Playlist
Show Playlist
Hide Playlist
Liver Cancer
-
Slides LiverCancer Surgery.pdf
-
Download Lecture Overview
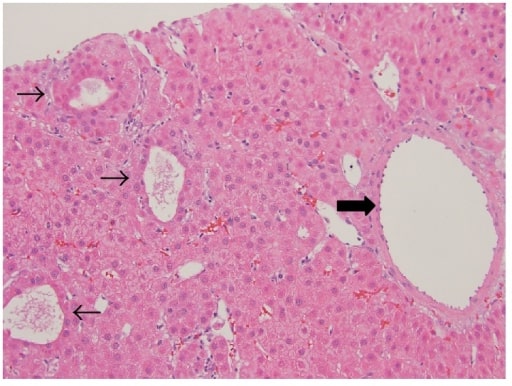
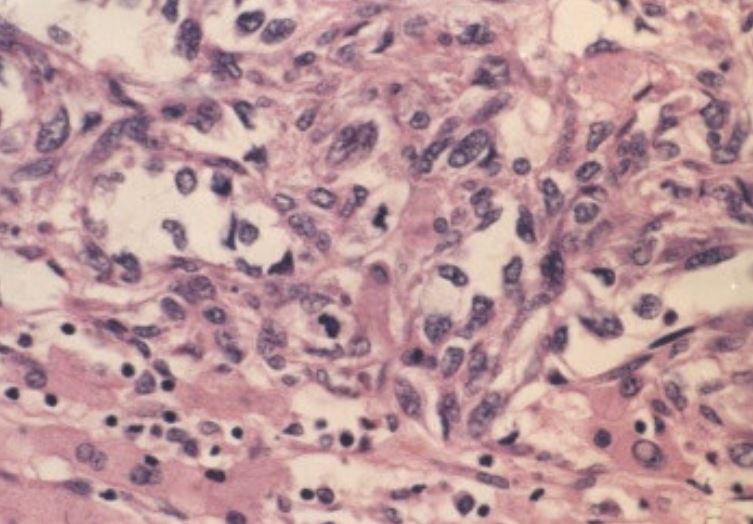
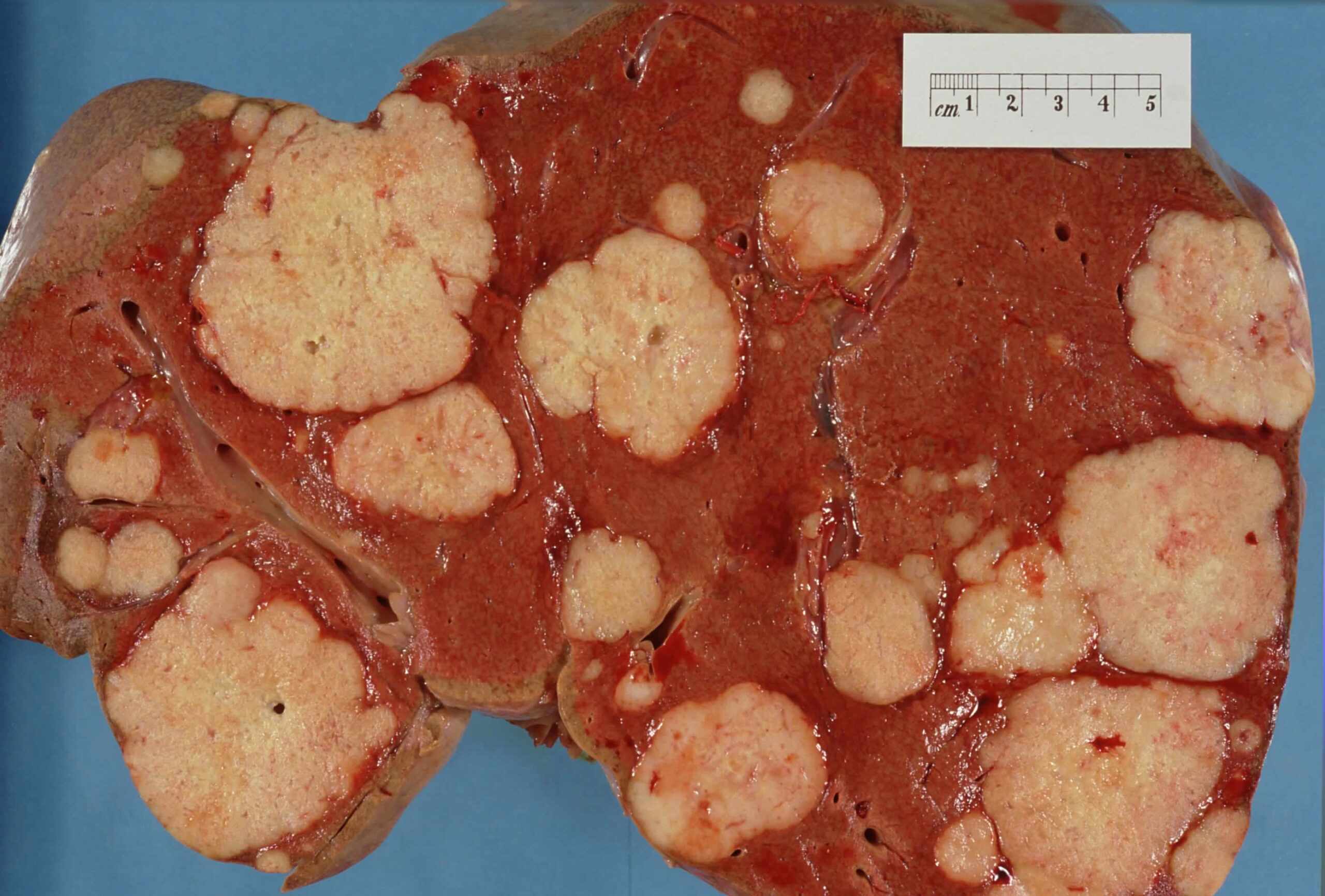
00:01 Welcome back. Thanks for joining me on this discussion of liver cancer under the section of general surgery. What’s primarily called primary hepatoma is actually hepatocellular carcinoma. 00:15 All factors that predispose to cirrhosis are risk factors for hepatomas or hepatocellular carcinoma. 00:23 As I mentioned, it’s a common misnomer but in fact, primary hepatomas of the liver are malignant and should really be called hepatocellular carcinoma. Again, cirrhosis and hepatitis particularly B and C are risk factors for hepatocellular carcinoma. Increasingly, NASH or nonalcoholic steatohepatitis which is associated with obesity, type 2 diabetes, dyslipidemia, hypertension are the metabolic syndrome. The incidence are the highest in Asia largely because of active hepatitis infections. NASH, to remind you is again increasingly common due to the obesity and metabolic syndromes particularly in the west. NASH stand for nonalcoholic steatohepatitis associated with the metabolic syndrome. Physical findings of liver cancer may include a palpable mass or a nonspecific right upper quadrant discomfort. The vast majority of patients do not complain of any abdominal pain. In later stages, there may be cancer-related weight loss and there may be jaundice when the biliary system is obstructed. In very late stages of cirrhosis, you may find ascites or fluid. This is due to the poor portal venous system drainage. 01:50 These findings would be consistent with cirrhosis. Here is a picture of a patient getting ascites drained from the abdomen. This is likely secondary to the hepatic cirrhosis. Also note, this patient also appears to be jaundiced. Unfortunately, draining of the ascites is usually just symptomatic treatment as it does not treat the cirrhosis. What are some other common findings? We talked about weight loss, potentially early satiety, and anemia. On common laboratory values, we may actually see a low sodium level. Hyponatremia is a poor prognostic indication for liver function. 02:36 Additionally, we may actually see a drop in the hematocrit. Other common tests that are obtained is the alpha-fetoprotein as a tumor marker for liver cancer. Additionally, we always assess the liver synthetic function mainly by its coagulation profile, PT, PTT, and INR. As you’re aware of, they are vitamin K dependent factors that are synthesized in the liver. AST and ALT may be variably elevated. Here’s a cross sectional imaging or CT scan of the abdomen and pelvis demonstrating multiple liver lesions. You’ll notice the highlighted regions. There are approximately three lesions in this liver. Now, remember from previous lectures, this may also represent metastatic disease. 03:27 So, the clinical context is very important. Should we do a biopsy? It’s controversial. 03:35 It’s not worthwhile for small lesions, less than 1 cm. As a reminder, CT scan images may not even pick up lesions smaller than 1 cm. But it is probably worthwhile for larger tumors to determine the next steps. Remember, liver biopsy, although often done percutaneously either by an interventional radiologist or by a hepatologist under guidance, now usually ultrasound does carry some risks. These risks include bleeding particularly if the patient is cirrhotic and already has liver synthetic dysfunction. An important classification for the cirrhosis severity is called Child Pugh classification. Each of the five categories are assigned a score of 1 to 3. 04:22 They include encephalopathy, ascites, bilirubin, albumin, and INR. The combining of these scores gives you an idea of how much of postoperative or perioperative mortality the patient may experience. 04:40 Here’s the classification. You’ll commonly hear us discuss Child’s Pugh class A, B, or C. 04:47 Class A patients have a total of about 5-6 points. This is considered mild cirrhosis and has a less than 5% chance of operative mortality. In Child’s B classification, these patients have heightened risks. Their total points are approximately 7-9 with moderate to severe disease of cirrhosis. These patients carry significant perioperative mortality of upwards of 25%. 05:11 The sickest of all cirrhotic patients are class C. These patients score approximately 10-15 points that are severe cirrhotics and generally speaking not candidates for surgery as they have prohibitive operative mortality. Recently, development of MELDs or Model for End Stage Liver Disease has surpassed Child’s Pugh as a more accurate predictor of mortality. Although originally developed for assigning cirrhosis staging for liver transplantation, multiple studies now have demonstrated that MELD is actually quite accurate for predicting perioperative mortality. It’s a little bit different than the Child’s Pugh classification, however. Take a look at this table. MELD includes creatinine, bilirubin, INR, and the latest iteration is the incorporation of sodium. Recognize that unlike the Child’s Pugh classification, these are objective findings, all laboratory results as opposed to encephalopathy or ascites which are potentially subjective. I like to pose a question to you. 06:25 What constitutes resectable disease in liver cancer? I’ll give you a second to think about this.
About the Lecture
The lecture Liver Cancer by Kevin Pei, MD is from the course General Surgery.
Included Quiz Questions
What is the geographic area with the highest incidence of hepatocellular carcinoma?
- Asia
- Africa
- Europe
- South America
- North America
Non-alcoholic steatohepatitis is associated with all of the following EXCEPT?
- Type 1 diabetes mellitus
- Obesity
- Insulin resistance
- Dyslipidemia
- Hypertension
Which one of the following is NOT included in calculating the Child-Pugh score?
- Creatinine
- Serum albumin
- Ascites
- INR
- Bilirubin
Which one of the following classes of liver cirrhosis indicates the worst prognosis?
- Child-Pugh class C
- Child-Pugh class A
- Child-Pugh class B
- Child-Pugh class D
- Child-Pugh class E
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |