Playlist
Show Playlist
Hide Playlist
Overview of Ischemic and Hemorrhagic Stroke
-
Slides Stroke and intracranial hemorrhage.pdf
-
Download Lecture Overview
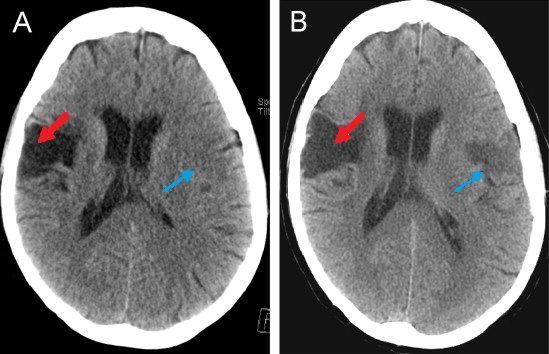
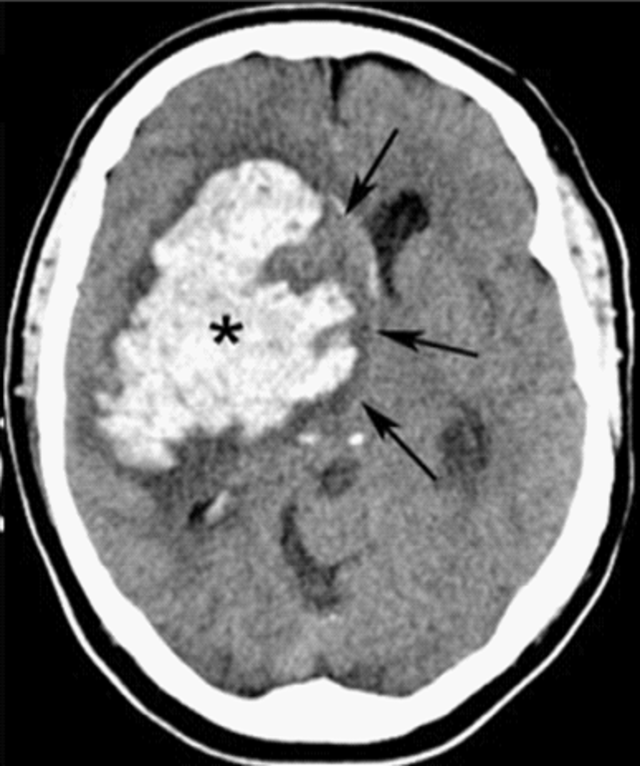
00:01 Let's now do a quick summary of ischemic stroke and hemorrhagic stroke. 00:06 We're going to hit the highlights for the causes, the diagnostic workup and treatment for each of these two major types of stroke. 00:13 In subsequent lectures, we'll dive deep in to each of these. 00:16 Here, we're going to go some tables that hit the highlights. 00:20 When I think about ischemic stroke, I think of five major causes. 00:24 We can see ischemia or a blood clot reduction in blood flow to a part of the brain from thromboembolism, intracranial atherosclerosis, lacunar infarcts, watershed ischemia, and embolism or cardio embolism, and those five causes are what we evaluate in patients or the clinical vignettes when we're evaluating for an ischemic stroke. 00:48 As we look at those, the different types of stroke lead to different symptom presentations and size of lesions on CT scans and MRI scans. 00:59 Our embolic strokes, cardioembolic strokes and thromboembolic strokes result from a blood clot either in the heart or the carotid arteries that dislodges and travels up to the brain. 01:11 Those are typically larger clots and they lodge in larger blood vessels. 01:16 We often see larger territory strokes on imaging, larger territory of stroke in terms of the patient's symptoms and exam findings, and this large territory ischemic lesions tip us off to be worried about an embolic phenomenon, and you can see that here in this large territory. 01:33 Atherosclerotic disease are hardening of the blood vessels. 01:37 Plaques, atherosclerotic plaques or atheroma, that form on the blood vessels, can form anywhere in the cerebrovascular system, out in the distal blood vessels, or the medium sized blood vessels or even the proximal major blood vessels in the brain. 01:52 So we can see strokes of any sizes that we tend to see moderate territory strokes in the anteroposterior circulation, anywhere in the brain, and so atherosclerosis is a common risk factor we're evaluating an etiology we would be considering. 02:06 Lacunar strokes are small vessel strokes. 02:10 A lacuna is an island, and this is an island of stroke deep in the brain, often in the subcortical gray matter or sometimes white matter tracks. 02:19 These small strokes form on small blood vessels, the perforators. 02:24 We think about the thalamus stripe perforators and other small vessels in and around the brain that can lead to lacunar strokes. 02:31 And long standing hypertension is an important risk factor that we'll talk about. 02:35 And then the last type of stroke is the watershed stroke. 02:37 This doesn't come from a blood clot, it's the one ischemic stroke that's not from a clot in the blood vessel, but from reduced blood flow. 02:45 And we see this in areas where vascular blood beds are collateralizing, so it's at those collateral watershed territories in between major vessels that are supplying the brain. 02:56 When we think about the diagnostic workup, we're working up each of those major causes. 03:02 We'll do carotid ultrasounds to look at the blood vessels going to the brain or transcranial doppler to look at the blood vessels within the brain. 03:11 Transthoracic echo cardiography is done to evaluate the heart and look for a patent Foramen Ovale, as well as blood testing like a thyroid study and EKGs to look for paroxysmal atrial fibrillation. 03:22 Stroke risk factor modification is important and we evaluate cholesterol. 03:27 low density and high density lipoprotein, as well as hemoglobin A1c which are important risk factors for the development of stroke. 03:34 And rehab is critically important for recovery for any patient who's had a stroke and that includes physical, occupational, speech therapy and aggressive rehab. 03:43 So those are the types of diagnostic test and management that we'll do to help patients evaluate the cause of their strokes and begin their recovery process. 03:52 Ultimately, treatment is critical and we want to prevent the next stroke. 03:56 Primary prevention of stroke is to prevent the stroke before it's occurred, and secondary prevention is to prevent the next stroke once one has. 04:04 We think about antiplatelet agents like aspirin, Plavix, Aggrenox. 