 Now ultimately when you have generalized dysfunction of the entire PCT, maybe it is due to lead poisoning maybe it is heavy metals, what have you, but then generally speaking this is called Fanconi syndrome. So what is Fanconi syndrome? Do not confuse this with, those of you that might have heard of the diagnosis Fanconi anemia. One has nothing to do with the other. 06:31 Do not confuse the two. Fanconi syndrome is only dealing with the PCT. It is generalized dysfunction and so, therefore, you are going to end up losing everything that we just talked about. You have hyponatremia. You will end up losing a calcium, end losing a phosphate, end up losing your bicarb, get my point. But this is only in the PCT, only. Fanconi syndrome will not affect the DCT or collecting duct, but the only difference between syndrome and anemia in Fanconi anemia, you want to think of that as being bone marrow disease and it is an aplastic anemia. Think about where are you at, bone marrow. Leave that seperate. That is anemia. This is Fanconi syndrome. Is that clear? Please do not get the two confused. 07:13 PCT.
About the Lecture
The lecture Proximal Convoluted Tubule (PCT): Pathology by Carlo Raj, MD is from the course Diseases of the Nephron.
Included Quiz Questions
Which of the following casts are most likely found in a patient with lead nephropathy?
- Muddy brown casts
- Hyaline casts
- RBC casts
- Fatty casts
- Waxy casts
What type of anemia would you expect to find in a patient with lead poisoning?
- Sideroblastic anemia
- Megaloblastic anemia
- Fanconi anemia
- Aplastic anemia
- Iron-deficiency anemia
Which of the following is not associated with acute tubular necrosis?
- Megaloblastic anemia
- Muddy brown casts
- Necrosis of proximal tubule cells.
- Ischemia
- Mercury poisoning
Which of the following is not found when the proximal tubule cells are damaged?
- Hypernatremia
- Aminoaciduria
- Glucosuria
- Hypouricemia
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |