Playlist
Show Playlist
Hide Playlist
Paralytic Ileus with Case
-
Slides Gastroenterology 03 Constipation.pdf
-
Reference List Gastroenterology.pdf
-
Download Lecture Overview
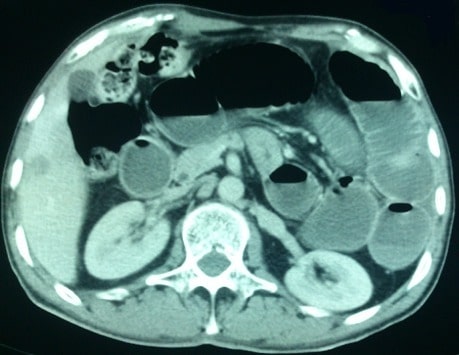
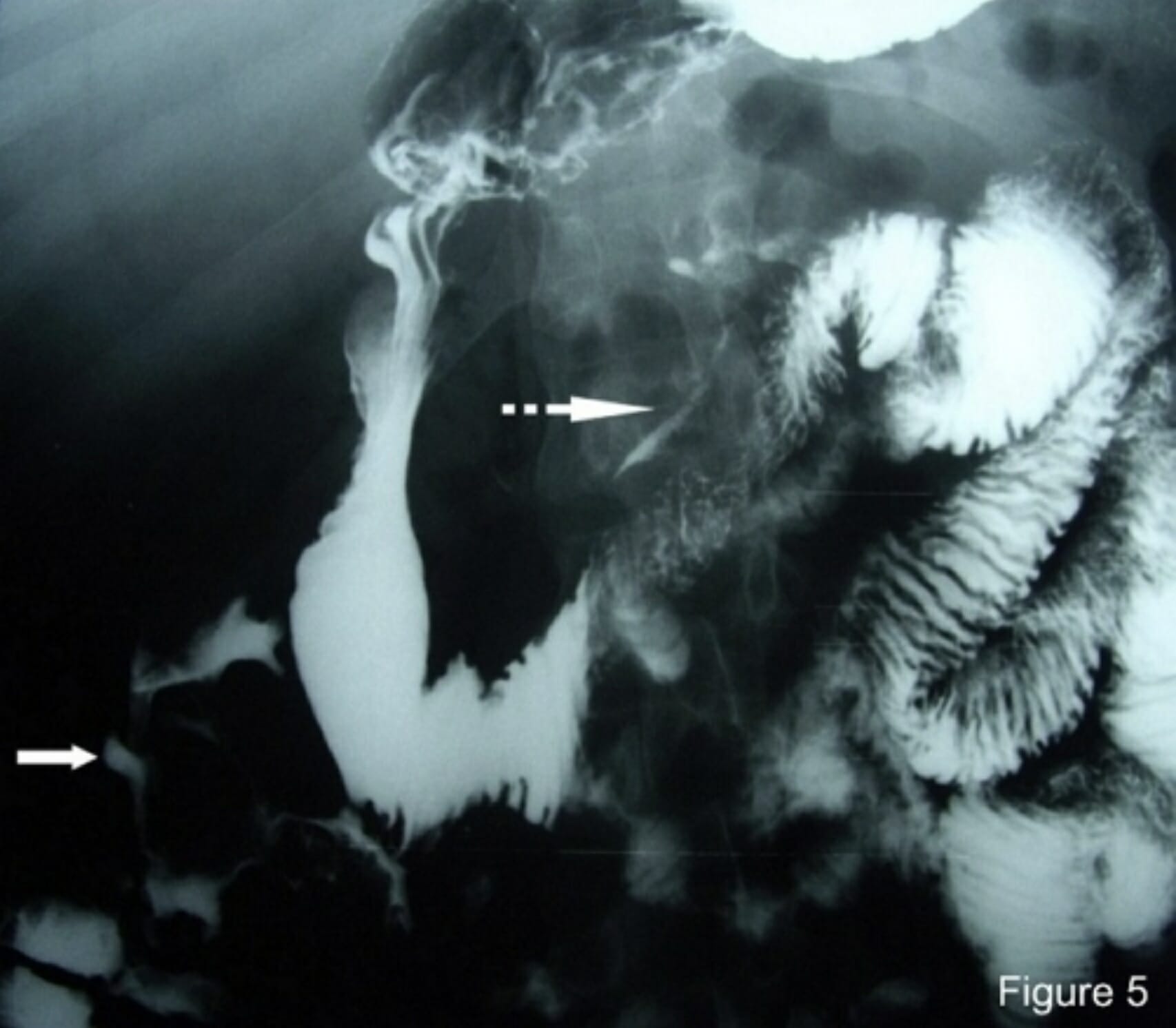
00:00 Let's move to our next case. 00:03 A 78-year old man with Parkinson's disease and dementia is brought to the emergency department form his nursing home for complaints of abdominal pain for the past day. 00:12 He has not passed a bowel movement in a week. 00:15 He takes a hydrocodone-acetaminophen for chronic back pain Vitals are normal. 00:21 On exam, he grimaces to palpation in the lower quadrants of his abdomen, but there is no rebound or guarding. 00:27 A digital rectal exam notes impacted stool in the rectum. 00:32 What is the best next step in management? So let's point out some clues in this case. 00:37 He has a known neurologic disorder that can impact stool transit. 00:41 In addition he is from a nursing home which places him at high risk for constipation. 00:46 He does also have chronic opioid use and on exam, he has fecal impaction. 00:54 So, let's talk about paralytic ileus. 00:58 This is a disruption in the normal motility of the GI tract. 01:03 Some important risk factors include a history of recent surgery, any medications that can cause slow transit such as opioids, or intraabdominal inflammation. 01:16 The clinical features of a paralytic ileus can be very difficult to differentiate from a small bowel obstruction. 01:22 because patients also presents with abdominal distention, pain, nausea and vomiting and constipation. 01:29 On exam, they often will have hypoactive bowel sounds. 01:33 As with SBO, the diagnosis is often made with an abdominal x-ray. 01:38 Here you can see an example of an abdominal x-ray from a patient with an ileus. 01:43 The common features on x-ray are dilated bowel loops and air on the rectum. 01:48 Note here that you do not see those air-fluid levels that we saw with the SBO. 01:53 So, that brings us to this important question: How do you tell the difference between a paralytic ileus and an SBO since they have so many common features? There are several things that we can use to distinguish between the two. 02:08 With an SBO, the bowel sounds on exam will often be hyperactive or completely absent. 02:16 They may also have peritoneal signs on exam. 02:20 And on imaging, on x-ray you will see dilated bowel loops and air-fluid levels. 02:28 On the other hand in a paralytic ileus, you often have hypoactive bowel sounds but they may also be absent. 02:35 It is very uncommon to have peritoneal signs with an ileus and on imaging you will see those dilated bowel loops but you will not see air-fluid levels and because patients are still able to pass gas throughout the colon, they will have air in the rectum. 02:51 So the treatment of constipation depends on several different factors. 02:56 First, we can recommend lifestyle and dietary changes including increasing fiber intake and physical activity. 03:05 Pharmacologically, we can also offer fiber supplements, osmotic laxatives or stimulants. 03:12 In very severe cases such as with fecal impaction when stool becomes stuck or impacted in the rectum, you may need to manually disimpact those patients, or provide an enema for relief. 03:27 So that brings us to the common medications we use for treating constipation. 03:31 We'll break it down by category. 03:33 The first category are fiber supplements, examples include psyllium or methylcellulose. 03:39 and they work by increasing dietary fiber intake to bulk up the stool and allow it to pass easily. 03:47 The next category is osmotic laxatives. 03:50 These are things like lactulose, sorbitol, polyethylene glycol. 03:55 In principle, these are all poorly absorbed or non-absorbed sugars that then draw water into the colon via osmotic pressure and allow for easier passage of stool. 04:06 Our next category are stimulant laxatives, so things like senna or bisacodyl and they work by stimulating the intestinal motor activity to help push stool along. 04:20 Our last category is prosecretory agents. 04:23 Things like linaclotide, or lubiprostone. 04:26 These are medications often used in the treatment of irritable bowel syndrome and they work by increasing the natural secretions of the colon. 04:34 So now that we've reviewed that, let's return to our case. 04:38 Our 78-year old man with Parkinson's disease - so a known neurologic disorder that can impact stool transit plus he's from a nursing home and he has chronic opioid use. 04:49 So all major risk factors for constipation. 04:52 He has fecal impaction on exam, so the best next step in management would be to perform a fecal disimpaction or provide an enema. 05:00 Thank you very much for your attention.
About the Lecture
The lecture Paralytic Ileus with Case by Kelley Chuang, MD is from the course Approach to Patients with GI Symptoms.
Included Quiz Questions
Which of the following is more characteristic of small bowel obstruction than paralytic ileus?
- Air/fluid levels on X-ray
- Hypoactive bowel sounds
- Air in rectum
- Jaundice
- Diarrhea
Which of the following is the best next step in the management of severe constipation with fecal impaction in the rectum?
- Manual disimpaction
- Increased dietary fiber
- Increased physical activity
- Osmotic laxatives
- Stimulants
Which of the following is a possible risk factor for paralytic ileus?
- Opioid use
- Hernia
- Volvulus
- Cancer
- Intussusception
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |