Playlist
Show Playlist
Hide Playlist
Immune Thrombocytopenic Purpura
-
Slides BleedingDisorders QuantitativePlateletAbnormalities.pdf
-
Download Lecture Overview
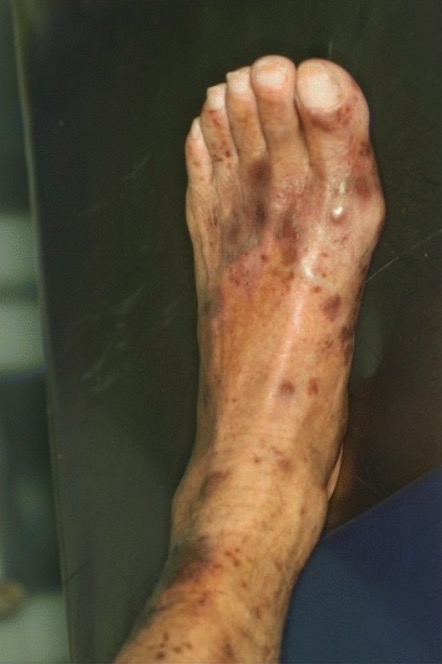
00:01 Immune Thrombocytopenic Purpura, as the name implies, it is an autoimmune disease. 00:05 The type of hypersensitivity in which the autoantibodies such as IgG may then attack the glycoproteins on a platelet. 00:13 So what does that mean to you? So as I had referred to earlier, you wanna keep the two compartments separate because of diagnostic purposes. 00:23 If it was aplastic anemia or if it was myelophthisic anemia due to infiltration, then the bone marrow has been compromised, correct? So the megakaryocyte itself is not developing properly resulting in thrombocytopenia or in this case, in peripheral circulation, not in the bone marrow, we have these autoantibodies that are then attacking the glycoproteins, could be either Ib. Picture that. 00:46 What was that binding to? Von Willebrand factor, or IIb/IIIa, that was binding to your fibrinogen or fibrin. 00:52 If then, you had this autoantibodies that are attacking these glycoproteins, then guess what? You don't have proper functioning platelets. 01:00 Welcome to Immune Thrombocytopenic Purpura. 01:02 You may then consume your platelets resulting in purpura and you also have the spleen which will get involved. 01:10 So these new, well, these abnormal platelets will then be taken to the spleen for destruction resulting in thrombocytopenia. 01:21 Welcome to ITP. 01:22 Now, as simple as it may seem in terms of pathogenesis, the symptoms could be quite difficult, so this often times ends up being a diagnosis of exclusion, as we shall see. 01:32 Let's take a look at the clinical presentation of immune thrombocytopenic purpura. 01:38 As we get older, each one of us can look forward to bruise easily. 01:42 In a patient's ITP or who may suffer from ITP, patient may also suffer from bruising easily. 01:50 However, more symptoms will be given. 01:53 Superficial bleeding may be taking place in the skin. 01:55 Look for pinpoint petechia and also purpura that might be taking place in lower extremities. 02:02 We are going to be dividing ITP into acute and chronic. 02:07 Acute will occur more commonly in children. 02:09 Self-limited as we shall see. 02:10 Whereas because this is immune, then the gender in an adult would be more commonly found in woman. 02:17 So therefore, not only would that be prolong bleeding from the cuts, we talk about increase in bleeding time, spontaneous bleeding from the gums, bleeding in to the urine or stool, and if it's a lady, when she's then having her menses, she may have increase menstrual flow. 02:33 So now you should be thinking about two situations in which there would be an increase in menstrual flow. 02:38 One would be von Willebrand disease but that's completely different. 02:41 We talk about how there might be an increase in bleeding time but then also an increase in PTT because of the lack of let's say von Willebrand factor. 02:50 That's the one that you definitely wanna know as being more common. 02:53 In ITP though, remember, these are autoantibodies attacking glycoprotein. 02:57 And profuse bleeding taking place during surgery, difficult, difficult to know that your patient may have ITP prior. 03:05 So that will be, a rather unfortunate situation. 03:08 But acute ITP is seen more commonly in children often following viral and luckily within 6 months is self-limited. 03:15 If the child has only mild bleeding symptoms, such as brusing, but otherwise asymptomatic, observation is recommended treatment regardless of platelet count. 03:23 If the patient has mucosal bleeding or other symptoms that degrade the quality of life, steroids are the first-line medication. 03:30 If its chronic ITP, then in terms of adults, it would be woman affected more so remember, in general, immune diseases affect women more commonly than men. 03:40 Gradual onset of petechia, ecchymoses. 03:44 So it started out small and the bleeding gets larger. 03:47 Diagnosed by thrombocytopenia and in your bone marrow, you're gonna find normal megakaryocyte. Why? Because once again, these autoantibodies are attacking the glycoproteins on the surface of the platelet membrane, not the bone marrow. 04:05 Treatment maybe IVIg and if counts are less than 50,000. 04:06 Treatment for these patients depends on their symptom profile. 04:10 In Cases with severe bleeding, treament includes platelet infusions, steroids, and IVIg regardless of platelet count. If patients have minimal bleeding and counts less than 50,000 or they have no bleeding but counts less than 30,000, they should get steroids and IVIg. 04:26 And finally, for patients with no bleeding symptoms and counts greater than 30,000, observation alone is considered adequate. 04:34 And you may have the spleen which may undergo splenomegaly and so therefore, splenectomy may at times be recommended.
About the Lecture
The lecture Immune Thrombocytopenic Purpura by Carlo Raj, MD is from the course Hemostasis: Basic Principles with Carlo Raj.
Included Quiz Questions
Glycoprotein IIbIIIa is a receptor on platelets for which of the following during the clotting process?
- Fibrinogen
- Tissue factor
- Factor VIII
- Prothrombin
- Thrombin
What is the most common site where petechia initially appear in patients with immune thrombocytopenic purpura and platelet deficiency?
- Lower legs
- Forearms
- Palms
- Trunk
- Scalp
Which of the following statements regarding immune thrombocytopenic purpura is NOT correct?
- Glucocorticoids are not effective.
- It is a diagnosis of exclusion.
- Involvement in children after viral infections is often self-limited.
- Incidence is higher in females.
- Intravenous immunoglobulin may be used in the treatment.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |