Playlist
Show Playlist
Hide Playlist
Hereditary Thrombosis
-
Slides ThromboticDisorders.pdf
-
Download Lecture Overview
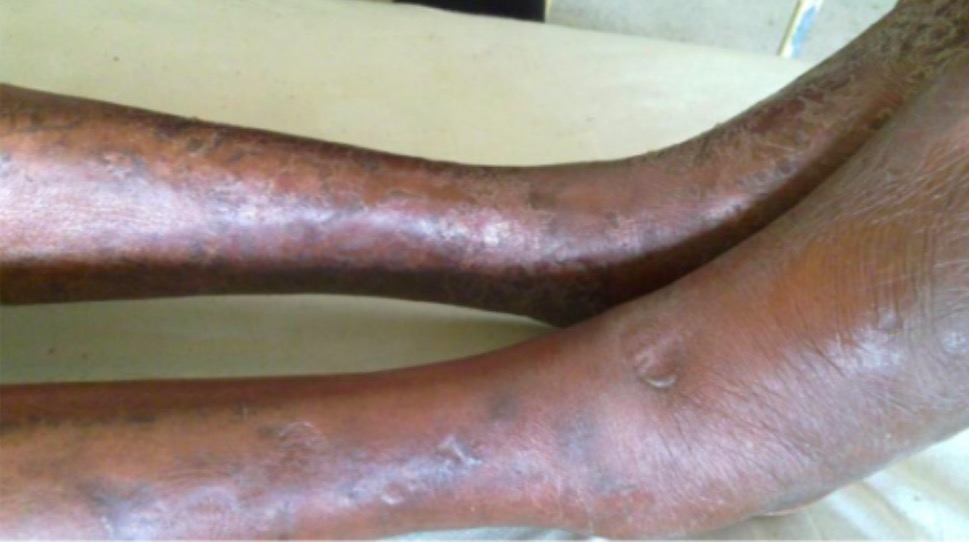
00:01 Under hereditary thrombosis, here's the most common hereditary one. 00:05 Remember that picture that I kickstarted an entire discussion with? And I gave you Factor V Leiden. 00:12 And I told you that here, normally, you have protein C and S, which does what? Which then cleaves the Factor V and Factor VIII. 00:23 But here, we have a mutation taking place between the Glutamine and the Arginine. 00:30 And when it does, the Factor V becomes resistant to the cleavage of protein C and S. 00:37 Welcome to recurrent DVT in a young lady. 00:40 Here's antithrombin III deficiency, rare. 00:45 Could it occur? Absolutely. 00:46 Normally, antithrombin III, does what? As the name implies, it knocks out the thrombin, so that the patient or you and I could not have excess thrombi. 00:57 If you're deficient of antithrombin III either congenital or acquired, remember acquired? How do we get that? Remember the urine being frothy? Lots of protein, nephrotic syndrome, there you go. 01:07 In nephrotic syndrome, the acquired type, you may lose antithrombin III. 01:12 Next activity is enhanced by heparin as we know. 01:16 And there's no prolongation of PTT after injecting a standard dose of heparin, and that is important, isn't it? Why? Because the patient is already antithrombin III deficient, so you're not gonna find what you would expect in terms of prolongation if you did not suspect the deficiency. 01:35 The hereditary type is quite rare. 01:37 Let me put it that way. The entire section here is hereditary. 01:40 Hence, usually the clinicians will not suspect or will have only diagnose it after noticing that there was no increase in PTT. 01:51 Fascinating, rare but could occur. 01:53 Protein C and S, normally does what? It cleaves Factor V, but this time you don't have it, if you don't, then you'll be in a state of once again thrombi formation and when you are, you may then cause microthrombi, and it may cause necrosis of the skin. 02:08 Kinda behaves like a... well, maybe warfarin, right?
About the Lecture
The lecture Hereditary Thrombosis by Carlo Raj, MD is from the course Hemostasis: Basic Principles with Carlo Raj.
Included Quiz Questions
Protein C cleaves which of the following pairs of clotting factors?
- Factor V and VIII
- Factor I and IV
- Factor II and VII
- Factor IX and X
- Factor XII and II
Which of the following anticoagulants is LEAST likely to be effective in the treatment of deep vein thrombosis in a patient with anti-thrombin III deficiency?
- Unfractionated heparin
- Warfarin
- Apixaban
- Rivaroxaban
- Argatroban
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |