Playlist
Show Playlist
Hide Playlist
Herpes Simplex Encephalitis: HSV-1 and HSV-2
-
Slides 10 CNSInfections Neuropathology I.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
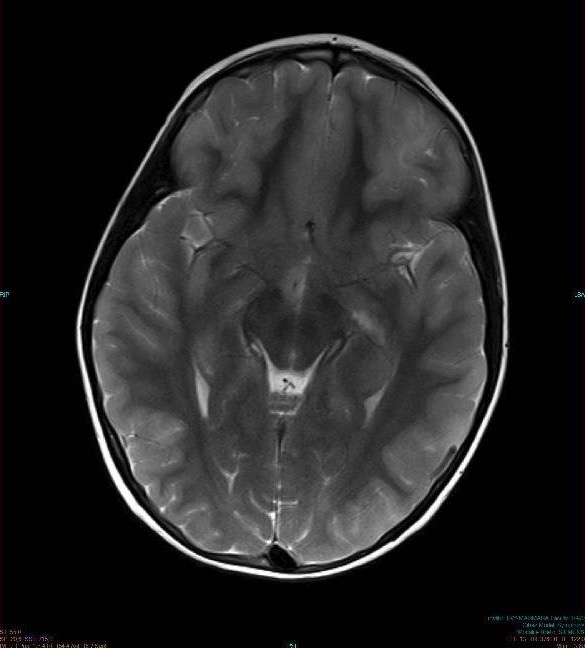
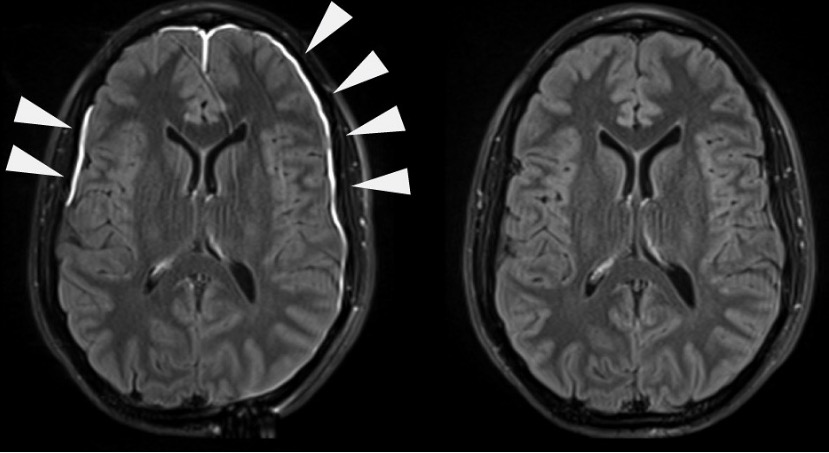
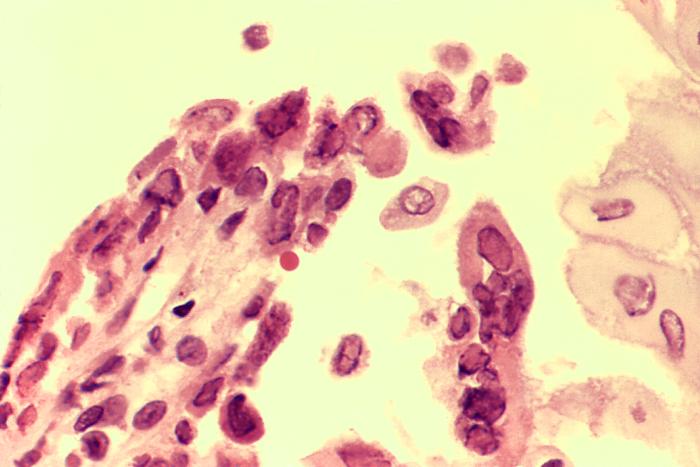
00:01 The topic now brings us to encephalitis. 00:03 We’ll make sure that we organize our thoughts before we move on. 00:06 Up until this point, we have pretty much looked at meningitidis, CNS infections, and now we are dealing with infection of the brain parenchyma. Picture that. 00:21 Confusion, delirium, focal neurologic, seizures, and coma. 00:26 May I asked you something? If your patient has meningitis, how likely is it that your patient may have seizures? If it was strictly meningitis, maybe, not necessarily. 00:38 Seizures could also be a possibility because we have encephalitis. 00:43 The main causes of seizures in patients with HSV encephalitis are related to viral induced hyperexcitability and the host immune response related to elevated body temperature. 00:56 The latter is more important in infants than young children. 00:59 Now, the infections that come into the following categories, arboviruses including your St. Louis, Eastern/Western Equine, West Nile virus. 01:11 Enteroviruses and where we will be spending time with will be HSV-1 Herpes. 01:18 If your patient is in a state of immunocompromised maybe cytomegalo, EBV, or even perhaps varicella-zoster. 01:27 What's my topic? Encephalitis. 01:30 And you'll notice for the most part, these are viruses that are commonly found as ideologies. 01:37 Our topic is herpes simplex encephalitis but here we're dealing with HSV-1. 01:43 What we'll do here is to divide HSV-1 and HSV-2 and then I will highlight to you what parts of brain are being affected with either type of viral infection. 01:55 This must be black and white for you otherwise a clinical presentation on your boards or in clinical practice is going to be difficult and if you miss it, I am going to be very upset. 02:07 Most commonly in children, young adults. That's why I'll be upset. 02:10 Most common in children, in young adults. 02:13 What parts of the brain will be affected? You should know that it's the frontal and temporal lobe. 02:19 Seizures could also be a possibility because we have encephalitis which then behaves as a space occupying lesion. 02:27 Now, HSV-1 in terms of pathology, once again, please make sure that you're familiar with, what parts of the brain? The temporal and frontal, you focus on that. 02:37 Here, the brain is undergoing such extensive damage that we have necrotization and we have often hemorrhagic, dangerous. 02:46 As soon as you hear about HSV-1 or herpes in general, you should be thinking about Tzanck and then, what kind of inclusion bodies? Cowdry. 02:54 And then the CSF, you should be thinking about PCR, polymerase chain reaction as being the most accurate diagnostic procedure. This is HSV-1. 03:05 Now, with HSV-1 we have a child that's being affected, do not waste time. 03:12 You get a history and you suspect there's mood and memory in such that's taking place and now, at this point treatment, you begin IV acyclovir as soon as possible. 03:24 Do not waste time in a child because the brain is still developing. This is HSV-1. 03:30 We're gonna move on to HSV-2 where the presentation is a little bit different. 03:35 With the HSV-2 this is then referred to as being your herpetic viral meningitis. 03:41 Granted, we also call this with HSV-1 but HSV-2 is more genital in region, isn't it? Generalized, what does that mean to you? Let me make sure that I emphasize this, if it's HSV-1, you should be thinking about the frontal and temporal lobe that's commonly affected. 03:59 If it's HSV-2, generalized encephalitis and usually much more severe. 04:06 50% of neonates born by vaginal delivery to women with active primary HSV genital infections, as soon as you hear about HSV-2, you should be thinking about that all common herpes and one in five individuals have herpes, so extremely common. 04:27 And this is one the twitches, isn't it? Vertical transmission. 04:30 And if imagine a baby, a newborn that is born with HSV-2 type of encephalitis, severe. 04:38 In AIDS patients, HSV-2 may cause an acute hemorrhagic necrotizing type of encephalitis, dangerous. 04:47 Here's the table once again on a CSF findings, guess, what we're focusing upon this time? Obviously, HSV encephalitis. 04:55 The WBC is here will be elevated primarily lymphocytes. 04:59 Neutrophils wouldn't be much elevated. 05:01 If RBCs would be found, and that's important, remember? Because brain parenchyma. 05:07 And we have glucose, well, a little bit higher than protein but your focus should be in RBCs and with the specifics that we walked through with HSV-1. 05:18 What parts of the brain? Good, temporal and frontal. 05:23 If it's HSV-2, it's called herpetic type of encephalitis. 05:29 And we call it herpetic because if it's 50% of newborns who have - who are born to a mother that has a primary HSV infection, that newborn, the brain may be completely necrotized, generalized, severe. 05:45 AIDs patient, there is no age group. 05:50 As soon as you have a patient who is severely immunocompromised who then can thrive HSV-2, what happens? Acute hemorrhagic necrotizing type of encephalitis. 06:02 Could it be anymore dramatic about HSV? Here we have another type of viral encephalitis but this is called progressive multifocal leukoencephalopathy. 06:13 As soon as you hear about PML, by reflex you should be thinking about JC, JC, JC Virus. 06:20 And in pharmacology there's certain drugs that could be then given in which your patient is predisposed to JC virus and make sure you're quite familiar with those drugs and in which the patient, amazingly, is susceptible to leukoencephalopathy. 06:39 What does that mean to you? What's "leuko" mean? White. 06:42 What's "encephalopathy" mean? Damage to the brain parenchyma, multifocal. 06:48 So, if there's destruction of your white matter, if we take a look at this imaging study, you see the areas that are opaque-ish or whitish, those are the areas in which the brain parenchyma is undergoing demyelination. 07:05 Look at this, I said demyelination as soon as your myelin in your CNS, you tell me what kind of cell is? Good, oligodendrocytes, right? So now, we have virus preferentially, unbelievably this virus will then prefer the oligodendrocytes, resulting in what? Leukoencephalopathy. 07:27 Demyelination, occurs in immunocompromised patients and also think about those drugs. 07:33 And PML does not enhance on MRI as opposed to CNS lymphomas and toxoplasmosis. 07:40 In those regions we have absence enhancement. 07:44 Here, with brain damage, you're gonna find more of your leukoencephalopathic type of findings. 07:51 VZV, when would you find this perhaps causing damage or infection of the brain? Reactivation, and with reactivation you should be thinking about a patient immunocompromised, older, and of course, this then brings you to a topic of shingles. 08:10 But there's a possibility that a brain infection may take place. 08:14 We have persistent post-herpetic neuralgia syndrome in up to 10% of patients. Be careful with this. 08:21 We say post-herpetic because what is varicella zoster? It's herpes family, isn't it? Also, associated with known as granulomatous arteritis. 08:32 And may cause an acute encephalitis with numerous sharply circumscribed lesions characterized by early demyelination. 08:43 Inclusion bodies can be found in the glia and neurons. 08:48 Here for the most part, think of reactivation please with varicella zoster virus and please don't forget about the post-herpetic neuralgia syndrome in up to 10% of your patients.
About the Lecture
The lecture Herpes Simplex Encephalitis: HSV-1 and HSV-2 by Carlo Raj, MD is from the course CNS Infections - Clinical Neurology. It contains the following chapters:
- Encephalitis
- Herpes Simplex Encephalitis: HSV-1
- Herpes Simplex Encephalitis: HSV-2
- Acute Viral Meningitis: CSF Findings
- Progressive Multifocal Leukoencephalopathy
- Varicella Zoster Virus (Herpes Zoster)
Included Quiz Questions
Which age group does HSV encephalitis most commonly affect?
- Children and young adults
- Infants and children
- Young adults and the elderly
- Elderly people
- Newborns and infants
Which part of the brain is most commonly involved in HSV encephalitis?
- Frontal and temporal lobes
- Frontal and parietal lobes
- Frontal lobe and thalamus
- Temporal and parietal lobes
- Temporal and occipital lobes
What of the following is typically seen in HSV encephalitis?
- Cowdry inclusion body
- Lewy bodies
- Basophilic inclusion bodies
- Henderson-Paterson bodies
- Auer rods
Which of the following is the most accurate diagnostic test in the management of HSV?
- CSF HSV PCR
- CSF cell counts
- CSF protein
- CSF glucose
- Clinical diagnosis
An 18-day-old girl is brought to the ER after a seizure episode. She was delivered vaginally at term and does not have any medical conditions. If encephalitis is suspected, which of the following is the most likely causative agent?
- HSV-2
- HSV-1
- St. Louis encephalitis virus
- Neisseria meningitidis
- Borrelia burgdorferi
Which of the following cells is affected in a patient with progressive multifocal leukoencephalopathy?
- Oligodendrocytes
- Microglia
- Astrocytes
- Ependymal cells
- Schwann cells
A 55-year-old man with a history of type 2 diabetes mellitus presents to the ER with altered sensorium. His wife says that he had a painful rash about 10 days ago, but he did not seek any treatment. Physical examination shows a vesicular rash in a dermatomal distribution on the left side. Which of the following is the most likely cause of his condition?
- Herpes zoster
- Herpes simplex virus type 1
- Herpes simplex virus type 2
- Borrelia burgdorferi
- St. Louis encephalitis virus
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |