Playlist
Show Playlist
Hide Playlist
Leukemia: Polycythemia – White Blood Cell Pathology
-
Slides Leukemia White Blood Cell Pathology.pdf
-
Download Lecture Overview
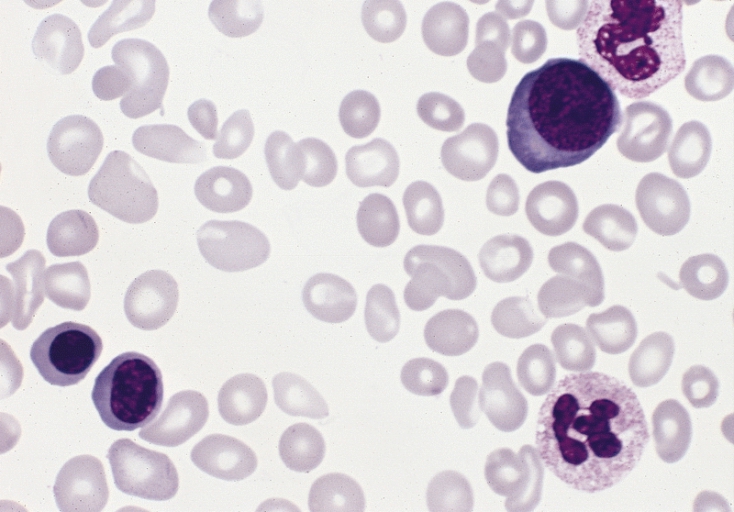
00:01 Our topic here is polycythemia. 00:04 What does it mean to you? Polycythemia means excess increase in RBC mass. 00:10 Only? Well, it depends. 00:12 I'm going to walk you through a very important table coming up. 00:14 Primary polycythemia. It's absolutely independent of erythropoietin. 00:22 Independent. That means what? That means that you would find the tumor, the neoplasia, within the bone marrow. 00:30 Welcome to polycythemia vera. 00:32 So, what do you think my erythropoietin level will be in a patient that has primary polycythemia? Decreased, decreased, decreased. 00:40 It shuts erythropoietin levels down. That must be understood. 00:44 Next, if you have a primary neoplasm in the bone marrow, it has a choice of really producing anything it wants. 00:51 It can produce your, let's say your RBC, it can produce a lot of platelets but for thrombosis. 01:00 It can produce a heck of a lot of basophils, it can. 01:03 And if it does, now your patient takes a hot bath and feels, "Hey, doc, I feel itchy." There's itchiness taking place after a hot bath. 01:12 Pruritus after hot bath, ladies and gentlemen, that is going to be polycythemia vera. 01:18 Why? Due to excess basophilia. 01:20 Primary. Secondary. Secondary means any cause that caused an increase in EPO. 01:29 Thus, specifically increase in RBC mass. 01:34 For example, what if you had a patient that was in high altitude? Hypoxia. 01:40 Maybe about three weeks later, that hypoxia is going to trigger the kidney through this erythropoietin. 01:47 Erythropoietin works in the bone marrow to increase RBC mass. 01:51 Welcome to secondary polycythemia. Hypoxia, cause number one. 01:56 Cause number two, maybe your patient had an erythropoietin cancer. 02:01 What do I mean? An erythropoietin paraneoplastic cancer. 02:04 So renal cell carcinoma, that might be producing too much erythropoietin will cause what kind of polycythemia? Secondary polycythemia, or you can have athletes. 02:15 Most recently, embarrassingly, the athlete that was stricken of all of his awards from Tour de France, Lance Armstrong. 02:25 He was blood doping. 02:27 He was taking injections of EPO so that he can win all his races. 02:31 Of course, whatever, he got busted, but the point is blood doping is an example of secondary polycythemia. 02:38 Chronic hypoxemia, paraneoplastic, or blood doping are causes of secondary polycythemia. 02:45 Increased EPO, increased RBC mass, secondary polycythemia. 02:50 Are you going to find itching here with hot bath? No. 02:54 Erythropoietin only stimulates what? Erythrocytes. 03:00 Polycythemia vera, everything. 03:02 Why? It's independent of EPO. 03:05 It is a neoplasia in the bone marrow producing any cell that it wants, including what? Including basophil. 03:12 Therefore, causing, perhaps, hot bath kind of pruritus because of release of? Histamine, histamine. 03:19 Polycythemia vera, it's one of the myeloproliferative disorders. 03:22 If you want, do this for me. 03:24 With myeloproliferative disorders, you group three together, PPP. 03:29 PPP, polycythemia vera. If you want to do this, you may do primary thrombocythemia. 03:37 And you have this one, and you want to call this chronic myelogenous leukemia, but then you have another one called your primary myelofibrosis. 03:45 We talked about that earlier as being a space occupying lesion resulting in leukoerythroblastic picture. 03:50 So, there will be a total of four myeloproliferative disorders; polycythemia vera, essential or primary thrombocythemia, primary myelofibrosis, which we talked about in anemia, and we have chronic myelogenous leukemia, which we discussed already in leukemias, 9 and 22. 04:13 With vera, markedly increased RBC on peripheral blood smear. 04:16 Increased RBC and myeloid precursor in your bone marrow. 04:20 Everything is increased, except the fact that the EPO has been shut down. 04:25 I have a tumor within my bone marrow. 04:28 You take a look at the left here and we find wide-open spaces, and those are your fat vacuoles. 04:33 Where are you? Bone marrow. That's normal. 04:36 In the middle there would be a pool of stem cells. 04:40 On the right is a bone marrow with polycythemia vera. Look at that. 04:44 Do you see the open spaces of fat vacuoles? Nope. They're gone. 04:50 Crowding, congestion. This is not fibrosis, please. 04:53 This is in fact polycythemia vera with the congestion in too many stem cells. 04:59 How's the patient going to present? Hyperviscosity syndrome. 05:05 Also, I told you about pruritus with hot bath. Vera, trilineage expansion. 05:11 You're going to have increase in RBC, increase in granulocytes including your basophil, and thrombocythemia. 05:18 Please note that you have decreased erythropoietin. 05:21 Normal range, if you want to remember for EPO, it would be between 11-48. 05:25 What's absolutely important here to make sure you know that you have a low erythropoietin. 05:31 Secondary polycythemia shows expansion of RBC only. 05:35 Here, you'd find a high erythropoietin. Our topic here is secondary polycythemia. 05:41 An increased RBC mass, more viscous. 05:43 Therefore, from head to toe, you have thrombosis, thrombosis, thrombosis. 05:48 Stroke, hyperviscosity, bowel infarction, Budd-Chiari, hepatic vein thrombosis. 05:56 You get the point. So, hyperviscosity involved in many of your polycythemias. 06:02 EPO here, in secondary, high. In polycythemia vera, low. 06:09 An important table for us to walk through. You're going to like this. 06:15 Everything that you need to know about polycythemia is on this graph. 06:19 Pay attention. I'll walk you through a step by step by step. 06:22 Let's first begin. I want you to take a look at the bottom of this illustration. 06:28 You'll notice a saturation of oxygen in erythropoietin. 06:31 I want you to pay attention to first column on your left, and you see it to be normal. 06:38 That small green box that you're seeing there that's filled, that represents saturation of oxygen. 06:46 Patient A, I'm going to walk you through these scenarios as different patients. 06:52 Patient A, the normal patient, normal saturation of oxygen. 06:56 N is normal. N, normal erythropoietin, normal RBC mass. 07:01 Now, you see this black line here, demarcated? If you move further down, this would indicate an increase in RBC mass. 07:11 Right now, the control is what you see here. 07:15 Above the line which is the shaded green represents plasma volume. 07:19 If you go much above that line, this represents an increase in plasma volume. 07:24 This is normal control. Patient A, here are my parameters. 07:29 Let's take a look at Patient B. 07:32 Patient B, what is the only thing that you see in this patient? Volume depletion. 07:39 Would you please take a look at plasma volume? I want you to compare the normal and his or her plasma volume versus volume depletion, and you see it to be decreased. 07:50 "Why is this even here, Dr. Raj?" Are we talking about polycythemia? Correct. 07:55 If you have volume depletion only, doesn't it appear within your circulation that you have an increase in RBC mass? Yes. 08:04 Why? Because of plasma volume depletion. 08:06 What do you call this type of polycythemia? Relative, relative, relative polycythemia. 08:13 Next, well, Patient C and Patient D. 08:17 You're going to group them together, only because patients C and D both have a condition called secondary polycythemia. 08:25 Really? Mm-hmm. Patient C will be appropriate, Patient D will be inappropriate, but both will have absolute, absolute increase or absolute polycythemia. 08:39 Secondary type. So let's take a look at Patient C. 08:42 What happened here? Why is it appropriate, Dr. Raj? Well, you see the saturation box, that little box? Normal, the green box had been filled. 08:51 I want you to now walk over to Patient C, and you see that now the box is only half filled. 08:57 Uh-oh. So, when your saturation of oxygen decreased, give yourself an example. 09:01 High altitude. High altitude, you would have decreased access. 09:06 So you would have, at some point, decrease in PbGeO2, and you have a decrease in saturation of oxygen, okay? So, when you have a decrease in saturation of oxygen, what's going to kick in? Take a look, kidney with EPO. That would be number two. 09:24 You have an increase in EPO. So this is an absolute increase. 09:29 Is this appropriate? Yes, it's hypoxia, your high altitude, whatever. 09:34 Whatever the reason, hypoxia might be, ventilation, perfusion, diffusion defect, whatever it may be, hypoxia, resulting in increased EPO. 09:43 What does that increased EPO going to do? Is it going to affect plasma volume or RBC mass? RBC mass. 09:50 Take a look at number three. That's RBC mass, and you find that to be increased. 09:57 Compare RBC mass in that patient, Patient C, to Patient A. This is absolute appropriate. 10:05 Let's take a look at Patient D, the fourth one from your left. 10:10 Here, you'll find the following. Saturation of oxygen, the square box, perfectly normal. 10:18 You'll begin with erythropoietin, the orange shaded area. 10:22 That's number one. That increased in EPO is then causing number two. 10:28 Is it RBC mass? You see that green rectangle or the bar, and it's increased. 10:35 That's the consequence of increased EPO. 10:39 What's causing the increased EPO here if it wasn't the saturation of oxygen? Renal cell carcinoma, paraneoplastic. 10:49 So this would be absolute polycythemia, inappropriate type. 10:54 Both patients C and D are secondary polycythemia. 10:59 Both of these patients have an increase in EPO. 11:02 Take a look at the blue shaded box and the orange shaded box. 11:07 You find that EPO levels are increased. 11:10 Secondary polycythemia, and that is how things are worded. 11:14 Absolute appropriate, absolute inappropriate. 11:17 What kind of polycythemia is it called when there's volume depletion? Relative polycythemia. 11:24 Finally, we come to Patient E. The final patient all the way to the right. 11:30 Where do you begin here? Number one, RBC mass. 11:36 That's where you begin. Where is my tumor? In your bone marrow. 11:42 Who is your patient? This patient taking a hot bath, feeling itchy. 11:48 You see him or her? Polycythemia vera. It's a myeloproliferative disorder. 11:53 If you have an increase in RBC mass, what's my consequence? Take a look at the red shaded area, a decrease in EPO. 12:02 Number two, you're done, you're done. 12:06 Here's everything that you need to know about polycythemia. 12:08 You go from normal to relative to two different types of absolute, appropriate or inappropriate, and then you have primary polycythemia or polycythemia vera, and that's your JAK2 stat. 12:22 That polycythemia vera patient, bath, pruritus, splenomegaly, and thrombosis. 12:28 Most common cause, MCC stands for most common cause of death. 12:32 From where? Oh my goodness, IVC thrombosis, super vascular accident, so on and so forth. 12:39 Spend a little bit of time. 12:40 Make sure that you go through this bar graph for all the differentials that I've given you for polycythemia, and you keep going over this and over this and over this with me, there's no way you're going to miss a question.
About the Lecture
The lecture Leukemia: Polycythemia – White Blood Cell Pathology by Carlo Raj, MD is from the course Leukemia – White Blood Cell Pathology (WBC).
Included Quiz Questions
Which of the given etiological factors causes increased levels of circulating red blood cells, independent of erythropoietin production?
- Polycythemia vera
- High altitude
- Blood doping
- Lung disease
- Renal cell carcinoma
Which of the following conditions features a prickly sensation after a hot bath?
- Polycythemia vera
- Acute myeloid leukemia
- Hairy cell leukemia
- Acute lymphoblastic leukemia
- Renal cell carcinoma
Which of the given conditions is NOT caused by polycythemia vera?
- Thrombocytopenia
- Strokes
- Pulmonary embolism
- Heart attacks
- Hyperviscosity syndrome
What do you call the type of polycythemia that results from plasma volume depletion?
- Relative polycythemia
- Chuvash polycythemia
- Primary polycythemia
- Physiologic polycythemia
- Absolute polycythemia
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Great lecture. Thanks you for the detailed discussion. I like Rajs lectures- this is one of the best