04:08 We'll learn about each of those. 04:10 We also think about anticoagulation, Coumadin, Lovenox, and some of the direct oral anticoagulant medications or antithrombotic medications. 04:20 What about the a hemorrhagic stroke? What's the sort of summary, the things we should consider when we're thinking about hemorrhagic stroke? Well, again, just as there's five causes of an ischemic stroke there are five causes that I want you to think about for hemorrhagic stroke. 04:35 Hypertensive hemorrhage is the most common cause of hemorrhagic stroke. 04:40 Hemorrhagic transformation of ischemic stroke is something we'll talk about in greater detail in understanding when that may occur, but hemorrhage can happen after an ischemic stroke. 04:50 Certain brain tumors, brain metastases, as well as primary gliomas can hemorrhage. 04:54 Vascular malformations in the brain including arteriovenous malformations and aneurysms can burst and bleed. 05:02 And then amyloid angiopathy is a degenerative condition. 05:06 Patients can develop amyloid dementia and we also can see leaking of the blood vessels in that condition, and a risk of lobar hemorrhage. 05:14 Again, when we think about the types of hemorrhagic stroke, there are two basic types of hemorrhagic stroke, there's intracerebral or intraparenchymal hemorrhage and subarachnoid hemorrhage. 05:26 The hypertensive hemorrhage, the hemorrhagic transformation of a stroke, the tumors, and the amyloid angiopathy, those four causes all present with intraparenchymal or intracerebral hemorrhage. 05:38 Aneurysms, are the etiology that really present with subarachnoid hemorrhage, those two causes of intracerebral, excuse me, those two causes of hemorrhagic stroke. 05:49 What do we do from a diagnostic standpoint for hemorrhagic stroke is quite different from that for the ischemic stroke. 05:55 With ischemic strokes we're looking why the clot may be there. 05:58 With hemorrhage, it's happened and we're making sure it doesn't get worse. 06:02 Patients undergo a non-contrast head CT somewhere between 6 and 24 hours to make sure the bleeding isn't expanding and the patient doesn't require further intervention. 06:12 MRI may be considered if we're looking for a tumor. 06:15 Vascular imaging or angiography, some type of non-invasive or invasive angiography, can look for a vascular lesion, and we look to manage blood pressure to reduce the risk of further expansion of that hemorrhage. 06:29 And then treatments are also very different. 06:31 So when we juxtapose the treatment for ischemic stroke and hemorrhagic stroke, with ischemic stroke we're adding antiplatelets and anticoagulants; with hemorrhagic stroke we're taking those away. 06:40 There's nothing we can do to stop that hemorrhage that's occurred, but we want to prevent its expansion. 06:46 We hold the anti-thrombotic, we stop anticoagulants. 06:50 We don't use those for prophylaxis for patients who are in the hospital and we would use things like sequential compression devices as you see here. 06:57 And some patients may develop seizures, so we're managing those potential side effects particularly in seizures, excuse me, in hemorrhage, that involve the outer cortical surface in gray matter. 07:07 So this important summary gives us an idea of the things we need to be thinking about, and we'll dive in to greater detail into each of these details.
About the Lecture
The lecture Overview of Ischemic and Hemorrhagic Stroke by Roy Strowd, MD is from the course Stroke and Intracranial Hemorrhage.
Included Quiz Questions
What is the cause of a small vessel stroke that affects the thalamus?
- Lacunar infarct
- Watershed stroke
- Thromboembolic stroke
- Amyloid angiopathy
- Hemorrhagic transformation
What is the most common cause of a hemorrhagic stroke?
- Hypertension
- Diabetes
- Hyperlipidemia
- Metastatic brain lesions
- Amyloid angiopathy
What is the overall most common type of stroke?
- Ischemic stroke
- Lacunar stroke
- Hemorrhagic stroke due to a ruptured aneurysm
- Subarachnoid hemorrhage
- Embolic stroke
What finding must be considered while performing a transthoracic echocardiogram (TTE) for ischemic stroke workup?
- Patent foramen ovale (PFO)
- Decreased ejection fraction
- Valvular heart disease
- Pericarditis
- Atherosclerosis
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |