Playlist
Show Playlist
Hide Playlist
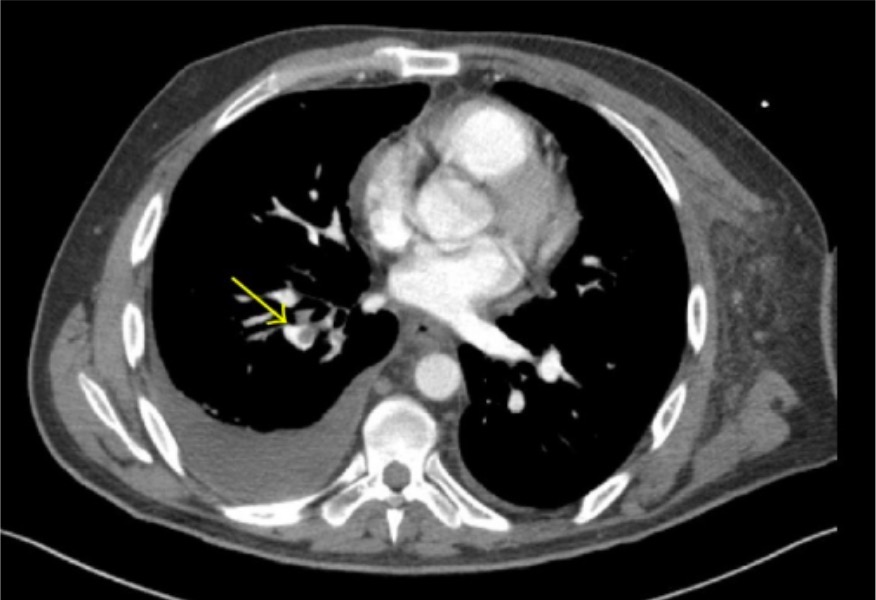
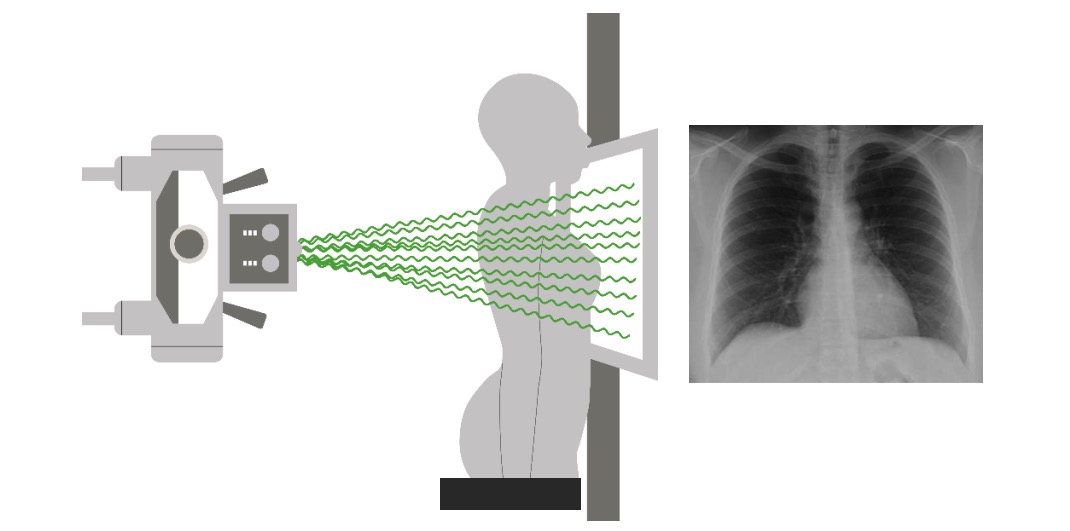
Pulmonary Embolism (PE): Examination
-
Emergency Medicine Bord Pulmonary Embolus.pdf
-
Download Lecture Overview
00:01 And then we want to think about our focus history. 00:03 So in our focus history, we want to think about risk factors, family history, and then any prior history. 00:09 So what are the risk factors? One of the key risk factors is immobilization. 00:14 So how has the patient been hospitalized? Have they been lying in bed because they've had another kind of an injury? Did they recently have surgery? Classically after a surgery or during hospitalization, patients will get DVT prophylaxis, so they'll get either things on their legs that squeeze their legs that prevent a DVT or get injections of Lovenox or low molecular rate heparin in their abdomen. 00:36 So there's things that can be done during those periods of immobility that can prevent DVT, but they are not always 100% effective and people aren't always totally compliant with those treatments. 00:48 The other thing that sometimes people associate in immobilization is very long plane fights. 00:53 So patients who get on a plane, they sit there in their seat for a long period of time, they don't get up to use the bathroom, that technically is a period of immobilization. 01:02 So I always ask about whether or not people have been on long flights. 01:06 This doesn't matter like, did you fly on a short two hour flight, it's more of those kind of longer distance, long haul kind of experiences. 01:13 And I had actually taken care of a patient who, after a very long flight, did in fact developed a pulmonary embolus; so asking about that, an immobilization, are key things to do. 01:26 Also you want to think about estrogen and a state of pregnancy. 01:30 So is the patient on any oral contraceptive agents? Yeah, not all oral contraceptive agents contain estrogen, but a large proportion of them do. 01:39 Also patients when they're in postmenopausal, sometimes will take estrogen replacement therapy, so you want to kind of try and get that information out of someone. 01:48 Patients who are pregnant have a higher estrogenic state. 01:52 In order to maintain the pregnancy the body secretes more estrogen and the placenta does, and in a state of pregnancy, patients will have elevated estrogen levels, so that's another risk factor. 02:04 And then, lastly, malignancy. 02:06 Malignancies can predispose patients to clotting and also you may have some of that immobility that takes place as well, so asking about any history of cancer or any currently active treated cancer can help you make this diagnosis. 02:22 Family history of clotting disorders is also very important to ask about. 02:27 So you wanna ask about, I generally say first degree relative, so mother, father, brothers or sisters that potentially have had any kind of clotting. 02:34 This is something that really can kind of sway me one way or the other about what I'm gonna do for additional diagnostic testing, so keeping that in mind, Is there any family history of clotting? And then for the patient, have they ever had a DVT or pulmonary embolus before? In some of these situations especially in recurrent situations, patients are generally maintained on life-long anticoagulation. 02:59 But, in this situation, sometimes patients are only advised to take these medications for shorter periods of time especially in what we call a provoked PE. 03:09 A provoked DVT can occur in case of prolonged immobilization as in a postoperative period with old immobile patients and patients with stroke. 03:20 And in those situations, they might have the patient only take the anticoagulation medication for a period of time and then they stop it. 03:28 So asking about if the patient has ever had a DVT or pulmonary embolus before can help stir you again to figure out what diagnostic testing to get. 03:38 And on your physical exam, it's very important to remember that the exam findings can be very nonspecific, you might not have anything that kind of jumps out of you on your exam. 03:49 You want to think about tachycardia, is the patient's heart rate fast? Unexplained tachycardia in a patient in the emergency department should always prompt you to be thinking about pulmonary embolus. 03:59 Unexplained tachycardia is one of those things that we're always thinking about and always saying, why is the patient's heart rate fast, especially if you can't find another etiology like a fever or pain, you want to think about PE. 04:13 The lung exam, generally patients will have clear lungs so you'll listen to their lungs you won't hear anything very exciting. 04:21 It's important to remember there have been some studies out there that show that they is an association with COPD, so patients who are being admitted to the hospital and pulmonary embolus, so those patients potentially may have wheezing in their lungs. 04:34 But clear lungs, is one of the most common findings for patients with pulmonary embolus. 04:40 You want to examine their lower extremities, do they have any leg swelling or tenderness? A tenderness in the posterior portion of the calf is what we call Homan's sign, so if you go ahead and squeeze the back portion of the patient's leg and it hurts them, that could be denoted as a positive Homan's sign. 04:57 Now classically, you're looking for swelling in one of the leg versus the other. 05:01 But you can definitely go ahead and think about swelling in both legs could potentially be a presentation of a DVT as well. 05:09 So you want to make sure you are taking note of that. 05:11 Patients may also have chronic leg swelling, so you wanna think about that as well. 05:16 So how do we make the diagnosis? So we've taken out history, we've asked all of those important questions, we figured out if the patient has risk factors, you want to do your physical exam. 05:29 Again, the physical exam may not potentially help you that much here. 05:32 The leg swelling, I would say, would be the one thing that would help you the most, but the patient may not have anything that jumps out to you in terms of physical examination. 05:40 Then we want to think about our diagnostics and our decision roles and this is really the thing that I think helps the most when we're thinking about pulmonary embolus.
About the Lecture
The lecture Pulmonary Embolism (PE): Examination by Sharon Bord, MD is from the course Respiratory Emergencies.
Included Quiz Questions
Which of the following is NOT a risk factor for pulmonary embolism?
- Alcohol intake
- Immobilization
- Estrogen intake
- Malignancy
- Pregnancy
What is the most common auscultation finding in patients with pulmonary embolism?
- Clear breath sounds
- Wheezing
- Rhonchi
- Crackles
- Decreased breath sounds
Patients with pulmonary embolism may also present with a positive Homan’s sign. What is a positive Homan’s sign?
- Tenderness in the posterior calf
- Decreased sensation in the affected leg
- Decreased tendon reflex
- Swelling of the affected leg
- Pallor of the affected leg
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |