Playlist
Show Playlist
Hide Playlist
Other Dementia: Frontotemporal Lobar Dementia
-
Slides Other Dementias.pdf
-
Download Lecture Overview
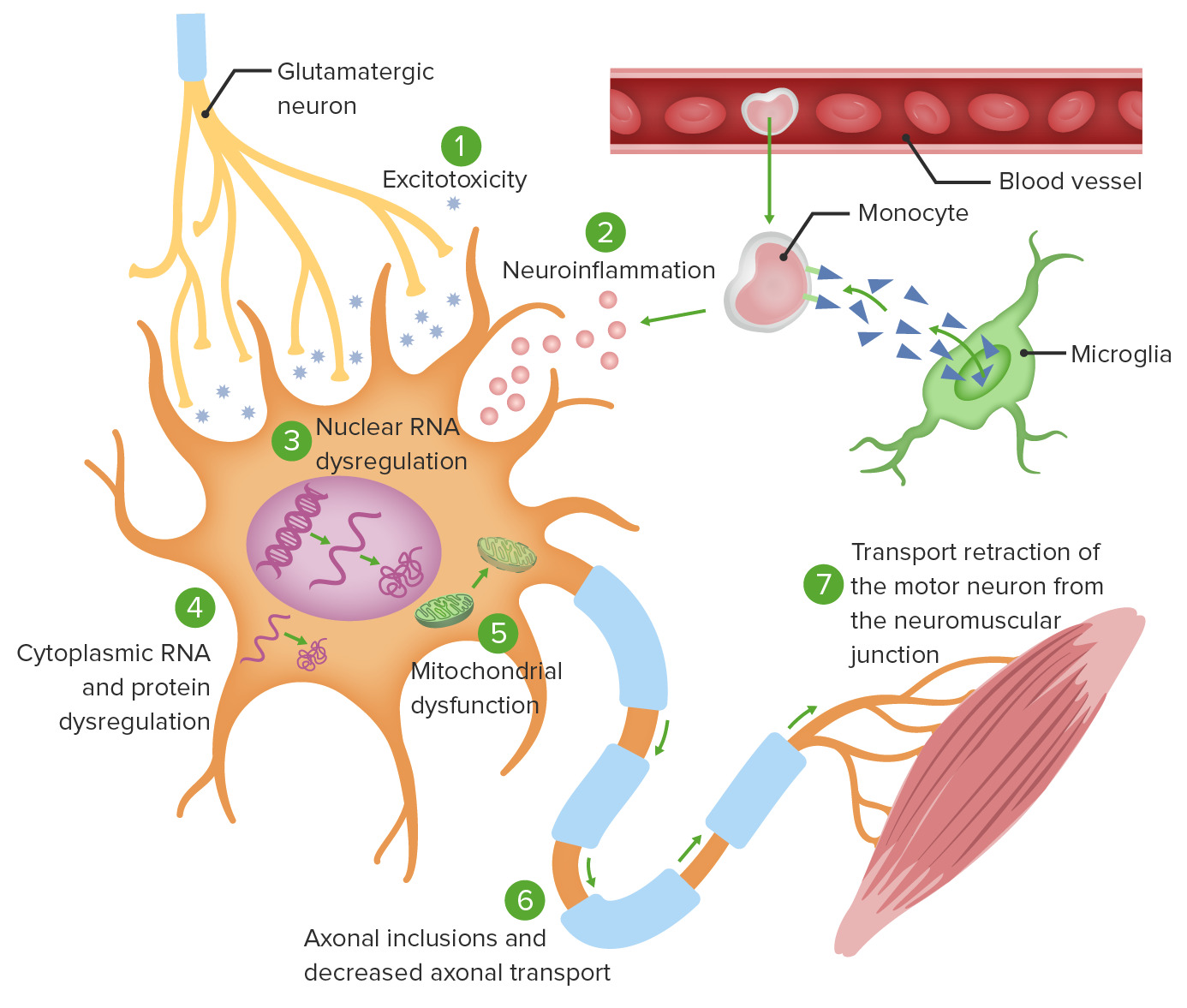
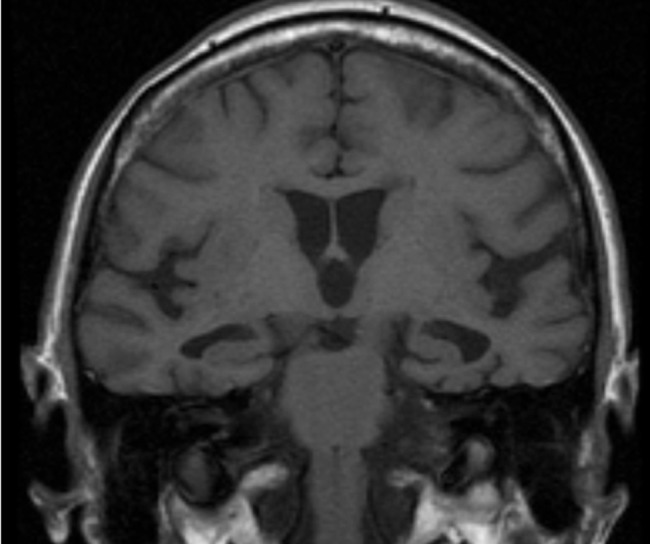
00:01 Now let's talk about frontotemporal dementia. This is one of the uncommon causes of dementia but with a unique presentation that should warrant understanding and ability to evaluate these patients. This term is really used to describe several different types of dementia. That can affect the frontal lobe and the temporal lobe variably. 00:20 In terms of epidemiology, this most affects people ages 50-60 so it can be younger onset in Alzheimer's disease but it can also manifest earlier and later in life with both a rapid onset form and a late onset form. The pathology that's going on in the patient's brain is damaged to neurons shrinking, atrophy of the frontal and temporal lobes as a result of progressive deposition of tau. It is assumed that there is a stronger genetic component with frontotemporal dementia than with some of the other types of dementias and specifically Alzheimer's disease. So when we think about frontotemporal dementia, I think it's helpful to break this into 3 categories. There is a frontal lobe variant where the primary problem is in the frontal lobe, really sparing temporal lobe dysfunction called primary progressive aphasia or aphasia frontal lobe dysfunction predominance. There is a semantic dementia. This is the temporal variant where there is prominent temporal lobe atrophy really with a paucity of frontal lobe dysfunction and those patients have prominent under difficulty with understanding things, a semantic dementia. And then the last is the behavioral variant which is a higher cognitive frontal dysfunction in this behavioral variant at FTD is the third variant of FTD. Let's walk through each of these subtypes of FTD. The first is primary progressive aphasia. This is clinically and pathologically a heterogenous group of degenerative disorders. Patients develop symptoms that slowly progress over time. 01:58 Patients with PPA, primary progressive aphasia, present with progressive language difficulty and relative sparing of memory and other cognitive dysfunctions. So these patients just stop talking. Slowly over time often over the course of months or years, patients have progressive reduction in the amount of speech and fluency of speech ultimately becoming mute with a relative paucity of other cognitive dysfunction occurring. 02:25 Now let's talk about semantic dementia. 02:27 This is the temporal lobe variant of frontotemporal dementia characterized by progressive cognitive and language deficits and the inability to match words with the images or their meaning. You know what things are but can't match the word to the right meaning. And then lastly, the behavioral variant. This is the most common subtype of FTD characterized by progressive changes in personality and behavior, disinhibition, agitation which is present early and prominent early in the course of this disease. Now let's talk about the spectrum of FTD. It's really a spectrum of a number of disorders that's occurring from the same underlying brain pathology. There are patients with prominent behavioral symptoms, language symptoms, or movement symptoms. And you can see the number of diagnoses where FTD is at play; behavioral variant FTD, semantic dementia, primary progressive aphasia, there's an ALS subtype that's associated with FTD, corticobasal syndrome, progressive supranuclear palsy. 03:32 Each of those clinical diagnosis has, as the underlying neurodevelopmental problem, frontotemporal degeneration. And this results from dysfunction of a number of different genes and molecular phenotypes. The FTD tau contributes to some of these diagnoses as well as FTD TDP which is present in ALS with FTD and other variants. When we think about FTD, we're talking about a dementia affecting the frontal lobe. So how do we test the frontal lobe on exam? How do we look at the function of the frontal lobe, memory in the frontal lobe, and evaluate for dysfunction in those patients. 04:09 Well, the frontal lobe is the motor lobe. So the first thing we want to do is test for motor cortical strength. What is the patient's strength exam? We also look at premotor function. This is the speed and dexterity or flow of movements, the ability to pantomime movements, abnormalities in the ability to pantomime is idiomotor apraxia which is a frontal lobe task. We want to look at oculomotor function, the frontal lobe and specifically frontal eye fields controls goal-directed eye movements. 04:40 We test the voluntary pursuit and saccadic eye movements or goal-directed eye movements looking for slowness or jerking of movements that indicate dysfunction of the frontal eye fields and this is suggestive of some type of frontal dysfunction. 04:55 We also want to test the dorsolateral prefrontal cortex. And here I like the Luria test. 05:01 This is a 3-step exam where we're demonstrating a series of movements to the patient and asking them to perform these back. We use 3 movements; a fist, the edge of the hand, and the palm of the hand and ask the patients to repeat this and that dorsolateral prefrontal cortex is important in understanding that series of events and performing them in order. So problems with the Luria test indicate pathology within the dorsolateral prefrontal cortex. We can look at orbitofrontal dysfunction testing for anosmia or a Go/No-Go testing the ability of the patient to understand a series of commands and go or not go to those. We can look at cingulate function. 05:46 Lesions to the cingulate can result in apathy and abulia particularly bilateral cingulate lesions. And then we can look for a number of frontal release reflexes like grasp, sucking, pulmomental, and the glabellar tap. These are things that you might see in a neonate. They go away over time as the brain myelinates and then can reoccur in patients who develop frontal dysfunction, degeneration, or abnormalities of some kind.
About the Lecture
The lecture Other Dementia: Frontotemporal Lobar Dementia by Roy Strowd, MD is from the course Other Dementias.
Included Quiz Questions
Which anatomic regions of the brain are most commonly affected in frontotemporal dementia?
- Frontal and temporal
- Occipital and temporal
- Frontal and parietal
- Brainstem and inferior temporal
- Corpus callosum and substantia nigra
Which of the following is not a subtype of frontotemporal dementia?
- Occipital (visual) variant
- Frontal lobe variant (primary progressive aphasia)
- Temporal lobe variant (semantic dementia)
- Behavioral variant
Which of the following is the predominant symptom in primary progressive aphasia?
- Reduction in the amount of speech and fluency of speech
- Progressive motor decline and ataxia
- Inappropriate emotional responses
- Inability to match certain words with their meaning
Which of the following is the predominant symptom in semantic dementia?
- Inability to match certain words with their meaning
- Reduction in the amount of speech and fluency of speech
- Progressive decline in visual acuity
- Inability to recognize familiar faces
Which of the following is the predominant symptom in behavioral dementia?
- Progressive changes in personality and behavior, disinhibition, and agitation
- Reduction in the amount of speech and fluency of speech
- Inability to match certain words with their meaning
- Hypersexuality and hyperorality
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |