Playlist
Show Playlist
Hide Playlist
Pain Management: Safe Prescribing of Opioids
-
Slides Pain ChronicCare.pdf
-
Download Lecture Overview
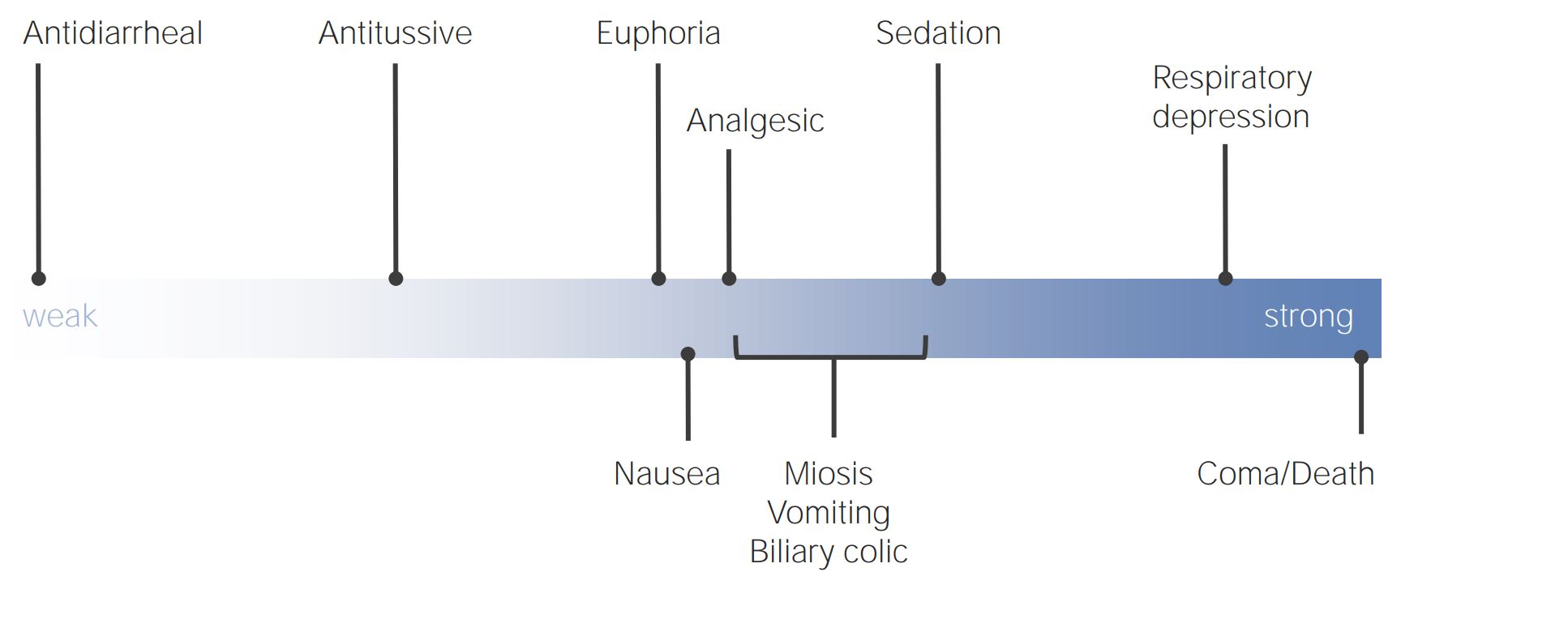
00:01 So, overall, we know that acetaminophen seems safer than NSAIDs for all those reasons. 00:07 That's why it's recommended by over 40 societies as initial management for pain. 00:12 But what about tramadol? Tramadol is a partial opioid receptor agonist. 00:17 It doesn't have the abuse potential we consider for other types of opioids. 00:22 So, maybe it could be a good middle-of-the-road agent and save patients from taking NSAIDs and the potential risk to stomach, kidney and even heart that are associated with NSAID use. 00:34 Well, this is a trial looking at diclofenac versus tramadol. 00:39 Tramadol was up to it with a pretty high dose. 00:41 And they found – this was a smaller study, 97 patients. 00:44 But, really – there really wasn't a difference between the two diclofenac versus tramadol. 00:50 There wasn’t a difference for pain, stiffness or function. 00:54 The patients thought that they are about the same in terms of the efficacy. 00:59 And the risk of overall adverse events was the same, but there was an episode of GI bleeding in the diclofenac group. 01:05 Nonetheless, this makes me think that tramadol is not superior certainly, and yet it is an opioid receptor agonist, and so maybe it would be better just to keep patients on NSAIDs and try to mitigate the risk of GI bleeding, with a drug like a proton pump inhibitor. 01:22 But tramadol doesn’t appear to be the answer. 01:25 It’s only mildly effective for patients with musculoskeletal pain. 01:31 What about other opioids? So, this is a systematic review that looked at 20 randomized controls of opioids for low back pain. 01:40 Again, that's the most common type of pain in the United States. 01:44 The short-term pain reduction versus a placebo, very mild, really kind of similar to what you saw back when we went over the slide with acetaminophen and NSAIDs and muscle relaxants. 01:56 Opioids weren’t stronger in reducing pain. 01:59 And, overall, the researchers judged that that barely met or did not meet criteria for a clinically important pain relief. 02:10 Generally, you want at least 1 point to 2 points on a scale of – on a 10-point scale, improvement in order to judge that to be clinically effective, something that patients actually feel is better. 02:22 And even using over 200 mg daily of morphine equivalents failed to achieve that. 02:32 Finally, in the study of opioids, the drug didn't – just not work that well. 02:39 It wasn’t very well tolerated either. 02:41 So, there was a high discontinuation rate. 02:44 In half of the trials, exceeded 50% due to adverse events associated with opioids. 02:50 And we know that opioids, besides opening the door for misuse, are associated with high rates of nausea, vomiting, and universally they promote constipation, which you have to treat frequently with more drugs. 03:02 So, really not a great option. 03:04 Currently, the CDC says that we shouldn't need opioids for more than three days, maximum of seven days of treatment for acute pain episodes, and to avoid them in chronic pain because, as you can see from this large systematic review, the evidence really isn't there to support their use in those patients. 03:25 How do we curb opioid use? First of all, it’s good stewardship and it's promoting those safer options, acetaminophen, even NSAIDs, because it doesn't seem to be much of a difference for most chronic pain states. 03:40 And at the same time, we want to emphasize that the – if opioids are used, they should be taken for a limited time only. 03:48 And that’s something we really have to hold the line on. 03:51 Final note is, there is an interaction between pain and mental illness. 03:56 So, we know that patients who are depressed and anxious, they report increased pain and severity. 04:03 So, they tend to feel pain more severely. 04:07 And so, that's one thing. 04:08 But it also plays out in terms of important functional outcomes, like disability from work. 04:15 So, this is looking – this study looked at the number of claims of days out due to illness in the past three months among different patient groups. 04:25 Those with pain only, still a lot of days out from work. 04:28 So, if you take 90 days, 18 of them were missed for work. 04:32 Add anxiety to pain, now 32 days missed from work. 04:35 Add depression to pain, 38 days missed from work. 04:38 And in patients with all three disorders, they were missing essentially half of their previous 90 days at work due to illness. 04:48 So, it's not just about feeling better, it’s not just about reducing a 10-point scale from an 8 to a 6, it’s about serious consequences such as work. 04:58 So, therefore, do consider that and try to treat your pain patients completely. 05:04 And consider those mood disorders because treating the depression or anxiety should improve pain as well. 05:11 Thanks. 05:12 And hopefully, that was helpful.
About the Lecture
The lecture Pain Management: Safe Prescribing of Opioids by Charles Vega, MD is from the course Chronic Care.
Included Quiz Questions
According to the CDC, what is the maximum recommended days for opioid use in acute pain?
- 7
- 14
- Until pain subsides
- 1 month
- 3 weeks
Which of the following is a weaker opioid?
- Tramadol
- Oxycodone
- Hydrocodone
- Pethidine
- Methadone
According to the lecture, which of the following groups of patients miss the highest number of days from work due to pain?
- Those with pain, anxiety and depression
- Those with pain and anxiety
- Those with pain and depression
- Those with pain only
Which of the following is an advantage of diclofenac over tramadol?
- Lower risk of dependence
- Lower risk of gastrointestinal bleeding
- Lower risk of kidney dysfunction
- Lower risk of coronary events
- Higher rate of pain control
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |