Playlist
Show Playlist
Hide Playlist
Lacrimal Apparatus and Extraocular Muscles – Anatomy Review
-
Slides Structures of the external eye.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
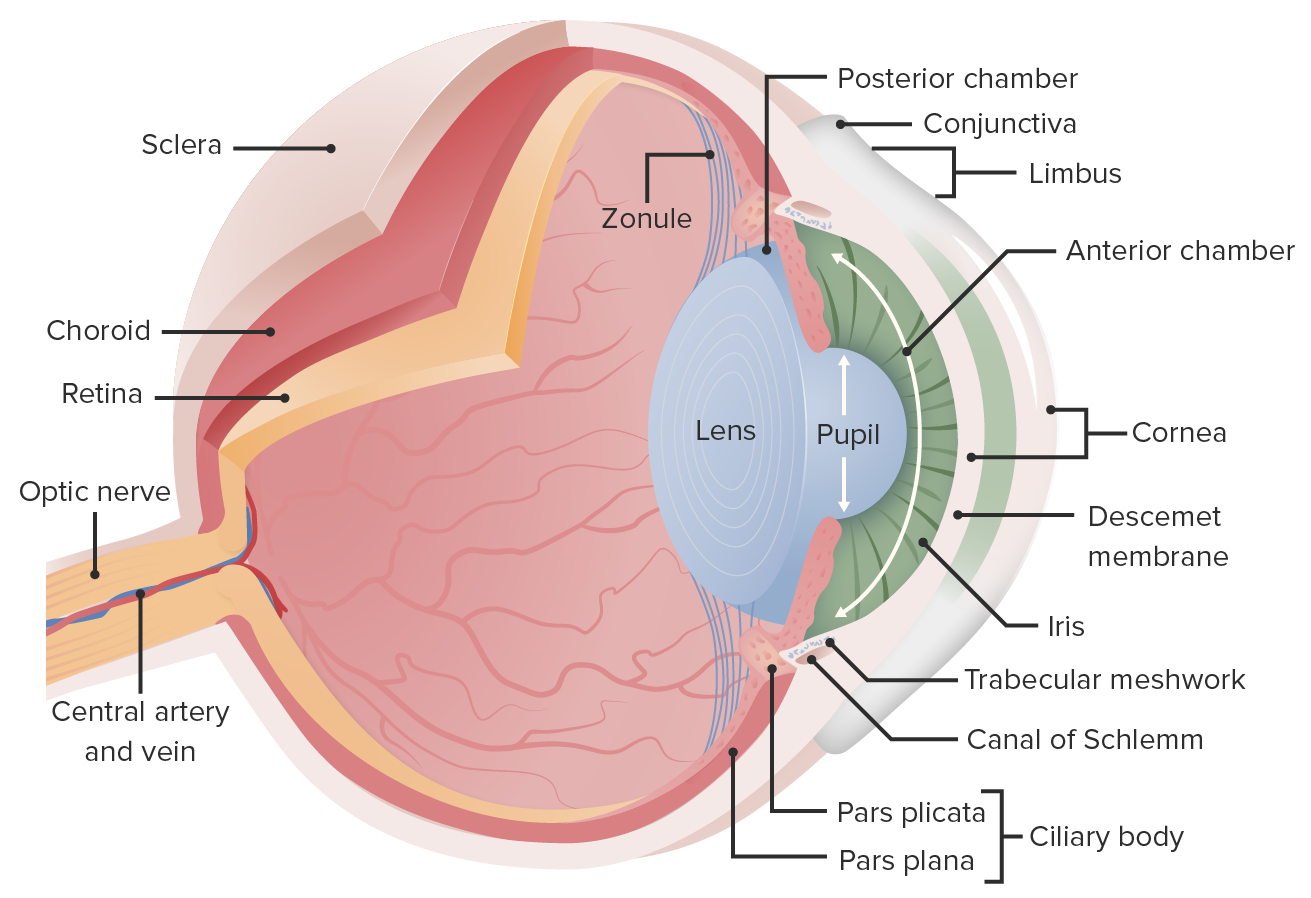
00:00 Now, we're going to look at tear ducts. 00:02 Really impressive to me that the lacrimal gland actually sits up in the upper outer quadrant of the eye. 00:11 So, if you're looking at me, it's up here on the lateral side, above the eye and that's where we're making the components of tears, lacrimation actually, it's more than just water. 00:25 There is an aqueous component, there's a mucinous component, there is a fatty component. 00:30 And the idea is lacrimal gland is providing liquid that will help to keep the eye motion. 00:37 If you think about it, the eye is basically being exposed to air all the time and we need to keep it reasonably well lubricated to keep the cells that form the eye alive. 00:48 So, the lacrimal gland is going to be very important in doing that. 00:52 The movement of the tears, the contents, the aqueous, the mucinous, the fatty component from the lacrimal gland, across the eye, comes sweeping down from that upper outer, lateral towards the medial nose and goes out our lacrimal caruncle. So the lacrimal caruncle is there, and it drains through superior and inferior lacrimal canaliculi, little tiny ducts. 01:21 And those little tiny ducts then drain into a lacrimal sac and that lacrimal sac actually drains out then through the nose. 01:29 So that's when you cry, you're actually - you can get a runny nose, and it's because of all of the fluid being made by the lacrimal glands sweeping across, going out those ducts and going out your nose. 01:40 So now you understand that as well. Kind of cool, huh? You can have inflammation. So, these various little tiny ducts can be blocked, they can become inflamed, they can fail, and then, we'll get dacryocystitis. 01:55 So, dacryo just referring to the lacrimal gland apparatus, cystitis is an inflammation of the lacrimal sac. 02:05 And it can be due to distal obstruction, you can also have inflammation of the superior and inferior canaliculi. 02:13 You can also have dacryoadenitis, if you have inflammation of the lacrimal gland itself. 02:20 Okay, let's peel back a few more layers. 02:24 Now, we're getting just to the orbit of the eye. 02:26 And we're having an anterior view, we're going to look at the musculature, all that white really important. That's the sclera. 02:33 The sclera is this dense collagenous matrix that allows the muscle to firmly attach. 02:38 So that's what provides integrity to what is basically a ball of fluid, a very important ball of fluid, but that's what the eye is. 02:47 Okay, the anterior view, and there are muscles kind of dangling off here, we'll talk about them in turn. 02:53 So, up top is the superior oblique muscle, it actually pulls the eyes so that when it is operating, it pulls the eye down and out. 03:05 It's innervated by the trochlear nerve, cranial nerve IV, as you see there, but it goes - and we'll talk more about motion in a bit, but it goes down and out, pulls the eye down and out. 03:15 We have the superior rectus muscle, innervated by the ocular motor or cranial nerve III, and that pulls the eye up. 03:23 We have the medial rectus also innervated by cranial nerve III, the ocular motor, and that pulls the eye in. 03:31 And we have the lateral rectus. All this makes sense. 03:34 Lateral rectus is on the lateral side, but it's innervated by a different nerve, cranial nerve VI, which is the abducens nerve. 03:40 And then, we have the inferior oblique, and the inferior oblique is going to pull the eye up and out. 03:53 So, it's innervated by the ocular motor. 03:55 So superior oblique pulls it down and out, and the inferior oblique is up and out. 04:01 Okay, that gets us most of the muscles. 04:03 There's one more that we can only see really well. 04:05 If we do a lateral shot. Here's our lateral shot. 04:08 So the eyeball is the white thing over there on the left, we have all the muscles wrapped around. They are inserted into the sclera. 04:16 And you can see the superior rectus and the lateral rectus is staring right at us. 04:20 So, you can see all the things that are innervating. 04:22 The muscle bundle we couldn't see previously is the inferior rectus. 04:27 This pulls the eye down, innervated by cranial nerve III, or the ocular motor. 04:33 So, they've got all the muscles, we haven't yet put them all together. 04:36 But when we do, it allows us to have eye motion. 04:39 Okay, so this is looking now down at the top of the orbits and the various muscles. 04:44 We've identified the medial rectus. 04:46 There is a video clip here, and we'll run that. 04:49 And as I'm talking, you'll see that if the medial rectus palsy eyes pulls the orbits in, you can cross your eyes. So now whenever you cross your eyes, you know that you're working on your medial rectus bilaterally and pulling the eyes in. 05:06 And with that, we finished kind of the basics of the outside of the eye.
About the Lecture
The lecture Lacrimal Apparatus and Extraocular Muscles – Anatomy Review by Richard Mitchell, MD, PhD is from the course Introduction to Ophthalmology.
Included Quiz Questions
What is one of the three components of lacrimal secretion?
- Aqueous
- Gaseous
- Crystalline
- Colloidal
- Purulent
What does the lacrimal sac drain its contents into?
- Medial nose
- Mouth
- Esophagus
- Larynx
- Duodenum
What is inflammation of the lacrimal sac called?
- Dacryocystitis
- Dacryoadenitis
- Blepharitis
- Chalazion
- Sialadenitis
What structure provides insertion to the ocular muscles?
- Sclera
- Conjunctiva
- Cornea
- Iris
- Retina
What muscle causes the eye to move upward and outward?
- Inferior oblique
- Lateral rectus
- Superior oblique
- Medial rectus
- Inferior rectus
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |