Playlist
Show Playlist
Hide Playlist
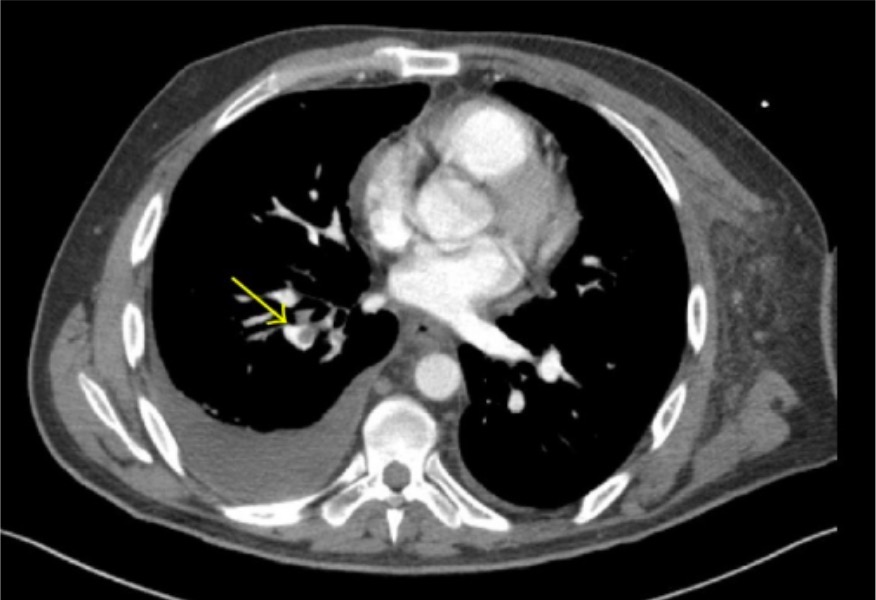
Pulmonary Embolism (PE): Signs & Symptoms
-
Emergency Medicine Bord Pulmonary Embolus.pdf
-
Download Lecture Overview
00:01 Hi! We’re gonna be talking about pulmonary embolus, and how we think about, and evaluate for pulmonary embolus in the emergency department. 00:09 So we’re gonna start up by talking about a case study, a patient case. 00:14 So you’re taking care of a 32-year-old woman, who’s coming into the emergency department with some left-sided chest pain and difficulty breathing. 00:22 She tells you the pain is worse when she takes a deep breath and you start thinking about whether or not this could be a presentation of a pulmonary embolus. 00:30 So when we’re thinking about this patient, what additional questions do you wanna ask the patient, right? So in the emergency department our key goal is for you to take a focused history and perform a focused physical exam to try and get to the bottom-line. 00:45 So thinking about what other questions to ask this individual, you wanna ask her about any other medications that she’s on, you wanna ask about any recent hospitalizations or mobilizations, you wanna ask about any other procedures that she’s had, you wanna ask if the shortness of breath began suddenly or began gradually, you wanna ask if there’s any other alleviating factors, if there’s any other associated symptoms with her shortness of breath. 01:11 And what do you wanna focus on on your physical exam? In this situation, when you’re thinking about pulmonary embolus and shortness of breath, you wanna focus on the cardiac exam as well as the pulmonary exam but you don’t wanna discount the other portions of the physical exam. 01:26 So you wanna make sure that you’re doing a quick focused exam on those few areas. 01:31 So what are our classic presenting signs and symptoms? So what would make you think more likely that this is a pulmonary embolus? Now, I wanna be clear that pulmonary embolus is one of those things in medicine that can present very subtly and differently in different patients. 01:48 I’ve taken care of patients who have had very different and varying presentations for pulmonary embolus. 01:53 I’ve taken care of a patient who had shoulder pain that began very suddenly and that was a presentation for a pulmonary embolus. 02:00 I’ve taken care of patients that who have had flank pain and that was a pulmonary embolus diagnosis in the end. 02:07 So you really wanna make sure that although you’re thinking about these classic presenting signs and symptoms, that you’re also thinking broadly about things. 02:13 That you are also thinking… always thinking about this diagnosis and we’re gonna review some of the subtle things that you can think about along the way. 02:21 But the classic way that your textbook is gonna tell you that patients are gonna present is with pleuritic chest pains. 02:27 So pleuritic chest pain is chest pain that is worse when someone inhales. 02:31 So when your patient takes a breath in, they’re saying that the pain hurts more when they do that. 02:36 Classically, patients will tell you that they feel short of breath. 02:41 That they are feeling like they’re having a hard time catching their breath and different patients describe this sensation in a different way but someone will report some shortness of breath to you. 02:51 Classically, they’ll have swelling in their leg, because where the blood clots come from? Classically, they come from a DVT. 02:59 They come from a deep venous thrombosis. 03:01 Generally, in a leg, although patients can also have DVTs in their arms but historically we think about it or classically we think about it coming from the leg. 03:09 So it’s a clot that comes from your leg that goes up to your lung. 03:12 So unilateral leg swelling, swelling of one of the legs is another classic thing that can be associated with it. 03:18 Palpitations, they may feel like their heart is racing. 03:22 Their heart may in fact actually be going fast. 03:24 They may have this sensation that their heart is going fast. 03:28 And then on the physical exam and on those vital signs, remember that vitals are vital. 03:33 We always wanna make sure we’re looking at them and thinking about all the vital signs in the ED they were looking for hypoxia, so their oxygen saturation will be low and who are possibly tachycardia that their heart rate would be fast. 03:46 So those two vital signs indicate that there may be a pulmonary embolus. 03:51 Now, these are of course nonspecific, right? There’s lots of different things that can cause hypoxia. 03:56 There’s lots of different things that can cause a patient to be tachycardic. 04:00 But when you’re thinking about whether or not someone has a PE, these are the classic things that the vital signs will show.
About the Lecture
The lecture Pulmonary Embolism (PE): Signs & Symptoms by Sharon Bord, MD is from the course Respiratory Emergencies.
Included Quiz Questions
Which of the following statements regarding evaluation of pulmonary embolism is INCORRECT?
- Disregard other organ systems that are not associated with breathing.
- Conduct a focused physical examination on the lungs and heart.
- Ask additional questions regarding recent immobilization.
- Ask for other associated symptoms with shortness of breath.
- Ask for alleviating factors.
Which of the following is NOT a classic presentation of pulmonary embolism?
- Bradycardia
- Pleuritic chest pain
- Palpitations
- Shortness of breath
- Unilateral leg swelling
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |