Playlist
Show Playlist
Hide Playlist
Perianal and Perirectal Abscess
-
Slides GIP Perianal Perirectal Abscess.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
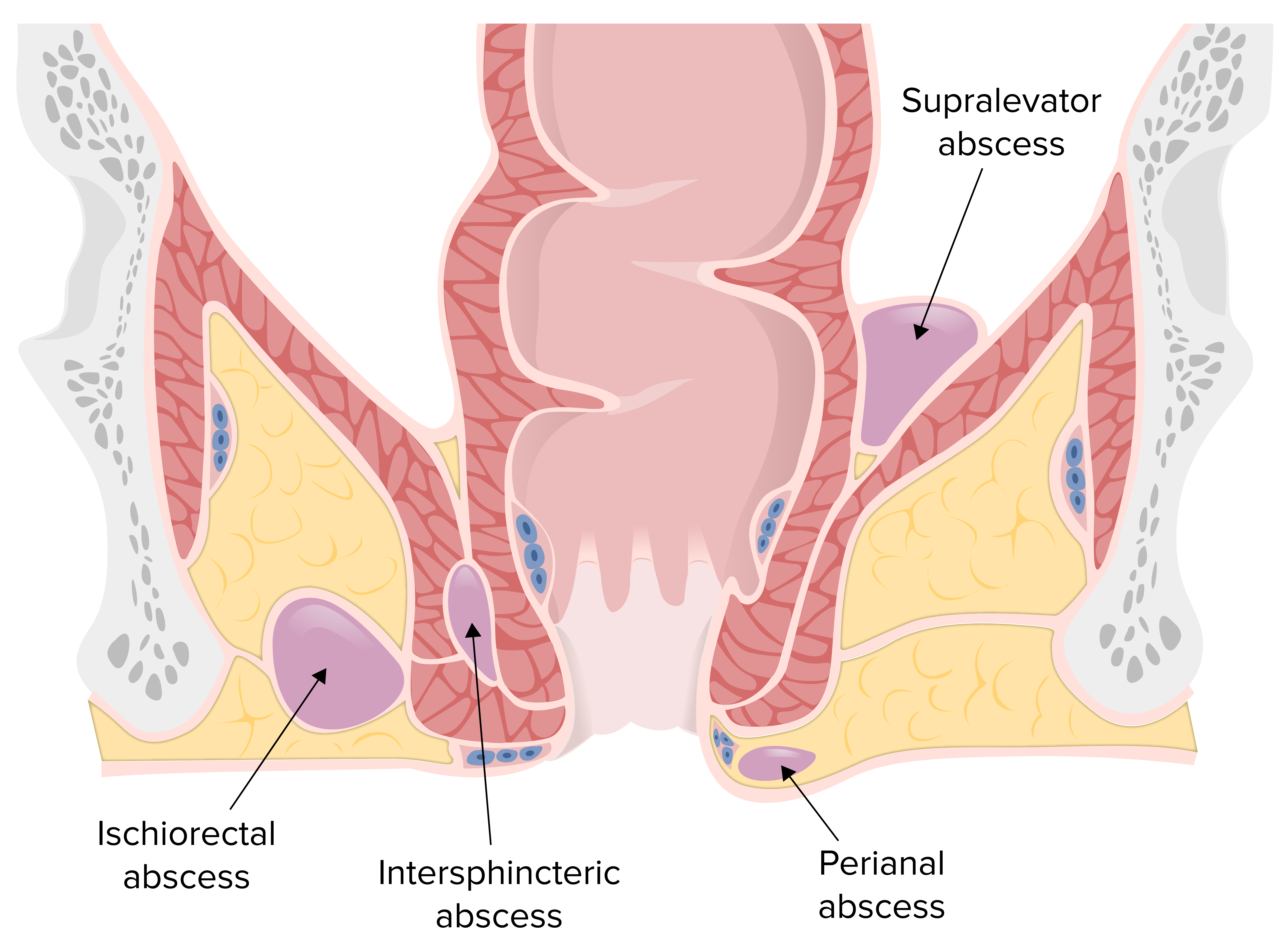
00:01 Welcome. Once again, we have a lovely topic to discuss, perianal and perirectal abscess. 00:09 And as you're already thinking to yourself, that's not going to be fun. 00:13 Yes, if you're a patient with this, it's not fun. 00:16 So, these are collections of pus, local areas of necrosis with an intense neutrophilic infiltrate caused by anal gland obstruction and secondary infection. 00:29 The epidemiology of these overall is that it can pretty much happen throughout one's lifetime. 00:35 Men seem to be more frequently affected than women by a two to one margin. 00:40 30% of these patients have had prior anal rectal abscess. 00:45 So, if you've had it once, it's likely to come back. Immunosuppression is also a risk factor for these. 00:51 The pathophysiology is basically obstruction of the anal glands. There are a number of anal glands. 00:57 We'll talk about these in turn. I don't think you need to memorize them, just be aware of the specific locations and how that may impact your ability to diagnose and/or treat. 01:07 But the anal glands drain into crypts along the dentate/pectinate line. 01:13 So, they are dumping their contents. These are going to be mucus to help lubricate stool at the very last stages of elimination from the colon. 01:22 Those anal glands normally drain if they become obstructed or if there's retrograde infection, then, we will develop perianal, perirectal abscess. 01:33 The gland obstruction can be due to a number of things listed here. So, there's non-specific. 01:40 Meaning, we don't know. That's the vast majority of cases. 01:44 Inflammatory bowel disease and especially Crohn's disease involving the rectum will classically do this. 01:51 Trauma, and trauma not in the sense of an automobile accident but having something inserted forcefully into the rectum. 01:58 Malignancy or extension of an adjacent infection, all of these are reasons for having the glandular components to be obstructed and then, infected. 02:10 Any of the glands that are associated with the rectum or the anus can be involved and have various locations. 02:22 Clearly, whatever microorganism is living in that part of the anus will be able to infect. 02:30 So, it can be an E. Coli or Klebsiella, any normal GI flora. 02:35 So, we're looking at a number of the normal locations for glands. 02:38 And let's talk about when they become infected. 02:42 So, the most common perianal infection abscess is going to be the - is going to be the perianal abscess and it extends and continues into the fat of the buttocks. 02:54 These are going to be the most superficial, most easily incised and drained from an external approach but fortunately, also, the most common so that we can see them and treat them. 03:05 There are perianal abscesses that involve the ischiorectal location. 03:13 So, lateral and posterior to the anus and inferior to the levator ani. 03:17 There are those that involve the inter-sphincter regions between the various muscles involved in the sphincter. 03:28 And then, finally, the space above the levator ani, giving you a super levator abscess. 03:35 Some of these are going to be much more easy to palpate and see. 03:39 Others are going to be clearly deeper such as this one. Clinical presentation. 03:44 So, pain is going to be the primary manifestation, tends to be rather severe, can be dull and achy. 03:51 It's a constant pain and it's clearly exacerbated by the movement of fecal material along the bowel and with straining at stool. 04:00 An external or digital rectal exam will demonstrate swelling, tenderness, and fluctuance and that is going to be probably your best indicator that there is a perirectal abscess. 04:12 Because of the inflammation, because of the pain, patients may variably describe either constipation, kind of an obstruction to movement of stool or if there's a lot of inflammation and that's causing in fact evacuation of the anal canal, then, you may get diarrhea. 04:31 Depending on whether there is actual drainage from the obstruction, you may have purulence in the stool. 04:37 You may have blood in the stool. 04:39 There's occasionally, because of secondary inflammation associated urinary retention. 04:45 And clearly with significant infections, you may have systemic signs. 04:49 So, fever, elevated white count, and things like that. Making your diagnosis. It is primarily a clinical diagnosis. 04:57 You turn your patient over, you do a gentle external examination, and for the vast majority of your perianal abscesses, that's going to be it. 05:06 For those that are deeper, you know, so, those involving for example, the levator, you may need CT or MRI or ultrasound to look for fluctuant accumulations. 05:18 Management, so, management is - let's treat the infection. And surgery. 05:24 So, in most cases, once you have an abscess, antibiotics alone are insufficient to treat and that's an abscess anywhere on the body. You need to incise and drain, an I and D, to remove the vast majority of the necrotic debris and the bacteria and allow healing to proceed. 05:42 So, antibiotics and surgery are going to be your mainstays. And with that, a painful topic comes to a close.
About the Lecture
The lecture Perianal and Perirectal Abscess by Richard Mitchell, MD, PhD is from the course Small and Large Intestines Disorders.
Included Quiz Questions
Which statement about perirectal abscesses is correct?
- They are more common in men than in women.
- Ninety percent of patients have had a prior anorectal abscess.
- They are most common in children.
- They are most common in elderly patients.
- Ten percent of patients have had a prior anorectal abscess.
What is the most common cause of gland obstruction leading to an anorectal abscess?
- No known specific cause
- Inflammatory bowel disease
- Malignancy
- Trauma
- Extension of adjacent infection
What is the primary presenting symptom of an anorectal abscess?
- Severe pain
- Diarrhea
- Constipation
- Urinary retention
- Purulent stool
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |