Playlist
Show Playlist
Hide Playlist
Phagocytosis – Inflammation and Wound Repair
-
Slides Inflamation Cellular Pathology.pdf
-
Download Lecture Overview
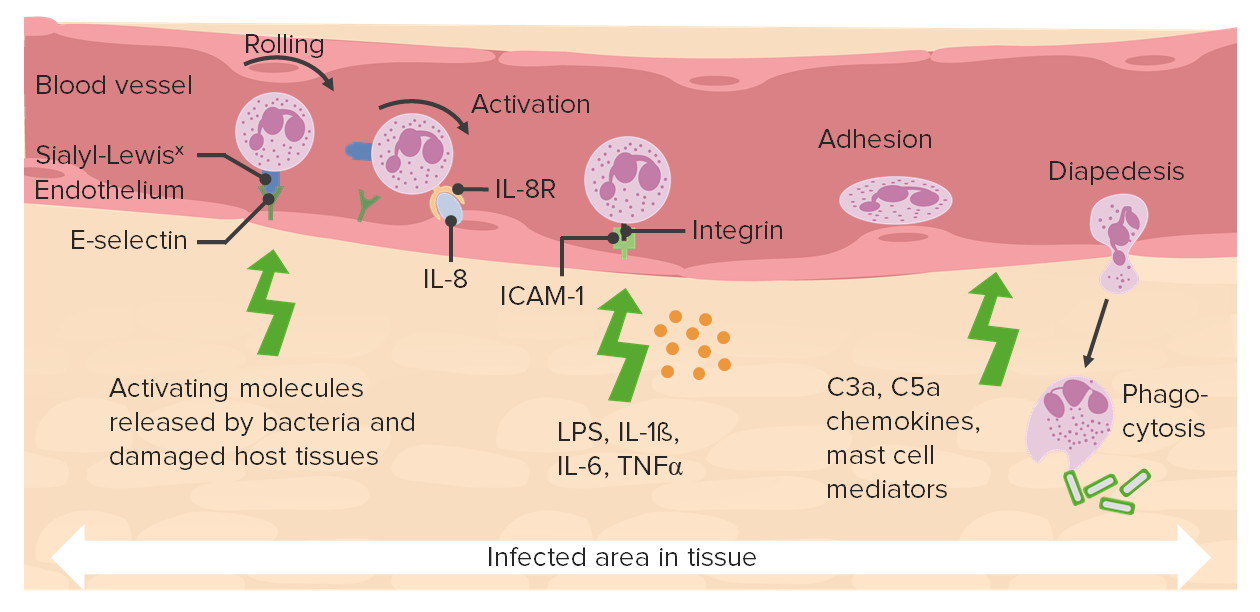
00:02 In this picture, with phagocytosis I want you to understand what's going on in great detail. I want you to begin with the inset picture on the left, and that is a neutrophil. Where are you right now in terms of acute inflammation? The neutrophil has left the blood vessel. It has now approached the bacteria in my interstitium which you call an exudate and we are about to engulf our bacteria. I have taken this neutrophil the inset and we blown it up in this picture, completely blown it up. I've given you a little area here in the middle where we are going to swallow and engulf the bacteria. 00:47 If you take a look at that green pellet, it says bacteria. You are going to take this up, and when you do this is where we begin. 00:57 Your first enzyme you see there is NADPH oxidase. I repeat NADPH, not NADH. Is that understood from biochemistry. 01:13 You tell me where NADPH is produced in biochemistry. You've heard of HMP shunt or the hexose monophosphate shunt or pentose phosphate pathway. Lot of P's huh. Can you picture that. Would you tell me what the rate limiting enzyme is in your HMP shunt. Good. Glucose-6-phosphate dehydrogenase or G6PD. You must have NADPH so that you can properly form NADPH oxidase. 01:49 So you can take the oxygen. Once again would you tell me what cell this is. A phagocytic cell, good. And perfectly normal for a phagocytic cell to create free radicals. I am walking you through this very methodically because now we actually are going to inject pathologies and you may or may not have seen this pathologies. So there is going to be new information here that you want to be very clear about. Up until now I have been really quick with the information. 02:21 Now we have created the most important free radical at this point. This is called a superoxide. You see that superoxide. 02:29 So you have created it. How did you create it? With the help of NADPH oxidase. Let's stop here for one second. I said pathology. 02:38 What if you have a patient that is deficient of NADPH oxidase. And you have a child that has recurrent infections. 02:46 Recurrent infections especially to catalase positive organism. Welcome to chronic granulomatous disease. Right. At some point I will walk you through a table where I am going to go through the details of some of these diseases. Let's continue. 03:05 So now you have formed a superoxide. Now you have a next enzyme. It's called a superoxide dismutase. Perfect. 03:12 And you are going to create another very important component. That's called H2O2. What's another name for H2O2? Hydrogen peroxide. Very important that you know about hydrogen peroxide. Let's talk about a few things here. See that iron, Fe, can you tell me a condition in which iron might be overloaded? Haemochromatosis. What does iron damage? Oh my goodness everything in the body. Skin, heart, pancreas, gonads, everything. How is it causing such damage? You have heard of Fenton reaction. What does that mean? Iron or maybe perhaps copper may then take the hydrogen peroxide it may create a free radical. And if this free radical is found outside the neutrophil in excess it's going to cause massive damage to normal tissue. Are we clear about Fenton reaction. Let's continue. So now we have formed a hydrogen peroxide. 04:19 In a neutrophil, you take this one step further and you must know the enzyme MPO, myeloperoxidase. That myeloperoxide will form a very important type of free radical in which it cause ultimate destruction of this bacteria. Welcome to bleach, amazing huh. 04:39 The inner body, we produce bleach. Unbelieveable. Hypochlorous acid. This takes care of the bacteria, myeloperoxidase. 04:48 Okay in the meantime, so you have engulfment of a bacteria, picture that. Just because you engulf something, does it mean that you kill the bacteria? No. Would you tell me in a neutrophil, it's origin, is called a granulocyte is'nt it. 05:09 What does the granule contain in a neutrophil? These enzymes, these hydrolytic enzymes. You see them. NADPH oxidase, the myeloperoxidase, okay. So you have taken out the bacteria but then you have the granule that has to make it's way. 05:27 And then it combines with phagosome and then you form a phagolysosome. It's only when you have proper fusion of the granule containing the enzyme and this phagosome containing the bacteria. Kind of like a video game. They combine and once they do, destruction of the bacteria. Simple enough. I know I was being silly there but it works I hope. Give you another pathology. 05:51 What if the lysosome, the granule does'nt properly make it's way over to the phagosome. And you don't kill your bacteria. 06:00 What's the name of that disease? Good, that's Chediak Higashi. Two diseases here right off the bat. NADPH oxidase deficiency, chronic granulomatous disease or don't properly migrate your lysosome over this then results in Chediak Higashi disease. 06:19 Spend a little bit time. Not to worry I will give you further details. In the meantime, I want you to take a look at something else here. There is my hydrogen peroxide and by that I mean take a look at the right side. There is my hydrogen peroxide and with that hydrogen peroxide you will notice that you have glutathione taking care of that hydrogen peroxide. 06:40 How do you form reduced glutathione, that GSH? You need NADPH. How do you form that NADPH? The G6PD. Glucose-6-phosphate dehydrogenase. 06:52 I want us to stop here. I am going to give you a third pathology. From henceforth, every single time that you hear about NADPH you should be thinking biochemistry, has to be G6PD. Good. And what if you're deficient of that enzyme. Who's your patient most likely in G6PD deficiency. Well, maybe African. And really it's an X-linked recessive, right, X-linked recessive. 07:21 So you need to have proper amounts of G6PD so that you can then create the NADPH so that you can have proper reduction of your glutathione. So you can protect yourself against the free radicals. Alright, okay. Now, is it possible with G6PD deficiency, usually when you think about G6PD deficiency may I ask you; Are you going to be dealing with this cell. What is this cell? A neutrophil. No. Usually right you think G6PD deficiency Dr. Raj that is hemolytic anemia. 07:53 That is an RBC. Why are you even talking about it here? Because when you have a patient and you're reading a stem of a question. 08:02 You are reading a chart of a patient. And they have hemolytic anemia and they are susceptible to catalase positive organims. 08:11 This patient has G6PD deficiency. Okay, Dr. Raj I understand that the patient ate fava beans and they ended up developing hemolytic anemia, I get that. Because now the RBC cannot protect itself. But why is the patient susceptible to catalase positive organisms? What's the name of that enzyme that we just talked about that's responsible for creating superoxide? Take a look. NADPH oxidase. In G6PD deficiency, you cannot produce any NADPH. If you can't produce NADPH, how can you form NADPH oxidase. Is that clear. You can't. Two cells that are damaged in G6PD deficiency; RBC's, neutrophils. 09:06 No other condition is going to give you such a recurrent type of behavior. So what about in chronic granulomatous disease, what did you learn about that in Immunology. Only a patient that is susceptible to catalase positive organism. 09:23 There is no such thing as NADPH oxidase and RBC to protect the RBC. Only the neutrophil. Three pathologies from this diagram and more information that I've given you here Fenton reaction and myeloperoxidase. Spend time here, make sure that you're completely comfortable with everything that I've talked to you about with enzymes and the biochemistry. The last little point that I want you to make. I want you to go to the right top. See the bacteria there. It's covered by chocolate. What? No, I'm being serious but it's covered by C3b. What am I referring to? I'm not a huge fan of strawberries, okay. 10:07 But you put that strawberry in chocolate, I cannot get enough. So, what is it that you're taking the bacteria think of it as being a strawberry. In all seriousness, you are taking the bacteria, you are dipping it into chocolate making it mighty tasty for the neutrophil. It's called an opsonin. You see the bacteria. The chocolate is the C3b. 10:28 It's an opsonin also IgG. You are making it really really tasty for the neutrophil to then bring about phagocytosis. 10:38 Is that clear? If it is, good. If it's a little bit too much, digest this accordingly. Lot of good information. 10:47 All of this that I've talked about is high yield at any point in time. In Pathology, Biochemistry, Immunology, questions will arise.
About the Lecture
The lecture Phagocytosis – Inflammation and Wound Repair by Carlo Raj, MD is from the course Cellular Pathology: Basic Principles with Carlo Raj.
Included Quiz Questions
Which of the following is required for the production of the free radical superoxide?
- NADPH oxidase
- NADH
- OH
- GSH peroxidase
- G6PD
What causes damage to normal tissues in patients with hemochromatosis?
- Overproduction of free radicals
- Oxidation of other metals
- Deactivation of superoxide dismutase
- Overproduction of HOCl
- Rapid consumption of NADPH
Which disease is due to the failure of the phagosome to fuse with the lysosome?
- Chediak-Higashi syndrome
- Chronic granulomatous disease
- NADPH oxidase deficiency
- G6PD deficiency
- Hemochromatosis
Which of the following molecules make bacteria more susceptible to phagocytosis?
- C3b
- NADPH
- MPO
- HOCl
- GSSG
Customer reviews
4,7 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
1 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Sublime talk about so many topics,correlating systems, comming from the basics, using only one image, congratulations Dr Raj. Totally recommended and worth to watch over and over.
A most clear, fun lecture on the respiratory burst so far!
wonderful details & very enjoyable teaching way - u really know how to teach pathology thank u
Dr Raj makes everything more simple, it is a good effort you make to teach