Playlist
Show Playlist
Hide Playlist
Normal Hemostasis Clotting Factors
-
Slides NormalHemostasis.pdf
-
Download Lecture Overview
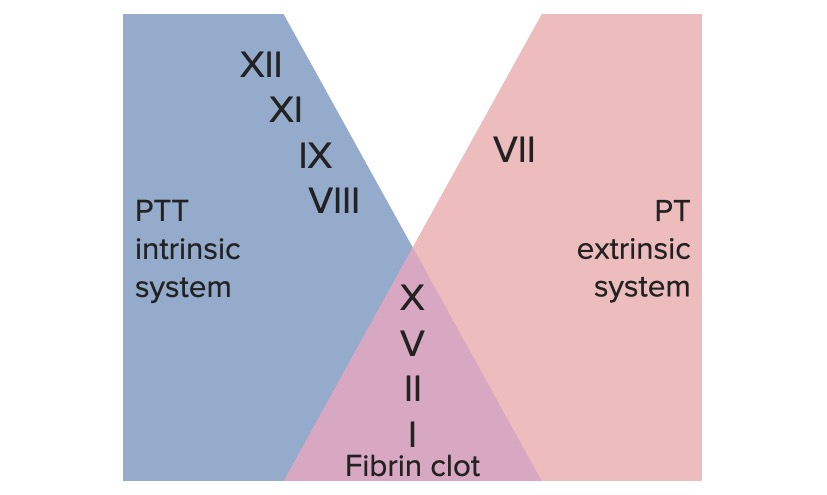
00:01 Now what about the clotting factors? Most of them are produced in the liver. 00:05 What are they again? Ah, I’ll give you II, VII, IX, and X, and protein C and S but the clotting factors II, VII, IX, and X. 00:13 They're dependent on whom? Vitamin K. Vitamin K epoxide is the naturally occurring reduced or inactive form of vitamin K. 00:21 It is converted to its active reduced form, vitamin K hydroquinone, by vitamin K epoxide reductase or short VKOR Vitamin K hydroquinone is a necessary cofactor in the carboxylation of specific glutamate residues within the vitamin K-dependent proteins – factors II, VII, IX, and X, and protein C and S – a process which is necessary to activate them. 00:48 The carboxylation reaction is catalyzed by gamma-glutamyl carboxylase. 00:53 Vitamin K hydroquinone is oxidized to the epoxide form during the carboxylation reaction, and recycled back to its hydroquinone form by VKOR. 01:04 Warfarin inhibits VKOR so vitamin K cannot be recycled from its oxidized form to its reduced form, and the vitamin K-dependent proteins therefore cannot be activated. 01:17 Now the one particular factor that will not be produced in the liver is factor VIII. 01:24 Close your eyes, tell me about factor VIII again? Factor VIII is it part of intrinsic or extrinsic? You got this. It’s part of intrinsic, isn't it? Intrinsic begin with which factor? Factor XII. 01:42 What is the other name for factor XII? Hageman factor. We went from XII we went to XI, and we went to IX and we went to VIII. 01:51 We spent time with factor VIII and I told you factor VIII require what for stabilization? Ah, there it is, von Willebrand Factor. 02:00 Who’s the patient? Who's deficient of von Willebrand Factor? A young lady and she had excessive bleeding during menses, right, why? Because she didn’t have the von Willebrand Factor to properly adhere to glycoprotein 1b nor did she have the von Williband factor to destabilize Factor VIII, now be careful, may I ask you a question? You all should know that when your Factor VIII deficient, what is the name of that disease? I'm sorry what was it? What if this patient comes in with severe bleeding in the joints and such, doesn’t have to be a female, correct? This could be a young child. This is called hemophilia. Which one? There’s two that you're responsible for. 02:44 One is called hemophilia A, the other one is called hemophilia B. 02:48 Well do this, A comes before B, VIII comes before IX, therefore hemophilia A is factor VIII defect, hemophilia B is factor IX defect, okay? At this point, let’s focus on factor VIII and know that it requires von Willebrand Factor for stabilization. 03:10 So the vitamin K dependent clotting factors are II, VII, IX, and X. 03:16 Remind me again, which one are we missing? Protein C and S. Why are they missing in this statement? Because these are the only the clotting factors that we’re discussing at this point in time. 03:28 Remind me again what the drug that will then work upon this particular mechanism? Warfarin. 03:34 Let’s talk about anticoagulants, alright. Anticoagulants. So now that we've form a clot let’s break it down. 03:45 Is it called, the process called fibrinolysis, isn't it? Why do we call it fibrinolysis? Because in order for you to have a stable clot, a stable clot, it was fibrinogen or was it fibrin? Fibrin. 03:58 So now let’s break it down. Who helps in breaking this down? Who initiates or who cleaves your plasminogen? Remember, plasmin is “the enzyme” that will be responsible for breaking down your fibrin, is that understood? Factor XII will help you do this. 04:18 Next, the plasmin will then break this down, now what do you call when you have excessive fibrin breakdown, what's the name of that particular test? Oh, these are called D-dimers, aren’t they? So any condition in which you find excessive breaking down of thrombi is obviously going to give you an elevated level of D-dimers. 04:39 So, so far I've given you three tests. PT, for the extrinsic system, the PTT is to measure which branch of the coagulation cascade the intrinsic, good, the time there is 25-40 seconds. 04:55 And here’s the third test that I'm giving you known as the D-dimer which represents what? Breaking down of your thrombi. 05:02 So what about this plasmin and such? What's important about this? Well, we talked about how factor XII does it naturally. 05:11 It’s called natural plasminogen activator. Fascinating? Because aren’t there some drugs that you should know in which your analogs, the TPA? Sure! What's the suffix that you’re going to be looking for? ASE. Tenecteplase, streptokinase, alteplase -- ASE. 05:30 These are naturally acting tissue plasminogen activators or analogs that behave like the natural fibrinolytic agent. 05:39 And finally under this discussion of anticoagulant, here my vitamin K dependent factors that are anticoagulants and which one are these? Protein C and S, and there we have it, it summarizes ultimately that discussion or the discussion we've had throughout the entire time I've been telling you that we have six vitamin K dependent factors. 06:02 Now, something else that I need to bring to your attention. 06:05 If a patient comes to you says, 'Doc, I seem to have a little bit of pain in my leg down by the calf." If they're giving you textbook type of presentation upon dorsiflexion of the foot, do that for me, dorsiflexion of the foot, oh, there's pain in the calf region. 06:25 The history goes on to say that she's a lady who is pregnant perhaps or maybe she's obese and maybe she's in a job in which she's not moving around much or maybe she's on a transatlantic or transpacific type of flight. 06:41 In other words, she's the perfect candidate of maybe developing a DVT, correct? When we have a DVT is the Warfarin, is that the first drug that you're going to give, warfarin? Of course not, it’s going to be heparin. Heparin works within seconds. 06:57 Heparin works via antithrombin III. We’ll talk about that and then you must give heparin as a bridge therapy in a hospital setting via parenteral either IV or subcutaneous before you start giving warfarin. 07:15 And the reason that becomes really important, because proteins C and S has a half life that is so incredibly short. 07:25 I emphasize short, why? If proteins C and S disappear first and you're giving warfarin, what are the only vitamin K dependent factors that are circulating in that patient’s body? II, VII, IX, and X. You might have micro thrombi taking place up and down the body if you didn’t get that, repeat what I just said, please.
About the Lecture
The lecture Normal Hemostasis Clotting Factors by Carlo Raj, MD is from the course Hemostasis: Basic Principles with Carlo Raj.
Included Quiz Questions
Which of the following clotting factors is NOT produced by hepatocytes?
- VIII
- II
- IX
- X
- VII
Which of the following coagulation factors is deficient in hemophilia B?
- IX
- XIII
- VII
- VIII
- X
What is the main mechanism of action of heparin?
- Activation of antithrombin III
- Activation of protein C
- Inhibition of antithrombin III
- Inhibition of protein C
- Inhibition of protein S
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
This lecture is high level, OMG! With some reading and this lecture I finally feel that I understand the cascate of coagulation. Thank you Dr. Carlo Raj, you are definitely a great teacher!
Highly recommended lecture as well as the whole Hemostasis series. Finally feel like I understand Hematology and Coagulation. Thank you so much Dr. Carlo Raj. Awesome!