Playlist
Show Playlist
Hide Playlist
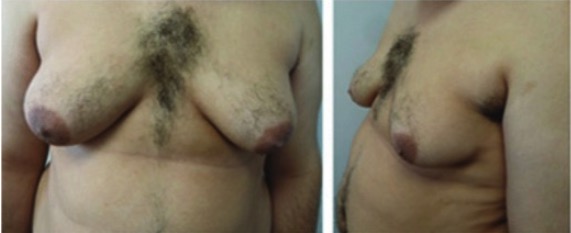
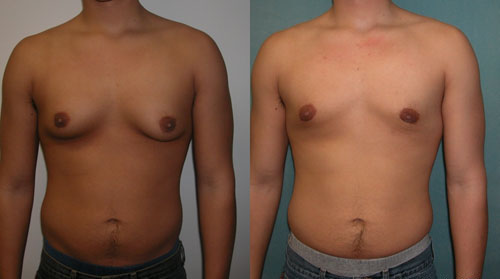
Gynecomastia
-
Slides Gynecomastia Male ReproductivePathology.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
00:00 The topic begins here with the gynecomastia. With gynecomastia in pharmacology, make sure that you are familiar with the list medications that are responsible for developing gynecomastia. 00:13 There are mnemonics out there. If I were you, I would Google it to be honest and know the list. 00:19 Our topic will begin into endocrine disorders that result in gynecomastia, actual pathology. 00:26 Hyperthyroidism could be a possibility. Primary hypogonadism especially if we’re dealing with a condition called Klinefelter which we will talk about in great detail and you should be extremely familiar with. A patient who has a genotype of XXY might also have pragmatism, jaw, masculine-like and gynecomastia or hormone-secreting tumors. For example, if you have a hormone such as estrogen that’s being released in a male, with a tumor known as your let’s say, the granulosa cell tumor, granulosa cell and producing too much estrogen resulting in gynecomastia or perhaps even hCG with the choriocarcinoma. Chronic systemic illnesses resulting in gynecomastia. 01:17 Renal diseases and hepatic diseases at times are associated with gynecomastia. Marijuana, look for that quite a bit especially in today’s society where access to marijuana, of course is becoming easier and easier. Idiopathic. Now, if gynecomastia is observed in your patient, consider malignancy if the following: unilateral, ulcerative, not concentric with nipple. 01:44 These are definite types of characteristics of gynecomastia that raises concern as to whether or not malignancy is involved. Oftentimes with gynecomastia, you might find bloody discharge or perhaps even axillary lymphadenopathy. Keep in mind though with axillary lymphadenopathy if it’s a female. Remember we were dealing with the male here but breast cancer could be found in both patients. And if it’s axillary lymphadenopathy, maybe perhaps even breast cancer. 02:14 Lab wise, renal hepatic function, important. Chronic systemic illness, renal failure, big time important. Liver failure. Testosterone to then evaluate the level of your hypogonadism if it’s indicated in a patient that has gynecomastia. I remind you to make sure that you know these alarming signs of gynecomastia that may raise concern for malignancy including unilateral, ulcerative, and not concentric with the nipple. Laboratory, FSH and LH. 02:48 If it’s going to be primary hypogonadism, you expect your FSH and LH with the gynecomastia. 02:54 Low with exogenous steroids, for example, if you have a patient who is taking steroids resulting in gynecomastia. Also, keep in mind that if a patient is taking testosterone, there’s every possibility that testosterone may undergo aromatization process. That increases estrogen resulting in gynecomastia. Here we have hypergonadotropic hypogonadism. 03:16 At this point, I expect you to know why that’s occurring. Laboratory: other things you’re looking for. Maybe perhaps you have a patient who has excess prolactin, hCG, I gave you a malignancy such as choriocarcinoma. If it’s a male, obviously it will be a germ cell tumor. 03:35 This hCG may then contribute to development of gynecomastia. Estradiol, in other words estrogen secreting tumors. I even gave an example here such as your granulosa cell tumor of the testicle. 03:48 Hyperthyroidism. With hyperthyroidism, you check to see the TSH level. If you find it to be depressed and your patient is showing you gynecomastia, well you’re also looking for other signs and symptoms of hyperthyroidism. Management: you need to get into the underlying issue but most likely cosmetic problem. You may have slight increased risk of breast cancer always with gynecomastia, especially if for example, when you talk about Klinefelter. In gynecomastia, you are worried about breast cancer developing in that patient with Klinefelter. Treatment: you need to get the underlying cause. What’s causing it? Is it the medication? Then remove the offending agent. Is it malignancy, so on and so forth? Over time, the enlarged breast tissue becomes fibrotic and will not shrink even if hormonal status normalizes. Long term damage, fibrosis. Options: anti-estrogen, for example tamoxifen, partial agonist or perhaps surgery if you’re suspecting a tumor in your patient.
About the Lecture
The lecture Gynecomastia by Carlo Raj, MD is from the course Reproductive Hormone Disorders.
Included Quiz Questions
Which of the following is NOT a cause of gynecomastia?
- Squamous cell carcinoma of the skin
- Hyperthyroidism
- Primary hypogonadism
- Granulosa cell tumors
- Choriocarcinoma
Which finding favors benign gynecomastia over malignant gynecomastia?
- Bilateral status
- Axillary LN enlargement
- Nonconcentric enlargement with nipples
- Ulcers
- Bloody discharge
Which of the following is NOT needed in the lab evaluation of gynecomastia?
- ACTH
- LH/FSH
- Testosterone
- Liver function test
- TSH
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |