Playlist
Show Playlist
Hide Playlist
Multiple Sclerosis: Clinical Features, Epidemiology, Pathology, Location of Lesions
-
Slides 01 Multiple Sclerosis Neuropathology II.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
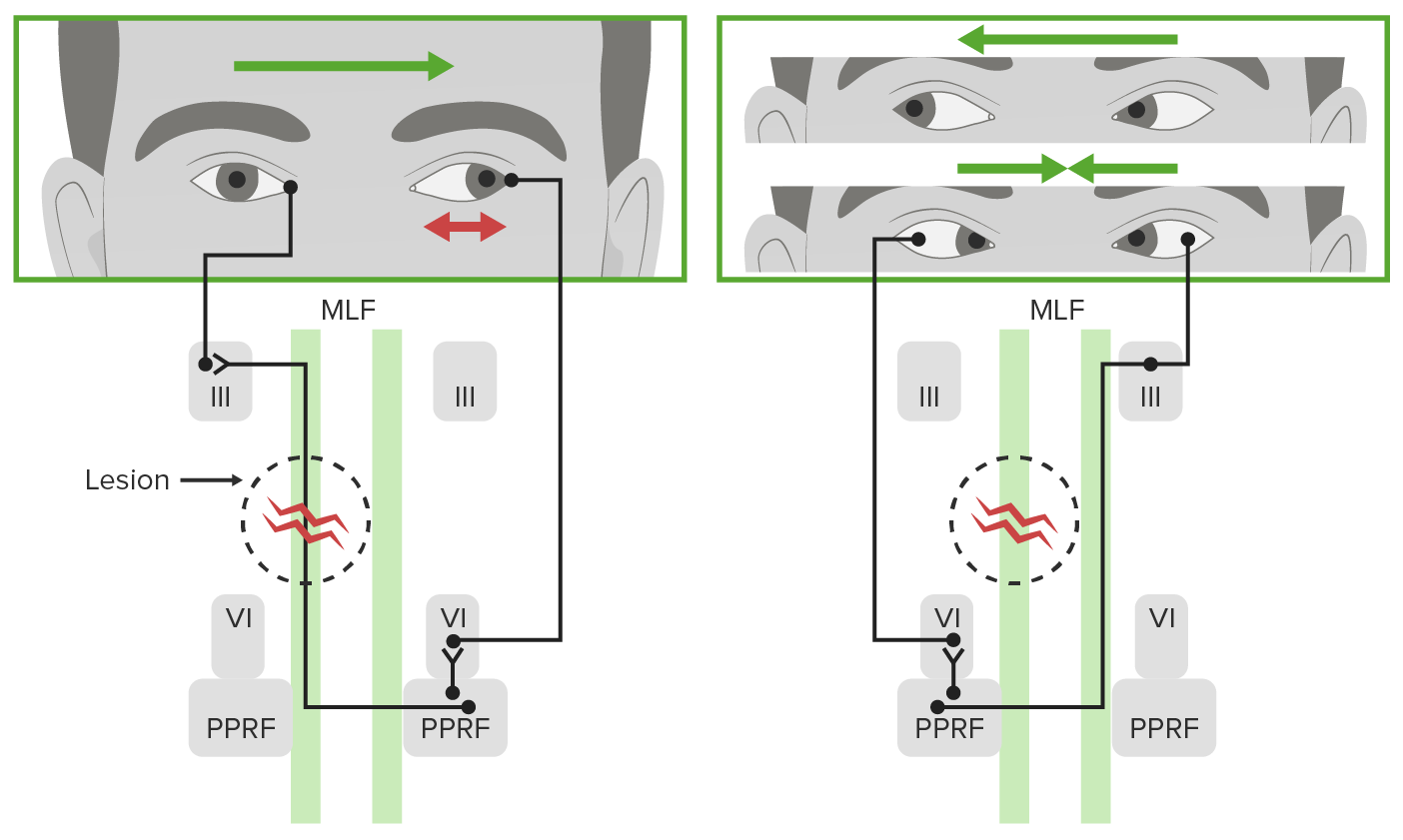
00:02 Multiple sclerosis. 00:03 So, how do we begin? How do you know? You’re reading a chart of a patient, you’re reading a clinical vignette. 00:09 How do you know the patient has multiple sclerosis? Things that you will be paying attention to immediately, unilateral visual impairment. 00:17 Once again, I emphasized unilateral visual impairment, and this is due to optic neuritis. 00:23 And so whenever you’ve heard the team optic neuritis, you should then translate into the patient having difficulty with vision. 00:32 Or retrobulbar neuritis is frequently the initial manifestation. 00:37 Now, we have to understand in clinical practice, you could have variants all the time, and I’ll walk you through a few of those, but at some point in time, we have to know as to what is the most common presentation. 00:48 Cranial nerve signs: you could have ataxia, nystagmus. 00:53 And then at some point in time, the eyes, both of them, start moving back and forth, back and forth, back and forth maybe. 01:00 And at that point, you might be thinking about lesion to the medial longitudinal fasciculus. 01:04 Please pay attention to internuclear ophthalmoplegia. 01:08 It’s a disorder of conjugate lateral gaze from interruption of fibers of the medial longitudinal fasciculus. 01:16 INO, internuclear ophthalmoplegia; MLF, medial longitudinal fasciculus. 01:22 Those are some clinical pearls there that you want to pay attention to. 01:26 Spinal cord lesions, spasticity and urinary incontinence could also be part of the syndrome. 01:32 But pay attention to, firstly, what is the initial presentation, and you’re paying attention to different behaviors of the eyes, huh? Visual impairment, optic neuritis, nystagmus or the conjugate gaze type of issue, and that’s your internuclear ophthalmoplegia. 01:52 Let’s move on. 01:54 Other clinical features that you want to keep in mind. 01:56 One is called Lhermitte’s sign. 01:58 It’s a shock-like sensation that goes up and down the spine from the neck, either due to flexion or extension. 02:05 Shock-like sensations that is moving up and down the spine, not a very good sensation. 02:11 And you have another one called Uhthoff’s phenomena. 02:13 Now, Uhthoff here, you’re looking at symptoms typically are going to get worse upon exposure to heat temperature. 02:20 So, maybe when taking a hot bath or hot shower. 02:23 These are particular clinical manifestations of multiple sclerosis. 02:29 Epidemiology: Well, what may then cause it? Well, it is kind of difficult to pinpoint exactly as to what the etiology is. 02:35 However, environmental, perhaps, genetics have been shown to play a possible role. 02:40 Immunologic factors as well, all implicated in pathogenesis. 02:44 The peak incidence: Very much pay attention to young, young, young patients, please. 02:48 And that’s unfortunate. 02:50 So imagine that this patient has the most common in clinical course, which is what again? And the peak incidence here is only between 20 to 30 years of age, very young. 02:59 So therefore, onset in childhood: much below, let’s say 20, if it’s a child at age of 10, or above the age of 50, extremely rare to find multiple sclerosis. 03:09 Could you? Well, absolutely. 03:10 However, the peak incidence is between your 20 and 30. 03:14 May become clinically apparent at any age though. 03:17 So, even though you might start young, it all depends on the variants of clinical courses. 03:23 Risk is higher when disease is present in a first-degree relative. 03:27 So therefore, there is some evidence of family history as well. 03:33 It is much more common in Caucasian. 03:35 And in the Caucasian population, it will be women that are affected more so than men. 03:43 Let’s talk about the pathology. 03:44 What then happens here? The white matter. 03:47 Okay, where? In the brain. 03:49 That’s where you begin, please. 03:50 White matter undergoes inflammatory lesions, and you could have primary and secondary, very unclear, so we’ll focus on the primary. 03:58 Now, with these white matter lesions, which I’ll show you in a second, multiple, hence the name multiple, okay? Then what? Sclerosis. 04:06 Meaning what? Well-circumscribed, irregular-shaped plaques. 04:12 What’s happening? It’s the fact that the neurologic deficit, which is separated in what? Time along with separation in space, which is represented by the white matter deterioration called these plaques. 04:26 Now, these plaques commonly occur where? Beside the lateral ventricle. 04:30 Picture that for me and I’ll show you an image in a second. 04:33 So around the lateral ventricle is where you’d expect these plaques. 04:36 What do the plaques represent? Destruction of the white matter. 04:39 It may be demonstrated to follow the course of your paraventricular veins, and we call this “Dawson’s Fingers.” Don’t worry so much about the name but understand that this has shown, interesting enough, where it follows the course of the periventricular vein. 04:57 So, very close to the lateral ventricles. 04:59 Plaques may also be found in the brain stem, spinal cord, and of course, the optic nerve, all representing what? Deterioration of the white matter. 05:07 What’s the initial presentation most commonly? Good. 05:11 Impaired vision, which is called technically? Optic neuritis. 05:18 So what about the location? Well, as you can see in the image here, you got these plaques, and these plaques are located where? Around the ventricles. 05:27 It may then follow what kind of pattern? Optic nerve could also be found, brain stem, and then also spinal cord. 05:34 Remember, you could, at some point in time, also have those shock-like lesions up and down the spine, and it could also be sensitive to temperature in terms of hot shower or hot bath. 05:43 Keep those in mind, Uhthoff's sign. 05:47 Multiple sclerosis only affects the central nervous system. 05:50 That’s important for you to understand, CNS much more so.
About the Lecture
The lecture Multiple Sclerosis: Clinical Features, Epidemiology, Pathology, Location of Lesions by Carlo Raj, MD is from the course Multiple Sclerosis. It contains the following chapters:
- Multiple Sclerosis: Clinical features
- Multiple Sclerosis: Epidemiology
- Multiple Sclerosis: Pathology
- Multiple Sclerosis: Location of Lesions
Included Quiz Questions
What is the name of the shock-like sensation that passes down the spine in a patient with multiple sclerosis?
- Lhermitte sign
- Uhthoff phenomenon
- Brudzinski sign
- Sunset sign
- Kernig sign
A 25-year-old woman presents with difficulty in her vision for the past several days. On examination, an impairment in the conjugate lateral gaze is noted. What is the most likely location of the lesion?
- Medial longitudinal fasciculus
- Lateral longitudinal fasciculus
- Medial dorsal column
- Lateral dorsal column
- Red nucleus
Which of the following is NOT a common feature in multiple sclerosis?
- Argyll Robertson pupil
- Internuclear ophthalmoplegia
- Nystagmus
- Optic neuritis
- Retrobulbar neuritis
Which of the following is NOT a likely area for the formation of plaques in multiple sclerosis?
- Pituitary gland
- Pons
- Beside lateral ventricles
- T5 to T10 spinal cord segments
- Cranial nerve II
Plaques that are seen beside lateral ventricles follow the course of which structures?
- Paraventricular veins
- Paraventricular arteries
- Paraventricular nerves
- Paraventricular lymphatics
- Paraventricular blood vessels
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |