Playlist
Show Playlist
Hide Playlist
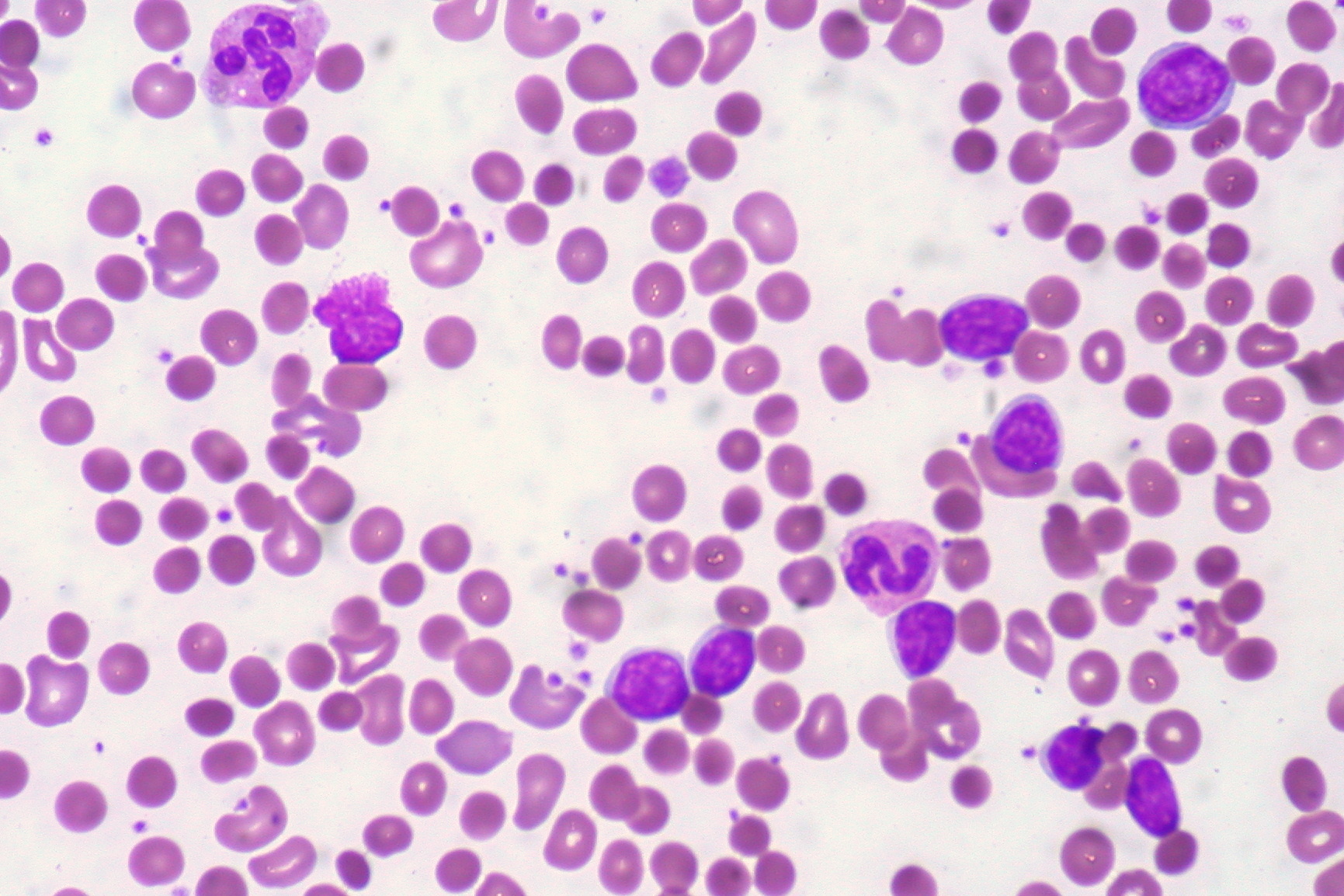
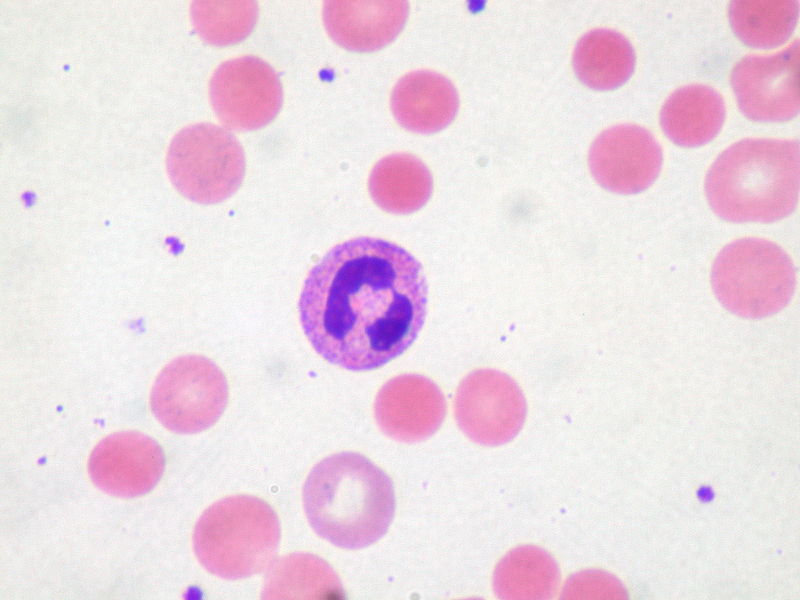
Hemolytic Anemia: Classification
-
Slides HemolyticAnemia RedBloodCellPathology.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
00:01 Under hemolytic anemias, some things that you want to keep in mind intrinsic and extrinsic, I just showed you as to how things are divided. 00:07 If you have something taking place in a pathology within the RBC itself, that would be an intrinsic defect. 00:14 Extrinsic, for example, let’s say an RBC -- Boom! Hits a mechanic valve. 00:18 Okay, and then it dies, right? So that’s an extrinsic defect, that’s not within the RBC, the valve is causing damage and destruction of your RBC. 00:27 Overall, we have hemolysis. 00:31 And the question that you’re asking yourself clinically is which one? Is it intravascular or extravascular type of hemolysis? Because that will then tell you if your patient has massive hemoglobinuria, would mean intravascular. 00:46 Extravascular would mean significant jaundice, I will give you more detail as we go through here. 00:52 Now, what about the destruction? This is what you want to pay attention to, intravascular hemolysis. 00:59 This would mean that there is a disease in which the destruction of your RBC is taking place within the blood vessel. 01:06 That is not where your RBC normally gets destroyed. 01:07 Can we agree upon that? The answer to that question, yes. 01:11 So what does that mean? You’re destroying the RBC within the vasculature, you are now releasing your hemoglobin. 01:17 That hemoglobin will most likely not get further degraded because this is not at the level of the spleen. 01:24 This will then get filtered by the kidney who is the hemoglobin. 01:28 Thus, in intravascular hemolysis, you would expect to find hemoglobinuria. 01:34 Remember that patient that I’ve been talking about over and over again in which he or she wakes up in the morning, gets surprised because he or she is passing red urine or after exercise, right? That’s intravascular hemolysis. 01:49 Clear? Extravascular. 01:53 Where does an RBC go to get destroyed? Well, it used to be called the reticuloendothelial system, that is more of an obsolete type of description, but it’s in reference to those organs such as the spleen primarily responsible for destruction of the RBC. 02:10 The spleen is not in your bed vessel. 02:13 So therefore, your RBC has been removed from the vasculature. 02:19 It’s taken to the – You know about the Billroth, the cords of Billroth, and you have a splenic macrophage that will destroy it. 02:27 You will then further degrade your heme into – Tell me about your biochemistry. 02:31 Good. 02:31 Heme, biliverdin – What kind of bilirubin? Unconjugated or indirect bilirubin. 02:40 What does that mean to you? Lipid-soluble. 02:43 How is your patient going to present? Jaundice, icterus. 02:48 Are we clear? This is the question that you’re asking yourself every single time that we go through hemolytic anemia. 02:56 I don’t care if it’s intrinsic or extrinsic, this will then tell you what your patient is suffering from. 03:01 Now, let’s continue, but one more thing. 03:04 That spleen that will be involved in extravascular, that’s a little bit of a problem, isn’t it? At some point, what if the spleen gets destroyed? Now, microbiology, what kind of organisms are you now susceptible to? Encapsulated organisms. 03:20 Now, we can move on. 03:23 So, this is a nice little picture here to show you extravascular hemolysis.
About the Lecture
The lecture Hemolytic Anemia: Classification by Carlo Raj, MD is from the course Hemolytic Anemia – Red Blood Cell Pathology (RBC).
Included Quiz Questions
Which of the following is most likely a complication of extravascular hemolysis?
- Jaundice
- Cirrhosis
- Methemoglobinuria
- Methemoglobinemia
- Aseptic meningitis
Acute intravascular hemolysis most likely presents with which of the following findings?
- Hemoglobinuria
- Pigment gallstones
- Methemoglobinuria
- Methemoglobinemia
- Cholesterol gallstones
Customer reviews
4,0 of 5 stars
| 5 Stars |
|
0 |
| 4 Stars |
|
1 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
His way of talking is bit confusing as some of the words are not clear it will be better if he talks little slow and clear